The authors describe a patient with spontaneous vertebro-vertebral arteriovenous fistula (VVAVF) presenting with multiple episodes of recurrent embolic stroke. A 58-year-old man had developed aggravating neurological symptoms caused by eight episodes of posterior circulation stroke during period of three years. Many imaging studies and medical testing could not explain the cause of multiple recurrent strokes. Initial magnetic resonance imaging (MRI) of the brain showed multiple infarctions in right cerebellum and cerebellar peduncle. Follow-up MRI obtained 3 years after initial onset revealed multiple old infarctions in bilateral thalami, bilateral cerebellum, brainstem, and bilateral temporo-occipital lobes. MR angiography of the cervical spine disclosed an abnormal tubular-like lesion projected from posterolateral aspect of the proximal right V3 segment. There were irregularity and tortuosity of bilateral V1 and V2 segments. The digital subtraction angiography demonstrated the right VVAVF located at the level of C1-2, draining directly into deep cervical veins. To close the fistula, embolization with coiling was successfully performed under general anesthesia. Two years after the endovascular treatment, the right vertebral angiography confirmed complete obliteration of the fistula. The patient has gradually recovered and could get back to the activities of daily living at home. During a follow-up period of 3 years, the patient had no further recurrent embolic events.
spontaneous, vertebro-vertebral arteriovenous fistula, vertebral artery, recurrent embolic stroke, thrombosis
Vertebro-vertebral arteriovenous fistulas (VVAVFs) are abnormal connections between the extracranial vertebral artery (VA) or its branches and neighboring veins including paravertebral veins, epidural venous plexus, internal jugular vein, and/or perimedullary veins [1,2]. They are uncommon lesions and can be categorized into traumatic, iatrogenic, and spontaneous cause [3]. Spontaneous VVAVFs have been associated with fibromuscular dysplasia (FMD), Neurofibromatosis Type 1 (NF1), and Ehlers-Danlos syndrome (EDS) [4-7]. Spontaneous fistulas usually occur at the level between C1 and C2. The common presenting symptoms include bruit, pain, radiculopathy, and/or myelopathy [3]. Ischemic or embolic stroke caused by VVAVF is extremely rare [8-12]. We describe a patient with spontaneous VVAVF manifesting with multiple recurrent ischemic strokes during a period of 3 years, resulting in worsening neurological symptoms. We also review the literature of patients having VVAVFs presenting with ischemic or embolic stroke.
A 58- year-old man with a medical history of hypertension, diabetes mellitus, and dyslipidemia, was admitted to the local hospital due to sudden onset of vertigo, ataxia, and diplopia. Previous medication included amlodipine 10 mg, metformin 500 mg, and simvastatin 20 mg once daily. There was no history of trauma. Computed tomography (CT) scan and magnetic resonance imaging (MRI) of the brain obtained the same day showed multiple infarctions in right cerebellum and cerebellar peduncle (Figure 1). Clopidogrel 75 mg once daily was given to him. With fully recovery, he was discharged home one week later. After first attack, the patient suffered from another 7 episodes of stroke in the last 3 years before transferring to our institute. Every episode, he was brought to multiple hospitals, and obtained CT, MRI, and/or magnetic resonance angiography (MRA) of the brain and neck. All hospitals reported cerebral infarction in posterior circulation territory without occlusion of extracranial and intracranial vessels. Despite changing different types of antiplatelet or even trying to give double antiplatelet together with strict control of stroke risk factors was attempted during this period, episodes of acute neurological deficit still occurred. Finally, recurrent ischemic stroke had prevented with clopidogrel 75 mg and aspirin 325 mg once daily. Serologic evaluation, thrombophilia screen or coagulation studies (i.e., protein C, protein S, antithrombin III, anticardiolipin antibodies), duplex ultrasonography of carotid and vertebral arteries, electrocardiography including 24-hour Holter monitoring, and transthoracic echocardiography were done which all showed unremarkable to explain the cause of frequent recurrent cerebral infarctions. Following multiple recurrent stroke, the patient developed aggravating neurological symptoms, including ptosis, dysarthria, dysphagia, right hemiparesis, right arm numbness, and the worst quadriparesis. These problems likely occurred together and some of them resolved almost completely in a few weeks to a month. Few months before transferring, his daughter noticed that the patient gradually developed cognitive decline and was unable to remember people’s names, places and often lost the way in his house. Sometimes he reported visual hallucinations. Furthermore, she also noticed that his speaking is rather slower than usual. His activities of daily living had deteriorated and need partial support.
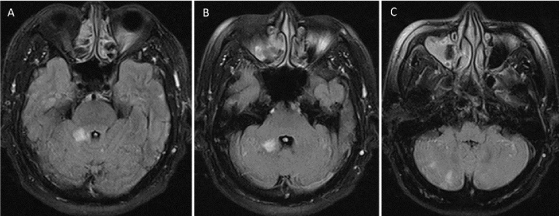
Figure 1. Magnetic resonance imaging (MRI) of the brain obtained after initial onset. Sequential images of axial fluid-attenuated inversion recovery (FLAIR) MRI at the level of pons (A), cerebellar peduncle (B), and medulla (C) shows multiple hyperintensities in the right side of cerebellum, representing of multiple infarctions of the posterior circulation
The patient was transferred to Prasat Neurological Institute for further investigation and proper treatment. On physical examination, there was no pulpable thrill or loud bruit over both sides of neck. No abnormal skin lesions were detected. The patient had never complained about audible bruit. On ophthalmic examination, the right eye had ptosis, and limited medial eye movement. His pupils were equal and respond to light normally. Intraocular pressure and visual acuity were in normal limit. Visual field could not evaluate due to uncooperating of the patient. The neurological examination revealed right ptosis, limited medial eye movement of the right eye, left-sided facial weakness, spastic dysarthria, right hemiparesis (power grade 4/5), decreased pinprick sensation of right arm, dysmetria, and a positive Babinski reflex in both feet. He had impaired recent memory.
All previous imaging studies were reviewed and found that multiple recent infarctions had occurred on several areas in different time during period of 3 years. These infarcts involved bilateral thalami, midbrain, pons, left cerebellum, and bilateral medial temporo-occipital lobes. In our institute, MRI of the brain obtained 3 years after initial onset revealed multiple old infarctions in bilateral thalami, bilateral cerebellum, brainstem, and bilateral temporo-occipital lobes. There were encephalomalacic changes of bilateral occipital lobes. Susceptibility weighted imaging (SWI) and T2*-weighted gradient-recalled echo (GRE) image demonstrated evidence of old hemorrhagic transformations (Figure 2). Maximum intensity projection from 3D time-of-flight MRA of the cervical spine also showed an abnormal tubular-like lesion projected from posterolateral aspect of the right V3 segment between the level of C1 and C2. Also, there were irregularity and tortuosity of bilateral V1 and V2 segments (Figure 3A). The digital subtraction angiography (DSA) was further investigated and demonstrated the right VVAVF located at the level of C1-2 and drained directly into deep cervical veins (Figure 3B and 3C).
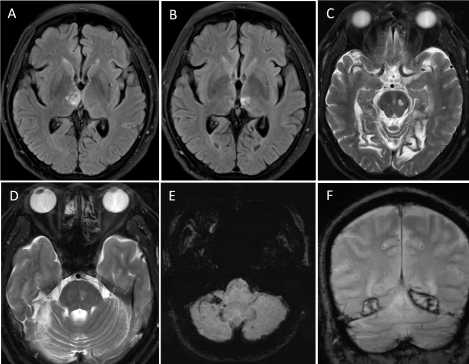
Figure 2. Follow-up magnetic resonance imaging (MRI) of the brain obtained 3 years after initial onset. Sequential images of axial fluid-attenuated inversion recovery (FLAIR) MRI at the upper (A) and lower (B) level of the brain reveal bilateral thalamic infarcts. Sequential images of axial T2-weighted MRI at the level of midbrain (C) and pons (D) also disclose multiple infarctions in brainstem and right cerebellum. There are encephalomalacic changes of bilateral occipital lobes. Axial susceptibility weighted imaging (SWI) (E) and coronal T2*-weighted gradient-recalled echo (GRE) image (F) show evidence of old hemorrhagic transformations
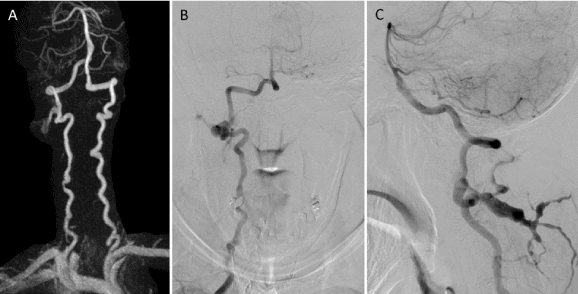
Figure 3. Anteroposterior view of maximum intensity projection from 3D time-of-flight magnetic resonance angiography of the neck (A) shows an abnormal tubular-like lesion projected from posterolateral aspect of the right V3 segment. There are irregularity and tortuosity of bilateral V1 and V2 segments. Anteroposterior (B) and lateral (C) views of the right vertebral artery injection demonstrate vertebro-vertebral arteriovenous fistula at the level of C1-2, draining early into deep cervical veins.
From consensus of multidisciplinary team conference, surgical treatment was the best option due to possibility of difficult in navigating the microcatheter through tortuous and irregular arterial course. Interestingly, intraoperative finding disclosed the thrombus located within draining venous plexus. Intraoperative ultrasound disclosed absent flow of this venous plexus. Closure of the fistula with surgical clip and resection of thrombosed venous plexus were performed under indocyanine green fluorescence imaging. Pathological examination confirmed organizing thrombosis within vessels (Figure 4). One month after operation, follow-up angiography demonstrated that the right VVAVF had still remained. Then, the patient was scheduled for endovascular treatment few weeks later. Under general anesthesia, a Prowler plus (Cordis, Miami Lakes, Fla) microcatheter and Agility® (Codman Neurovascular, Raynham, MA) 0.014-inch soft microwire were difficultly navigated into the draining vein via the right tortuous vertebral artery. Subsequently, nearly complete obliteration of the fistula was successfully done with using a combination of Axium™ coils (ev3, Irvine, CA, USA) and fibered coils (InterlockTM-35, Boston Scientific, Natick, MA) under angiographic road-mapping (Figure 5).
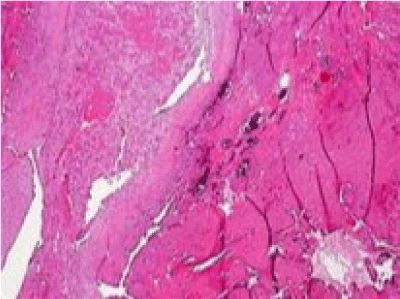
Figure 4. microscopic examination of surgical tissue shows arterial vascular wall containing organizing thrombus, characterized by fibrinous materials and proliferative fibroblasts. The adjacent venous vessels are mildly thickened
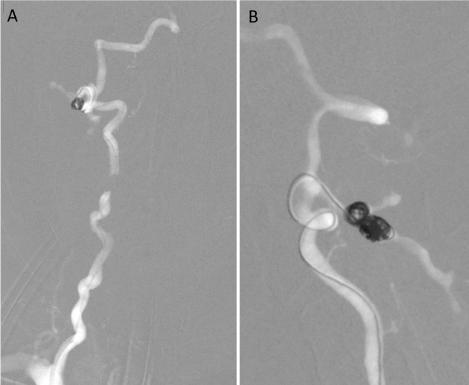
Figure 5. Anteroposterior (A) and lateral (B) views of the right vertebral artery injection during angiographic road-mapping demonstrate the microcatheter placement with coil embolization into the deep cervical veins
After embolization, the patient has gradually recovered and could get back to the activities of daily living at home. Two years after the endovascular treatment, the right vertebral angiography confirmed complete obliteration of the fistula (Figure 6). During a follow-up period of 3 years, the patient had no further recurrent embolic events and was placed only 81 mg of aspirin once daily. There were no new lesions at the follow-up imaging studies. However, his impairment of recent memory has still persisted. He was diagnosed as vascular dementia and donepezil 5 mg per day has been continued for this symptom.
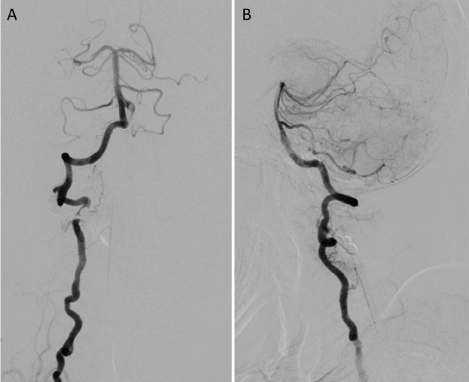
Figure 6. Anteroposterior (A) and lateral (B) of the right vertebral artery injection obtained 2 years after the endovascular treatment with coils confirm nearly complete obliteration of the fistula AVF
Based on the TOAST (Trial of Org 10172 in Acute Stroke Treatment) classification system [13], acute ischemic stroke was subtyped into 5 categories, including large-artery atherosclerosis, cardioembolism, small-vessel occlusion, stroke of other determined etiology, and stroke of undetermined etiology. In the present study, recurrent ischemic strokes in our case had occurred in multiple vascular territories, suggestive of a clinical diagnosis of embolic strokes. Under extensive evaluation, our patient fulfilled the diagnostic criteria for cryptogenic stroke or embolic stroke of undetermined source (ESUS), including non-lacunar stroke on neurological imaging, no arterial stenosis more than 50% or occlusion in a corresponding large artery, lack of major cardioembolic source, and lack of other determined stroke causes [14]. About 17% of patients with ischemic stroke met criteria for ESUS, and recurrent stroke rate is 4.7%. [15]. To date, standard medical treatment of ESUS consists of antiplatelet drugs and statins [16]. Despite the use of dual antiplatelet therapy, the patient had still suffered from multiple recurrent ischemic strokes. The patient was then transferred to our institute for second opinion and further possible investigation. The affected brain lesions, including bilateral cerebellum, bilateral thalami, temporal, occipital lobes, and pons, corresponded with the territories of bilateral posterior inferior cerebellar artery, posterior cerebral artery, and basilar perforators, representing posterior circulation strokes. Fortunately, spontaneous VVAVF was suspected in our patient after reviewing of all imaging studies,and confirmed by DSA. It is the extremely rare cause of recurrent embolic stroke. Then, our case should be classified in stroke of other determined etiology.
We reviewed the literature of VVAVFs manifesting as ischemic or embolic stroke, and found 8 patients, including our present case, with 9 fistulas due to bilateral lesions in one case (Table 1) [4,8-12]. There were 4 males, 3 females, and 1 unknown gender with median age of 49 years, ranging from 9 to 60 years. Out of 9 fistulas, 4 were spontaneous cause, 3 iatrogenic cause, and 2 traumatic cause from a gunshot wound. The fistulas were located at V3 segments of the VA in 5 fistulas, V2 segments in 3, and V1 segment in only 1. Symptoms and signs were variable depending on affected brain regions of each vascular territory. Two patients also had cervical myelopathy secondary to compressive engorged draining veins. All except one fistula were successfully treated by endovascular treatment. One fistula spontaneously regressed without treatment. Preservation of parent artery was achieved in 2 patients. All patients had no recurrent stroke or further neurologic signs or symptoms after treatment.
Table 1. Literature review of vertebral arteriovenous fistulas manifesting as ischemic or embolic stroke
Authors |
Gender/Age |
Cause |
Fistula Side |
Fistula level
(segment) |
Symptoms and signs |
Treatment |
Recurrent
Stroke
after treatment |
O'Shaughnessy [8] |
M/23 |
Trauma |
R |
V3 |
Depression of consciousness |
Endovascular treatment with coils**. |
No |
Crowley [9] |
M/22 |
Trauma |
L |
V2 |
Quadriplegia, severe headache, dizziness, syncope, Right-sided homonymous hemianopia |
Endovascular treatment with coils and vascular plugs**. |
No |
Adams [10] |
M/9 |
Iatrogenic* |
R |
V1 |
Right-sided homonymous hemianopia |
Spontaneous regression |
No |
Jang [12] |
F/57 |
Iatrogenic |
L |
V3 |
Dysarthria, right facial palsy, drowsiness |
Endovascular treatment with coils**. |
No |
|
F/45 |
Iatrogenic |
L |
V3 |
Pulsatile tinnitus, vertigo, nausea, dysarthria, muscle weakness |
Endovascular treatment with coils**. |
No |
John [11] |
N/A/60 |
Spontaneous* |
L |
V3 |
Acute onset vertigo, ataxia, cervical myelopathy |
Endovascular treatment with coils-assisted Onyx. |
No |
Iampreechakul [4] |
F/53 |
Spontaneous |
Bilateral |
V2 |
Progressive cervical myelopathy following diagnosis of acute ischemic stroke for 2 years. |
Endovascular treatment with coils**. |
No |
Present study |
M/58 |
Spontaneous* |
R |
V3 |
Dysmetria, muscle weakness, dysarthria, dysphagia, ptosis, cognitive impairment |
Endovascular treatment with coils following unsuccessful surgery. |
No |
F: female; M: male; L: left; R: right; V: vertebral artery; N/A: not applicable; *: low-flow arteriovenous fistula; **: parent artery sacrifice
O'Shaughnessy, et al. [8] reported a 23-year -old man with the right traumatic VVAVF and pseudoaneurysm at the level of C1 following a gunshot wound. CT scan of the brain revealed a right cerebellar infarction. They postulated that distal thromboembolism may arise from the pseudoaneurysm lumen. Obliteration of the pseudoaneurysm and fistula with parent artery sacrifice was successfully performed with coil embolization. With the same cause, Crowley, et al. [9] reported a 22-year-old man with the left traumatic high-flow VVAVF at the level of C6. Delayed ischemic stroke occurred approximately 2 months after his injury. The patient experienced a severe headache, dizziness, and eventually progressed to syncope. In addition, he developed a right-sided homonymous hemianopia. MRI showed an acute left-sided occipital infarction. The involved segment of the VA was successfully sacrificed with a combination of platinum coils and vascular plugs.
Due to iatrogenic cause, Adams, et al. [10] reported a 9-year-old boy with von Hippel-Lindau syndrome developed a right-sided homonymous hemianopia caused by right VVAVF at V1 segment from attempted central venous catheterization. MRI revealed the presence of a left-sided occipital infarction. Complete spontaneous regression occurred without interventional treatment. We previously reviewed the literature of spontaneous obliteration of VVAVFs and found 12 cases, including this boy. The mechanisms of spontaneous regression or closure of VVAVFs were discussed in the previous study [5].
Also, Jang, et al. [12] reported 2 patients with iatrogenic high-flow VVAVFs following C1 screw insertion. The fistulas were located adjacent to C1 screws, i.e. V3 segment. First patient, a 57-year-old woman presented with an abrupt and severe nuchal pain with blurred vision, dysarthria, right facial palsy, and drowsy consciousness. The diffusion MRI disclosed a multifocal acute infarction on bilateral cerebellum and occipital lobes. The other patient, a 45-year-old woman presented with pulsatile tinnitus, vertigo, nausea, dysarthria, and a subjective weakness and numbness of extremities. Both patients were successfully treated by sacrifice of the involved VA using endovascular coil embolization.
Recently, we previously reported a 53-year-old woman with bilateral spontaneous VVAVFs associated with FMD presenting with progressive cervical myelopathy following diagnosis of ischemic stroke for 2 years. [4] However, stroke in this case was supratentorial stroke, probably related to dysplastic changes of the internal carotid artery.
Similar to the present study, John, et al. [11] reported a 60-year-old patient with spontaneous VVAVF at the left V3 segment presenting with acute ischemic stroke in left cerebellum and concomitant findings of multiple old strokes producing encephalomalacia caused by multiple prior embolic events. DSA showed an ectatic left V3 segment with pseudoaneurysm and slow drainage into the left suboccipital plexus and into epidural vein within the spinal canal causing cord compression. They postulated that slow flow into the venous outlet may have resulted in reflux of venous clot. The degree of encephalomalacia in the left cerebellum was an indication that the patient had been having multiple embolic strokes from the VVAVF for a long time. The fistula was successful treated by coil-assisted Onyx embolization. In our case, encephalomalacic changes of bilateral occipital lobes represented long-run course of recurrent multiple embolic strokes from the fistula for 3 years. In addition, VVAVF in the present study may be low-flow lesion due to no bruit detected on routine physical examination and the absence of flow from intraoperative ultrasound. According to intraoperative findings and pathological examination, we concluded that the VVAVF was the source of embolic strokes resulting from thrombus formation in the fistula probably having abnormal flow pattern.
The ideal goal of the treatment of the VVAVF is the occlusion of the fistula and preservation of the patency of the VA. Nevertheless, preservation of the parent artery is often not possible but well tolerated [7]. From our review, most fistulas were treated by obliteration of the fistula and parent artery sacrifice without any complications. Interestingly, parent artery preservation was achieved in 2 VVAVFs defined as low-flow fistula, including our case. Recently, V3 segment VVAVF was successfully treated using an intracranial covered stent for preservation of the VA [17]. For our patient, however, it is difficult to navigate the stent through irregularity and tortuosity of the vertebral artery. Clearly, obliteration of VVAVF can terminate further recurrent thromboembolic events in all patients having VVAVFs manifesting with embolic stroke in our review.
We describe a case of multiple recurrent thromboembolic strokes in a patient with low-flow spontaneous VVAVF. Delayed diagnosis of this source of embolic strokes resulted in worsening neurological symptoms. Obliteration of the fistula by endovascular treatment can reduce further recurrent stroke in a long-term follow-up.
The patient has given consent to be enrolled and has his data published.
Nil
There are no conflicts of interest.
- Halbach VV, Higashida RT, Hieshima GB (1988) Treatment of vertebral arteriovenous fistulas. AJR Am J Roentgenol 150: 405-412. [Crossref]
- Beaujeux RL, Reizine DC, Casasco A, Aymard A, Rüfenacht D, et al. (1992) Endovascular treatment of vertebral arteriovenous fistula. Radiology 183: 361–367. [Crossref]
- Aljobeh A, Sorenson TJ, Bortolotti C, Cloft H, Lanzino G. (2019) Vertebral Arteriovenous Fistula: A Review Article. World Neurosurg 122: e1388-e1397. [Crossref]
- Iampreechakul P, Liengudom A, Wangtanaphat K, Lertbutsayanukul P, Wattanasen Y, et al. (2018) Progressive Cervical Myelopathy Caused by Bilateral Spontaneous High-Flow Vertebro-Vertebral Arteriovenous Fistulas Associated with Fibromuscular Dysplasia Successfully Treated by Endovascular V2 Segments Sacrifice Using Fibered Coils: A Case Report. Clin Med Rev Case Rep 5: 1-12.
- Iampreechakul P, Siriwimonmas S. (2016) Spontaneous obliteration of spontaneous vertebral arteriovenous fistula associated with fibromuscular dysplasia after partial surgery: A case report. Interv Neuroradiol 22: 717-727. [Crossref]
- Pereira VM, Geiprasert S, Krings T, Caldas JG, Toulgoat F, et al. (2007) Extracranial vertebral artery involvement in neurofibromatosis type I. Report of four cases and literature review. Interv Neuroradiol 13: 315-328. [Crossref]
- Goyal M, Willinsky R, Montanera W, Terbrugge K. (1999) Spontaneous vertebrovertebral arteriovenous fistulae clinical features, angioarchitecture and management of twelve patients. Interv Neuroradiol 5: 219-224. [Crossref]
- O'Shaughnessy BA, Bendok BR, Parkinson RJ, Shaibani A, Batjer HH. (2005) Transarterial coil embolization of a high-flow vertebrojugular fistula due to penetrating craniocervical trauma: case report. Surg Neurol 64: 335-340. [Crossref]
- Crowley RW, Medel R, Dumont AS. (2009) Traumatic high flow vertebral-venous fistula presenting with delayed ischemic stroke: endovascular management with detachable coils and Amplatzer Vascular Plugs. Neurosurg Focus 26: 1-4. [Crossref]
- Adams A, Allouni K, Basheer S, Evanson J, Mankad K. (2013) Case report: spontaneous resolution of an established iatrogenic vertebral arteriovenous fistula. J Child Neurol 28: 255-258. [Crossref]
- John S, Jaffari N, Lu M, Hussain MS, Hui F. (2014) Spontaneous vertebral arteriovenous fistula causing cervical myelopathy and acute ischemic strokes treated by endovascular balloon-assisted coiling and Onyx embolization. J Clin Neurosci 21: 167-170. [Crossref]
- Jang HJ, Oh SY, Shim YS, Yoon SH. (2014) Endovascular treatment of symptomatic high-flow vertebral arteriovenous fistula as a complication after C1 screw insertion. J Korean Neurosurg Soc 56: 348-352. [Crossref]
- Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, et al. (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of Org 10172 in Acute Stroke Treatment. Stroke 24: 35-41. [Crossref]
- Hart RG, Diener HC, Coutts SB, Easton JD, Granger CB, et al. (2014) Cryptogenic Stroke/ESUS International Working Group. Embolic strokes of undetermined source: the case for a new clinical construct. Lancet Neurol 13: 429-438. [Crossref]
- Hart RG, Catanese L, Perera KS, Ntaios G, Connolly SJ (2017) Embolic Stroke of Undetermined Source: A Systematic Review and Clinical Update. Stroke 48: 867-872. [Crossref]
- Geisler T, Mengel A, Ziemann U, Poli S. (2018) Management of Embolic Stroke of Undetermined Source (ESUS). Drugs 78: 823-831. [Crossref]
- Geng J, Hu P, Ma Y, Zhang P, Zhang H (2019) Endovascular treatment of V3 segment vertebro-vertebral arteriovenous fistula with Willis covered stent: Case report and literature review. Interv Neuroradiol 25: 97-101. [Crossref]






