Background: Surgical site infection (SSI) is a major source of adverse operation-related events in patients undergoing surgery, including increased morbidity, additional cost and delay of postoperative adjuvant therapies. The aim of this randomized clinical trial is to determine whether prophylactic antibiotics are indicated in patients undergoing modified radical mastectomy (MRM) and to identify the risk factors that increase the rate of post-operative SSI in Indian population.
Patients and methods: This study was a randomized double-blinded clinical trial involving 173 patients who underwent modified radical mastectomy, 76 in the control group; 97 in the antibiotic group. Injection Cefazolin 1 g intravenous and normal saline were used. Post operatively patients were followed for up to 30 days for SSI defined according to CDC criteria.
Results: There was no significant difference in the rate of infection with the use of antibiotics. The rate of infection in the antibiotic group was 17.5% while it was 19.7% in the placebo group. There was no significant different in the infection rates with use of antibiotics (p = 0.844). Older patients, those with BMI greater than 25, diabetics and hypertensives had higher rates of SSI. It was found that patients who had wound approximated with silk sutures had higher incidence of infection compared to the patients in whom staplers were used for skin closure. Patients who developed infection had significantly longer duration of hospital stay. The mean total duration of stay in patients who had infection was 21.4 days as compared to 14.19 days in the patients who did not have SSI. Longer preoperative stay due to various reasons resulted in higher incidence of SSI and consequently those patients had to stay longer for infection control post operatively also.
Conclusion: Although there was no difference in the rate of infection in both the groups, due to the high rate of infection, role of prophylactic antibiotics cannot be ignored. But the choice of antibiotic has to be studied further. Antibiotic administration to be considered for patients at higher risk of developing surgical site infection. Longer pre-operative hospitalisation is to be avoided.
mastectomy, cefazolin, surgical site infection
Surgical site infections (SSIs) are concerning adverse events in patients undergoing breast cancer surgery, causing increased morbidity, psychological trauma, additional cost and delay of postoperative adjuvant therapies. The surgical site infection rate is higher in breast surgeries compared to other clean procedures where the infection rate is below 5% [1]. The infection rate following breast surgeries range between 1–30%. This depends on the definition used to detect surgical site infections, type of surgery, co morbidities associated with the patients, the time of follow up, perioperative procedures including chemotherapy and reporting institution. The use of antibiotics in the preoperative and perioperative period was found to reduce the rates of infection in clean surgeries. At the same time there has been no consensus regarding the prophylactic use of antibiotics in mastectomy patients [2]. Multiple trials have been conducted to assess the prophylactic use of antibiotics in patients who underwent primary breast surgery [3-6]. The results were statistically significant in favour of the group receiving antibiotics, however there is not enough evidence either to support or to repudiate this proposal. The lack of definitive guidelines to administer preoperative antibiotics combined with lack of uniformity in study population has necessitated this study. To date no study has been done exclusively defining the role of perioperative antibiotics in patients undergoing surgery for carcinoma breast in India. The aim of this study was to determine whether prophylactic antibiotics are categorically indicated in patients undergoing modified radical mastectomy (MRM) and to identify the factors associated with SSI in these patients.
This was a double-blind randomized study in patients undergoing modified radical mastectomy from January 2013 to May 2014 in a tertiary care institute in South India after obtaining clearance from the Institute Research Committee and Institute Ethics Committee.
Study population
All consecutive patients undergoing MRM who consented for the study during the study period were included in the study. The patients who were hypersensitive to intravenous Cefazolin, patients with local skin infections at the site of surgery, patients on steroids and with immunosuppressive diseases were excluded from the study. Patients requiring breast reconstruction were also excluded from the study as antibiotics were administered as a policy in the post-operative period.
Sample size, randomization, allocation concealment, and blinding
A total of 219 patients were operated during the study period. Nineteen patients were excluded as they were on antibiotic coverage for fungating breast carcinoma. The remaining 200 hundred patients were randomized to the control group and study group by block randomization (block size of 10) using Microsoft Excel 2010 (Microsoft Corp, Redmond, WA, USA). Allocation concealment was done using serially numbered opaque sealed envelopes. Randomization and sealed envelopes were prepared by an independent nurse not involved in the study. Envelopes were opened on the day of surgery outside the operating room by a nurse not involved in the study. The antibiotic solution or the multivitamin solution were prepared outside the operating room and the corresponding solutions were given to the anaesthetist and the operating team. As the colour of Injection Cefazolin and multivitamin were same in colour, blinding was easy. The patient and the investigator who assessed the outcomes also were blinded to the drug used. At the end of the study, the patients were decoded and analysed (Figure 1).
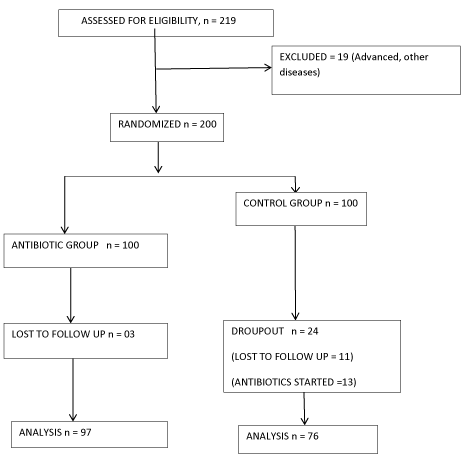
Figure 1. Consort diagram.
Procedure
Standard study protocol was followed in all the patients. The study group received one gram of Injection Cefazolin intravenously one hour before skin incision and the control group received 10 ml of Injection multivitamin as a placebo. Ioprep (1% w/v Iodine, Johnson & Johnson) was used for skin preparation in all the patients. Uniform operating steps were followed irrespective of the grade of the surgeon with respect to raising skin flaps, mobilization of the breast tissue, and for axillary dissection. Drains were placed in all patients and standard sterile dressing was done at the end of the procedure. No post-operative antibiotics were used. Dressings were removed at 48 hours after surgery, when the first wound inspection was done. Subsequent wound inspections were done daily until discharge of patient. Patients were discharged at the discretion of the operating surgeon. Patients were followed up every week until the 30th post-operative day. All the patients were educated about the symptoms and signs of SSI and were instructed to report to us in case they developed any such symptoms and signs. SSI were recorded as per Centers for Disease Control and prevention (CDC) guidelines.
Data collection
Patient demographics, co-morbidities, American society of Anaesthesiologist’s (ASA) score, neoadjuvant treatment, breast cancer stage, number of prior biopsies/surgeries, preoperative hospital stay, post-operative hospital stay, grade of surgeon, duration of surgery and wound complications were assessed. Severity of wound complication was assessed using Southampton Wound Assessment Scale.
Grade of the surgeon was defined as: Consultant - Surgeon who had experience of 5 years or more, Senior Resident – Surgeon who had experience of > 3 years but less than 5 years, Junior resident - Surgeon who had experience of > 2 years but less than 3 years.
Outcome
The primary outcome of the study was to determine whether antibiotic prophylaxis was statistically significant in reducing the SSI. The secondary outcomes were to assess the factors causing SSI.
Statistical analysis
Statistical analysis was performed using SPSS version 16 for Windows (SPSS, Inc., an IBM company, Chicago, Illinois, USA). The variables were summarized using mean, standard deviation, median, interquartile range, percentages based on the characteristics of the variable. Independent sample student t test for means and Mann Whitney U test were used as appropriate for continuous variables like age, BMI, duration of surgery, days of hospital stay based on the normality of the distribution. Chi-Square test was used for categorical variables like stage of the disease, comorbidities, ASA grade, whether patient received prior chemotherapy or not, previous number of invasive procedures. A p value of < 0.005 was considered statistically significant.
The study population was divided into two groups namely antibiotic group and control group for analysis of the data. Demographic data were comparable in both the study and control group (Table 1). The mean age of the total study population was 50.39 years. The median age in the study group was 54 years and the range was 34 to 84 years. The age range in control group was 24 to 72 years. Patients in both the groups were comparable with respect to body mass index.
There was no significant difference among distribution of diabetic and hypertensive patients in both the groups. Antibiotic group had 34 patients each in stage II B and stage III A while control group had 32 and 29 patients respectively (Table 1).
Table 1. Baseline demographic and clinical data in study population
|
Antibiotic group
n = 97 |
Control group
n = 76 |
Total
n = 173 |
p value |
Age (Years)
Mean ± SD |
49.98 ± 10.12 |
50.91 ± 9.08 |
50.39 ± 9.66 |
0.527 * |
BMI (kg/m2)
Mean ± SD |
24.17 ± 3.49 |
23.97 ± 4.21 |
24.09 ± 3.81 |
0.737* |
Diabetes Mellitus
n (%) |
30 (58.8%) |
21 (41.2%) |
51 (29.5%) |
0.737† |
Hypertension
n (%) |
28 (49.1%) |
29 (50.9%) |
57 (32.9%) |
0.254† |
Clinical Stage
I
II A
II B
III A
III B
III C
IV
X |
2
11
34
34
8
1
0
7 |
0
5
32
29
7
0
1
2 |
2 (1.2%)
16 (9.2%)
66 (38.2%)
63 (36.4%)
15 (8.7%)
1 (0.6%)
1 (0.6%)
9 (5.2%) |
0.418‡
|
ASA Grading
I
II
III |
23 (23.7%)
65 (67.0%)
9 (9.3%) |
12 (15.8%)
60 (78.9%)
4 (5.3%) |
35 (20.2%)
125 (72.3%)
13 (7.5%) |
0.215† |
Neo Adjuvant Chemotherapy |
42 (58.3%) |
30 (41.7%) |
72 (100%) |
0.644† |
* - Independent Student T test
† - Chi square test
‡ - Chi square test (no interpretation can be drawn as the values in some of the cells were less than the expected values)
Majority of the patients belonged to ASA category II in both the groups. Forty-two patients (58.3%) in the antibiotic group and 30 patients (41.7%) in the control group had received neo adjuvant chemotherapy (Table 1).
The average pre-operative stay in the patients in the antibiotic group was 3 days with an interquartile range of 1.5 to 8.5 days. The average pre-operative stay in the control group was 7days with an interquartile range of 2 to 10 days. The mean stay preoperatively in the entire study group is 5.7 ± 4.72 days (Table 2).
Preoperative hospital admission was required in patients to optimize uncontrolled diabetic and hypertensive status. Being a tertiary care centre, providing free surgical treatment, the number of admissions in the surgical unit outnumber the operative slots per week. This was also a reason for increased preoperative stay in the study population.
Eighty percent of the patients in the antibiotic group (n = 61) had 2 procedures prior to MRM and seventy-six percent (n = 74) of the patients had undergone two procedures in the control group. The number of prior procedures were statistically insignificant among both the groups.
All patients received general anaesthesia, and 91 patients received suture site infiltration with 20 ml of 0.25% bupivacaine at the suture site post procedure. Out of them 50 patients were in study group and 41 patients were in the control group. Eleven patients had received paravertebral block along with general anaesthesia, of which 5 patients were in antibiotic group and the remaining 6 in the control group. Seventy-one patients did not receive any local or regional anaesthesia (Table 2).
Majority of the procedures were performed by senior residents (52.6%) followed by consultants (41.6%). There was no statistical significance in-between the two groups. The mean duration of surgery was also statistically insignificant between both the groups (2.38 hours vs 2.28 hours) (Table 2).
Table 2. Operative characteristics in study population
|
Antibiotic group
n = 97 |
Control group
n = 76 |
Total
n = 173 |
p value |
Pre-op stay (days)
Median (IQR) |
3 (1.5 - 8.5) |
7 (2 – 10) |
5.7 ± 4.72 |
0.018* |
Type of Anaesthesia, n (%)
GA
GA + LA
GA + RA |
42 (59.2%)
50 (45.1%)
5 (54.5%) |
29 (40.8%)
41 (54.9%)
6 (45.5%) |
71
91
11 |
0.662† |
Grade of surgeon
Consultant
Senior Resident
Junior Resident |
42 (43.3%)
59 (52.6%)
4 (4.1%) |
30 (39.5%)
40 (52.6%)
6 (7.9%) |
72 (41.6%)
91 (52.6%)
10 (5.8%) |
0.549† |
Duration of surgery (Hours)
Mean ± SD
|
2.38 ± 0.61 |
2.28 ± 0.61 |
2.33 ± 0.61 |
0.309‡ |
Skin Closure, n (%)
Sutures
Staplers |
82 (56.6%)
15 (53.6%) |
63 (43.4%)
13 (46.4%) |
145
28 |
0.837† |
* - Mann Whitney U test
† - Chi square test
‡ - Independent Student T test
LA: local infiltration with 0.25% bupivacaine
RA: Regional block –Paravertebral block
Post procedure, before closing the skin negative suction drains were placed, one for the flap and one for the axilla. The mode of skin closure was by using silk sutures or skin staplers. There was no significant difference among the groups in terms of closure methods used.
The mean duration of hospital stay in the antibiotic group was 9.58 ± 4.84 days while it was 10.17 ± 3.90 days in the control group. The mean day of suture removal in the study group was 9.79 ± 2.29 days and in the control group was 9.89 ± 2.38 days. The mean day of drain removal was 6.53 ± 2.03 days in the antibiotic group and 7.04 ± 2.34 days in the control group (Table 3).
Surgical site infection incidence was found to be 18.49 % in the total population. In the antibiotic group the rate of infection was 17.5% and the infection rate in the control group was 19.7%. Hence there was no statistically significant difference in the incidence of infection in both the groups (p = 0.844) (Table 3).
Table 3. Post-operative course and surgical site infection in study population
|
Antibiotic group
n = 97 |
Control group
n = 76 |
Total
n = 173 |
p value |
Duration of Post op stay |
9.58 ± 4.84 |
10.17 ± 3.90 |
9.84 ± 4.45 |
0.373* |
Suture removal day |
9.79 ± 2.29 |
9.89 ± 2.38 |
9.84 ± 1.56 |
0.131* |
Drain removal day |
6.53 ± 2.03 |
7.04 ± 2.34 |
6.75 ± 2.18 |
0.679* |
SSI
SSI present, n (%)
No SSI, n (%) |
17 (17.5%)
80 (82.5%) |
15 (19.7%)
61 (80.3%) |
32 (18.49%)
141 (81.5%) |
0.844† |
Time of Detection of SSI
At 48 hours
At week 1
At week 2
At week 3
At week 4 |
0
12
5
0
0 |
0
8
7
0
0 |
0
20 (62.5%)
12 (37.5%)
0
0 |
|
Wound Outcomes
Erythema
Pus
Wound gaping
Superficial Marginal necrosis |
11 (11.34%)
0
6 (6.19%)
13 |
10 (13.16%)
2 (2.63%)
3 (3.95%)
9 |
21 (12.13%)
2 (1.15%)
9 (5.2%)
22 |
|
Southampton Severity Score
1
2
3
4
5 |
3
11
8
0
6 |
1
10
5
2
3 |
4
21
13
2
9 |
|
*- Independent Student T test
† - Chi square test
In the present study, SSI was assessed with the help of Southampton scoring system which graded the wounds into 6 categories, out of the 50 patients with SSI, only 2 patients had purulent discharge from the wound which was culture positive and 9 patients had deep or severe wound infection which was also culture positive. Rest of the patients had either erythema or serosanguinous discharge.
The most common organism isolated was staphylococcus aureus in 15.6% of the SSI. Other organisms isolated were pseudomonas species, Klebsiella species, Acinetobacter baumanii, Enterobacter species and Proteus mirabilis. 37.5% of patients with SSI had no growth isolated from the pus culture.
Most of the infections were detected between post-operative days 5 and 8. Out of the 32 cases with SSI, 20 cases (62.5%) were identified in the first week and 12 (37.5%) were identified in the second week. In the present study, none of the patients had SSI after two weeks.
Southampton severity score was assessed, and 21 patients had a score of 2 while 13 patients had a score of 3. Nine patients had score 5 of which 3 were in the antibiotic group (Table 3).
Patient demographics, comorbidities, preoperative procedures done in the breast prior to the surgery, receipt of neoadjuvant chemotherapy, intraoperative factors like the surgeon’s qualification, suture material type, operative time, post-operative factors (i.e. drain removal day and suture removal day) were not associated with an increase in the postoperative infection risk (p ≥ 0.05) (Tables 4 and 5).
Table 4. Patient parameters and surgical site infection
|
SSI
n (%) |
No SSI
n (%) |
p value |
Age (years) Mean ± SD |
54.25 ± 12.12 |
49.51 ± 8.83 |
0.012* |
BMI (kg/m2) Mean ± SD |
24.22 ± 3.89 |
24.05 ± 3.80 |
0.824* |
ASA Grade
ASA 1
ASA 2
ASA 3 |
4 (11.43%)
23 (18.4%)
5 (38.46%) |
31 (88.57%)
102 (81.6%)
8 (61.5%) |
0.196† |
DM
Non-DM |
12 (23.5%)
20 (16.4%) |
39 (76.5%)
102 (81.6%) |
0.288† |
HT
Non HTN |
14 (24.6%)
18 (15.5%) |
43 (75.4%)
98 (84.5%) |
0.211† |
Neo-Adjuvant Chemotherapy
Received
Not Received |
11 (15.3%)
21 (20.8%) |
61 (84.7%)
80 (79.2%) |
0.429† |
*- Independent Student T test
† - Chi square test
Table 5. Operative variables and surgical site infection
|
SSI
n (%) |
No SSI
n (%) |
p value |
Preoperative Stay (Days)
Median (IQR) |
9 (3-11.75) |
4 (2-9) |
< 0.001* |
Anaesthesia
With local infiltration
Without local infiltration |
18 (19.8%)
14 (17.1%) |
73 (80.2%)
68 (82.9%) |
0.698† |
Grade of Surgeon
Consultant
Senior Resident
Junior resident |
18 (25%)
11 (12%)
3 (30%) |
54 (75%)
80 (87.9%)
7 (70%) |
0.068†
|
Duration of Surgery (Hours)
Mean ± SD |
2.51 ± 0.70 |
2.286 ± 0.57 |
0.097* |
Skin Approximation
Sutures
Staplers |
29 (20%)
3 (10.7%) |
116 (80%)
25 (89.3%) |
0.300† |
Postoperative Stay (Days)
Median (IQR) |
11 (8-15) |
9 (7-11) |
0.007‡ |
Total hospital Stay (Days)
Mean ± SD |
21.4 ± 9.44 |
14.19 ± 5.44 |
< 0.001* |
*- Independent Student T test
† - Chi square test
‡ - Mann Whitney U test
Preoperative hospital stay was longer in patients with SSI with a median of 9 days with interquartile range of 3 to 11.75 days compared to patients without SSI where the median hospital stay was 4 days with interquartile range of 2 to 9 days. This was significant statistically (p ≤ 0.001) (Table 5).
The post- operative hospital stay in the group with SSI was higher in view of the infection per se. The median post-operative hospital stay was longer for the patients who had SSI compared to those who did not (median hospital stay 11 days (8 to 15 days interquartile range) vs. 9 days (interquartile range of 7 to 11 days) respectively, p = 0.007) (Table 5).
The total hospital stay was also higher in patients with SSI, 21.49 days in patients with SSI compared to 14.19 days patients with no SSI, there was a statistical significance with p ≤ 0.001 (Table 5).
The study was undertaken to identify the effectiveness of single dose intravenous cefazolin as a prophylaxis for patients undergoing MRM in our centre. Though there was no significant statistical difference between the antibiotic and the control group, the authors determined the factors responsible for SSI in the study population. A comparison of previous studies with the present study in relation to the antibiotic and control used, randomization, SSI definition and follow up and conclusion has been tabulated in table 6.
Table 6. The comparison of studies in relation to the antibiotic and control used, randomization, SSI definition, follow up and conclusion.
|
Patients |
Antibiotic used |
Control |
Randomization |
Definition of SSI |
Follow up |
SSI in Antibiotic group |
SSI in Control group |
Result |
Present study |
173 patients undergoing modified radical mastectomy (MRM) |
Single dose IV 1 gm cefazolin at induction of anesthesia |
Placebo |
Yes |
CDC criteria |
30 days |
17.5% |
19.7% |
No significant difference in infection rates |
Gullogullu et al. [11] |
369 obese (BMI > 25) patients with primary non-recurrent operable breast cancer |
Single dose 1 gm ampicillin –sulbactam IV at anesthesia |
No antibiotic |
Yes |
SSI prevention guidelines by Mangram et al |
30 days |
4.8% |
13.7% |
Significant decrease in SSI rate in antibiotic group |
Cabaluna et al. [7] |
254 patients undergoing MRM |
Single dose IV 1 gm cefazolin at induction of anesthesia |
Placebo |
Yes |
SSI severity grading |
30 days |
13.4% |
15 % |
Antibiotics are not effective |
Yetim et al. [20] |
44 patients undergoing MRM |
Gentacoll containing 200 mg gentamycin sulphate placed under
the flaps and in axillary area |
No gentacoll |
Yes |
Not mentioned |
6 months |
0% |
18% |
Postoperative SSI rate significantly less in antibiotic group |
Paajanen et al. [21] |
292 patients undergoing non-reconstructive breast cancer
surgery following core needle biopsy |
Single dose 1 g of dicloxacillin administered
30 minutes before surgery |
Placebo |
Yes |
SSI score |
30 days |
5.6% |
8.8% |
Antibiotics did not prevent SSI |
Hall et al. [6]
|
618 patients of which 107 patients undergoing MRM |
Single dose IV Flucloxacillin 2 gm at
induction of anesthesia |
No antibiotics |
Yes |
Wound scoring system |
42 days |
3.2% |
4.6% |
Antibiotics not necessary |
Gupta et al. [22] |
357 patients undergoing different breast surgeries
of which 147 underwent MRM |
Single dose of IV 1.2 g Augmentin
(200mg clavulanic acid and 1000mg amoxycillin) |
Placebo |
Yes |
SSI severity grading |
10 – 14 days |
17.7% |
18.8% |
Antibiotics not required for clean breast surgeries |
Chow et al. [23] |
56 patients undergoing MRM |
Oral Clarithromycin at a dose of 500 mg twice a day,
from the day before to 3 days after surgery |
No antibiotic |
Yes |
Not mentioned |
5 days |
Not mentioned |
Not mentioned |
No difference in postoperative wound infections |
Wagman et al. [24] |
118 patients undergoing breast surgeries |
Multiple dose IV cefazolin 1 gm |
Placebo |
Yes |
SSI severity |
30 days |
5.08% |
8.47% |
Antibiotics not beneficial |
Antibiotic choice
In this study a single dose of IV cefazolin was given as the prophylactic antibiotic. Cefazolin has been used as a prophylactic antibiotic in the literature, but the dose of cefazolin was varied. One study had used single dose of cefazolin similar to the present study [7] while another study in the literature had used six doses of intravenous cefazolin. Various antibiotics have been used by different investigators in the previous studies. Cefazolin was chosen in our study as it has a proven efficacy against the gram-positive cocci which are responsible for most of the SSI’s [8].
Infection rate
In the present study, the overall infection rate was 18.49%, in patients undergoing MRM. The incidence of wound infection was 19.7% in the control group and 17.5% in the antibiotic group. The incidence of surgical site infection following breast surgeries ranges from 3% to 15 % [8]. The incidence of wound infection was higher in our study population when compared to other studies. This result was similar to a study done in patients who underwent MRM. The infection rate was 14.2% [7]. In a previous study done in our hospital for elective inguinal hernia repair, a wound infection rate of 8.7% was observed [9]. The reasons for higher infection rate could be attributed to higher preoperative stay in the hospital and the choice of antibiotic. The median preoperative hospital stay was 9 days in patients with SSI and 4 days in patients without SSI. This aspect has not been considered in most of the studies done previously as there are higher chances of getting SSI due to prolonged hospital stay. The delay in surgery for our patients after hospital admission is multifactorial.
Patient related parameters and SSI
The mean age of patients in both the antibiotic group and placebo group was similar. The mean age in the infected group is 54.25 years and in the uninfected group is 49.5 years. The literature reveals no age-related changes in the rates of SSI’s in accordance to our study results [10].
ASA class of the patient is one of the important risk factors for post-operative SSI. In our study, majority of the patients were in class I and II. ASA grades III and IV have been clearly established as risk factors for SSI [10]. However, present study did not have any patient with ASA class IV and above.
BMI is an important risk factor for developing postoperative SSI [10]. In the present study there was no statistically significant change in BMI among the two groups. One study in the literature has previously established the need for prophylactic antibiotics in obese breast cancer patients requiring surgery [11]. In the current study, it was found that patients with a BMI greater than 25 kg/m2 had higher incidence of post-operative wound infection as compared to those with a BMI lower than 25 kg/m2 (21.1% Vs 16.7%). But there was no statistically significant difference.
Co morbid illness was not a statistically significant risk factor for SSI in our study. But the literature had clearly established diabetes mellitus and hypertension to be risk factors for SSI [10].
Patients who had received NACT are at risk of developing SSI [10]. In our study a total of 72 patients had received NACT of which 55 patients had SSI. The results of the present study were in concordance with previous studies in the literature [7,12-14].
Surgery related parameters and SSI
Duration of surgery is one of the significant predictors for SSI which is an integral component of the National Nosocomial Infections Surveillance (NNIS) system, where it reflects the surgery related component of the score. The present study did not find any significant change in rate of infection due to duration of surgery which had a bearing to grade of surgeon. This was in line with the literature [7].
Duration of hospital stay and SSI
It is a well-known fact that increased pre-operative hospital stay increased the risk of colonization with resistant bacteria [15,16]. An earlier study done in our institute showed that patients who stayed for more than 2 days in the hospital pre-operatively had significantly high bacterial counts in the skin than who stayed for less than 2 days [15].
On further analysis, a pre-operative stay of more than 2 days was found to be cut off period where the infection rates approached statistical significance. However, antibiotic prophylaxis did not have any significant impact on the rates of SSI when pre-operative stay was more.
None of the prior studies in the literature have investigated the aspect of preoperative stay in breast cancer surgery. The cause of increased preoperative stay in the current study can be attributed to reasons suited to our population only. They are because, our tertiary centre provides free surgical treatment to a large population. Also, there was need for optimizing diabetes and hypertension prior to surgery.
The median post-operative stay was also significant factor between those with SSI and without SSI. This difference was due to treatment of underlying SSI before discharging the patient. The difference in total stay mainly reflects the prolonged post-operative stay in the infected group. This issue of prolonged hospital stays, delay in discharge from hospital and hence delay in starting adjuvant treatment is a major concern in the setting of a malignancy such as carcinoma breast.
All our patients underwent pre-operative preparation of axilla, the day before the surgery, which has been recognized as a significant risk factor for SSI [17]. Recent literature suggests that clipping or shaving may not have any significant effect on SSI rates [18].
Implications of the study in our centre
The patients in general surgical ward in our hospital are subjected to a high risk of cross infection as we treat a wide spectrum of surgical conditions. Cefazolin was the antibiotic used in our study. It was chosen because of its proven efficacy against the common organisms like Staphylococcus aureus, longer duration of action and low cost [19]. But wound swabs taken post operatively from infected wounds showed the presence of gram negative organisms. This might also be a reason for the ineffectiveness of our chosen antibiotic.
Routine antibiotic prophylaxis targeting gram negative organisms is not commonly practiced. However, Yetim I et al. [20] had studied the effect of Gentamicin impregnated collagen sponge implants in patients undergoing modified radical mastectomy. They found that the group of patients who had received the Genta coll implants had significantly lower incidence of post-operative infection rate, seroma formation, drainage volume and decreased hospital stay.
With the high incidence of infection rates post operatively in our set up, though significant difference could not be established in the group which received antibiotic and, in the group which received placebo, it would be recommended to routinely use prophylactic antibiotics.
But the choice of antibiotic needs further study by conducting comparative studies between different types of antibiotics with inclusion of gram negative coverage. Also, the use of antibiotics could be restricted to groups with higher risk of infection like diabetics and in patients with higher BMI. Though there was no statistical significance it certainly has a clinical bearing. Also, there are studies which found that antibiotics used in suboptimal doses are as ineffective [10] and hence antibiotic dose to be calculated according to the weight, in patients with higher BMI as diabetes and obesity are most often coexistent.
In the present study, there was no statistical difference in the rate of infection between the antibiotic and the control group. There were higher rates of surgical site infection in diabetics, hypertensives and in obese patients. The patients who developed surgical site infection were found to have had a longer mean duration of pre-operative hospital stay. Even though there was no statistical difference in the rate of infection in the antibiotic group and the control group, due to the high rate of infection, role of prophylactic antibiotics cannot be ignored. But the choice of antibiotic needs to be investigated further. It is also recommended to consider antibiotic administration for patients at higher risk of developing surgical site infection.
- Xue DQ, Qian C, Yang L, Wang XF (2012) Risk factors for surgical site infections after breast surgery: a systematic review and meta-analysis. Eur J Surg Oncol 38: 375-381. [Crossref]
- Rodríguez-Caravaca G, de las Casas-Cámara G, Pita-López MJ, Robustillo-Rodela A, Díaz-Agero C, et al. (2011) [Preoperative preparation, antibiotic prophylaxis and surgical wound infection in breast surgery]. Enferm Infecc Microbiol Clin 29: 415-20. [Crossref]
- Lefebvre D, Penel N, Deberles MF, Fournier C (2000) [Incidence and surgical wound infection risk factors in breast cancer surgery]. Presse Med 29: 1927-1932. [Crossref]
- Platt R, Zucker JR, Zaleznik DF, Hopkins CC, Dellinger AW, et al. (1993) Perioperative antibiotic prophylaxis and wound infection following breast surgery. J Antimicrob Chemother 31: 43-48. [Crossref]
- Bold RJ, Mansfield PF, Berger DH, Pollock RE, Singletary SE, et al. (1998) Prospective, randomized, double-blind study of prophylactic antibiotics in axillary lymph node dissection. Am J Surg 176: 239-243. [Crossref]
- Hall JC, Hall JL (2004) The measurement of wound infection after breast surgery. Breast J 10: 412-415. [Crossref]
- Cabaluna ND, Uy GB, Galicia RM, Cortez SC, Yray MD, et al. (2013) A randomized, double-blinded placebo-controlled clinical trial of the routine use of preoperative antibiotic prophylaxis in modified radical mastectomy. World J Surg 37: 59-66. [Crossref]
- Bunn F, Jones DJ, Bell-Syer S (2012) Prophylactic antibiotics to prevent surgical site infection after breast cancer surgery. Cochrane Database Syst Rev 1: CD005360. [Crossref]
- Shankar VG, Srinivasan K, Sistla SC, Jagdish S (2010) Prophylactic antibiotics in open mesh repair of inguinal hernia - a randomized controlled trial. Int J Surg 8: 444-7. [Crossref]
- Olsen MA, Lefta M, Dietz JR, Brandt KE, Aft R, et al. (2008) Risk factors for surgical site infection after major breast operation. J Am Coll Surg 207: 326-335. [Crossref]
- Gulluoglu B, Guler S, Ugurlu U, Culha G (2013) Efficacy of prophylactic antibiotic administration for breast cancer surgery in overweight or obese patients: a randomized controlled trial. Ann Surg 257: 37-43. [Crossref]
- Forouhi P, Dixon JM, Leonard RCF, Chetty U (1995) Prospective randomized study of surgical morbidity following primary systemic therapy for breast cancer. Br J Surg 82: 79- 82. [Crossref]
- Danforth DN Jr, Lippman ME, McDonald H, Bader J, Egan E, et al. (1990) Effect of preoperative chemotherapy on mastectomy for locally advanced breast cancer. Am Surg 56: 6-11. [Crossref]
- Broadwater JR, Edwards MJ, Kuglen C, Hortobagyi GN, Ames FC, et al. (1991) Mastectomy following preoperative chemotherapy. Strict operative criteria control operative morbidity. Ann Surg 213: 126-129. [Crossref]
- Sistla SC, Prabhu G, Sistla S, Sadasivan J (2010) Minimizing wound contamination in a 'clean' surgery: comparison of chlorhexidine-ethanol and povidone-iodine. Chemotherapy 56: 261-7. [Crossref]
- Garibaldi RA, Cushing D, Lerer T (1991) Risk factors for postoperative infection. Am J Med 91: 158S-163S. [Crossref]
- Alexander JW, Fischer JE, Boyajian M, Palmquist J, Morris MJ (1983) The influence of hair-removal methods on wound infections. Arch Surg 118: 347-352. [Crossref]
- Tanner J, Woodings D, Moncaster K (2006) Preoperative hair removal to reduce surgical site infection. Cochrane Database Syst Rev 3: CD004122. [Crossref]
- (1992) ASHP therapeutic guidelines on antimicrobial prophylaxis in surgery. ASHP Commission on Therapeutics. Clin Pharm 11: 483-513. [Crossref]
- Yetim I, Ozkan OV, Dervişoglu A, Erzurumlu K, Canbolant E (2010) Effect of local gentamicin application on healing and wound infection in patients with modified radical mastectomy: A Prospective Randomized Study. J Int Med Res 38: 1442 – 1447. [Crossref]
- Paajanen H, Hermunen H (2009) Does preoperative core needle biopsy increase surgical site infections in breast cancer surgery? Randomized study of antibiotic prophylaxis. Surg Infect (Larchmt) 10: 317-321. [Crossref]
- Gupta R, Sinnett D, Carpenter R, Preece PE, Royle GT (2000) Antibiotic prophylaxis for post-operative wound infection in clean elective breast surgery. Eur J Surg Oncol 26: 363-366. [Crossref]
- Chow LW, Yuen KY, Woo PC, Wei WI (2000) Clarithromycin attenuates mastectomy-induced acute inflammatory response. Clin Diagn Lab Immunol 7: 925-931. [Crossref]
- Wagman LD, Tegtmeier B, Beatty JD, Kloth DD, Kokal WA, et al. (1990) A prospective, randomized double-blind study of the use of antibiotics at the time of mastectomy. Surg Gynecol Obstet 170: 12-16. [Crossref]

