Abstract
Introduction: Studies comparing the group prenatal care (GPC) model to individual prenatal care have found a significant reduction in risk for preterm birth in infants born to mothers who participated in group care. The cause of this observed effect has never been fully explained.
Methods: We reviewed the literature examining extrinsic factors that could lead to improved maternal-fetal health outcomes, focusing specifically on health literacy, and then mapped the components of group prenatal care to improved health literacy to consider the effects on the physical and psychological well being of women and their children.
Results: GPC may function to reduce rates of preterm birth through intervening at the level of health literacy. By synthesizing leading models of GPC with literature on the effects of improved health literacy on health outcomes, we propose a framework by which rates of preterm birth are reduced by specifically targeting improvement of health literacy as a means of intervention.
Discussion: GPC effectively targets all aspects of health literacy and improves patients’ access to healthcare, patient-provider interactions, and patient self-care practices. Further research will be required to evaluate the change in health literacy that patients in GPC undergo and whether health literacy lies on the causal pathway between GPC and improved health outcomes.
Significance: The literature suggests that improvements in health literacy positively affect health outcomes. Research has also demonstrated that group prenatal care significantly reduces preterm birth and maternal psychosocial stress. However, maternal health literacy has not been evaluated before in regards to affecting birth outcomes, specifically preterm birth. We propose a framework that suggests a potential health literacy explanation for the observed reduction in preterm birth rates.
Key words
health literacy, group prenatal care, preterm birth, maternal health, birth outcomes, prenatal care
Background
Preterm birth is the leading contributor to infant mortality in the United States [1], with approximately 9.6% of all US births occurring before 37 weeks in 2015 [2]. This high rate of PTB is not only biological, but has been linked to various social and environmental determinants of health [3]. Thus, targeting these through Group Prenatal Care (GPC) offers an effective approach to reducing PTB rates. In a randomized controlled trial, pregnant women aged 14 to 25 years who were assigned to receive GPC experienced significantly fewer preterm births (9.8%, n=623) compared to women receiving standard care (13.8%, n=370) [4]. This reduction in preterm birth rates was also demonstrated amongst low risk women in South Carolina [5] and was noted for African American women in a systematic review and meta-analysis [6]. During GPC, pregnant women meet in a group with an obstetrical care provider for up to ten sessions of clinical care, support and education. Each session deals with specific prenatal care topics, focusing on group discussion, encouraging women to ask questions and share answers, and fostering problem solving and personal empowerment. Qualitative work has found that GPC provides enhanced educational benefits, social support and connection with a provider [7] and it has been suggested that GPC might be effective due to these benefits. However, the mechanism of why GPC decreases preterm birth rates has not been discovered.
We propose that GPC may work to improve perinatal outcomes by improving health literacy, defined as “the cognitive and social skills which determine the motivation and ability of individuals to gain access to, understand, and use information in ways which promote and maintain good health” [8]. This assessment of health literacy moves beyond the narrow definition of literacy - the capacity to read and comprehend information – and fits closely with the patient empowerment goals of GPC. Maternal health literacy is potentially an effective point of intervention for improving birth outcomes. According to the National Assessment of Adult Literacy of 2003, only 12% of adults were found to be fully proficient [9]. While information outlining concepts and consequences surrounding health literacy is abundant, little research has linked diminished health literacy in mothers specifically to poorer birth outcomes. However, the literature demonstrating that poor health literacy leads to poorer individual health outcomes is extensive. The Agency for Healthcare Research and Quality conducted an extensive review of health literacy studies and found significant data suggesting that low health literacy predisposed individuals to poorer health, including lower rates of medication adherence, poorer chronic disease self-management, lower screening rates, and higher numbers of hospitalizations [10,11].
The onus of poor health literacy does not fall on the patient, however, but largely rests with the provider and the healthcare system. Health literacy is not only defined as the skills of an individual, but also reflects the processes by which health systems and workers make health knowledge comprehensible and achievable. In a survey of patient education materials, a large gap was found between the average patient comprehension level and the level of medical resources [9]. In response to this gap, many patients hide their difficulties with navigating the healthcare system due to embarrassment or shame [12]. Given the short amount of time allocated for an average doctor’s visit and this communication gap, it can be difficult for a provider to accurately assess the patient’s knowledge of their condition and respond with appropriate information.
Poor maternal health literacy has been shown to influence maternal health knowledge and practices. One study has shown that women with poor health literacy knew less about prenatal screening tests for birth defects [13]. For many women, pregnancy and birth are their first contact with the healthcare system and the complexity of its navigation during pregnancy can be overwhelming. Given that the average appointment time with a physician is approximately fifteen minutes, and the wait time to see a physician can be far longer than the appointment itself, a more effective strategy to support mothers during their pregnancy is desired. This method would be patient-centered with a focus on identifying each patient’s needs, empowering them to take charge of their health, and helping them to navigate effectively through the healthcare system. We propose GPC as an efficacious mechanism by which this may be achieved.
Methods
We conducted a literature search to explore how existing health literacy models might explain the mechanism of action of GPC. Database searches used the keywords “health literacy,” “birth outcomes,” “premature birth,” and “group prenatal care.” We synthesized current leading models on how health literacy influences health outcomes. We then examined key studies comparing GPC to individual care in terms of health behaviors and outcomes, focusing specifically on women’s experience of GPC and mapping those findings to the principles of health literacy to create a theoretical model.
Results
While the importance of health literacy is universally accepted, a wide variety of definitions and frameworks have been proposed. Nutbeam (8) proposes three types of literacy: 1) functional literacy describes reading and writing ability; 2) interactive literacy describes an ability to communicate and interact with healthcare providers to address issues; and 3) critical literacy describes the capacity to assess information and apply it to a personal circumstance. While most health literacy studies and assessments focus solely on functional literacy, both interactive and critical literacy improvements are essential to realize positive health outcomes. This broader vision of health literacy captures the wide reaching goals of GPC and may best describe its mechanism of action.
The health literacy model proposed by Paasche-Orlow and Wolf [14] describes a causal pathway between health literacy and health outcomes. In their model, they offer three antecedents that contribute to health literacy: social factors, cognitive/physical factors, and demographic factors. The authors then elucidate the downstream consequences of improved health literacy along three separate points along the healthcare continuum: 1) access and utilization of healthcare; 2) provider-patient interactions; and 3) patient self-care. Improvements in health literacy positively affect each point along the continuum, leading to improved health outcomes. In the context of this model, we hypothesize that GPC intervenes iteratively at the intersection of health literacy and its consequences. It effectively targets health literacy and provides support for change at each of the three points along the continuum, leading to the demonstrated positive perinatal health outcomes (Figure 1).
Through participation in GPC, pregnant women learn how to: 1) better access and navigate the healthcare system; 2) more effectively participate in decision making with their provider; and 3) augment their own self-care practices. At the same time, mothers are refining their functional, interactive, and critical health literacy skills, further improving these three downstream factors. Taking a more detailed look into the GPC model, we see how each element of the model specifically works to directly improve literacy and downstream literacy factors (Figure 2), and potentially circumvent the negative effects caused by social disparities on birth outcomes. By providing real world skills, GPC empowers patients to control their own health and the health of their future children. The core elements of the GPC model work to specifically target downstream literacy factors as well as improve health literacy in general as a mechanism leading to improved birth outcomes.
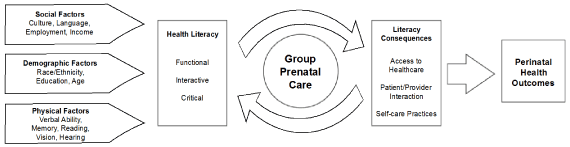
Figure 1. Framework for group prenatal care as an intervention.
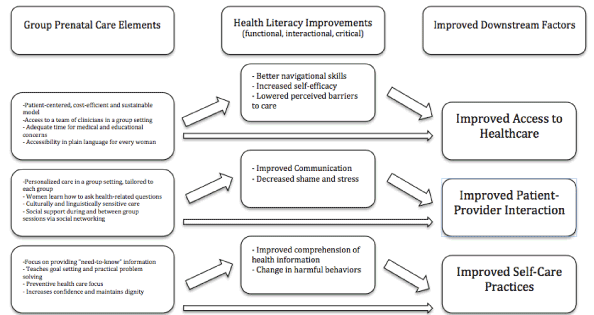
Figure 2. Group prenatal care central tenets and their relationship to health literacy factors.
Discussion
2021 Copyright OAT. All rights reserv
Improvement of access and utilization of care
Adopting a patient-centered group design: Effective interventions for the improvement of health literacy focus on patient-centered care and are a priority set forth by professional societies such as American Congress of Obstetricians and Gynecologists that provide leadership in prenatal care (15). In a standard setting, this involves encouragement of patient participation, assessment of patient understanding, using open-ended questions, and working together to create an action plan to attain a health goal. While this can be difficult to effectively carry out in a standard encounter, these techniques are built-in to the GPC model. Sessions are primarily participant directed, so that individual needs are directly addressed. A group consisting of first-time mothers from a socioeconomically disadvantaged background may focus more on preparing financially for a child, building a parenting skill set, and tapping into additional support networks. Conversely, a group of older mothers may choose to spend more time talking about long-term health concerns, adapting to a growing family, and integrating a new sibling into the home. This approach improves patient access to the healthcare system by reducing perceived barriers and complexity, learning navigation tips from peers, and tackling the fragmentation of care that plagues many healthcare systems. Additionally, pediatricians can visit the group and discuss newborn care, rather than booking individual appointments. This improves critical health literacy along the continuum from prenatal to newborn care, and facilitates easier access to pediatric care.
Improvement of patient-provider interactions
Improving written and verbal communication: Verbal communication often presents a barrier to care during clinical encounters. Patients often find that physicians speak above their comprehension level and do not allow for time to process information. Recommendations for physicians include speaking slowly and using nonmedical language, while breaking down information into manageable steps [16]. The teach-back method, where patients are encouraged to repeat back information to confirm comprehension and clarify misunderstanding, has been found to be effective in ensuring comprehension and promoting health literacy. In a randomized control study of the teach-back method in an emergency department, patients receiving the intervention were found to have significantly higher comprehension scores for post discharge self-care and follow-up [17]. GPC embodies the principals of the teach-back method through facilitated discussion, empowering women to answer questions first and avoiding the didactic approach usually employed in individual care. Verbal communication is emphasized and written communication is provided as a back up and reinforcement. Furthermore, all written material provided is accessible in plain language and available in multiple languages to ensure each woman can bring home the knowledge that she learns in each session for future reference. Comprehension can be improved even further outside of the group encounter through electronic social networking, which provides ongoing peer-to-peer communication.
Limited health literacy on the part of the patient, overestimation of health literacy on the part of the provider and limited patient-provider time can all contribute to miscommunication between physician and patient. GPC minimizes these barriers to care. Discussions are tailored to the needs and knowledge level of the participants, focusing on the material that women “need to know.” Feedback through interactive discussion is conducted at each session to ensure the program is meeting each individual’s needs. During normal prenatal visits, patients are scheduled at 10-15 minute intervals, an inadequate amount of time to address all issues, even with a skilled healthcare provider. Women participating in GPC however, can access a total of 20 hours of care with a provider, split into ten 2-hour sessions [4]. These strategies increase patient-provider interaction and enhance interactive literacy.
Reducing maternal stress and increasing confidence
Poor health literacy can lead to increased stress during medical encounters, as well as feelings of shame due to self-perceived lack of knowledge. This often prevents patients from asking questions of their provider [18]. As a result, poor health literacy can be invisible to those providers. Wadwha et al. [19] found a significant correlation between increased maternal psychological stress and higher rates of preterm birth, proposing potential stress-related biological explanations for this link. This has been confirmed in studies associating high biological levels of chronic stress, or “allostatic load,” with increased incidence of preterm birth [20,21]. GPC has been found to function as a successful intervention to decrease maternal psychosocial stress [22]. The power dynamic of a doctor-patient relationship that sometimes prevents patients from speaking openly is minimized through peer support and encouragement. Women also can discuss external stressors and get advice from other group members, who are their peers. Qualitative work suggested that women appreciated receiving “more than they realized they needed” through participating in a group in which they were able to learn from other women’s questions [7]. GPC can thus increase self-confidence and provide social support, both of which can minimize stress and improve both critical and interactive literacy.
Improvement of patient self care
Understand, interpret, and analyze health information: Little time is spent during standard care visits interpreting results and understanding both the causes and consequences of health behaviors. GPC instead provides a one-stop visit where patients can record their own weight and blood pressure, receive testing such as blood draws, and monitor their own progress. The GPC model then uses tailored language to assist patients with analyzing their information and discussing results in a group setting. These discussions allow patients to gain problem-solving techniques as a group in a self-directed and thus culturally appropriate fashion. Individual problem-solving skills may be improved as a result.
Encourages behavioral change
GPC can be an effective tool to raise levels of health literacy and provide women with an environment in which to contemplate, plan, and implement behavior change in order to eliminate unhealthy habits. Behavior change is a difficult process, and one that requires confidence, commitment and support. For example, a woman who is struggling with her weight gain might receive practical advice from her peer group and likely gain tremendous encouragement when the goals are met. In a study comparing GPC to traditional care, adolescent women in GPC were more likely to achieve gestational weight guidelines and breastfeed exclusively, as well as experience lower rates of post-partum depression [23]. GPC was also shown to increase utilization of postpartum family-planning services [24], thus providing positive lifestyle support throughout the reproductive period and increasing the likelihood of pregnancy intentionality and healthy birth spacing.
Conclusion
GPC functions on each level of a broad health literacy model to reduce barriers to the optimal healthcare experience and promote healthy perinatal outcomes. This may explain the observed reduction in the rate of preterm birth among women receiving GPC [4,5] and specifically African American women receiving GPC [6]. In intervening at the level of health literacy, GPC attempts to diminish the upstream effects that certain social factors such as income, race, education level, and cultural factors have on health outcomes. Further studies will need to be completed in order to determine if, in fact, maternal health literacy levels of women who have completed GPC are improved. In addition, better literacy assessments must be developed to measure not only functional, but also interactive and critical literacy. The precise link between improved maternal health literacy and better perinatal outcomes still remains to be proven. However, given both the history of health literacy research in the improvement of individual health outcomes and the tenets of the GPC model with a focus on specifically improving elements of health literacy, this is a potential and promising mechanism for explaining the preterm birth reduction.
References
- Matthews TJ, MacDorman MF, Thoma ME (2015) Infant mortality statistics from the 2013 period linked birth/infant death data set. National Vital Statistic Reports 64.
- Martin JA, Hamilton BE, Osterman MJ (2017) Births: Final data for 2015. National vital statistics report. Hyattsville, MD: National Center for Health Statistics 66.
- Green NS, Damus K, Simpson JL, Iams J, Reece EA, et al. (2005) Research agenda for preterm birth: recommendations from the March of Dimes. Am J Obstet Gynecol 193: 626-635. [Crossref]
- Ickovics JR, Kershaw TS, Westdahl C, Magriples U, Massey Z, et al. (2007) Group prenatal care and perinatal outcomes: a randomized controlled trial. Obstet Gynecol 110: 330-339. [Crossref]
- Picklesimer AH, Billings D, Hale N, Blackhurst D, Convington-Kolb S (2012) The effect of Centering Pregnancy group prenatal care on preterm birth in a low-income population. Am J Obstet Gynecol 206: 415. [Crossref]
- Carter EB, Temming LA, Akin J, Fowler S, Macones GA, et al. (2016) Group prenatal care compared with traditional prenatal care: a systematic review and meta-analysis. Obstet Gynecol 128: 551-561. [Crossref]
- McNeil DA, Vekved M, Dolan SM, Siever J, Horn S, et al. (2012) Getting more than they realized they needed: a qualitative study of women's experience of group prenatal care. BMC Pregnancy Childbirth 12: 17. [Crossref]
- Nutbeam D (2000) Health literacy as a public health goal: a challenge for contemporary health education and communication strategies into the 21st century. Health Promotion International 15: 259-267.
- Kutner M, Greenberg E, Jin Y, Paulsen C (2006) The health literacy of America's adults: Results from the 2003 National Assessment of Adult Literacy (NCES 2006–483). Washington, DC: National Center for Education Statistics.
- Berkman ND, Dewalt DA, Pignone MP, Sheridan SL, Lohr KN, et al. (2004) Literacy and health outcomes. Evidence report/technology assessment (Summary) 87: 1-8.
- Berkman ND, Sheridan SL, Donahue KE, Halpern DJ, Crotty K (2011) Low health literacy and health outcomes: an updated systematic review. Ann Intern Med 155: 97-107. [Crossref]
- Barrett SE, Puryear JS (2006) Health literacy: improving quality of care in primary care settings. J Health Care Poor Underserved 17: 690-697. [Crossref]
- Cho RN, Plunkett BA, Wolf MS, Simon CE, Grobman WA. (2007). Health literacy and patient understanding of screening tests for aneuploidy and neural tube defects. Prenat Diagn 27: 463-467. [Crossref]
- Paasche-Orlow MK, Wolf MS (2007) The causal pathways linking health literacy to health outcomes. Am J Health Behav 31: 19-26. [Crossref]
- American College of Obstetricians and Gynecologists’ Committee on Patient Safety and Quality Improvement; Committee on Health Care for Underserved Women. (2016) Committee Opinion No. 676: Health Literacy to Promote Quality of Care. Obstet Gynecol 128: e183-186. [Crossref]
- Hersh L, Salzman B, Snyderman D (2015) Health Literacy in Primary Care Practice. Am Fam Physician 92: 118-124. [Crossref]
- Griffey RT, Shin N, Jones S, Aginam N, Gross M (2015) The impact of teach-back on comprehension of discharge instructions and satisfaction among emergency patients with limited health literacy: A randomized, controlled study. J Commun Healthc 8: 10-21. [Crossref]
- Parikh NS, Parker RM, Nurss JR, Baker DW, Williams MV (1996) Shame and health literacy: the unspoken connection. Patient Educ Couns 27: 33-39. [Crossref]
- Wadhwa PD, Entringer S, Buss C, Lu MC (2011) The contribution of maternal stress to preterm birth: issues and considerations. Clin Perinatol 38: 351-384. [Crossref]
- Wallace ME, Harville EW (2013) Allostatic load and birth outcomes among white and black women in New Orleans. Matern Child Health J 17: 1025-1029. [Crossref]
- Olson DM, Severson EM, Verstraeten BS , Ng JW, McCreary JK, et al. (2015) Allostatic Load and Preterm Birth. Int J Mol Sci 16: 29856-29874. [Crossref]
- Heberlein EC, Picklesimer AH, Billings DL, Covington-Kolb S, Farber N, et al. (2016) The comparative effects of group prenatal care on psychosocial outcomes. Arch Womens Ment Health 19: 259-269. [Crossref]
- Trotman G, Chhatre G, Darolia R, Tefera E, Damle L (2015) The effect of Centering Pregnancy versus traditional prenatal care models on improved adolescent health behaviors in the perinatal period. J Pediatr Adolesc Gynecol 28: 395-401. [Crossref]
- Hale N, Picklesimer AH, Billings DL, Covington-Kolb S (2014) The impact of Centering Pregnancy Group Prenatal Care on postpartum family planning. Am J Obstet Gynecol 210: 50. [Crossref]


