The configuration (molding) of the fetal head during childbirth is an important process that has not been sufficiently studied and evaluated by perinatologists, obstetricians, pediatric neuropathologists and pathologists. The configuration can be physiological and pathological. The configuration of fetal head is a compensatory-adaptation process providing adaptation of its size and shape to forces acting on it when passing through the parturient canal. Thus, the shape of fetal head changes and transforms in compliance with forces acting on it. The first force is pressure acting from above and caused by labors. The second force impacting on the head is pressure caused by resistance of insufficiently disclosed maternal passages. The head movement and eventually childbirth occur due to the configuration. This process is executed owing to sutures and fontanels and elasticity of the skull bones and primarily owing to their ability to displace in relation to one another and to overlap each other. The ability of the head to adjust to sizes of the parturient canal is called configurability [1].
Despite any grade of the head configuration is generally favorable for a mother and contributes to a normal course of delivery, from the fetus’ perspective, one should differ physiological and pathologic (abnormal) configurations. The physiological configuration is not accompanied by a cerebral injury, while the abnormal configuration leads to such kind of an injury. Moreover, we may distinguish three types of the abnormal configuration: (1) excessive, (2) rapid, and (3) asymmetrical. Many authors evaluate the configuration grade by skull biometry and by measuring different sizes (direct, major oblique, and others), and then they determine the configuration indexes [2-4]. I assess the configuration grade by the quantity of sutures with overlapping of bones, since the greater is the mechanical impact experienced by the fetal skull, the greater number of sutures is used to determine overlapping of bones. Here, I identify three grades of head configuration: 1, overlapping of bones over one of sutures; 2, overlapping of bones within 2–3 sutures; and 3, overlapping of bones over 4–5 sutures. The configuration is a dynamic process. Its grade is subject to change in different labor phases provided the forces acting on the fetal head alter. However, only one short-term episode of transformation of the physiological configuration to pathological one may lead to birth traumatic injuries which are dangerous for infant’s life. I found that the increase in the head configuration grade leads to the increased frequency of leptomeningeal (including subarachnoidal), subependymal, intraventricular and intracerebral hemorrhages and also cerebellar hemorrhages, periventricular leukomalacia, telencephalic gliosis, and cerebral infarctions [5].
Also, I found that in cases of overlapping of bones over the sagittal suture, the leptomeningeal hemorrhages are predominantly localized on the side of the parietal bone which overlaps the contralateral one, i.e., is superjacent; a subperiosteal blood congestion usually moves to the same side. Meanwhile, subdural hemorrhages (just as tentorium ruptures) are more frequently localized on the side of the subjacent bone, i.e., extending under the opposite bone, since an important role belongs to the asynclitic head fitting (or presentation) in the genesis and localization. After birth, the head is subjected to reconfiguration with the reconstruction of its shape, disappearance of overlapping or protrusion of bones, and increase of the middle oblique diameter and anterior fontanel. According to Muller [1], the reconfiguration process normally ends within 3–4 days, and according Kriewall [6], it ends within 7 days.
Poorly understood mechanisms leading to disturbances of cerebral circulation in the head configuration. The resulting brain damage can be both hypoxic and traumatic. Little studied various types of bone displacement. One of these types is cross-entry of bones, when one part of the bone enters the opposite, and the other part goes under the opposite bone (Figure 1). This type of bone displacement, often observed in premature babies, has a compensatory-adaptive value, as it prevents a significant displacement of the bones and the pressure of the underlying bone on the underlying surface of the brain.
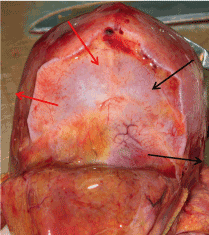
Figure 1. The cross overlapping of bones at the lambdoid suture: the occipital bone below overlaps the left parietal bone, and in the upper third, on the contrary, the parietal bone overlaps the occipital bone: only in the lower third, the occipital bone overlaps the right parietal one, and the parietal bone overlaps the occipital bone from above (arrows).
The configuration of the head in relation to the mother is always an adaptive mechanism. However, if we evaluate the importance of this mechanism for the fetus and newborn child, it can be both positive and negative, leading to brain damage. Study of configuration features may help explain the cause of intracranial injury, as well as to objectively evaluate the nature of the flow of labor.
- Muller D (1973) Die subakuten Massenverschiebungen des Gehirns unter der Geburt. Leipzig: VEB Georg Thieme.
- Issel EP (1976) Configuration of the skull of the newborn infant through the mechanical forces of labor and refiguration. Zentralbl Gynakol 98: 1301-1306. [Crossref]
- Kriewall TJ, Stys SJ, McPherson GK (1977) Neonatal head shape after delivery: an index of molding. J Perinat Med 5: 260-267. [Crossref]
- Sorbe B, Dahlgren S (1983) Some important factors in the molding of the fetal head during vaginal delivery--a photographic study. Int J Gynaecol Obstet 21: 205-212. [Crossref]
- Vlasyuk VV (2018) Birth Trauma and Perinatal Brain Damage. Springer-Verlag GmbH.
- Kriewall TJ (1982) Structural, mechanical, and material properties of fetal cranial bone. Am J Obstet Gynecol 143: 707-714. [Crossref]

