Migraine is quite common neurological disorder posing significant disability. It is a neurovascular disorder with genetic predisposition. Migraine and stroke have complex relationship with each other. The stroke has been reported with Migraine with aura. The migraine is a risk factor for stroke and stroke can be comorbid illness with migraine. Cerebral venous thrombosis is relatively uncommon neurological disorder, which contributes to 0.5-1 % of all types of stroke. The case report highlights the young female, who had cerebral venous thrombosis associated with Migraine with aura. The venous stroke in Migraine has not been reported in the literature.
migraine with aura, venous stroke, prothrombotic state, cerebral venous thrombosis, headache
Migraine is one of the commonest neurological disorder encountered by physicians. It affects around 20% of the females and 12% males of the normal population. It is a genetically determined, neurovascular disorder having complex pathophysiology [1]. Cerebral venous thrombosis is a rare type of stroke, which affects 0.5-1% of all types of strokes .Cerebral venous thrombosis presents with varied neurological manifestations, which include headache, seizures, altered sensorium, focal neurological deficits and intracranial hypertension. There are various infective and non infective conditions associated with cerebral venous thrombosis [2].
Migraine has very intricate relationship with stroke. The literature revealed that migraine can be a risk factor, having causal association and may act as comorbid factor with ischemic stroke. Migraine can be regarded as an epiphenomenon of complex vasculopathy [3]. In this case report, we intend to report a case of Migraine with aura, who presented with cerebral venous thrombosis. The migraine as a cause of venous stroke has not been mentioned in the literature.
A 24 year old, previously healthy female presented with severe headache of 4 days duration.It started with right side of forehead, then radiating to right neck region. It was associated with visual aura, scintillating scotoma, vomiting & photophobia. She was a diagnosed case of migraine with aura and was taking medications as acute abortive therapy and prophylaxis, intermittently for last 3-4 years. She was suffering from oligomenorrhea, for which she was advised Oral Contraceptive Pills for last 3 months. During the phase of migraine headache preceded by visual aura, after 3 days, she felt tingling & numbness of left side of body, followed by weakness of the same side of body. She was admitted to neurology department of our hospital. On day 3, post admission, she complained of blurring of vision.
On clinical examination, her vitals were within normal limits. The patient was well conscious and responding to verbal commands. Her visual acuity was 6/9 in both eyes. Her pupils were normal in size and reacting to light. Fundus examination revealed bilateral, severe papilledema (grade 4 fisher’s grading) (Figure 1). Other cranial nerves were normal on examination. Motor examination showed reduced power on left side of the body (3/5 MRC grading). The plantar reflex showed flexor response on right and extensor on left side.
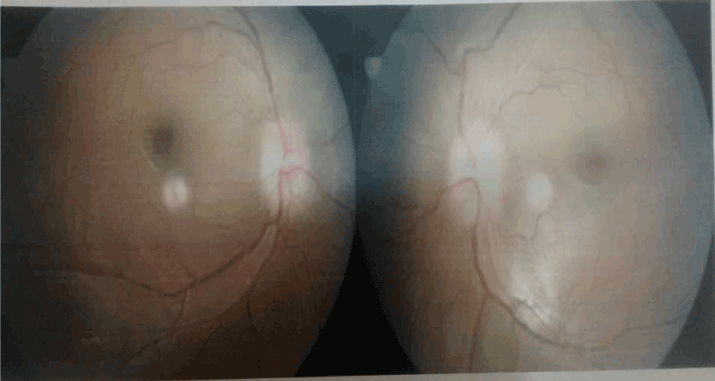
Figure 1. Fundus photograph showing bilateral papilledema.
The hematological parameters revealed normal results. The biochemical indicators which include liver function test, renal assessment, blood sugar, lipid profile and thyroid study were unremarkable. The serological test for HBsAg, HCV, HIV I & II were non reactive. Cerebrospinal fluid examination showed total number of cells 5/Cumm (all lymphocytes), protein 32 mg%, and sugar 46 %.
Gram’s stain, Acid fast bacilli stain and Indian ink preparation were negative for bacteria, mycobacterium tuberculosis and fungi respectively. CSF virology was negative for HSV, Japanese encephalitis virus, Dengue and Entero virus.
The assessment for procoagulant state, showed Protein C (85%) & Protein S (90%) and were within normal limits .Factor 5 Leiden mutation and MTHFR study revealed normal results. Serum homocysteine level was within normal range (11.98 ng/dl). MRI (Cranium) with venogram study demonstrated occlusion of superior sagittal sinus, inferior sagittal sinus and right transverse sinus. Diffusion Weighted Image showed, acute infarct in right parieto temporal area (Figure 2).
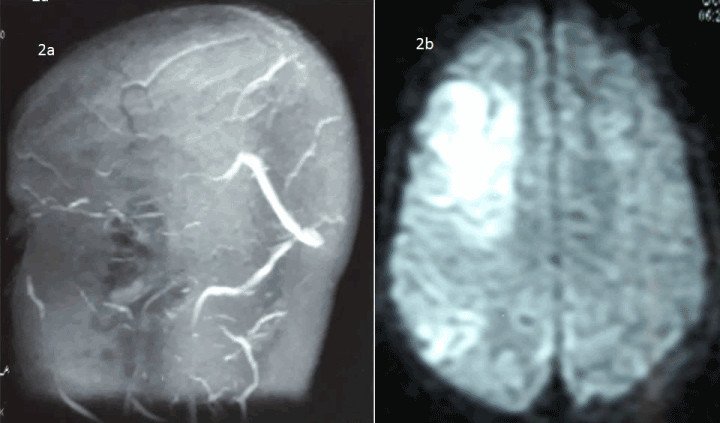
Figure 2. MRI (Cranium) with venogram study demonstrated non-visualization of superior sagittal sinus, inferior sagittal sinus and right transverse sinus (2a), Diffusion Weighted Image revealed acute infarct in right parieto temporal area (2b).
With this clinical assessment and neuroimaging findings, the diagnosis of cerebral venous thrombosis was considered. Since the ictus happened during headache phase of Migraine, Migraine associated stroke could be the possibility in our patient.
She was started on enoxaparin 0.6 mg twice a day for 5 days, overlapped with warfarin on day 2, with appropriate therapy for Migraine. Other supportive measures were taken and raised intracranial pressure was treated with decongestants. The contraceptives were withdrawn. The patient responded well to the treatment and regained her power in span of 7 days. Prothrombin Time (INR) was monitored at regular intervals.
After one and half months, she complained of multiple rash on her body. We suspected anticoagulation related bleeding diathesis. The International Normalized ratio was 13.5 seconds. The platelets count was within normal limits. The anticoagulants were stopped immediately and patient was hospitalized. Fortunately, there were no other serious hemorrhagic events and INR was normalized after 4 days. The follow up MRI Venogram study demonstrated recanalization of venous sinuses (Figure 3). At follow up after 6 months, she was in perfect health and her migraine also get controlled with prophylactic therapy.
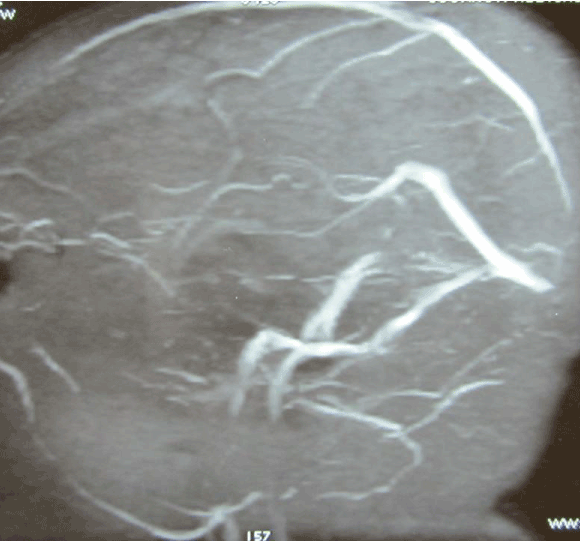
Figure 3. Repeat MRI (Venogram) study exhibited recanalization of sinuses.
Cerebral venous thrombosis is relatively uncommon condition, which contributes to 0.5-1 % of all types of stroke. Cerebral venous thrombosis has multitude of clinical manifestations and that’s why the diagnosis in early stages become difficult. The various predisposing conditions reported are pregnancy, oral contraceptives use, hypercoagulable state, malignancy and infections [4]. The infection constitutes a small group, causing cerebral venous thrombosis. The literature mentioned about various type of infections associated with venous stoke. The dehydration could be the important inciting factor for cerebral venous thrombosis [5].
Migraine is a common chronic headache disorder frequently encountered by physicians and neurologists. The various epidemiological studies state, that the prevalence of migraine in general population is estimated to be around 6 to13%.It is more common in females as there is complex relationship of Migraine with female hormones [6].
Our patient presented with cerebral venous thrombosis associated with migraine. Interestingly, the venous stroke happened during episode of headache with prolonged aura. The relationship between migraine and stroke is quite complex in nature. The various epidemiological studies have established that migraine can be one of the risk factors for ischemic stroke. On the other hand, migraine can cause stroke, substantiated by many large scale studies [7].
The meta-analysis discerned that pooled relative risk of stroke in patients with migraine was 2.16,95% Confidence interval 1.89-2.48 [8]. Migraine with aura is much more causally related with ischemic stroke as compared with migraine without aura category. Our patient was on oral contraceptives at the time of presentation. The risk of stroke has 8 fold increase in migraine subjects who were using oral contraceptives [9].
There are certain criteria described for Migrainous infarction. It should occur during an attack of migraine with aura, presence of focal neurological deficits lasting for more than 1 hour and neuroimaging should demonstrate infarction [10]. Uncommonly, migraine and stroke can be part of various clinical syndromes like, CADASIL, MELAS and hereditary endotheliopathy, retinopathy, nephropathy, and stroke (HERNS) [11].
The pathophysiological factors related to increased predisposition for stroke in migraine have been well described through elegant studies. Migraine and stroke are interlinked with 3 important factors, which include Leo cortical spreading depression, vasoconstriction and hypercoagulable state [12]. The community studies have highlighted certain factors which are shared by patients with migraine and stroke. The factors mentioned are hypertension, impaired lipid profile, increase body mass index (BMI), insulin resistance, and presence of metabolic syndrome, increase homocysteine level and coronary artery disease [13].
Inflammatory markers have shown to be elevated during migraine episodes: CRP, proinflammmatory cytokines and associated with vasoconstriction, endothelial dysfunction [14].
This patient was suffering from migraine with aura and presented with CVT probably potentiated by oral contraceptives. Migraine is now known for having hypercoagulable state. This has been explained by increased platelet aggregation property, elevated levels of platelet-activating factor (PAF) and Von Willebrand factor. The oral contraceptives exacerbated this prothrombotic state leading to CVT [15].
The anticoagulants are mainstay of treatment in CVT and this patient completely recovered within span of one month. The anticoagulants should be administered even in presence of hemorrhagic infarction [16].
In conclusion, Migraine and stroke are interlinked through well-defined pathophysiological factors. The literature well mentioned about relationship between migraine and arterial strokes. However, venous stroke associated with Migraine is not reported in literature. There should be high index of suspicion of CVT, if any individual suffering from Migraine with aura developed persistent focal neurological deficits and unusual headache during headache phase of Migraine. The early diagnosis results in good clinical outcome.
- Horev A, Wirguin I, Lantsberg L, Ifergane G (2005) A high incidence of migraine with aura among morbidly obese women. Headache 45: 936–8. [Crossref]
- Bousser MG, Ferro JM (2007) Cerebral venous thrombosis: an update. Lancet Neurol 6: 162–170. [Crossref]
- Tietjen GE (2005) The risk of stroke in patients with migraine and implications for migraine management. CNS Drugs 19: 683–92. [Crossref]
2021 Copyright OAT. All rights reserv
- Kashyap AS, Anand KP, Kashyap S (2005) Thrombosis of the cerebral veins and sinuses. N Engl J Med 353: 314–315.
- Saadatnia M, Fatehi F, Basiri K, Mousavi SA, Mehr GK (2009) Cerebral venous sinus thrombosis risk factors. Int J Stroke 4: 111–23. [Crossref]
- Lipton RB, Bigal ME, Diamond M, Freitag F, Reed ML, et al. (2007) Migraine prevalence, disease burden, and the need for preventive therapy. Neurology 68: 343-349. [Crossref]
- Curtis KM, Mohllajee AP, Peterson HB (2006) Use of combined oral contraceptives among women with migraine and nonmigrainousheadaches:a systematic review. Contraception 73: 189-194. [Crossref]
- Spector JT, Kahn SR, Jones MR, Jayakumar M, Dalal D, et al. (2010) Migraine headache and ischemic stroke risk: an updated meta-analysis. Am J Med 123: 612–24. [Crossref]
- MacClellan LR, Giles WH, Cole J, Wozniak M, Stern B, et al. (2007) Probable migraine with visual aura and risk of ischemic stroke: The Stroke Prevention in Young Women Study. Stroke 38: 2438–45. [Crossref]
- Headache Classification Committee of the International Headache Society (2004) The international classification of headache disorders, 24. Cephalalgia, (2ndedn), 9–160.
- Stam AH, Haan J, van den Maagdenberg AM, Ferrari MD, Terwindt GM (2009) Migraine and genetic and acquired vasculopathies. Cephalalgia 29: 1006–17. [Crossref]
- Tietjn GE (2007) Migraine and ischaemic heart disease and stroke: potential mechanisms and treatment implications. Cephalalgia 27: 981–7. [Crossref]
- Scher AI, Terwindt GM, Picavet HS, Verschuren WM, Ferrari MD, et al. (2005) Cardiovascular risk factors and migraine: the GEM population-based study. Neurology 64: 614–20. [Crossref]
- Sarchielli P, Alberti A, Baldi A, Coppola F, Rossi C, et al. (2006) Proinflammatory cytokines, adhesion molecules and lymphocyte integrin expression in the internal jugular blood of migraine patients without aura assessed ictally. Headache 46: 200–7. [Crossref]
- Kurth T (2007) Migraine and ischaemic vascular events. Cephalalgia 27: 967–75.
- Mathew T, Sarma GR, Kamath V, Roy AK. Subdural hematoma, subarachnoid hemorrhage and intracerebral parenchymal hemorrhage secondary to cerebral sinovenous thrombosis: a rare combination. Neurol India 55: 438–9. [Crossref]



