cerebral venous thrombosis, isolated cortical venous thrombosis, T2*- T2-GRE sequence, susceptibility imaging, migraine
While rare, with an estimated annual incidence of 4 cases per million and accounting for only 0.5% of all strokes, cerebral venous thrombosis (CVT) is a challenging diagnosis. Isolated cortical venous thrombosis (ICoVT), a rare presentation of CVT, is even more difficult to diagnose [1,2]. We report 2 cases that illustrate pitfalls in this condition.
A 39-year-old woman, with a medical history was significant for migraine headaches, presented to our Hospital with a 7-day history of frontal headaches, mild in intensity. Her only medication was an estrogen-based oral contraceptive pill (OCP). At admission, neurologic examination was unremarkable. Laboratory studies showed complete blood count, basic metabolic panel within normal limits.
A brain CT scan without contrast revealed on the last slice, a hyperdense serpiginous vessel in the left frontal lobe, ie a “cord sign”, thus suggesting a diagnosis of a thrombosed frontal cortical vein (Figure 1a, arrow). On brain MR imaging on a 3T scan the conventional sequences were normal: T1-weighted-image (T1WI), T2-weighted-image (T2WI), fluid- attenuated inversion recovery (FLAIR) and diffusion-weighted imaging (DWI). Susceptibility-weighted imaging (susceptibility-weighted angiography, SWAN sequence) (Figure 1b), showed a dark serpiginous vessel in the area relative
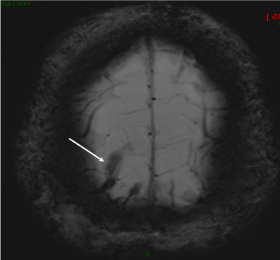
Figure 1a. Axial non-contrast CT scan of the brain shows, on the “last slice” a hyperdense serpiginous structure at the left frontal convexity, consistent with a thrombosed cortical vein
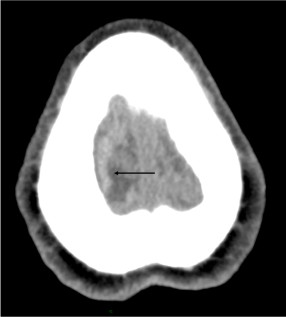
Figure 1b. susceptibility-weighted angiography (SWAN sequence) shows a dark tubular structure at the frontal convexity, compatible with a thrombosed right frontal vein. Note the blooming effect of this sequence
to that of the “cord sign” on the non-contrast CT, confirming the diagnosis of thrombosed frontal vein. 3-Dimmensional contrast-enhanced T1WI MRI sequence (CE 3D T1) showed on multiformat reformat (MPR) an intraluminal-filling defect surrounded by contrast in a left frontal vein at the same level (Figure 1c, arrow), suggestive of an intraluminal thrombus.
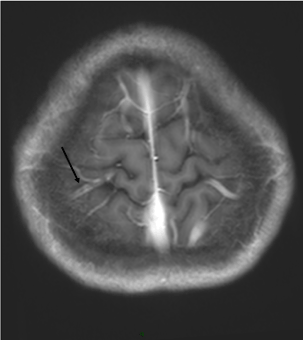
Figure 1c. Dimmensional contrast-enhanced T1WI MRI sequence (CE 3D T1) shows on multiformat reformat (MPR) an intraluminal-filling defect surrounded by contrast in a left frontal vein (arrow). Compare with the opposite side: the filling of the cortical vein by the contrast is complete
Coagulation studies normal including lupus anticoagulant, homocysteine, thrombin time, antithrombin activity, prothrombin mutation, factor V Leiden, serum anticardiolipin antibodies (IgA, IgM, IgG), protein C and protein S were unremarkable.
Thoracic and abdominopelvic CT showed no evidence of malignancy.
A 33-year-old man, without past medical history, presented 3 days after a lumbar puncture for an isolated neurological syndrome (right-sided upper extremity ataxia)
nausea, photophobia, and throbbing frontal headache with rapidly progressing intensity, that was positional in nature. A diagnosis of PDPH was established. After failure of appropriate treatment to resolve the headache, the patient underwent Brain CT, considered as “normal”, and subsequently a Brain MRI.
On contrast-enhanced MRV (CE MRV) a hypoplastic- atretic right lateral sinus (Figure 2a, arrow) was misdiagnosed as a sinus venous thrombosis, despite the absence of hypointense signal at the site of the right lateral sinus, and the patient was referred to our hospital to be managed. T2* (T2 gradient recalled echo sequence = T2 GRE sequence) revealed a dark cord in the left frontal area (Figure 2b, arrow), consistent with the diagnosis of frontal cortical venous thrombosis and on FLAIR sequence a hypersignal within the central sulcus (Figure 2c, arrow), related to a convexity subarachnoid hemorrhage (cSAH). The 3D CE T1 sequence showed a filling defect within the cortical vein (Figure 2d, arrow) visible as a dark serpentine structure on T2* (T2 GRE) sequence.
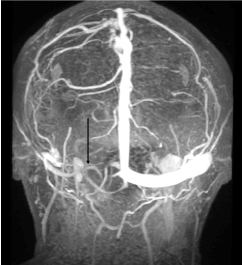
Figure 2a. Post-contrast MR venography (MRV) shows an atretic right lateral sinus (arrow)
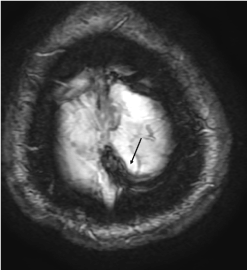
Figure 2b. T2* (T2 GRE) sequence shows on the “last slice” a serpentine, tubular structure of dark hypointense signal, compatible with a cortical vein thrombosis (arrow). Note the blooming effect of this sequence
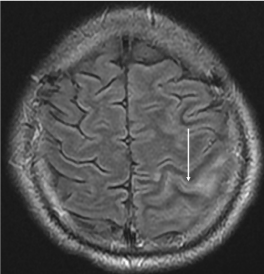
Figure 2c. FLAIR sequence shows a hypersignal within the central sulcus, indicating a convexity subarachnoid hemorrhage (cSAH) (arrow)
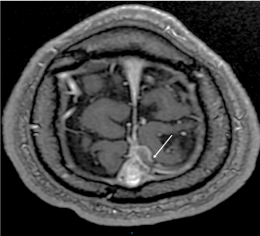
Figure 2d. Dimmensional contrast-enhanced T1WI MRI sequence (CE 3D T1) shows on multiformat reformat (MPR) an intraluminal-filling defect surrounded by contrast in a left frontal vein (arrow)
In both cases, anticoagulation was started with low-molecular-weight heparin (LMWH) that was switched to warfarin with an international normalized ratio (INR) target range of 2.0 to 3.0. Three-month follow-up brain MRI showed the disappearance of the anomalies on susceptibility imaging and complete recanalization of the occluded vein on CE 3D T1 sequence. The patients had a good outcome.
Many aspects of the 2 reported cases are interesting, showing that ICoVT have clinical and radiological pitfalls.
From a clinical point of view, as shown in Case 1, ICoVT may present as isolated migraine-like headache and be easily missed. The misdiagnosis can lead to a clinical worsening and aggressive management.
In Case 2 complaints and clinical findings were consistent with an orthostatic headache that appeared as a result of dural puncture, i.e. compatible with post-dural puncture headache (PDPH). In PDPH, if the headache persists and does not respond to treatment the diagnosis of CVT should be discussed, particularly in a young woman at risk, and imaging, at best a brain MRI should be performed to guide diagnosis. And it should be remembered that the use of a needle with a small diameter reduces the incidence of PDPH [3]. It is important to underline that dural puncture can cause intracranial hypotension, which may represent an additional risk factor for CVT [4]. The association CVT - PDPH has only been mentioned in a few case reports.
From a radiological point of view, in both cases the ICoVT was identified only on the “last slice”, on non-contrast CT and on susceptibility MR images. It should be reminded here that the optimal sequence for diagnosis of ICoVT, as reported by several authors, is the susceptibility sequence which allows the diagnosis at the hyperacute phase. MRV cannot identify them, given the size and anatomic variability of cortical veins [2,5]. In addition, in Case 2 a concurrent cSAH, limited to 1 sulcus was present in the vicinity of the cortical vein thrombosis [6]. CVT and ICoVT are one of the causes of cSAH [6,7].
In CVT, isolated headache is frequent and may masquerade in a common migraine presentation or be attributed to a dural puncture, that may represent a risk factor. The clinicians, especially in emergency department, radiologists should remember not to miss the last slice on brain imaging, CT scan and/or MRI.
None declared
All authors had access to the data and played a role in writing this manuscript.
The authors have no conflict of interest.
- Idbaih A, Boukobza M, Crassard I, Bousser MG, Chabriat H (2006) MRI of clot in cerebral venous thrombosis: high diagnostic value of susceptibility-weighted images. Stroke 37: 991-995.
- Boukobza M, Crassard I, Bousser MG, Chabriat H (2009) MR imaging features of isolated cortical vein thrombosis: diagnosis and follow-up. AJNR Am J Neuroradiol 30: 344-348.
- Arevalo-Rodriguez I, Muñoz L, Godoy-Casasbuenas N, Ciapponi A, Arevalo JJ, et al. (2017) Needle gauge and tip designs for preventing post-dural puncture headache (PDPH). Cochrane Database Syst Rev 4: CD010807.
- Honig A, Eliahou R, Pikkel YY, Leker RR (2016) Iatrogenic intracranial hypotension and cerebral venous thrombosis. J Neurol Sci 366: 191-194.
- Ihn YK, Jung WS, Hwang SS (2013) The value of T2*-weighted gradient-echo MRI for the diagnosis of cerebral venous sinus thrombosis. Clin Imaging 37: 446-50.
- Boukobza M, Crassard I, Bousser MG, Chabriat H (2016). Radiological findings in cerebral venous thrombosis presenting as subarachnoid hemorrhage: a series of 22 cases. Neuroradiology 58:11-16.
- Graff-Radford J, Fugate JE, Klaas J, Flemming KD, Brown RD, et al. (2016) Distinguishing clinical and radiological features of non-traumatic convexal subarachnoid hemorrhage. Eur J Neurol 23: 839-846.







