Purpose: To present the succesfull endovascular repair of impending rupture of thoracic saccular aneurysm in patient with MAGIC syndrome.
Case: A 51-year-old man with a history of MAGIC syndrome was transferred to our vascular unit with a 3 days history of thoracic pain and hemoptysis. Contrast enhanced computed tomography depicted a contained rupture of a saccular aneurysm in the distal part of descending thoracic aorta. The patient was successfully managed with thoracic endovascular aortic repair (TEVAR) and Anti-TNFa factor. His immediate postoperative course was uneventful. Follow up at 2 months depicted thrombosed saccular aneurysm with excellent patency and absence of migration and endoleak.
Conclusion: Mid-term outcome of endovascular repair in patients with MAGIC syndrome seems to be safe. Due to the nature of the disease and its rarity, more studies are necessary to establish its efficacy.
MAGIC (Mouth And Genital ulcers with Inflamed Cartilage) syndrome is a very rare entity, which includes clinical manifestations of Behçet’s disease (BD) and Relapsing Polychondritis (RP) [1]. Aneurysms are considered a common complication in patients with MAGIC syndrome (21.1%), even under immunosuppression therapy, requiring emergency surgery due to its clinical presentation. Vascular involvement occurs in 14.7%-27.7% of Behcet’s Disease patients [2-4]. Aortic aneurysm is well described pathology even in this subpopulation, and its optimal treatment with immunosuppressant therapy and surgical treatment, remains to be defined. In Relapsing Polychondritis patients, aneurysms or aortitis develop in 5-10% of the patients and are multiple in 50% of them, usually involving the ascending aorta [2]. They are characterized by their presence even during remission of the disease and under lifelong immunosuppression therapy [3]. Aortic involvement is generally asymptomatic, most patients present with sudden rupture of the arterial wall with devastating and poor outcome. These aneurysms typically have a faster growing rate and rupture more easily, due to the inflammatory nature of the underlying disease. The recommended treatment for aneurysmatic disease in patients with Behçet’s Disease and Relapsing Polychondritis is based on series of isolated cases reports with small number of patients, including lifelong immunosuppressant therapy and surgical intervention, either open or endovascular. We report the successful endovascular repair of a ruptured saccular aneurysm in descending thoracic aorta followed by Anti-TNFa therapy in a patient with MAGIC syndrome.
A 51-year-old patient was admitted to our Vascular Unit from a district hospital where he was hospitalized for hemoptysis and thoracic pain. A contrast-enhanced computed tomography (CT) was performed depicting a contained rupture of a saccular thoracic aneurysm (Figure 1). On admission the patient was hemodynamically stable, hemoglobin (Hgb) was 12.5 g/dl, platelets number was 156000 and biochemical markers (including renal, liver function and electrolytes within normal range of values). His medical history was highly remarkable. He was clinically diagnosed 4 years ago with MAGIC syndrome due to presence of mouth and genital ulcers as well as a necrotic inflammation of the nasal cartilage (chondritis) leaving a permanent deficit (Figure 2). At young age he suffered from Guillain-Barre syndrome, with progressive myopathy of upper and lower extremities, and hypoglobulinemia successfully managed with lifelong immunosuppressive and immunoglobulin intravenous therapy. The patient experienced autoimmune hemolytic anemia and autoimmune thrombocytopenic purpura 4 years ago managed with high doses of corticosteroids and a stroke without permanent neurologic deficit. Due to severe steroids induced myopathy and longstanding immunosuppresive state he interrupted therapy 1 year ago by himself. The patient was fully informed for the endovascular repair and possible complications and written consent was obtained.
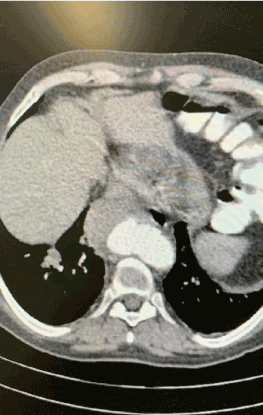
Figure 1. Contrast enhanced CT depicted contained rupture of descending thoracic aorta.
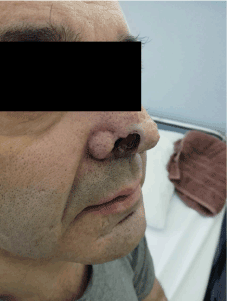
Figure 2. Nasal chondritis led to saddle-nose deformity and necrotic inflammation, leaving a permanent deficit.
The procedure was carried out in a fully equipped operation theatre under general anaesthesia. Surgical access was gained through common femoral arteries in standard surgical fashion. The patient was systematically heparinized (75 units/kg). A Terumo guidewire (Terumo Corporation, Tokyo, Japan) was inserted through the right common femoral artery to the ascending aorta which was exchanged with a 0.035 Backup Meier (Boston Scientific, USA) stiff wire. An 8F-60 cm arrow (Arrow International, Inc., Reading, PA, USA) was advanced through the left common femoral artery to the descending thoracic aorta. An aortography was performed which revealed the saccular aneurysm at the distal part of descending thoracic aorta (Figure 3). An Ankura ( Lifetech Scientific, Shenzhen, China) endovascular stent graft with 32 mm diameter and 16 cm length was deployed under fluoroscopic control. Completion arteriogram was performed with exclusion of the saccular aneurysm and absence of endoleak (Figure 4). Post operatively anti TNF-a (infliximab, 3 ml/kg) in conjunction with steroids therapy was added to patients regimen. His recovery period was uneventful. He was discharged in good general condition the 10th postoperative day under lifelong single antiplatelet therapy (aspirin), proton-pump inhibitor therapy (pantoprazole), 32mg prednisone daily for the first month followed by 16mg prednisone daily according to rheumatology specialist.
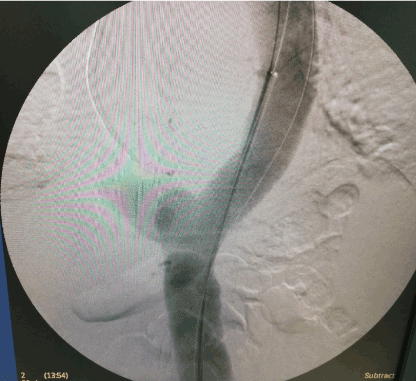
Figure 3. Intraoperative DSA revealed the saccular aneurysm of thoracic aorta.
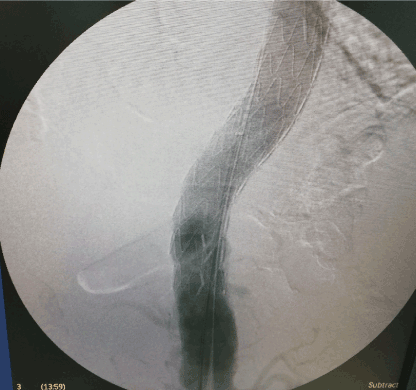
Figure 4. Final DSA after deployment of Ankura thoracic stent graft showed complete exclusion of the aneurysm without endoleak.
At 2 months post operatively, follow up CT angiography was performed depicting totally thrombosed saccular aneurysm without endoleak and migration of the endograft (Figures 5, and 6).
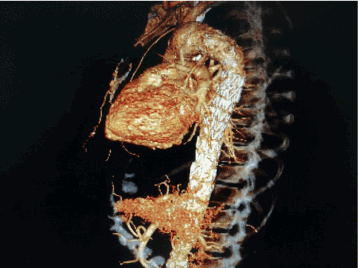
Figure 5. Follow up CT angiography of thoracic aorta revealed complete thrombosis of saccular aneurysm without endoleak or migration of the endograft.
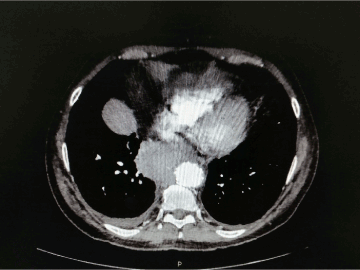
Figure 6. Follow up CT angiography of thoracic aorta revealed complete thrombosis of saccular aneurysm without endoleak or migration of the endograft.
MAGIC syndrome is a rare entity, which includes clinical manifestations of Behçet’s disease (BD) and Relapsing Polychondritis (RP). It was recognised as a distinct syndrome in 1984 by Firestein et al. who proposed the name and documented the first 5 cases [5]. Since then, less than 20 more cases have been reported in the literature [3, 6-10]. To define MAGIC syndrome, the diagnostic criteria of both the BD and RP have to be met, as these were proposed by McAdam et al. in 1976 [11] and revised by Damiani et al. in 1979 [12] for RP, and by the Behcet’s Disease International Study Group (ISG) in 1990 [13] and the International Team for the Revision of the International Criteria for Behcet’s Disease (ITR-ICBD) in 2014 for BD [14]. The diagnosis is based on clinical criteria for both diseases, as a pathognomic test does not exist for either condition. Our patient had a history of genital and oral apthosis, vascular, neurological manifestations and chondritis of nasal cartilages fulfilling the criteria BD and RP.
Behcet’s Disease is categorized as a systemic vasculitis of various-sized vessels. The most common vascular site are the veins followed by the arteries, which in turn are more likely to be thrombosed than give rise to aneurysm formation. When an arterial aneurysm in BD occurs, the most common location is a peripheral artery, like femoral, popliteal, radial, ulnar or iliac artery [15]. Abdominal and thoracic aorta are considered uncommon but well recognized locations of aneurysms in BD patients. Rupture is a devastating outcome and is the most common cause of death in BD patients.
In Relapsing Polychondritis patients, aneurysms or aortitis develop in 5-10% of the patients and are multiple in 50% of them, usually involving the ascending aorta, and can cause aortic valve insufficiency by dilatation of the aortic root, as demonstrated by Cipriano et al. [16]. Aneurysm rupture is the second cause of death in RP patients, after respiratory tract infections.
Regarding literature review, open and endovascular repair of aneurysms in patients with MAGIC syndrome have been reported in few case reports [3,17-20]. All patients were women, with a mean age of 35.6 years. Of these five, 3 had a recurrence of the aneurysm and one had a second recurrence and subsequently died intraoperatively. Ascending aorta aortic arch and aortic isthmus were the sites most commonly affected. To the best of our knowledge this is the first successful endovascular repair of descending thoracic aorta in a man with MAGIC syndrome. Our patient presented with an eccentric saccular aneurysm. These aneurysms should be treated regardless diameter due to their underlying inflammatory pathology, as they yield a higher rate of rupture.
Timing of aneurysm intervention in patients with underlying vasculitis and other inflammatory diseases has also long been debated. Although advocates of both early and late intervention exist, the international vascular society has not established specific guidelines. What is currently universally accepted as a rule of thumb is that any intervention should be made while the inflammatory process is on remission with immunosuppressant therapy, so that the active inflammation does not cause catastrophic complications. Patients presented with rupture should be urgently treated, open or endovascular repair, regardless the status of inflammatory process.
MAGIC syndrome is a rare clinical entity treated conservatively with immunosuppression therapy. Whenever complicated by rapidly growing aneurysm formation, open or endovascular repair is the treatment of choice depending on location. Thoracic endovascular repair (TEVAR) is considered a minimal invasive technique with low perioperative morbidity and mortality. However due to the small number of reports, more studies are necessary to establish its efficacy in this subgroup of patients.
No conflict of interest.
None.
The patient had been informed and written consent had been obtained from him.
- Alibaz-Oner F, Karadeniz A, Ylmaz S, Balkarl A, Kimyon G, et al. (2015) Behçet disease with vascular involvement: effects of different therapeutic regimens on the incidence of new relapses. Medicine (Baltimore) 94: e494.
- Cipriano PR, Alonso DR, Baltaxe HA, Gay WA Jr, Smith JP (1976) Multiple aortic aneurysms in relapsing polychondritis. Am J Cardiol 37: 1097-1102.
- Mekinian A, Lambert M, Beregi JP, Morell Dubois S, Launay D, et al. (2009) Aortic aneurysm in MAGIC syndrome successfully managed with combined anti-TNF-alpha and stent grafting. Rheumatology (Oxford). 48: 1169-1170.
- Kötter I, Deuter C, Günaydin I, Zierhut M (2006) MAGIC or not MAGIC - does the MAGIC (mouth and genital ulcers with inflamed cartilage) syndrome really exist? A case report and review of the literature. Clin Exp Rheumatol 24: 108-112.
- Firestein GS, Gruber HE, Weisman MH, Zvaifler NJ, Barber J, et al. (1985) Mouth and genital ulcers with inflamed cartilage: MAGIC syndrome. Five patients with features of relapsing polychondritis and Behçet's disease. Am J Med 79: 65-72.
- Lê Thi Huong D, Wechsler B, Piette JC, Papo T, Jaccard A, et al. (1993) Aortic insufficiency and recurrent valve prosthesis dehiscence in MAGIC syndrome. J Rheumatol 20: 397-398.
- Gamboa F, Rivera JM, Mayoral L, Grilo A (1998) Behçet's disease and relapsing polychondritis (MAGIC syndrome) associated with antiphospholipid syndrome. Med Clin (Barc) 110: 678-679.
- Imai H, Motegi M, Mizuki N, Ohtani H, Komatsuda A, et al. (1997) Mouth and genital ulcers with inflamed cartilage (MAGIC syndrome): a case report and literature review. Am J Med Sci 314: 330-332.
- Gertner E (2004) Severe recurrent neurological disease in the MAGIC syndrome. J Rheumatol 31:1018-1019.
- Karaca NE, Aksu G, Yildiz B, Gulez N, Turk B, et al. (2009) Relapsing polychondritis in a child with common variable immunodeficiency. Int J Dermatol 48: 525-528.
- McAdam LP, O'Hanlan MA, Bluestone R, Pearson CM (1976) Relapsing polychondritis: prospective study of 23 patients and a review of the literature. Medicine (Baltimore) 55: 193-215.
- Damiani JM, Levine HL (1979) Relapsing polychondritis-report of ten cases. Laryngoscope 89: 929-946.
- Criteria for diagnosis of Behçet's disease (1990) International Study Group for Behçet's Disease. Lancet 335:1078-1080.
- International Team for the Revision of the International Criteria for Behçet’s Disease (ITR-ICBD). The International Criteria for Behçet's Disease (ICBD): a collaborative study of 27 countries on the sensitivity and specificity of the new criteria. J Eur Acad Dermatol Venereol 28: 338-347.
- Tascilar K, Melikoglu M, Ugurlu S, Sut N, Caglar E, et al. (2014) Vascular involvement in Behçet's syndrome: a retrospective analysis of associations and the time course. Rheumatology 53: 2018-2022.
- Cipriano PR, Alonso DR, Baltaxe HA, Gay WA Jr, Smith JP (1976) Multiple aortic aneurysms in relapsing polychondritis. Am J Cardiol 37: 1097-1102.
- Ng CS, Hogan P, McKenzie S, Gibbs H, Strutton G, et al. (2007) Mouth and genital ulcers with inflamed cartilage (MAGIC) syndrome complicated by aneurysmal aortitis. J Clin Rheumatol 13: 221-223.
- Fernández-Monrás F, Fornós C, Argimón J, Pujadas R (1997) Aneurysmatic aortitis in the MAGIC syndrome. Med Clin (Barc) 109: 684-685
- Hidalgo-Tenorio C, Sabio-Sanchez JM, Linares PJ, Salmerón LM, Ros-Die E, et al. (2008) Magic syndrome and true aortic aneurysm. Clin Rheumatol 27: 115-117.
- Caceres M, Estrera AL, Buja LM, Safi HJ (2006) Transverse aortic arch replacement associated with MAGIC syndrome: case report and literature review. Ann Vasc Surg 20: 395-398.






