Living with cancer is associated with significant psychological strain. The prevalence and severity of this distress varies according to the time, type, and stage of cancer, as well as other variables including treatment regimen, side effects, and prognosis. More often than not, these struggles are neglected as part of the traditional cancer care plan. Yet, if left unaddressed, emotional strain can add to the suffering caused by cancer by negatively affecting treatment compliance. Faith communities, such as churches, provide an ideal atmosphere to serve and support individuals battling cancer. However, research indicates that spiritual care is often a neglected component in cancer care. Therefore, the purpose of this investigation was to describe felt needs of current cancer patients, availability of psychological services within religious settings, and the capacity of pastors to provide emotional support to cancer patients. Our investigation showed that the majority of church leaders recognize this need and desire training in this particular area. Therefore, a need for an effective church-equipping program is evident and should be a priority of cancer care providers.
cancer, care providers, religious settings
This year there are expected to be more than 1.6 million new cancer cases in the United States [1]. Advances in early detection and treatment have increased the 5-year survival rates for the most common forms of cancer to approximately 64%, up from 43% just two decades ago [2]. This means that more people are living as cancer survivors than at any other point in history. In fact, the Centers for Disease Control now label cancer as a chronic disease [3], rather than a terminal illness.
Living with cancer is associated with significant psychological strain. Depression and anxiety [4,5], as well as symptoms of post-traumatic stress disorder [6] are very common in cancer survivors. The prevalence and severity of this distress varies according to the time, type, and stage of cancer, as well as other variables including treatment regimen, side effects, and prognosis [7]. Psychological distress often interferes with an individual’s quality of life [8], and can even lead to premature death in caregivers [9]. Typically, psychological distress contributes to impaired social functioning [8], sleep difficulties [10], fatigue, and pain [11]. Even if a patient is not experiencing clinically significant symptoms, they are still likely to experience emotional distress in the form of worry, fear, loss of control, anger, guilt, sadness, confusion, mood disturbance, and anxiety [12]. Moreover, a cancer diagnosis often brings about spiritual struggle of faith, as the patient examines their own mortality, as well as their relationship with God [13]. In fact, spirituality was identified as a core domain for quality of life in cancer patients [14], and if left unmet, may interfere with a patient’s ability to cope with their illness [15].
However, more often than not, these struggles are neglected as part of the traditional cancer care plan [16]. Studies indicate that oncologists tend to underestimate the psychological distress their patients experience [17]. Additionally, patients report a lack of communication about their psychosocial needs with their health care providers [18]. In fact, a National Survey of US Households Affected by Cancer reported that 28% of patients felt they did not have a doctor who paid attention to factors beyond their direct medical care [19].
If left unaddressed, emotional strain can add to the suffering caused by cancer by negatively affecting treatment compliance [13] and exacerbating illness and other chronic conditions. Faith communities, such as churches, provide an ideal atmosphere to serve and support individuals battling cancer. This is not a new concept, as the link between religion and medicine date back to ancient cultures. Jesus Christ, whom the Christian church holds as its founder, instructed His followers to heal the sick. As such, the Christian emphasis on charity is what gave rise to many of the modern-day hospitals we know today. In fact, the Pontifical Council for the Pastoral Care of Health Care Workers reports that the church manages one-third of the world’s health care facilities [20]. However, research indicates that spiritual care is often a neglected component in cancer care [21]. Recognizing this impact of emotional strain of suffering caused by cancer, the purpose of this investigation was to describe felt needs of current cancer patients, as well as the availability of psychological services within religious settings. In addition, we analyzed the capacity of pastors to provide emotional support to cancer patients, and created an action plan to overcome the barriers to support, as identified in the pastoral survey.
Data collection: Data collection took place over three phases. The first phase involved a focus group with 15 patients of Maple Tree Cancer Alliance, a non-profit organization in Dayton, Ohio, which provides free exercise training, nutrition counseling, and spiritual support to individuals battling cancer. Focus groups have been shown to provide broader insights to how people perceive a particular problem [22]. Patients were eligible to participate if they were 18 years of age or older and receiving care at Maple Tree Cancer Alliance. Informed consent was obtained from all participants prior to their participation.
The focus group took place at the Life Enrichment Center in Dayton, Ohio. The goal of the focus group was to determine the spiritual needs of cancer patients, and the current ability of the church to meet their needs. The following questions were used to elicit these beliefs:
- What surprised you about your cancer journey?
- Was anything easier than you thought it would be?
- What was the most difficult part of your journey?
- How were you able to overcome these difficulties?
- Tell me about your support network.
- Are you currently a member of/attending church on a regular basis?
- Would you consider your church/faith to play a major role impacting your ability to cope with cancer? Why/why not?
Phase two involved an analysis of evangelical Christian churches in and around the Dayton Area. A total of 69 churches identify themselves as “Christian” in Dayton. For each church, data regarding their doctrine statement, contact information, and support services were collected using each church website and phone calls to church staff. In addition, a note as to whether or not the church provided support specific to cancer patients was made, as well as the type of support, when applicable.
Phase three involved pastoral interviews and surveys. Direct recruitment approach was used to recruit pastors. Response rate was 91%. Participants who declined cited lack of interest as the reason. Thirty-six local pastors were given a survey designed by the research team to measure barriers to providing cancer support through their church. The questions asked in these survey were written in English, and were as follows:
- What is your role in the church?
- How long have you been working in ministry?
- Does your church currently have an outreach for cancer patients? If yes, please describe.
- On a scale of 1 to 5, with 1 being you have zero confidence in your knowledge of cancer, 3 being average confidence, and 5 being you feel very confident in your cancer knowledge, How do you feel your level of knowledge is regarding cancer? What areas are you strong? Where do you feel you are weak?
- What questions do you have regarding cancer? Where do you feel you need support?
- If given the opportunity, do you think your church would be interested in equipping materials or trainings to better serve cancer patients and their caregivers? What would you be most interested in?
Data analysis: Data included written notes and audio recording from the focus group. The recording was transcribed verbatim. Translated scripts were read alongside the original recording to confirm accuracy. Initial analysis determined the descriptive characteristics of the patients who participated in the focus group. The needs and availability of patient support services determined from the focus group were summarized. Scores from the pastoral survey were averaged and summarized. Results from each of the three phases of data collection were used to develop an action plan to meet patient need and overcome the barriers to support.
Phase one-focus group: Of the 15 focus group participants, 60% were women. A breakdown of their demographic and cancer information is in Table 1.
Table 1. Focus group subject characteristics
Gender |
Male |
6 |
Female |
9 |
Age |
58 ± 4.3 years |
Length of time in treatment |
16 ± 3.4 months |
Type of Cancer |
Breast |
7 |
Prostate |
1 |
Colon |
3 |
Lung |
1 |
Other |
3 |
Each respondent reported something different with regards to surprises during their cancer journey. One 48-year-old woman said she was surprised at the financial cost of cancer, explaining that she had to take a medicine for neuropathy that cost her $100 per pill. Another respondent reported that chemotherapy was easier than she expected, reporting that she kept “waiting to get sick”, but never did. On the contrary, several other individuals in the focus group reported that chemotherapy was “worse than they expected”. One 62-year-old male reported that the care he received from the physicians and nurses was very good. He explained that an oncology nurse held his hand and prayed with him on several occasions. Others in the group agreed. Several others noted that their oncologists spent more time with them than they expected – some up to three hours a visit.
When asked what was easy about their journey, we received mixed responses. The woman identified above restated that her chemotherapy treatment was not as bad as she expected. Others said finding resources to help educate them and handle treatment-related side effects were almost so easy that it overwhelmed them. One 42-year-old female participant explained that at her “chemo class” (which was a class she took soon after her diagnosis to learn the facts about her cancer, treatment plan, and resources available to her), she received so much information that she tucked it all away and couldn’t even bring herself to look at the material for the first 6 months of treatment.
Everyone in the focus group agreed that worry was the most difficult part of their journey. All said they were afraid they were going to die. Several respondents were mothers and said they worried about their children. One 59-year-old female said she didn’t feel like she was “done being a mom yet”. In addition, two males said that surgery was more painful than they expected.
The support networks varied. One 71-year-old male reported having little family and friends around to help him. On the contrary, the 42-year-old female patient said she had so many offers to help her out that she stopped responding to texts and emails.
When asked how they were able to overcome the difficulties, responses were mixed. A 62-year-old female said that the cancer diagnosis made her turn to her faith. She explained that she used to have doubts about God, but now had a feeling of peace about her diagnosis. She attributed her feeling of peace to a relationship with God. However, when asked the follow-up question regarding her church membership, she quickly said she didn’t attend church, because when she received her diagnosis (stage IV, colon cancer), her pastor did not call her. Of the fifteen participants in the focus group, two individuals reported feeling supported by her church. The remainder were not attending church (n=4), or not receiving emotional support by their church leaders (n=9). The nine patients who were not being supported by the church reported that they continued to go to church because they wanted to live, because of the social atmosphere, to help them maintain a good attitude, and because they wanted to keep their faith strong.
Phase 2-church assessment: A total of 69 Protestant/Evangelical Christian churches in and around the City of Dayton were analyzed. Of these 69 churches, one church had an outreach program specifically for cancer patients. One offered a bereavement ministry, three offered fitness and running groups, and three offered a health and wellness ministry. In addition, one church said they worked closely with the American Cancer Society by participating in the Relay for Life each year.
Phase 3-pastoral surveys: A total of 36 pastors were asked to complete a survey to identify barriers to providing cancer support through their church. The surveyed pastors identified themselves as either senior or associate pastor of their respective church, and had been in ministry for an average of 19.36 years. None of the pastors who completed the survey had an outreach for cancer patients at their church. Figure 1 presents a summary of the pastors’ reported cancer knowledge on a scale of 1 to 5. The average rating was 2.37, which indicated that, in general, pastors reported a lower than average understanding of cancer. This was identified as the number one barrier preventing pastors from addressing cancer concerns with members of their respective churches.
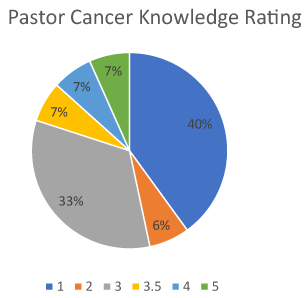
Figure 1. Average cancer knowledge ratings of senior and associate pastors (N=36)
Seventy-three percent of the pastors who were surveyed said they would like specialized training on providing support groups for cancer patients, as well as their caregivers. Additional areas of interest for specialized cancer training included dealing with suffering, cancer prevention, alternative treatments, medical options and biblical integration, and equipping. Ninety-seven percent of the surveyed pastors said they would be interested in receiving equipping materials or trainings to help them better serve cancer patients.
Emotional strain can be a devastating effect of cancer. Lack of support can interfere with an individual’s quality of life [8] through impairments in social functioning [8], sleep difficulties [10], fatigue, pain [11] and premature death [9]. The church provides an ideal setting to serve and support individuals battling cancer, however presently, they often overlook the needs of cancer patients [21]. Therefore, the purpose of this investigation was to describe the felt needs of cancer patients, assess current psychological services within religious settings for cancer patients, and measure the capacity of pastors to provide emotional support to cancer patients.
Experiencing a life-threatening medical diagnos2021 Copyright OAT. All rights reservfact, approximately 43% of cancer survivors experience significant psychological stress, meeting criteria for clinical diagnoses such as depression, anxiety, and adjustment disorders [4,5]. An even higher percentage of patients who do not develop clinical syndromes experience worry, fear, and anxiety, causing them significant distress [12]. Moreover, cancer can drastically test a patient’s faith and perceived relationship with God, as they are left to face the reality and possibility of death. According to the National Cancer Institute, these feelings lead patients to feelings of anger, isolation, and lower self-esteem [13]. However, 87% of the participants in our focus group reported feeling a lack of support from religious clergy. This is further supported by our finding that 98.5% of Christian evangelical churches in the City of Dayton do not have an outreach for cancer survivors. This points to a significant unmet need in the religious community.
One possible explanation for this lack of outreach for cancer patients is the gap in understanding of the unique features of cancer. Our survey of seasoned pastoral leaders revealed that they had a lower than average cancer knowledge. This finding is in line with previous studies, which found that overall public knowledge of cancer is poor [23,24]. Yet, an encouraging 73% of church leaders in the present study indicated that they would be interested in trainings to increase their knowledge. This led our research team to develop an action plan with recommendations for increasing knowledge and outreach for cancer patients in a religious setting.
Recommendation-improved knowledge: Experts in cancer care should create and lead a standardized training to increase general cancer knowledge with regards to the unique features of cancer from a spiritual perspective. Topics to be addressed should include: suffering, terminal disease, remission, pediatric cancer, and caregiver stress.
Recommendation-method of delivery: This training should be made available to church leaders and lay ministry personnel through an online portal. An expert in cancer care should be made available to address questions and changes in cancer care that may arise.
Recommendation-program deliverables: This training should culminate in a certificate of endorsement whereby attendees are qualified to implement and lead a cancer support ministry within their own church body. Curriculum materials and support should be made available to each endorsed trainee.
The reach and devastation of cancer is widespread. Traditionally, cancer care has focused heavily on the physiological symptoms of cancer [16]. However, if left unaddressed, emotional strain of cancer can add to suffering by negatively affecting treatment compliance [13] and interfering with a patient’s quality of life. The church provides an ideal atmosphere to support the unique needs of cancer patients. Our investigation showed that the majority of church leaders recognize this need and desire training in this particular area. Therefore, a need for an effective church equipping program is evident and should be a priority of cancer care providers.
- American Cancer Society, Facts and Figures, 2016.
- Jemal A, Clegg LX, Ward E, Ries LAG, Wu X, et al. (2004) Annual report to the nation on the status of cancer, 1975-2001, with special feature regarding survival. Cancer 101: 3-27. [Crossref]
- Chronic Disease Prevention and Health Promotion. Date of Access: April 7, 2017. https://www.cdc.gov/chronicdisease/
- Carlsen K, Jensen AB, Jacobsen E, Krasnik M, Johansen C (2005) Psychosocial aspects of lung cancer. Lung Cancer 47: 293-300. [Crossref]
- Hegel MT, Moore CP, Collins ED, Kearing S, Gillock KL, et al. (2006) Distress, psychiatric syndromes, and impairment of function in women with newly diagnosed breast cancer. Cancer 107: 2924-2931. [Crossref]
- Kangas M, Henry J, Bryant R (2002) Posttraumatic stress disorder following cancer. A conceptual and empirical review. Clin Psychol Rev 22: 499-524. [Crossref]
- Zabora J, BrintzenhofeSzoc K, Curbow B, Hooker C, Piantadosi S (2001) The prevalence of psychological distress by cancer site. Psychooncology 10: 19-28. [Crossref]
- Katon WJ (2003) Clinical and health services relationships between major depression, depressive symptoms, and general medical illness. Biol Psychiatry 54: 216-226. [Crossref]
- Schultz R, Beach SR (1999) Caregiving as a risk factor for mortality: The caregiver health effects study. JAMA 282: 2215-2219. [Crossref]
- Spitzer RL, Kroenke K, Linzer M, Hahn SR, Williams JB, et al. (1995) Health-related quality of life in primary care patients with mental disorders. Results from the PRIME-MD 1000 study. JAMA 274: 1511-1517. [Crossref]
- American Psychiatric Association (APA) (2000) Diagnostic and statistical manual of mental disorders, text revision (DSM-IV-TR). 4th ed. Washington DC: APA.
- Charmaz K (2000) Experiencing chronic illness. In: Albrecht GL, Fitzpatrick R, Scrimshaw SC, editors. Handbook of social studies in health and medicine. Thousand Oaks, CA: Sage Publications.
- National Cancer Institute (NCI) (2004) Living beyond cancer: Finding a new balance. President’s cancer panel 2003-2004 annual report. Bethesda, MD: Department of Health and Human Services, National Institutes of Health. Date of Access: April 7, 2017. https://pubs.cancer.gov/ncipl/detail.aspx?prodid=P986
- Brady MJ, Peterman AH, Fitchett G, Mo M, Cella D (1999) A case for including spirituality in quality of life measurement in oncology. Psychooncology 8: 417-428. [Crossref]
- Lin HR, Bauer-Wu SM (2003) Psycho-spiritual well-being in patients with advanced cancer: an integrative review of the literature. J Adv Nurs 44: 69-80. [Crossref]
- Institute of Medicine (IOM) (1982) Health and behavior: frontiers of research in the behavioral sciences. DA Hamburg, GR Elliot, and DL Parron, eds. Washington DC: National Academy Press.
- Keller M, Sommerfeldt S, Fischer C, Knight L, Riesbeck M, et al. (2004) Recognition of distress and psychiatric morbidity in cancer patients: a multi-method approach. Ann Oncol 15: 1243-1249. [Crossref]
- Epstein RM, Street RL (2007) Patient-centered communication in cancer care: Promoting healing and reducing suffering. NIH Publication. No. 07-6225. Bethesda, MD: National Cancer Institute.
- USA Today, Kaiser Family Foundation, and Harvard School of Public Health. 2006. National survey of households affected by cancer: summary and chartpack: Menlo Park CA, and Washington DC: USA Today, Kaiser Family Foundation, and Harvard School of Public Health. Date of Access: April 7, 2017. http://kff.org/health-costs/poll-finding/summary-and-chartpack-national-survey-of-households/
- Catholic hospitals comprise one quarter of world’s healthcare (2010) council reports: Catholic News Agency (CNA). Catholic News Agency, 10.
- LeMay K, Wilson KG (2008) Treatment of existential distress in life threatening illness: a review of manualized interventions. Clin Psychol Rev 28: 472-493. [Crossref]
- Temu TM, Bahiru E, Bukachi F, Bloomfield GS, Muiruri P, et al. (2017) Lay beliefs about hypertension among HIV-infected adults in Kenya. Open Heart 4: e000570. [Crossref]
- Adlard JW, Hume MJ (2003) Cancer Knowledge of the General Public in the United Kingdom: Survey in a Primary Care Setting and Review of Literature. Clin Oncol (R Coll Radiol) 15: 174-180. [Crossref]
- Crawford SM, Skinner J, Coombes E, Jones AP (2017) Cancer of Unknown Primary: A Cancer Registry Study of Factors Affecting Access to Diagnosis. Clin Oncol (R Coll Radiol) 29: e39-e46. [Crossref]

