This paper investigates HIV-positive mothers’ compliance to medical advice in order to reduce the risk of passing HIV from mother to infant during the complementary feeding period. A qualitative study was carried out in Manhiça and Namaacha rural districts of Maputo province. The study consisted of in-depth interviews, focus group discussions with HIV-positive mothers recruited at the healthcare facilities, and semi-structured interviews with nurses.
We used Bourdieu’s theory of practice as a guideline framework to identify factors influencing HIV-positive mothers on compliance to medical advice. Five themes were identified: i) adherence to postnatal visits; ii) introduction of complementary food; iii) cessation of breastfeeding, iv) adherence to antiretroviral therapy; and v) adherence to contraceptive methods.
Findings show participants complied with some recommended medical advice such as adherence to postnatal and child at risk clinic visits, and lifelong antiretroviral therapy as they perceived these recommendations as beneficial. However, participants often introduced complementary food before the recommended six months. As well, they often introduced inadequate complementary food due to lack of knowledge, poor economic conditions and, social and cultural norms. Furthermore, a considerable number of participants stopped breastfeeding at six months, while others continued with it after introducing complementary food. Participants did not adhere to the recommendations about contraceptive dual method use due to a lack of decision-making power.
In conclusion, participants did not comply with some of the recommended medical advice due to multiple factors, including individual and collective perceptions, inadequate advice from the healthcare providers and the family and the complexity of breastfeeding policy. This study recommends that all healthcare providers should be trained in a new protocol to ensure that mothers receive the same advice, and that partners and mothers-in-law should also be included in health education to ensure they support mothers during breastfeeding.
breastfeeding, complementary food, HIV-positive mothers, Mozambique
In developing countries, the risk of postnatal transmission of HIV from mother-to-infants is considered high among the breastfeeding population. The risk of a HIV-positive mother to transmit HIV to her infant through breastfeeding is estimated at 25-35% in the first 6 months following childbirth and 30-45% among mothers who breastfeed their infants between 18 and 24 months [1]. In 2016, about 77 000 infants acquired HIV from their mothers in some developing countries, particularly those located in sub-Saharan Africa region [2]. Transmission of HIV from a mother-to-infants therefore remains a public health problem in developing countries.
Scientific evidence in developing countries [3-5] has confirmed that passing HIV from mother-to-infants can be reduced if HIV-positive mothers comply with medical providers’ advice during postnatal period. This includes exclusive breastfeeding and following recommendations on when to stop breastfeeding and to introduce appropriate complementary food [3,6,7]. Some authors [8] suggest if HIV-positive mothers adhere to antiretroviral therapy, they can also breastfeed up to 24 months and still prevent their infants to HIV infection. Nonetheless, other researchers [9,10] concluded there was still a risk of HIV transmission among mothers who continued breastfeeding after 6 months. Despite lack of consensus among authors, in 2013 the World Health Organization (WHO) recommended that all HIV-positive mothers should exclusively breastfeed in the first six months following childbirth, introduce complementary food thereafter and continue with breastfeeding until the infant is 12 months old. Moreover, all HIV-positive mothers are recommended to continue with antiretroviral therapy during and after stopping breastfeeding [6].
Since 2013, following the WHO’s recommendations, the Ministry of Health of Mozambique recommends that all HIV-positive mothers follow medical advice during the complementary feeding period. They are advised to comply with lifelong antiretroviral therapy, introduce appropriate complementary foods from 6 months following childbirth, and to continue breastfeeding for the first 12 months of life [11]. HIV-positive mothers are requested to attend 3 postnatal visits in the 3 weeks following childbirth. They should also attend a child at risk clinic for one month after childbirth, and thereafter once per month until the baby is a full year old. From 13 months, mothers should attend sessions at a child at risk clinic once every two months until the baby is 18 months old or after a final HIV status diagnostic of the child is disclosed. Throughout this time frame, the mother and the child access HIV treatment from the clinic [12]. HIV-positive mothers are only recommended to stop breastfeeding when a nutritionally adequate and safe diet without breast milk can be provided [6]. They are also requested to use dual contraceptive method – combining condoms and injection, intra-uterine device or pills [11]. These recommendations are an update of a previous guideline formulated by the Ministry of Health of Mozambique in 2012. This guideline [13] advised that HIV-positive mothers should exclusively breastfeed until 6 months and stop thereafter.
Since 2013, the Mozambican Ministry of Health recommends the use of formula or modified breast milk as complementary food for infants who are more than 6 months old [11]. Modified breast milk consists on expressing breast milk and heating to eliminate viral load, and as a means to reduce the postnatal transmission of HIV from mother to child [7,14]. Mothers are advised to use formula or modified breast milk for infants under 6 months if the baby has low weight, or during the transition period of breastfeeding weaning. Additionally, formula should be used when the mother is sick and cannot breastfeed or if there is a temporary lack of antiretroviral drugs for the mother [11]. Mothers are also advised not to end breastfeeding abruptly. They are requested to introduce different complementary foods according to the age of the infant. Formula and semi-solid food – such as soup, puree and pap – should be introduced when infants are between 6 and 9 months, and solid food – family food – from the age of 12 months [1]. However, in 2011, the Demographic Health Survey (DHS) revealed that at the national level, the population of Mozambique generally introduces complementary food to their babies at 4 months of age [15]. This practice could put infants born from HIV-positive mothers at risk of HIV infection.
Several studies [16-18] have documented early and inadequate introduction of food among infants of HIV-positive mothers living in sub-Saharan Africa countries. Fadnes et al. [19] confirmed that some mothers introduced foods such as banana, maize and beans to infants under 6 months old. Others revealed mothers introduced food at 6 [20] and 7 months old, but still continued breastfeeding [21]. Early introduction of foods is associated with low household income [22,23] and the occupation of the mother [16]. Also, the child’s gender seems to influence the early introduction of foods. In some communities, boys are more likely to be introduced to food earlier than girls [20]. As well, there is a perception that breast milk alone is not sufficient to nourish a child up to the age of 6 months [24], which has led mothers to give food to their infants before the recommended time.
In most sub-Saharan African countries, HIV-positive mothers stop breastfeeding between 4 and 6 months [18,21,25-27]. Nonetheless, other studies showed HIV-positive mothers ended breastfeeding when the infant was 11 months in Kenya [20], 12 months in Uganda [19] and 13 months in Ethiopia [17]. In Mozambique, the duration of complete breastfeeding in the general population is estimated to be 20 months [15], but the duration of breastfeeding among HIV-positive mothers is unknown.
Early cease of breastfeeding has also been associated with religious affiliation. For example, in Bangladesh, research [16] found that Muslim mothers were more likely to terminate breastfeeding earlier than non-Muslim mothers. Moreover, in most developing countries [16,20] studies have documented that mothers with a high level of education, and those who were employed are more likely to end breastfeeding earlier. Several authors [17] have also discovered that, if mothers disclosed their HIV-positive status to their partners, they were more likely to cease breastfeeding early. Furthermore, a study in Kenya [20] concluded that a higher monthly income of the household enabled mothers to afford foods and bottle feeding, which contributes to ending breastfeeding earlier.
Another challenge during the postpartum period is related to the low adherence to life-long antiretroviral therapy among HIV-positive mothers and HIV treatment for their HIV-positive infants. Some studies [28,29] have documented low adherence and attribute it to economic factors, emotional stress, depression and lack of HIV disclosure [28].
Despite some documentation of complementary breastfeeding in sub-Saharan Africa [19,21,26] little is yet known about such practices. At present, we do not know what factors influence complementary feeding among HIV-positive Mozambican mothers. This qualitative study therefore aims at analysing HIV-positive mothers’ practices with regard to complementary feeding and their compliance to medical advice in rural Maputo province in Mozambique. Our analysis focuses on infant feeding as a practice [30,31] as it is influenced by the social and cultural environment [32-34]. We use the theory of practice underlined by Pierre Bourdieu [35] to understand how both structural and individual factors influence breastfeeding within a specific context.
Bourdieu [30] maintains that food and eating practices depend on the ideas people have about the body and the effect food has upon it. It is linked with strength, health and beauty as well as several other categories used to evaluate these effects. Bourdieu further suggests that food and eating practices are associated with gender, identity and one’s position and status within a society. When it comes to infant feeding, the choice and time of introduction of complementary food may be influenced by the gender and social status of the infant as well as other social and cultural norms that are related to decision-making power in the household. In many instances, it is not necessarily the mother who decides on the introduction of food and the ending of breastfeeding. Bourdieu’s theory further allows to explain how compliance to the recommended feeding practices and adherence to antiretroviral drugs depends on HIV-positive mothers’ perceptions. Their position in terms of decision-making, their incorporated learned experiences as well as their social and cultural environment are significant. A better understanding of this can contribute to preventive practices that reduce infants’ risk of HIV infection.
Study design and study sites
This qualitative study is part of a broader research on perceptions and practices regarding pregnancy care and infant feeding among HIV-positive women in rural Mozambique. Data was collected in Namaacha and Manhiça rural districts of Maputo province, located in the south of Mozambique.
In 2015, Namaacha district had a population of 51, 257 [36] and 10 healthcare facilities. Approximately 263,736 inhabitants lived in Manhiça district [36] with 14 healthcare facilities and one rural hospital. Both districts are located in Maputo province, which accounts for 19.8% of HIV-positive people aged between 15 and 59 years. About 20% are HIV-positive women while 19.5% are HIV-positive men [37].
Recruitment of participants and data collection
Recruitment and interviews of study participants took place in 6 healthcare facilities between January and March 2015. These healthcare facilities implement a prevention of mother-to-child transmission of HIV program. Three healthcare facilities were selected in each district.
A purposive sample was applied to select 59 HIV-positive mothers. Only mothers who had infants or children aged between 0 and 2 years old were included in the sample. Twenty-five were located in Namaacha district and 34 in Manhiça district. Among these participants, 47 mothers were still breastfeeding, and 12 had already stopped breastfeeding and were giving their babies staple food. Of those still breastfeeding, 27 mothers had already introduced complementary food. These participants were especially important in accessing mothers’ practices about breastfeeding and complementary feeding.
To select participants, the main researcher approached all mothers who were at the child at risk clinic. Those who agreed to participate were interviewed. A total of 59 in-depth interviews were performed, out of which 25 mothers had infants between 0 to 6 months while 34 mothers had infants aged 7 to 18 months. Most participants were between 18 and 34 years old, married or living with a partner. Participants were mainly farmers and had more than one child. Some participants lacked formal education (Table 1). The majority of participants were not working. Nearly all participants were members of a Protestant church, 6 were Catholic and 1 was Muslim.
Table 1. Demographic characteristics of the study participants
Characteristics of participants |
Manhiça (n=34) |
Namaacha (n=25) |
Total |
Age range |
|
18-24 |
14 |
10 |
24 |
25-34 |
17 |
11 |
28 |
35-39 |
3 |
4 |
7 |
Educational Level |
|
None |
10 |
4 |
14 |
Less than primary education (1-6 years) |
8 |
6 |
14 |
Primary education completed (7years) |
15 |
12 |
27 |
Secondary education completed (12 years) |
1 |
3 |
4 |
Marital Status |
|
Single |
5 |
7 |
12 |
Married/Living with a partner |
27 |
17 |
44 |
Divorced/Widow |
2 |
1 |
3 |
Number of Children |
|
1-2 |
20 |
14 |
34 |
3-4 |
11 |
7 |
18 |
5-6 |
3 |
4 |
7 |
Occupation |
|
Factor worker |
0 |
1 |
1 |
Farmer |
24 |
19 |
43 |
Housemaid |
2 |
1 |
3 |
Own business/sale |
6 |
1 |
7 |
Student |
2 |
1 |
3 |
Teacher |
0 |
2 |
2 |
The study also included 5 focus group discussions (FGD) with HIV-positive mothers. Three were conducted in Manhiça district and two in Namaacha district. Each FGD was comprised of between 6 to 10 participants. Six semi-structured interviews were also conducted with nurses working in the prevention of mother-to-child transmission of HIV program. One nurse was interviewed in each healthcare facility. Both individual in-depth interviews and focus group discussions were conducted in Portuguese – the national language – for those who could read and write it. Tsonga, the local vernacular language, was used for those who could not understand Portuguese.
Ethical procedures
This study obtained ethical clearance from the Faculty of Medicine of Eduardo Mondlane University and Maputo Central Hospital Bioethics committee, protocol number CIBS FM&HCM/73/2014. Verbal information about the objective of the study was provided, and a written consent form was presented to each participant allowing them to make an informed choice on whether or not to participate in the study.
All participants read and signed the informed consent forms. Those who could not read and write chose someone in their trust to translate the information into the local language and to sign on their behalf. Three sociologists participated in the data collection: one male main researcher (the first author) and two female assistant researchers, who were trained on the objectives of the study and data collection instruments. The main researcher coordinated fieldwork, interviewed the participants and moderated the focus group discussions.
Data analysis
A thematic analysis approach [38,39] was applied to obtain key themes emerging from the data. The analysis involved 6 stages, as suggested by Bram and Clarke [39]. To begin, interviews were transcribed and then translated from Portuguese to English. Secondly, each transcription was read more than once and initial codes were generated [39]. Initial coding consisted of naming the participants’ narrative [38] and identifying out of the ordinary features for analysis [39]. This included knowledge, experiences, practices and decision-making with regard to breastfeeding. We also made note of frequently repeated words or numbers emerging from participants’ narratives. Third, the codes were used to identify and search various themes and sub-themes across the data [39]. A theme is a set of words capturing something important about the data and representing some level of patterned meaning within the dataset [39]. We identified several themes such as: mother’s adherence to postnatal visits and child at risk clinic, practices related to the introduction of food among infants, breastfeeding weaning and adherence to antiretroviral therapy and contraceptive methods. In each theme, several subthemes were also classified. These included reasons for attending postnatal visits, knowledge, practices and power-decision with regard to introduction of complementary food and ending breastfeeding. Fourth, the identified themes were revised and refined. All authors were involved in the process of revision and refinement of the themes. This consisted of checking the relationship between coding and the themes generated, as well as evaluating the relationship between themes and subthemes. The final themes were then defined in the fifth stage [39] and presented in the findings section. At this point, we went back to the participants’ interviews and organised the narratives according to the identified themes. Content and supporting data of each theme were then identified. Quantitative data emerging from interviews were summarised and presented in tables and figures. These data were reported in each relevant theme or subtheme. The last stage of thematic analysis consisted of producing a report on these research outcomes.
Findings
Study findings were organized into 5 key themes: 1) adherence to postnatal visits and child at risk clinic, 2) introduction of complementary food, 3) breastfeeding cessation, 4) adherence to antiretroviral therapy, and 5) adherence to contraceptive methods. In each theme, we explore mothers’ breastfeeding practices and analysed their compliance to medical recommendations concerning complementary feeding period.
Adherence to postnatal visits and child at risk clinic
The majority of participants attended all postnatal visits three weeks after childbirth. Only seven participants missed postnatal visits. As well, the majority of participants visited the child at risk clinic regardless of their place of residence, age, educational level, marital status and occupation (Table 2). These data reveal that most participants complied with medical recommendations with regard to adherence to postnatal visit. This might be associated with the need of access of antiretroviral drugs for the baby and the mother.
Table 2. Adherence of participants to child at risk clinic
Characteristics of participants |
Number of visits at child at risk clinic |
Manhiça (n=34) |
Namaacha (n=25) |
1-5 |
6-10 |
11 and more |
1-5 |
6-10 |
11 and more |
Age range |
|
18-24 |
5 |
5 |
4 |
2 |
3 |
5 |
25-34 |
9 |
1 |
7 |
5 |
3 |
3 |
35-39 |
3 |
0 |
0 |
0 |
2 |
2 |
Educational Level |
|
None |
5 |
2 |
3 |
1 |
2 |
1 |
Less than primary education (1-6 years) |
5 |
0 |
3 |
2 |
1 |
3 |
Primary education completed (7 years) |
7 |
4 |
4 |
4 |
4 |
4 |
Secondary education completed (12 years) |
0 |
0 |
1 |
0 |
1 |
2 |
Marital Status |
|
Single |
2 |
1 |
2 |
5 |
5 |
7 |
Married/Living with a partner |
14 |
5 |
8 |
1 |
3 |
3 |
Divorced/Widow |
1 |
0 |
1 |
1 |
0 |
0 |
Number of Children |
|
1-2 |
10 |
5 |
5 |
3 |
5 |
6 |
3-4 |
5 |
1 |
5 |
3 |
1 |
3 |
5-6 |
2 |
0 |
1 |
1 |
2 |
1 |
Occupation |
|
Factor worker |
0 |
0 |
0 |
0 |
1 |
0 |
Farmer |
14 |
4 |
6 |
7 |
7 |
5 |
Housemaid |
0 |
0 |
2 |
0 |
0 |
1 |
Own business/sale |
3 |
2 |
1 |
0 |
0 |
1 |
Student |
0 |
0 |
2 |
0 |
0 |
1 |
Teacher |
0 |
0 |
0 |
0 |
0 |
2 |
The number of visits at child at risk clinic is determined by the age of the baby (Figure 1). The majority of participants who had infants aged 1 to 6 months had visited less the child at risk clinic than other participants who had infants aged between 7 and 18 months. Nonetheless, some participants with infants aged between 7 and 18 months visited the child at risk clinic only two times. This suggests that some participant missed some visits following childbirth.
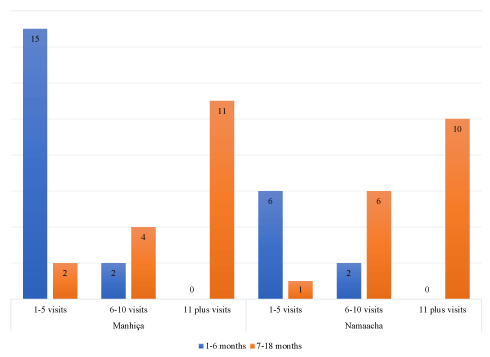
Figure 1. Number of visits to the child at risk clinic according to the age of the infants.
Reasons for attending postnatal visits and child at risk clinic
Participants offered several reasons for attending postnatal sessions and visits to the child at risk clinic. All participants viewed postnatal visits as useful for their babies because nurses diagnosed illnesses, checked to be sure the infant was growing well, measured the weight of the baby, gave vaccine to prevent diseases, and prescribed medication when the baby was sick. Some participants perceived visits to the healthcare facility as a way to comply with the healthcare providers advice. One of the participants expressed her views as follows:
I always go to the healthcare facility after childbirth because I want to follow the recommendations of healthcare providers. I want the welfare of the baby. Healthcare providers have control over the health of the baby, but myself I cannot control it. (34 years old, mother child, age 12 months).
Moreover, most participants associated postnatal visits with the wellbeing of their infants. As well, all participants perceived the visit to the child at risk clinic useful for their infants as well as their own health. This was because they could access medications such as antiretroviral drugs. One of the participants puts it as follows:
When I go to the postnatal visits, nurses help me to know if the baby is healthy, if his umbilicus has dried, and if myself I am fine or not. Nurses also prescribe medicine to the baby and me. (35 years old, mother of a child, age 1 month).
Some participants said they were motivated to attend the child at risk clinic because they received counselling about how to take care of their babies and themselves. Others however, said they attended to avoid reprimands by the nurses when they take their babies to the healthcare facility when they are sick. As one of the participants narrated it:
I always go to the child at risk clinic because I am scared to be insulted by the nurses. If you do not go to the child at risk clinic, the baby might get sick. When you take the baby to the child at risk clinic while he is sick, nurses insult you or they do not take care of your baby because you missed visits. (25 years old, mother of a child, age 5 months).
Adherence to postnatal visits and child at risk clinic was perceived as a way to comply with the recommendations of healthcare providers as well as a guarantee that they will be treated well by the healthcare providers when their infants were sick. One participant expressed her opinion in this way:
I always go to the healthcare facility because it is good to follow the recommendations of health providers and postnatal care. If I do not do that healthcare providers will get angry with me whenever I take the baby when he is sick. (24 years old, mother of a child, age 11 months).
Reasons to miss postnatal visits and child at risk clinic
Participants explained they sometimes missed postnatal visits due to lack of money for transport or because they lived very far from the healthcare facility. Participants who missed visits to the child at rick clinic also mentioned the same reasons. Indeed, some participants admitted they had not visited the child at risk clinic once since giving birth 3 months earlier. Other mothers with babies up to 7 months old had only attended the child at risk clinic twice.
Some participants referred they could not go the postnatal visit and child at risk clinic due to marital problems. One participant narrated how her divorce proceedings had influenced her participation in postnatal visits and attending the child at risk clinic as follows:
I missed the postnatal visits and child at risk clinic visits because I was under marriage problems with my husband, which ended my relationship with him. So, I had not time and I was not willing to go to postnatal and child at risk clinic due to depression. Today [2-03-2015] is the first day I come to the child at risk clinic since the baby was born seven months ago. The baby got even the first vaccine today. (29 years old, mother of a child age 7 months).
Nurses said that although the majority of mothers attended postnatal sessions, there was still a considerable number who did not comply with all visits at child at risk clinic. This was due to lack of money for transport; some mothers, soon after childbirth, had to relocate to be with their families or husbands in another district, province or in South Africa. This practice prevented mothers to comply with all postnatal visits, as one of the nurses narrated.
Some mothers do not comply with postnatal visits and visits at child risk clinic because they travel to South Africa to join their husbands who work there. Other also move from this district [Manhiça] to another district to practice agriculture or do their businesses. Most of these mothers do not inform us about their intention to emigrate, and we have no control over them. Sometimes, some mothers return to the healthcare facility after several months, and we discover they did not take the infant to the healthcare facility of the place where they have travelled to. (Nurse).
However, nurses added some mothers fully knew their babies were at risk of HIV infection. Some mothers did not persist with follow-up visits at child at risk clinics because they chose not to continue antiretroviral therapy, even though it put the baby at risk of HIV infection. One of the nurses explained a situation as follows:
I have a patient that did not want to continue with antiretroviral in this healthcare facility after childbirth. She said that she was following the same treatment in another healthcare facility close to this district [Namaacha]. But she was not following any treatment. She disappeared three months and she was breastfeeding. When she came back because the baby was sick, I noticed that she did not go to another healthcare facility because the card of the baby was not signed. I explained her the risk of lack of HIV treatment to her baby and her health, but she missed again the following visits at child at risk clinic. When she came back I tested the baby and he was HIV-positive. (Nurse).
Knowledge of introduction of complementary foods
Many participants lacked information about the recommended time of introducing complementary food; some said complementary food should be introduced when the infant was between 2 and 5 months and others reported between 7 and 12 months. However, a considerable number of participants knew they should introduce complementary food when the baby was six months old. One participants explained it as follows:
The baby should be exclusively breastfed up to six months following childbirth. During this time, the baby cannot be fed on staple food because he is still young. Only when the baby has completed six months he should be given other food rather than breast milk. (29 years old, mother of a child, age 11 months).
Participants from Manhiça district seem to have more accurate knowledge about the introduction of complementary food than participants living in Namaacha district. Almost half of the participants who correctly mentioned the recommended period of introducing complementary food was from Manhiça district. Only one third of participants from Namaacha district reported the right recommended period to introduce complementary food. Furthermore, participants between the ages of 18 and 34 with formal education, were more likely to know the recommended time (Table 3). Inversely, farmers or merchants without formal education, married or living with a partner, lacked knowledge of the recommended period.
Table 3. Knowledge of introduction of complementary food
Characteristics of participants |
Knowledge of introduction of complementary food |
Manhiça (n=34) |
Namaacha (n=25) |
2-5 months |
6 months |
7-9 months |
2-5 months |
6 months |
7-9 months |
Age range |
|
18-24 |
4 |
6 |
4 |
4 |
4 |
2 |
25-34 |
5 |
10 |
2 |
5 |
3 |
3 |
35-39 |
0 |
0 |
3 |
1 |
1 |
2 |
Educational Level |
|
None |
4 |
4 |
2 |
1 |
2 |
1 |
Less than primary education (1-6 years) |
3 |
3 |
2 |
1 |
2 |
3 |
Primary education completed (7 years) |
2 |
8 |
5 |
8 |
2 |
2 |
Secondary education completed (12 years) |
0 |
1 |
0 |
0 |
2 |
1 |
Marital Status |
|
Single |
0 |
3 |
2 |
4 |
2 |
1 |
Married/Living with a partner |
8 |
13 |
6 |
5 |
6 |
6 |
Divorced/Widow |
1 |
0 |
1 |
1 |
0 |
0 |
Number of Children |
|
1-2 |
7 |
10 |
3 |
5 |
6 |
3 |
3-4 |
2 |
4 |
5 |
2 |
2 |
3 |
5-6 |
0 |
2 |
1 |
3 |
0 |
1 |
Occupation |
|
Factor worker |
0 |
0 |
0 |
0 |
0 |
1 |
Farmer |
7 |
11 |
6 |
8 |
6 |
4 |
Housemaid |
0 |
1 |
1 |
1 |
0 |
0 |
Own business/sale |
2 |
2 |
2 |
0 |
0 |
1 |
Student |
0 |
2 |
0 |
1 |
0 |
1 |
Teacher |
0 |
0 |
0 |
0 |
2 |
0 |
Participants reported introducing complementary food when they perceived the baby had grown enough to digest other kinds of food. They also said at certain age, babies are not satisfied with only breast milk. Therefore, babies were given complementary food before the recommended duration of 6 months to enhance diet and enable their growth. The introduction of complementary food was also influenced by the knowledge the participants had about it. Some participants acquired knowledge from nurses during health education sessions at the postnatal period; as one participant narrated it:
I learnt from the nurse at the healthcare facility that a baby can only start eating complementary food when he is 6 months old because his stomach already needs other types of food. This is because the baby does not get satisfied with only breast milk. (39 years old, mother of a child, age 14 months).
However, the knowledge acquired form nurses was not often adequate. Some participants leaned that complementary food should be introduced at three months, following childbirth. This understanding was more common among mothers who attended some antenatal visits in South Africa. One of the participants explained how she learnt about introducing complementary food:
A baby can start eating complementary food when he is tree months old. I learnt about it from nurses at the healthcare facility, in South Africa. The nurses told me that I should give porridge to the baby whenever he is hungry, and when he completes 3 months. (33 years old, mother of a child, age 2 months).
Other participants acquired knowledge from their mothers, mothers-in-law or previous experience with breastfeeding and learned that they should introduce complementary food when the baby complete six months. One of the participants said:
The baby should start eating other kind of foods when he is 6 months old. I learnt that form my mother-in law. She advised me to give porridge because the baby used to cry a lot, and she told me that the baby was no longer satisfied with breast milk. Thus, I had to start giving him porridge. (20 years old, mother of a child, age 7 months).
Nonetheless the knowledge acquired from mothers and mothers-in-law or previous experiences of breastfeeding was not often adequate. Some participants learned they should introduce complementary food when the baby is 3 months, 7 months or 9 months; as the following narratives highlight:
I learnt from my ant that the baby should start eating other food different from breast milk when he is three months old. At this time his stomach can support other type of food. Besides, I noticed that the baby is very laze to suck and I think he can get hungry (…). I exclusively breastfeed until the baby completes three months, and thereafter I introduce other foods. (18 years old, mother of a child, age 12 years old).
I know that the baby should start eating other foods when he is 7 months old. I only know that from learned people from my family, such as brothers who went to school. They told me that the baby should start eating complementary food from this age [7 months]. (37 years old, mother of a child, age 6 months).
I think a baby should start eating other foods different from breast milk when he is 9 months. I learnt that from my own experience. I see that the baby gets satisfied with breast milk until now; but after sometimes, I know and see that the baby needs something else more than breast milk. By that time, I start giving porridge. (21 years old, mother of a child, age 5 months).
Practice of introduction of complementary food
Most participants who had infants between 6 and 18 months reported they introduced complementary food from six months onwards. However, other participants with infants younger than six months introduced complementary food between three and five months. Both participants reported introducing formula, water and traditional remedies before the baby was six months old.
Infants less than 6 months were fed breast milk or formula and porridge, pap and biscuits. Participants reported introducing complementary food earlier because of work, lack of money to buy formula, or problems producing enough breast milk for the baby; as one of the participants narrated.
I use both breast milk and formula to breastfeed the baby because he sucks only one breast and he does not get satisfied. I decided to use formula because he does not accept to suck another breast. I do not know why he does reject it. (24 years old, mother of a child, age 2 months).
As well, some participants said they introduced complementary food earlier because they perceived their infants were not satisfied with breast milk. In most instances, staple food was introduced before the age of 6 months; as one of the participants explained.
I use breast milk and food to feed the baby because he does not get satisfied only with breast milk and he does not accept to eat porridge. So, to complement breast milk, I give him food like that we eat every day. (30 years old, mother of a child, age 5 months).
Others observed earlier introduction of complementary food as a way to prepare breastfeeding cessation at 6 months. They perceived that introducing complementary food before 6 months would help the baby to get used to it. One of the participants explained it this way:
I have already introduced complementary food to the baby at 4 months as a way to prepare ceasing breastfeeding when he completes six months old. As the nurse advised me to stop breastfeeding at six months, I give him porridge so that he can get used to it. This will prevent me to stop breastfeeding abruptly when the baby completes six months. (19 years old, mother of a baby, age 4 months).
The most common complementary food among participants who had infants between 6 and 9 months were breast milk or formula and pap, porridge, bread, bananas, biscuits and family food. Infants between 10 and 12 months were fed breast milk or formula, pap and family food.
Participants said they introduced these kinds of complementary food because the infants had grown enough to eat other food rather than breast milk alone. Some participants said they introduced complementary food because they were HIV-positive and could not breastfeed after 6 months. Others simply stated that complementary food is an excellent nutritional source to enhance and maintain good weight gain of the infant.
Participants who continued breastfeeding after 6 months did not express or heat breast milk. They said they had not heard about doing this and nurses did not advise them to do it. However, some participants knew solid food such as family food – biscuits, banana and bread were not recommended for their infants between the ages of 6 and 9 months. But, they said, they did not have money to buy formula and pureed food for the baby. They reported giving their babies food available in their community, and in accordance to their economic conditions.
Decision-making on introduction of complementary foods
Most participants decided independently to introduce complementary food after learning to do so from nurses during antenatal and postnatal visits. But, for some, the decision was taken by other family members such as mothers, mothers-in-law, sisters-in-law, aunts and brothers.
Participants from Namaacha district were more likely to have decision-making power to introduce complementary food, compared to participants from Manhiça district. The decision to introduce complementary food in Manhiça district was mostly taken by the nurses (Table 4).
Table 4. Decision-making on introduction of complementary food
Characteristics of participants |
Decision-making on introduction of complementary food |
Manhiça (n=34) |
Namaacha (n=25) |
Myself |
Nurse |
Family |
Myself |
Nurse |
Family |
Age range |
|
18-24 |
3 |
8 |
3 |
5 |
1 |
4 |
25-34 |
10 |
6 |
1 |
10 |
2 |
0 |
35-39 |
1 |
1 |
1 |
2 |
1 |
0 |
Educational Level |
|
|
|
|
|
|
None |
5 |
1 |
4 |
1 |
1 |
2 |
Less than primary education (1-6 years) |
3 |
5 |
0 |
5 |
1 |
0 |
Primary education completed (7 years) |
6 |
8 |
1 |
9 |
1 |
2 |
Secondary education completed (12 years) |
0 |
1 |
0 |
2 |
1 |
0 |
Marital Status |
|
|
|
|
|
|
Single |
1 |
2 |
2 |
3 |
2 |
2 |
Married/Living with a partner |
13 |
11 |
3 |
13 |
2 |
2 |
Divorced/Widow |
0 |
2 |
0 |
1 |
0 |
0 |
Number of Children |
|
|
|
|
|
|
1-2 |
9 |
10 |
1 |
9 |
2 |
3 |
3-4 |
3 |
5 |
3 |
4 |
2 |
1 |
5-6 |
2 |
0 |
1 |
4 |
0 |
0 |
Occupation |
|
|
|
|
|
|
Factor worker |
0 |
0 |
0 |
1 |
0 |
0 |
Farmer |
10 |
11 |
3 |
13 |
3 |
3 |
Housemaid |
1 |
2 |
0 |
1 |
0 |
0 |
Own business/sale |
3 |
1 |
2 |
1 |
0 |
0 |
Student |
0 |
1 |
0 |
0 |
0 |
1 |
Teacher |
0 |
0 |
0 |
1 |
1 |
0 |
The difference between the two study sites with regard to the power decision making about complementary food might be linked to the influence of nurses over HIV-positive women and participants’ perceptions on when and who should take the decision of introducing complementary food.
Participants from Namaacha district most often perceived they had responsibility to decide when to introduce complementary food because they were the one who were taking care of the baby, as one of the participants said in a focus group discussion.
All the process of breastfeeding, including introducing complementary food to the baby, is under the responsibility of the mother. It is the mother who must feed and take care of the baby (…). Nurses are important [in the breastfeeding process] because they advise about what should be done [how to feed the baby] when the baby loses the weight. (35 years old, mother of 4 children).
Inversely, some participants from Manhiça district often perceived nurses should decide on when to introduce complementary food because nurses knew what was better for the baby. The responsibility of the mother was to feed the baby and take him/her to the healthcare facility, as one of the participants in a focus group discussion presented her view.
Nurses are very important during breastfeeding. They diagnosis and treat illness that the baby might have. This include HIV, tuberculosis, malaria and diarrhea. The mother must breastfeed according to the recommendation of the nurse to prevent the baby to get diarrhea and HIV. (…). When the nurses say: introduce this food or stop breastfeed; you have to obey, because they know why they are advising you that. The responsibility of the mother is to feed and take the baby to the healthcare facility to be diagnosed and treated. (29 years old, mother of 3 children).
Moreover, participants aged between 25 and 34 years old living in both districts were more likely to decide to introduce complementary food independently. Participants aged 18-24 years old reported that their family members or a nurse decide the introduction of complementary food.
Data also showed that some participants without formal education, particularly in Manhiça district, decided themselves to introduce complementary food; while other participants with formal education in the same district reported that the decision on introduction of complementary food was taken by the nurses. Nonetheless, some participants with formal education in Namaacha district took the decision to introduce complementary food independently. In both districts, most participants who were married and farmers also introduced complementary food themselves.
With regards to the number of children, participants who had between 1 and 4 children were more likely to decide themselves to introduce complementary food in Namaacha district; whereas participants with the same number of children in Manhiça district stated that the nurses and other members of the family took decision on when to introduce complementary food.
Knowledge of complete breastfeeding cessation
Most participants said all breastfeeding should end at 6 months after childbirth, regardless of their place of residence, age and level of education. However, some said breastfeeding ceased between three and five months, while others reported between seven and twelve months. A few stated all breastfeeding should be stopped between thirteen and twenty-four months.
From nurses, participants learned they should stop breastfeeding at six months. Conversely, others reported learning from their mothers and mothers-in-law, as well as their own previous experiences of breastfeeding.
Indeed, participants received varying recommendations from attendant nurses. Some nurses advised participants to cease complete breastfeeding at six months after childbirth. Yet, other nurses said the decision to end breastfeeding should come from the mothers themselves. These nurses maintained they only advised mothers to comply with six months of exclusive breastfeeding principle, not when they should fully stop feeding their babes in this manner. One of the nurses said:
We advise mothers to exclusively breastfeed their babies in the first six months after childbirth. We request them to introduce complementary foods at six months and continue breastfeeding. It is up to the mothers to decide when to stop complete breastfeeding after six months. The most important is that the mother should continue following antiretroviral therapy program. (Nurse).
Others nurses reported advising participants to introduce complementary food when the baby completes six months following childbirth, and thereafter continue breastfeeding. They said the mothers could stop breastfeeding after six months. However, they said all mothers should stop breastfeeding when the baby completes 16 months olds; as one nurse explained.
When the baby completes six months, mothers are advised to introduce complementary food such as porridge, fruits like papaw or others fruits available in the community. They should continue breastfeeding after introducing complementary food. They continue breastfeeding until they decide when they want to stop. However, we advise them to stop breastfeeding when the baby completes 16 months. (Nurse).
Participants who had previous experience of breastfeeding said nurses’ recommendations were different from their earlier experiences and knowledge of ending breastfeeding. Some participants reported being advised to stop breastfeeding between nineteen and twenty-four months for previous children. Some said they stopped breastfeeding their older children when they were twelve to eighteen months old. Yet others reported they had stopped breastfeeding after the child was three years old.
Several participants said they had breastfed longer because they were not yet HIV-positive and their HIV status influenced the duration of their breastfeeding. In a focus group discussion, participants said they strived to follow nurses’ advice, and stopped breastfeeding at six months to prevent HIV transmission to their infants.
Breastfeeding cessation experience
A considerable number of participants reported stopping breastfeeding when the baby reached 6 months of age while others continued breastfeeding well after 6 months. A considerable number of participants reported stopping breastfeeding due to their HIV-positive status. Participants were fear they could pass HIV to the infants, as one of the participants expressed her concern.
I stopped breastfeeding when the baby completed six months because I am sick [HIV positive]. The nurses advised me to stop breastfeeding when the baby reached six months following childbirth. I could not breastfeed longer because I could infect my baby. (26 years old, mother of a child, age 9 months).
Some participants ceased breastfeeding abruptly because nurses had advised them to immediately stop breastfeeding after a visit to the child at risk clinic. Participants said nurses advised them to stop breastfeeding after six months to prevent passing HIV to the baby. One participant explained it as follows:
I stopped breastfeeding the baby when he was six months old. Nurses advised me that I should stop breastfeeding because the baby was starting to get teeth and he could bite my nipples. This was dangerous because the baby could get my disease [HIV]. (26 years old, mother of a child age 10 months).
Other participants said they did not produce enough breast milk to continue breastfeeding, while others said the baby had grown enough and could be fed complementary food. However, a considerable number of participants with babies aged 7 months and more continued breastfeeding.
Participants who continued breastfeeding after 6 months said they were preventing illnesses in the baby such as stomach-ache and diarrhoea. In addition, they said breast milk was still important to help the baby to grow healthy after introduction of complementary foods. One participant said:
In my view, the baby must be breastfed up to 12 months to avoid disease for the baby. The breast milk also helps to open the mind of the baby so that he can be wise when he grows up. (22 years old, mother of a child, age 8 months).
Other participants continued breastfeeding because they did not have money to buy formula. Yet other mothers perceived that breast milk was healthy for the baby, especially to enhance his or her emotional health with continued physical bonding of mother and child. Some participants continued breastfeeding after 6 months and stopped when the infant completed seven months, following the recommendation of the nurses; as one participant explained.
I continued breastfeeding the baby after six months because the nurses advised me to do so. I had twins, but one died. So, the nurses advised me to breastfeed longer. That is why I stopped breastfeeding the baby when he was 7 months. (38 years old, mother of a child, age 13 months).
Decision-making power on breastfeeding cessation
Most participants said they had power to decide when to stop breastfeeding. However, others reported that nurses made the decision as to when to stop breastfeeding. Nevertheless, some participants said their husbands or other members of the family, such as mothers, mothers-in-law and grandmothers, decided on when to stop breastfeeding. In both districts, most participants decided to stop breastfeeding independently. Nonetheless, family members seem to have greater decision power on when to stop breastfeeding in Namaacha district than in Manhiça district. Inversely, nurses seem to have a greater influence on stopping breastfeeding among participants living in Manhiça district than in Namaacha district (Table 5).
Table 5. Decision-making power on breastfeeding cessation.
Characteristics of participants |
Decision-making power on breastfeeding cessation |
Manhiça (n=34) |
Namaacha (n=25) |
Myself |
Husband |
Nurse |
Family |
Myself |
My husband |
Nurse |
Family |
Age range |
|
18-24 |
11 |
2 |
1 |
0 |
3 |
4 |
0 |
3 |
25-34 |
8 |
6 |
2 |
1 |
5 |
4 |
1 |
1 |
35-39 |
2 |
0 |
1 |
0 |
3 |
1 |
0 |
0 |
Educational Level |
|
None |
6 |
3 |
0 |
1 |
2 |
0 |
1 |
1 |
Less than primary education (1-6 years) |
5 |
0 |
3 |
0 |
3 |
3 |
0 |
0 |
Primary education completed (7 years) |
10 |
4 |
1 |
0 |
4 |
5 |
0 |
3 |
Secondary education completed (12 years) |
0 |
1 |
0 |
0 |
2 |
1 |
0 |
0 |
Marital Status |
|
Single |
5 |
0 |
0 |
0 |
4 |
0 |
0 |
3 |
Married/Living with a partner |
14 |
8 |
4 |
1 |
6 |
9 |
1 |
1 |
Divorced/Widow |
2 |
0 |
0 |
0 |
1 |
0 |
0 |
0 |
Number of Children |
|
1-2 |
12 |
6 |
2 |
0 |
4 |
6 |
0 |
4 |
3-4 |
7 |
2 |
1 |
1 |
3 |
3 |
1 |
0 |
5-6 |
2 |
0 |
1 |
0 |
4 |
0 |
0 |
0 |
Occupation |
|
Factor worker |
0 |
0 |
0 |
0 |
1 |
0 |
0 |
0 |
Farmer |
15 |
5 |
4 |
0 |
7 |
8 |
1 |
3 |
Housemaid |
2 |
0 |
0 |
0 |
0 |
1 |
0 |
0 |
Own business/sale |
3 |
2 |
0 |
1 |
1 |
0 |
0 |
0 |
Student |
1 |
1 |
0 |
0 |
0 |
0 |
0 |
1 |
Teacher |
0 |
0 |
0 |
0 |
2 |
0 |
0 |
0 |
Data also reveal that participants of all ages have decision power on ceasing breastfeeding. However, family members still have decision-making power over participants aged 18 and 24 years old. Despite the important influence of the husband on stopping breastfeeding, a considerable number of participants who were married reported having power to decide to cease breastfeeding. As well, the more the number of children participants had, the more was the possibility to decide to stop breastfeeding independently.
Although nurses advised participants to stop breastfeeding at 6 months, some participants did not comply because they said their husbands did not accept this. They said they continued breastfeeding until their husbands told them to stop. One participant narrated the following:
Nurses recommend to stop breastfeeding when the baby completes six months. But when my baby completed six months my husband did not accept to cease breastfeeding. He did not buy formula and other complementary foods for the baby. He obliged me to continue breastfeeding. I ceased breastfeeding when my husband decided. The baby was twelve months old. I also started giving pap to the baby from six months. (31 years old, mother of a baby age 18 months).
The majority of participants were still on antiretroviral therapy during the breastfeeding period (Figure 2). They also reported following treatment of their infants. Some participants who had stopped breastfeeding said they were still taking antiretroviral drugs for their own life. As one participant explained:
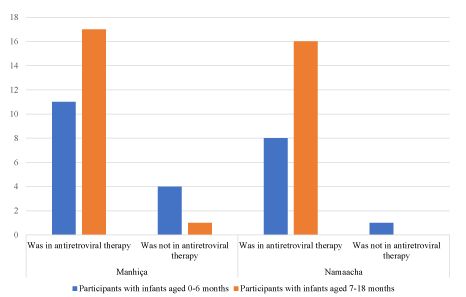
Figure 2. Adherence to antiretroviral therapy during breastfeeding period among the participants.
I completely ceased breastfeeding at six months. The first HIV test of my baby was negative. I am still taking antiretroviral because I know I have to take it until I die. I still take my baby to child risk centre until nurses tell me his final HIV status. (24 years old, mother of a baby age 12 months).
However, a few participants did not follow antiretroviral therapy. Some were still breastfeeding and reported they had interrupted taking antiretroviral drugs because they were away for two months in South Africa, visiting their husbands. They added they came to the healthcare facility for the child at risk clinic and to continue HIV treatment for themselves.
Other participants who had stopped taking antiretroviral drugs had also stopped breastfeeding. They said the nurses told them that their infants were free from HIV. Although they were advised to continue antiretroviral therapy from general clinic, they said they lacked money for transport. One participant explained it as follow:
I interrupted antiretroviral therapy three months ago because I had not money to come to the health facility. I stopped breastfeeding. My baby is still under control, but he did the test and he was considered HIV-negative. I have just come today [17-02-2015] to restart antiretroviral treatment at the general clinic. I know that I have to take antiretroviral for the rest of my life. (28 years old, mother of a baby, age 15 months).
Nurses explained that mothers received antiretroviral drugs from the maternal clinic when they were pregnant and from the child at risk clinic during the breastfeeding period. But when they stopped breastfeeding and a final HIV diagnosis of the infant was determined, they were discharged and advised to continue life-long antiretroviral treatment at the general clinic. Nurses said they had no control over the participants who were transferred from the child at risk clinic to the general clinic; as one nurse explained:
When a final HIV diagnosis of the infant is determined, the mother and the baby are discharged from the child at risk clinic. The mother is recommended to continue HIV treatment from the general clinic. She gets antiretroviral drugs from that clinic, and I have no control of this patient anymore. It is no longer my responsibility to take care of this patient. Other colleagues at the general clinic take care of the patients transferred from the child at risk clinic. She only comes back to this clinic when she gets pregnant and have a new baby. (Nurse).
However, some participants did not continue antiretroviral therapy at the general clinic immediately after receiving transference from the child at risk clinic. Nurses said mothers were less motivated because they thought their infants were not at risk of HIV infection. Moreover, they said some mothers felt physically healthy and did not really believe that they were living with HIV. Nurses said that typically, these women show up again at the healthcare facility when they were pregnant. One nurse explained as follows:
We often explain mothers that HIV treatment consists on adherence to life-long antiretroviral therapy. We advise them to continue taking antiretroviral drugs for their life, even after stopping breastfeeding. However, some mothers do not accept their HIV-positive status, they think they are HIV-positive because they are poor. These mothers are more vulnerable to stop taking antiretroviral drugs soon after ceasing breastfeeding. Some mothers who accept their HIV-positive status continue taking antiretroviral drugs after ceasing breastfeeding, but they soon stop when they feel physically health. We, at child at risk clinic, can only discover that some mothers did not continue with antiretroviral drugs after ceasing breastfeeding when they get pregnant and comeback to maternal child health clinic. (Nurse).
This narrative suggests that there is a gap between the process of discharging from the child at risk clinic and (re)integration in the general clinic. As nurses reported, they lacked control over patients when they moved from the child at risk clinic to the general clinic. Moreover, nurses added in most healthcare facilities they lacked the mechanisms to follow up whenever they realized patients missed a consultation for HIV treatment.
Most participants said sexual intercourse was resumed when the baby was between six and ten months. However, some suggested sexual intercourse could be resumed between three and five months, while others reported after twelve months. Participants perceived this as an acceptable period to resume sexual intercourse. This was because it was considered the baby had already grown up, passed the exclusive breastfeeding phase and the baby could not contract the disease due to the mother engaging in sexual intercourse. Nevertheless, some participants said they did continue breastfeeding after resuming sexual intercourse.
We have resumed sexual intercourse because the baby has grown up. The baby is already 7 months old, but I am still breastfeeding. Sexual intercourse is no longer dangerous to the baby. Before the baby completes six or seven months, sexual intercourse can cause problems such as diarrhoea and fever to the baby. (19 years old, mother of a child, age 9 months).
Indeed, most participants in the focus group discussion said sexual intercourse could not be resumed before 6 months because they believed the babies could get diarrhoea and fever. They said they acquired this knowledge from their mothers, grandmothers and mothers-in-law.
However, a considerable number of participants had resumed sexual intercourse between three and six months following childbirth. Some of these participants were still breastfeeding. This suggests that the perception of when to resume sexual intercourse varied according to when each participant perceived the “baby has grown up” and the decision-making power to resume sexual intercourse. As a matter of fact, most of the participants said the decision to resume sexual intercourse was made by their husbands. Only a few said the decision was made by consensus with their husbands, as one participant explained:
We [my husband and I] resumed sexual intercourse when the baby was 7 months old because we thought the baby has already grown up. The decision was based in consensus between my husband and myself. (22 years old, mother of a baby, age 8 months).
Some participants who had resumed sexual intercourse used contraceptive methods such as condoms or injections. However, very few participants used condoms. None of the participants reported using the dual method – injection with condoms or intrauterine devices with condoms. All participants said their husbands decided on what type of contraceptive methods would be used.
We use injection to prevent pregnancy because the baby was still young when we resumed sexual intercourse. The baby was 6 months old. My husband decided I should use injection to prevent pregnancy. (24 years old, mother of a baby, age11 months).
However, others resumed sexual intercourse and they did not use contraceptive methods because their husbands did not allow them neither did they accept to use a condom; as one participant explained.
We resumed sexual intercourse when the baby was 6 months. But, I am not using contraceptive methods because my husband does not allow me. He does not accept to use condom. (30 years old, mother of a baby, age 11 months).
Our findings suggest that compliance to the recommended medical advice among participants attending postnatal visits is influenced by a number of factors. These include perceptions, previous experiences, interaction with nurses, decision-making power on the introduction of complementary food, and breastfeeding cessation.
The study results call attention to the fact that participants often believe that complementary feeding should be introduced when the infant is grown up enough to eat other foods other than breast milk or formula. The perception of growing up and the type of food that is given to the baby however varies from participant to participant. Most participants decided themselves to introduce complementary food; while others followed nurses’ recommendations or family members’ advice. These finding reveal that infants feeding is a social and cultural practice as Bourdieu [30] suggested. It involves both individual and collective perceptions, the knowledge and experience of participants on complementary feeding; and how healthcare providers passed the information about complementary feeding to the participants.
Some participants ended breastfeeding at six months because they perceived breast milk as a potential source of passing HIV from mother to infant. Others however continued with breastfeeding since they viewed breast milk to be important for the psychological development of the infant. In many instances, these mothers were not aware that it was recommended to express their breast milk and heat it before feeding their infants, as this reduces the risk of HIV infection.
Introduction of complementary food before the age of six months was also documented by other studies in Mozambique [24] and Zambia [40]. Our findings however confirmed some participants introduced complementary food before 6 months to enhance the infants’ diet while others prepared themselves to end breastfeeding after 6 months. This practice is the result of poor knowledge about the recommended time to introduce complementary feeding and the recommended type of complementary food.
Further, the socioeconomic conditions of the participants influenced the type of food they use during the complementary feeding period. Some participants were aware that they were giving inadequate food to the baby but stated that they could not afford to do otherwise. Though most participants had decision-making power over the introduction of complementary food, they lacked adequate knowledge on when to introduce it. Introduction of inadequate complementary food has also been documented in Uganda [19] and Tanzania [18].
Furthermore, the study indicates some participants were subject to contradictory norms and lacked decision-making power. On one hand, they were advised by nurses to stop breastfeeding at six months and to introduce complementary food. Conversely, they were advised by family members to introduce complementary food earlier. Moreover, some were advised by their husbands and family members to continue with breastfeeding after six months or to stop breastfeeding at a time different from that recommended by the nursing staff. This lack of decision-making power influenced a considerable number of participants not to comply with the recommended prescriptions.
As well, the breastfeeding policy seems complex and it was abruptly altered. In 2012, it was recommended to conclude all breastfeeding at six months [13]. In 2013, the Mozambican Ministry of health recommended mothers should continue breastfeeding with modified breast milk and end all breastfeeding when the baby was one year old [11].
This unexpected change in recommendations affected nurses’ opinions. Some agreed with the change while others did not. In the end, nurses passed on the information they believed was correct to HIV-positive mothers, which thus influenced the compliance to the medical recommendations.
These findings corroborate with Bourdieu’s theory [30] about the existence of multiple factors that influence infant feeding. As he suggested, the position of the participants at the household and their economic conditions play an important role on when to introduce complementary food, the type of complementary food preferred and when to stop breastfeeding. The participants of this study were living in a family environment in which they had no power to decide on when to stop breastfeeding. Moreover, lack of money to buy the advised complementary food, and the need to strengthen the nutrition of the baby led participants to introduce inadequate complementary food. In addition, the ambiguity of breastfeeding policies, its constant change and the lack of training update among healthcare providers influenced the participants’ practices with regards to complementary feeding.
The majority of participants attended postnatal meetings and child at risk clinic visits. Nevertheless, some participants missed postnatal appointments and visits to the child at risk clinic due to a variety of challenges. These included, lack of money for transport, family problems, and lack of knowledge about the importance of postnatal visits to prevent passing HIV infection to the infant. This put several infants at risk of HIV infection because their mothers had missed the required medical follow ups.
Moreover, postnatal visits and child at risk clinic visits play an important role in the adherence to antiretroviral therapy because both mothers and infants access HIV treatment from the child at risk clinic. Our findings show that the majority of participants continued with antiretroviral therapy during and after stopping with breastfeeding. Nonetheless, few participants were not taking antiretroviral drugs regularly.
Participants seem to be less motivated to regularly continue with antiretroviral drugs due to a lack of money for transport, temporary migration, or when they knew their babies were not at risk of HIV infection. This result is congruent with other previous studies documenting challenges around keeping mothers on HIV treatment during the postpartum interval. This occurs throughout sub-Saharan Africa [41-45].
The transition from HIV treatment of the mother at the child at risk clinic to the general clinic seems to play an important role on adherence to antiretroviral therapy during postpartum period. This study’s findings show that participants did not immediately adhered to HIV treatment at the general clinic after they were transferred from the child at risk clinic. This gap plays an important role on life-long antiretroviral therapy. Thus, healthcare providers should design an appropriate mechanism to close the gap of HIV treatment between the child at risk clinic and general clinic.
Our study findings also reveal that participants did not adhere to contraceptive use, let alone the dual contraceptive use method, even though they had resumed sexual activity and were still breastfeeding. Typically, the male partner decided on the type of contraceptive to be used. Low adherence of contraceptive methods, including condom use during the postpartum period has also been documented in southern Mozambique [46], Zambia [47], and other sub-Saharan countries [48].
Limitation
Findings of this study are limited to the study setting and the selected participants. The study only included mothers attending postnatal visits during the study period. We did not include information on HIV-positive lactating mothers who did not attend postnatal visits.
This study suggest that participants complied with some recommended medical advice such as adherence to postnatal visits and child at risk clinics as well as taking prescription of antiretroviral drugs for the infant and themselves. However, they did not comply with the recommended time for the introduction of complementary food, the type of food according to the age of the infant and did not comply with the recommended period for breastfeeding cessation. Moreover, most participants did not adhere to contraceptive use and dual contraceptive use after resuming sexual activity.
Complementary feeding practices and breastfeeding cessation seem to be influenced by multiple factors, including the way participants perceive infant feeding, their socioeconomic conditions, previous experiences, advice from family, as well as a lack of knowledge about what practices could put infants at risk of HIV infection. In addition, factors such as the ambiguity of breastfeeding policies and the way the healthcare providers pass the information about the recommended medical advice to mothers influenced the participants’ practices.
These findings suggest several implications with regard to medical advice recommended in postnatal period. The first is that medical advice is often ambiguous and contradictory. Healthcare providers, for example, teach mothers that they can pass HIV to their infants through breastfeeding, but in turn, they advise mothers to breastfeed. This seem to create confusion among mothers, who subsequently engage into practices that can put the infants at risk of HIV infection.
Further, the recommended medical advice interfered with other sources of knowledge that most participants had, based on their own experience or their family’s experience with infant feeding. Moreover, some participants do not have decision-making power on when to introduce complementary food, ending breastfeeding or adhering to contraceptive use. Compliance to the recommended advice is therefore subjected to individual and collective perceptions as well as practices that are socially and culturally accepted in the community. This suggests that medical advice should also be disseminated among the relevant actors – male partners, mothers-in-law and grandmothers – rather than only to lactating mothers.
Lastly, but not least, these findings highlight that complementary feeding is influenced by mothers’ healthcare behaviour. Lack of adherence to postnatal visits and the child at risk clinic affected both the mothers and the infants. Mothers’ attitudes and practices are shaped by the knowledge – acquired in both family and healthcare providers – and experience of breastfeeding, as well as by the social and cultural norms about infant feeding. Factors influencing mother’s practice vary cross age, place of live, education, economic resources, access to accurate information about the recommended advice to prevent passing HIV to the infants and the decision-making power at the household about their own health and that of the infants.
The study recommends that all healthcare providers should be trained in a new protocol to ensure that mothers receive the same advice. Nurses must adequately educate mothers on the time of introduction of complementary food, expressing and heating breast milk, and the recommended type of complementary food; taking into account local socio-economic conditions and the cultural environment.
Partners of the mothers and other relevant actors – grandmothers and mothers-in-law – should be included in the health education to ensure that mothers receive the same support at the household. As well, nurses should promote peer support groups that should disseminate best breastfeeding practices for the new mothers within their local areas. Peer support groups should consist of mothers who have had children and successfully weaned their babies without infection. These groups could also support the new mothers to overcome challenges faced during breastfeeding.
Nurses should continue health education dealing with long life antiretroviral therapy and the benefits of dual contraceptive use during the postnatal period. They should explain to the mothers how compliance to this medical advice can prevent passing HIV from mother to child and contribute to longer life. To expand access of HIV treatment in the community, a travelling clinic should be put in place. This clinic would enable access to services to the mothers, their male partners and other members of the family/community, and it would reduce the distance and cost of travelling, and therefore ensure consistent adherence to antiretroviral therapy and infant care.
- De Cock KM, Fowler MG, Mercier E, de Vincenzi I, Saba J et al. (2000) Prevention of mother-to-child HIV transmission in poor resource countries. JAMA 283: 1174-1182. [Crossref]
- Joint United Nations Programme on HIV/AIDS (UNAIDS) (2016) HIV and AIDS estimates. Regional factsheets – African Eastern and Southern 2016. USA: Joint United Nation Program on HIV/AIDS.
- Peltier CA, Ndayisaba GF, Lepage P, Griensven JV, Leroy V, et al. (2009) Breastfeeding with maternal antiretroviral or formula feeding to prevent HIV postnatal mother-to-child transmission in Rwanda. AIDS 23: 2415-2423. [Crossref]
- Mofenson LM (2010) Antiretroviral drugs to prevent breastfeeding HIV transmission. Antiviral Therapy 15: 537-553. [Crossref]
- Mclntyre J (2010) Use of antiretroviral during pregnancy and breastfeeding in low-income and middle-income countries. Curr Opin HIV AIDS 5: 48-53. [Crossref]
- WHO (2013) Consolidated guidelines on the use of antiretroviral drugs for the treating and preventing HIV infection. Recommendations for a public health approach. [pdf] Geneva: WHO. Available at: www.who.int/iris/bitstream/10665/85321/1/9789241505727_eng.pdf [Accessed 15 May 2014].
- WHO, UNICEF (2003) HIV and infant feeding. A guide for health-care managers and supervisors. [pdf]. Geneva: WHO. Available at: www.who.in/nutrition/publication/HIV_IF_guide_for_healthcare.pdf [Accessed 20 February 2014].
- Leroy V, Karon JM, Alioum A, Ekpini ER, Medas N, et al. (2002) Twenty four months efficacy of a maternal short-course zidovudini regimen to prevent mother-to-child transmission of HIV-1 in West Africa. AIDS 16: 631-641. [Crossref]
- Coustsoudis A, Pillay K, Khun L, Spooner E, Tsai W, et al. (2001) Method of feeding and transmission of HIV-1 from mothers to children by 15 months of age: prospective cohort study from Durban, South Africa. AIDS 15: 379-387. [Crossref]
- De Schacht C, Mabunda N, Ferreira Jr, OC, Ismael N, Calú N, et al. (2014) HIV incidence in the postpartum period sustains vertical transmission in settings with generalized epidemics: a cohort study in Southern Mozambique. J Int AIDS Soc 17: 18808. [Crossref]
- Ministério da Saúde (MISAU) (Ministriy of Health) (2013) Política Nacional de alimentação infantil. Maputo: MISAU.
- Ministério da Saúde (MISAU) (Ministriy of Health) (2014) Prevenção da transmissão vertical do HIV. Manual do bolso. Maputo: MISAU.
- Ministério da Saúde (MISAU) (Ministriy of Health) (2012) Manual de referência de saúde. Formação de provedores de saúde em prevenção positive. [pdf] Maputo: MISAU. Available at: www.ensinoadistancia.ed.moz/sites/default/files/MANUALREFERÊNCIAPREVENÇÃO POSITIVA_part1_0.pdf [Accessed 10 May 2014].
- Israel-Ballard KA, Abrahams BF, Coustsoudis A, Sibeko LN, Cheryk LA et al. (2008) Vitamin content of breast milk form HIV-1-infected mothers before and after flash-heat treatment. J Acquir Immune Defic Syndr 48: 444-449. [Crossref]
- Instituto Nacional de Estatística (National Isntitute of Statistic) (INE) and MISAU, 2013. Inquérito Demográfico e de Saúde 2011. [pdf] Maputo: MISAU. Available at: www.dhsprogram.com/pubs/pdf/PR14/PR14.pdf [Accessed 15 March 2014].
- Akter S, Rahman MM (2010) The determinants of early cessation of breastfeeding in Bangladesh. World Health Popul 11: 5-12. [Crossref]
- Haile D, Belaschew T, Birhanu G, Setegn T, Biadgilign S (2014) Predictors of breastfeeding cessation among HIV infected mothers in Southern Ethiopia: A survival analysis. PLoS ONE 9: e90067. [Crossref]
- Williams AM, Chantry C, Geubbels EL, Ramaiya AK, Shemdoe AI, et al. (2015) Breastfeeding and complementary feeding practices among HIV-Exposed infants in coastal Tanzania. J Hum Lact 32: 112-122. [Crossref]
- Fadnes L, Engebretsen IMS, Wamani H, Semiyaga NB, Tylleskar T, et al. (2009) Infant feeding among HIV-positive mothers and the general population mothers: comparison of two cross-sectional surveys in Eastern Uganda. BMC Public Health 9: 124. [Crossref]
- Kimani-Murage EW, Maldise NJ, Fotso J, Kyobutungi C, Mutua M, et al. (2011) Patterns and determinants of breastfeeding and complementary feedings practices in urban informal settlements, Nairobi, Kenya. BMC Public Health 11: 396. [Crossref]
- Becquet R, Leroy V, Ekouevi DK, Viho I, Castetbon K, et al. (2005) Complementary feeding adequacy in relation to nutritional status among early weaned breastfed children who are born to HIV-infected mothers: ANRS1201/1202 Ditram Plus, Abidjan, Côte d’Ivoir. Pediatrics 117: e701-10.
- Ogbo FA, Agho KE, Page A (2015) Determinants of suboptimum breastfeeding practices in Nigeria: evidences from the 2008 demographic and health survey. BMC Public Health 15: 259.
- Alzaheb RA (2016) Factors associated with the early introduction of complementary feeding in Saudi Arabia. Int J Environ Res Public Health 13: E702. [Crossref]
- Arts M, Geelhoed D, De Schacht C, Prosser W, Alons C, et al. (2011) Knowledge, Beliefs, and Practices Regarding Exclusive Breastfeeding of Infants Younger Than 6 Months in Mozambique. A qualitative study. J Hum Lact 27: 25-32. [Crossref]
- Homsy J, Moore D, Barasa A, Were W, Likicho C, et al. (2010) Breastfeeding, mother-to-child HIV transmission, and mortality among infants born to HIV-infected women on highly active retroviral therapy in rural Uganda. J Acquir immune defic syndr 53: 28-35. [Crossref]
- Mengstie A, Tadese T, Tessema B (2016) Assessment of factors associated with infant and young feeding practices of human immunodeficiency virus (HIV) positive mothers in selected hospitals of southern nations, nationalities and peoples (SNNPR) Ethiopia. Journal of AIDS and HIV research 8: 80-92.
- Kuhn L, Aldrovandi GM, Sinikala M, Knikasa C, Semrau K, et al. (2008) Effect of early, abrupt weaning on HIV-free survival of children in Zambia. N Engl J Med 359: 130-141. [Crossref]
- Nachega JB, Uthman OA, Anderson J, Peltzer K, Wampold S, et al. (2012) Adherence to antiretroviral therapy during and after pregnancy in low-income, middle-income, and high-income countries: a systematic review and meta-analysis. AIDS 26: 2030-2052. [Crossref]
- Phillips T, Thebus E, Bekker L, Mcintyre J, Abrams EJ, et al. (2014) Disengagement of HIV-positive pregnant and postpartum women from antiretroviral therapy services: a cohort study. J Int AIDS Soc 17: 19242. [Crossref]
- Bourdieu P (1984) Distinction. A social critique of the judgement of taste. Harvard University Press, Massachusetts.
- Delormier T, Frohlich KL, Potvin L (2009) Food and eating as social practice. Understanding patterns as social phenomena and implications for public health. Sociol Health Illn 31: 215-228. [Crossref]
- Afflerback S, Carter, SK, Anthony AK, Grauerholz L (2013) Infant feeding in the age of intensive mothering and risk society. Journal of consumer culture 13: 1-19.
- Schmied V, Lupton D (2001) Blurring the boundaries: breastfeeding and maternal subjectivity. Sociology of health and Illness 23: 234-250.
- Shaw R (2004) Performing breastfeeding: embodiment, ethics and the maternal subject. Feminist review 78: 99-116.
- Bourdieu P (1977) Outline of a theory of practice. Cambridge University Press, USA
- INE (2010) Projeções anuais da população total, urbana e rural dos distritos da província de Maputo 2007-2040 [pdf]. Maputo: Instituto Nacional de Estatística. Avaible at: http://www.ine.gov.mz [Accessed 10 January 2015].
- INS, INE, ICF(2010) Inquérito Nacional de Prevalência, Riscos comportamentais e Informação sobre o HIV e SIDA em Moçambique (INSIDA) 2009 [pdf]. Maputo: INS/MISAU. Available at: http://www.dhsprogram.com/publication/publication-FR266-DHS-Final-Reports.cfm [Accessed 20 March 2014].
- Charmaz K (2006) Grounded Theory: A practical research guide through qualitative Analysis. Sage Publications, London.
- Bram V, Clarke V (2006) Using Thematic analysis in Psychology. Qualitative research in Psychology 3: 77-101.
- Katepa-Bwalya M, Mukonka V, Kankasa C, Masaninga F, Babaniyi O, et al. (2015) Infants and young children feeding practices and nutritional status in two districts of Zambia. Int Breastfeed J 10: 5. [Crossref]
- Hodgson I, Plummer ML, Konopka SN, Colvin CJ, Jonas E, et al. (2014) A systematic review of individual and contextual factors affecting ARTs initiation, retention and retention for HIV-infected pregnant and postpartum women. PLoS One 11: e111421. [Crossref]
- Okawa S, Chirwa M, Ishikawa N, Kapyata H, Msiska CY, Syakantu G, Myano S, Komada K, Jimba M, Yasuoka J (2015) Longitudinal adherence to antiretroviral drugs for preventing mother-to-child transmission of HIV in Zambia. BMC Pregnancy and Childbirth 15: 258. [Crossref]
- Myer L, Philips TK, Zerbe A, Ronan A, Hsiao N, et al. (2016) Optimizing antiretroviral therapy (ART) for maternal and health child (MCH): rational and design of the MCH-ART study. J Acquir Immune Defic Syndr 72: s189-s196. [Crossref]
- Haas AD, Msukwa M, Egger M, Tenthani L, Thweya H, et al. (2016) Adherence to antiretroviral therapy during and after pregnancy: Cohort study on women receiving care in Malawi’s Option B+ program. Clin Infect Dis 63: 1227-1237. [Crossref]
- Geldsetzer P, Yapa HMY, Vaikath M, Ogbuoji O, Fox MP, et al. (2016) A systematic review of interventions to improve postpartum retention of women in PMTCT and ART care. J Int AIDS Soc 19: 20679. [Crossref]
- Agadjanian V, Hayford SR (2009) PMTCT, HAART and childbearing in Mozambique: An institutional perspective. AIDS Behav 13: S103-S112. [Crossref]
- Hancock NL, Chibwesha CJ, Bosomprah S, Newman J, Mubiwana-Mbewe M, et al. (2016) Contraceptive use among HIV-infected women and men receiving antiretroviral therapy in Lusaka, Zambia: a cross-sectional study. BMC Public Health 16: 392. [Crossref]
- Blazer C, Prata N (2016) Postpartum Family Planning: current evidence on successful intervention. Open Access J Contracept 7: 53-67. [Crossref]


