Abstract
Objective: To investigate the potential clinical use of serial fetal CPR measurements during the last month of pregnancy for the prediction of adverse perinatal outcome in unselected low-risk pregnancies.
Methods: A multicenter prospective observational cohort study in 315 consecutively recruited low-risk pregnancies. All eligible pregnancies underwent serial sonographic evaluation of fetal weight and Doppler indices at two week intervals, from 36 weeks gestation until delivery. Data were converted into centiles correcting for gestational age. These data were not available for the obstetrical team and hence, could not influence management decisions. Primary outcomes were operative delivery for presumed fetal compromise and a composite neonatal outcome (arterial cord Ph < 7.20, Apgar scores at 5 minutes < 7 and neonatal intensive care unit (NICU) admission). Neonates were categorized according to CPR values (<10th centile, between 10th and 90th centile and >90th centile).
Results: Three hundred fifteen women were recruited in this study. We ecxluded 32 pregnancies because of small for gestational age babies (SGA), leaving 293 women and 583 CPR values for data-analysis. There were 85 (27%) adverse neonatal outcomes and 29 patients (9%) underwent operative delivery for presumed fetal compromise. Both primary and secondary outcomes were not significant different between the different CPR groups. Furthermore, we examined if individual serial CPR measurements could predict adverse outcome and found no linear correlation between repeated measurements of CPR and adverse outcomes.
Conclusion: Our study shows that routine serial screening by CPR measurements provides poor prediction for adverse perinatal outcome in uncomplicated pregnancies.
Key words
cerebroplacental ratio, fetal compromise, perinatal outcome, uterine artery doppler, middle cerebral artery doppler, appropriate for gestational age
Introduction
Fetal hypoxia in the intrapartum period may result in adverse perinatal outcomes including neurologic injury, seizures (neonatal encephalopathy) and death. During episodes of either acute or chronic hypoxia, the fetus preferentially redistributes its cardiac output to perfuse the vital organs, such as the brain: the brain-sparing effect.1-5 In terms of Doppler indices, the resistance in the umbilical artery (UA) increases upon which the resistance in the middle cerebral artery (MCA) decreases. Several studies have shown a significant association between presence of this brain-sparing effect and adverse perinatal outcomes, particularly in high-risk pregnancies [6-10].
The cerebroplacental ratio (CPR) was first described by Arbeille and colleagues in 1987 [3]. The CPR quantifies the redistribution of cardiac output by dividing the Pulsatility Index (PI) of the MCA by the PI of the UA. The CPR has been reported as a predictor for poor perinatal outcome in pregnancies complicated by intra-uterine growth restriction (IUGR) by many authors [11-22]. Nassr et al. [23] were the first to conduct a systematic review and meta-analysis and concluded that an abnormal CPR is strongly associated with a substantial risk of adverse perinatal outcomes. Several small studies showed that CPR is a better predictor for adverse perinatal outcomes than individual Doppler parameters [11,12], since the ratio may be abnormal while the PIs of both arteries are still within the normal ranges [13]. However, the usefulness of CPR measurements in clinical follow up of low risk pregnancies remains debatable. This could be explained by the lack of evidence in the current literature, since previous studies focused on small for gestational age (SGA) fetuses. Furthermore, the different ways to calculate the CPR (PI versus Resistance Index (RI)) and variable cutoff values used in different studies complicate the application in clinical practice. Various categorical cutoffs were described to predict adverse outcome [11,12]. Moreover, recent data suggest that CPR ranges may vary with gestational age (GA) [24,25]. Cross-sectional and longitudinal studies led to the development of gestational age-based nomograms [24,26].
It should be noted that up to 63% of intrapartum hypoxia events occur in pregnancies without antenatal risk factors [27]. Recent data show that CPR measurements could be a reliable predictor for adverse outcomes in uncomplicated pregnancies as well [27-34]. The objective of this prospective multicentre observational study is to investigate the potential clinical use of serial fetal CPR measurements during the last month of pregnancy for prediction of adverse perinatal outcomes in unselected low-risk pregnancies.
Materials and methods
We conducted a multicenter prospective observational cohort study to investigate the predictive value (detection rate, false positive rates and negative predictive value) of serial CPR measurements, in function of time-to-delivery, for adverse perinatal outcomes. Between December 2015 and February 2017 three hundred fifteen low-risk pregnancies were consecutively recruited in two centers in Belgium. Ethical approval was obtained by the ethics committees of both centers. All women with uncomplicated singleton pregnancies were eligible for this trial and after informed consent was obtained, they were enrolled in this study at 32 weeks GA. Exclusion criteria were multiple pregnancy, hypertensive disorders of pregnancy, sonographic suspicion of fetal abnormalities and suspected small for gestational age (SGA) babies defined as birthweight <p10 in local growth curves. All eligible pregnancies underwent serial sonographic evaluation of fetal weight and Doppler indices at two-week intervals, from 36 weeks GA until delivery. Sonographic surveillance included fetal biometry (biparietal diameter (BPD), head circumference (HC), femur length (FL), abdominal circumference (AC)) and Doppler flow evaluation (PI AU, PI MCA). All measurements were carried out by a group of 6 experienced sonographers according to the Fetal Medicine Foundation (FMF) criteria for Doppler flow assessment. The data were recorded and converted into centiles correcting for GA. Since the CPR was calculated retrospectively, the data were not available for the obstetrical ward team and hence, could not influence management decisions. Maternal age, parity, ethnicity, booking blood pressure, body mass index (BMI) and induction of labor were recorded. Timing and mode of delivery were done according to local protocols and guidelines. After delivery, intrapartal and neonatal outcomes were collected from the patient records. Primary outcomes were operative delivery (cesarean or instrumental delivery) for presumed fetal compromise (FC) and a composite neonatal outcome (arterial cord pH (pHa), Apgar scores (AS) at 5 minutes and NICU admission). Statistical analysis used SPSS. An a priori sample size was calculated for a power of 90%, indicating a total sample size of 295 women to calculate detection rates with a false positive rate of 5%. This was based on a known 1.75% rate of cesarean section and a 9% rate of instrumental deliveries for presumed FC in both centers. Categorical data were presented as numbers (%) and analyzed by the Mann-Whitney U-test. Further analysis included the 1-way analysis of variance (ANOVA). Logistic regression was used to identify and adjust for potential confounders. P-values < 0.05 were considered statistically significant. Neonates were categorized according to CPR-values (<10th centile, 10th - 90th centile, >90th centile) [35].
Results
Three hundred fifteen women were recruited over a 1-year period. We excluded 32 pregnancies because of birthweight below the 10th percentile, leaving 293 women and 583 CPR values for data-analysis. All cases were classified according to CPR percentile groups as below 10th percentile, between 10th and 90th percentile and above 90th percentile. No difference in maternal age (mean 29 years), BMI (mean 25), ethnicity or parity (42% primiparous, 58% multiparous) was observed between the different CPR groups. Neither in between comparisons showed statistical difference between the gestational age groups (36, 38 and 40 weeks gestation). Mode of delivery for all patients is reported in Table 1.
|
48 cesarean section (15%)
|
225 spontaneous vaginal deliveries (71%)
|
42 instrumental deliveries(14%)
|
|
8 for presumed fetal compromise (2%)
|
40 other indication (13%)
|
|
21 for presumed fetal compromise (7%)
|
21 other indication (7%)
|
| |
|
|
|
|
Table 1. Mode of delivery for 315 patients.
Both primary and secondary outcomes were not significant different between the different CPR-groups (Table 2-4). When all modes of delivery were compared using 1-way ANOVA, no differences were seen between the different CPR-groups at 36 weeks (p=0.43), 38 weeks (p=0.70) and ≥40 weeks gestation (p=0.43). Neonatal outcome was assessed by birthweight, Apgar scores, umbilical cord arterial pH and NICU admission. No significant difference was observed between the CPR percentile groups for Apgar score <7 at 5 minutes, umbilical cord arterial pH <7.20 or rate of neonatal NICU admission. Similarly, no significant difference in the composite neonatal outcome score was observed between the CPR groups for the 3 gestational age groups. Likewise, there was no significant correlation between the frequency of meconium stained liquor between the three groups at the different gestational age CPR measurements.
|
Demographic
|
CPR <p10
|
p10<CPR<p90
|
CPR>p90
|
ANOVA/χ2
p-value
|
|
Antenatal
|
|
|
|
|
|
Maternal age (mean)
|
29.8 (22-38)
|
29.3 (16-42)
|
29.5 (20-37)
|
0.78
|
|
BMI (mean)
|
24.3 (18-34)
|
24.8 (17-42)
|
26.0 (19-36)
|
0.37
|
|
Parity (% primiparous)
|
32.6 (15/46)
|
42.9 (78/182)
|
40.0 (10/25)
|
0.45
|
|
Intrapartum
|
|
|
|
|
|
Meconium
|
11% (5/46)
|
8% (14/182)
|
4% (1/25)
|
0.64
|
|
Mode of delivery
Spontaneous vaginal birth
Instrumental delivery FC
Instrumental delivery other
Cesarean section FC
Cesarean section other
Composite operative delivery FC
|
78% (36/46)
9% (4/46)
9% (4/46)
0% (0/46)
4% (2/46)
9% (4/46)
|
70% (127/182)
6% (11/182)
9% (16/182)
3% (5/182)
13% (23/182)
9% (16/182)
|
76% (19/25)
4% (1/25)
0% (0/25)
4% (1/25)
16% (4/25)
8% (2/25)
|
0.43
0.48
0.69
0.37
0.37
0.21
1.00
|
|
Neonatal
|
|
|
|
|
|
Birthweight (median)
|
3387 g
|
3470 g
|
3596 g
|
0.10
|
|
NICU admission (%)
|
4% (2/46)
|
5% (9/182)
|
0% (0/25)
|
0.77
|
|
Composite neonatal outcome
|
28% (13/46)
|
25% (46/182)
|
20% (5/25)
|
0.75
|
Table 2. Demographics, intrapartum and neonatal outcome according to CPR groups at 36 weeks.
|
Demographic
|
CPR <p10
|
p10<CPR<p90
|
CPR>p90
|
ANOVA/χ2
|
|
p-value
|
|
Antenatal
|
|
|
|
|
|
Maternal age (mean)
|
29.9 (20-39)
|
29.4 (16-42)
|
30.6 (20-40)
|
0.6
|
|
BMI (mean)
|
25.4 (19-37)
|
24.9 (17-42)
|
26.2 (19-38)
|
0.5
|
|
Parity (% primiparous)
|
40% (17/43)
|
44% (68/156)
|
28% (5/18)
|
0.5
|
|
Intrapartum
|
|
|
|
|
|
Meconium
|
7% (3/43)
|
8% (12/156)
|
11% (2/18)
|
0.8
|
|
Mode of delivery
|
|
|
|
0.7
|
|
Spontaneous vaginal birth
|
79% (34/43)
|
69% (108/156)
|
78% (14/18)
|
0.4
|
|
Instrumental delivery FC
|
5% (2/43)
|
8% (12/156)
|
6% (1/18)
|
0.9
|
|
Instrumental delivery other
|
2% (1/43)
|
9% (14/156)
|
6% (1/18)
|
0.4
|
|
Cesarean section FC
|
0% (0/43)
|
3% (5/156)
|
6% (1/18)
|
0.3
|
|
Cesarean section other
|
14% (6/43)
|
11% (17/156)
|
6% (1/18)
|
0.7
|
|
Composite operative delivery FC
|
5% (2/43)
|
11% (17/156)
|
11% (2/18)
|
0.5
|
|
Neonatal
|
|
|
|
|
|
Birthweight (median)
|
3492 g
|
3521 g
|
3613 g
|
0.6
|
|
NICU admission (%)
|
0% (0/43)
|
4% (7/156)
|
5% (1/18)
|
0.3
|
|
Composite neonatal outcome
|
26% (11/43)
|
27% (41/156)
|
17% (3/18)
|
0.7
|
Table 3. Demographics, intrapartum and neonatal outcome according to CPR groups at 38 weeks.
|
Demographic
|
CPR <p10
|
p10<CPR<p90
|
CPR>p90
|
ANOVA/χ2
p-value
|
|
Antenatal
|
|
|
|
|
|
Maternal age (mean)
|
29.5 (16-39)
|
29.4 (17-41)
|
28.6 (19-37)
|
0.85
|
|
BMI (mean)
|
25.4 (19-34)
|
24.8 (18-37)
|
24.9 (19-36)
|
0.83
|
|
Parity (% primiparous)
|
43% (10/23)
|
47% (36/76)
|
50% (7/14)
|
0.92
|
|
Intrapartum
|
|
|
|
|
|
Meconium
|
9% (2/23)
|
10% (8/76)
|
21% (3/14)
|
0.45
|
|
Mode of delivery
Spontaneous vaginal birth
Instrumental delivery FC
Instrumental delivery other
Cesarean section FC
Cesarean section other
Composite operative delivery FC
|
78% (18/23)
4% (1/23)
4% (1/23)
4% (1/23)
9% (2/23)
9% (2/23)
|
71% (54/76)
9% (7/76)
9% (7/76)
4% (3/76)
7% (5/76)
13% (10/76)
|
57% (8/14)
7% (1/14)
0% (0/14)
14% (2/14)
21% (3/14)
21% (3/14)
|
0.43
0.40
0.87
0.63
0.25
0.14
0.52
|
|
Neonatal
|
|
|
|
|
|
Birthweight (median)
|
3549 g
|
3681 g
|
3674 g
|
0.37
|
|
NICU admission (%)
|
4% (1/23)
|
4% (3/76)
|
0% (0/14)
|
1.00
|
|
Composite neonatal outcome
|
39% (9/23)
|
20% (15/75)
|
14% (2/14)
|
0.13
|
Table 4. Demographics, intrapartum and neonatal outcome according to CPR groups at 40 weeks.
There were 85 (27%) adverse neonatal outcomes (composite outcome defined as pHa<7.20 or NICU admission or AS <7 at 5 minutes) and 29 patients (9%) underwent operative delivery (instrumental delivery or cesarean section) for presumed fetal compromise.
There was one case of stillbirth at 36+5 weeks gestation. In this case we reported a CPR of 1.33 (p4) at 36 weeks. The PI of the A. Umbilicalis was 0.75 (p27) and the PI of the MCA was 1.03 (p2). As there was no correlation between solitary cut off points of CPR values at different gestational ages and the primary outcomes (Figure 1), we examined if individual serial CPR measurements could predict adverse outcomes. There is no significant linear correlation between repeated measurements of CPR and adverse outcomes, as demonstrated in figure 2 (CPR values according to the variable composite outcome and mode of delivery respectively). Line plots of the subgroups with the composite endpoint and with the operative delivery for presumed FC endpoint are displayed in Figures 3 and 4.
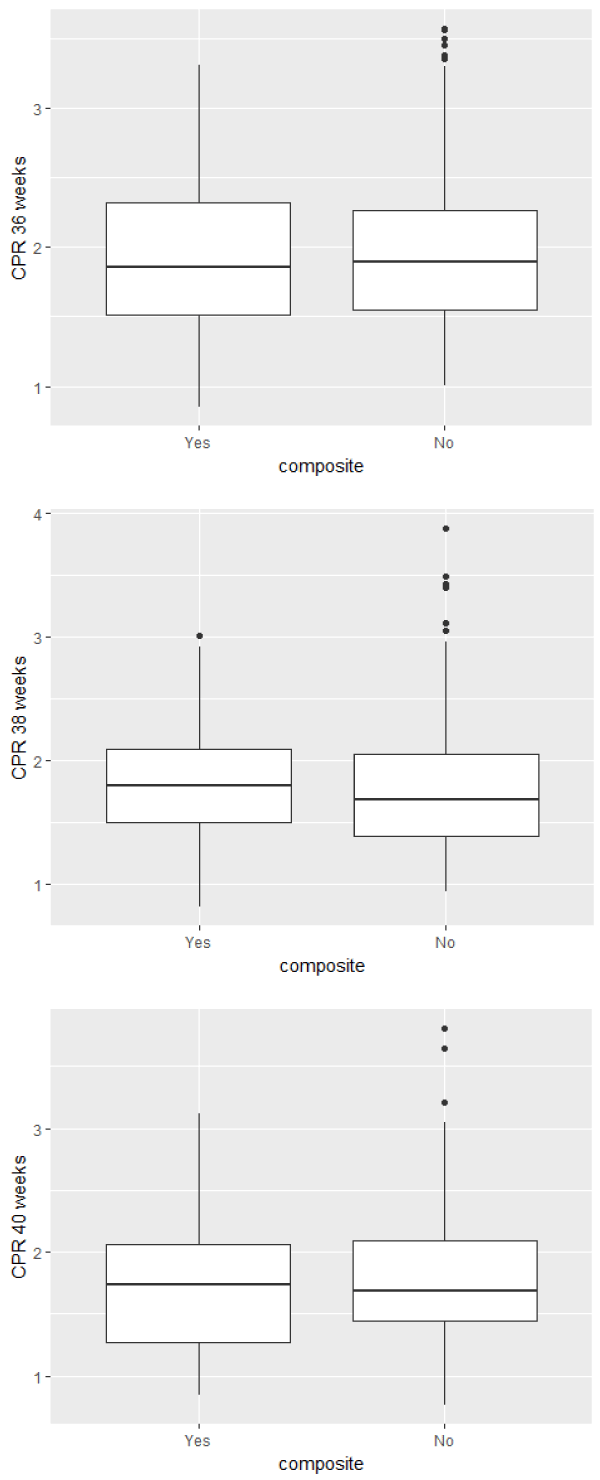
Figure 1. Box-and-whiskers plots of CPR values in AGA fetuses according to the composite variable outcome for the different GA groups showing no correlation between solitary cut off points of CPR values at different gestational ages and the primary outcomes.
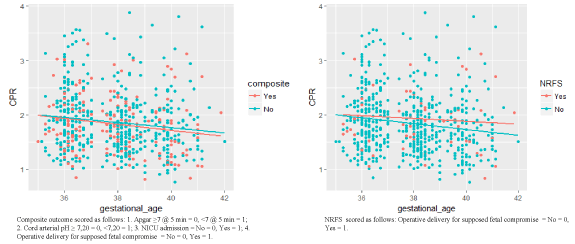
Figure 2. Scatter plots of all CPR values according to the variable composite outcome and mode of delivery respectively show there is no significant linear correlation between repeated measurements of CPR and adverse outcomes.
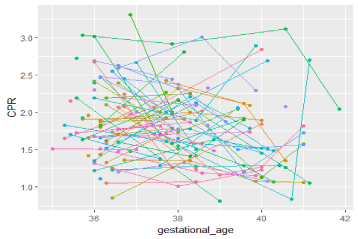
Figure 3. Line plot of CPR values per case of adverse composite outcome (n = 85) illustrates poor prediction of serial CPR measurements in predicting adverse composite outcome.
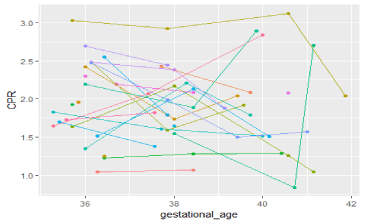
Figure 4. Line plot of CPR values per case of operative delivery for presumed FC (n = 29) illustrates poor prediction of serial CPR measurements in predicting operative delivery for presumed FC.
2021 Copyright OAT. All rights reserv
Discussion
Main findings of the study: Our study demonstrates that the performance of CPR assessment, even in a serial way, is poor in screening for adverse perinatal outcome in appropriate for gestational age (AGA) fetuses.
Strengths and limitations of the study: Strengths are the prospective design of this screening study and the proposed sample size based on accurate calculations of the frequency of adverse outcomes. CPR measurements were performed by trained sonographers (Of all attempts to measure the flow in the MCA correctly, only 11 were unsuccessful). Practitioners were blinded to the CPR results and hence not influenced by the CPR values when taking decisions about timing and conducting labor and delivery. Although adequate sample size calculation, events of perinatal adverse outcome were low (as expected in a cohort of low-risk pregnancies). Another limitation of this trial is that we did not stratify for smoking status of the mothers.
Comparison with findings of previous studies: Importantly, previous studies have focused on the value of fetal Doppler assessment in predicting adverse outcome, almost entirely in SGA fetuses [11-22]. Only three prospective studies have assessed CPR measurements as predictor for adverse outcome in AGA babies [31,33,34]. Prior et al. [31] showed that low CPR (defined as CPR < p10) immediately before established labor in AGA fetuses was associated with increased risk for cesarean section due to FC. Other outcomes were not significantly different between different CPR groups. This is in accordance with the findings of a later retrospective study showing significantly higher rates of both cesarean delivery and instrumental delivery for presumed fetal compromise for AGA with low CPR compared to AGA with normal CPR [28]. However this is in contrast with either the findings of our study as well as both other prospective studies concluding that the performance of CPR in routine screening for adverse perinatal outcome at 30-34 and 36 weeks respectively is weak [33,34]. As far as we know, this is the first prospective screening study assessing third trimester serial CPR measurements in AGA fetuses. We found no benefit for serial nor for solitary CPR measurements in predicting adverse perinatal outcome in AGA fetuses.
Conclusion: Our study shows that routine serial screening by CPR measurements provides poor prediction for adverse perinatal outcome, and it seems unlikely that such assessments would improve perinatal outcomes in AGA fetuses. However, current evidence remains scarce and inconclusive. The potential effectiveness of CPR assessments (minimally invasive and easily transferable to clinical practice) in risk stratification of normal pregnancies before labor needs to be demonstrated by further prospective research.
References
- Arbeille P, Patat F, Tranquart F, Body G, Berson M, et al. (1987) [Doppler examination of the umbilical and cerebral arterial circulation of the fetus]. J Gynecol Obstet Biol Reprod (Paris) 16: 45-51. [Crossref]
- Arbeille P, Roncin A, Berson M, Patat F, Pourcelot L (1987) Exploration of the fetal cerebral blood flow by duplex Doppler--linear array system in normal and pathological pregnancies. Ultrasound Med Biol 13: 329-337. [Crossref]
- Arbeille P, Body G, Saliba E, Tranquart F, Berson M, et al. (1988) Fetal cerebral circulation assessment by Doppler ultrasound in normal and pathological pregnancies. Eur J Obstet Gynecol Reprod Biol 29: 261-273. [Crossref]
- Arbeille P, Body G, Fignon A, Saliba E, Tranquart F, et al. (1989) Doppler assessment of the intracerebral circulation of the fetus. Clin Phys Physiol Meas 10 Suppl A: 51-57. [Crossref]
- Arbeille P, Maulik D, Fignon A, Stale H, Berson M, et al. (1995) Assessment of the fetal pO2 changes by cerebral and umbilical Doppler on lamb fetuses during acute hypoxia. Ultrasound Med Biol 21: 861-870. [Crossref]
- Borowski D, Szaflik K, Kozarzewski M, Sodowski K, Wyrwas D, et al. (2000) [Doppler evaluation as a predictor of asphyxia in fetuses with intrauterine growth retardation (IUGR)]. Ginekol Pol 71: 828-832. [Crossref]
- Borowski D, Czuba B, Wloch A, Wyrwas D, Hincz P, et al. (2006) Doppler assessment of the fetal asphyxia in pregnancies complicated by gestational hypertension and intrauterine growth retardation. Ginekol Pol 77: 184-189. [Crossref]
- Flood K, Unterscheider J, Daly S, Geary MP, Kennelly M M, et al. 2014. The role of brain sparing in the prediction of adverse outcomes in intrauterine growth restriction: results of the multicenter PORTO Study. Am J Obstet Gynecol 211: 288-292. [Crossref]
- Cruz-Martinez R, Savchev S, Cruz-Lemini M, Mendez A, Gratacos E, et al. (2015) Clinical utility of third-trimester uterine artery Doppler in the prediction of brain hemodynamic deterioration and adverse perinatal outcome in small-for-gestational-age fetuses. Ultrasound Obstet Gynecol 45: 273-278. [Crossref]
- Orabona R, Gerosa V, Gregorini ME, Pagani G, Prefumo F, et al. (2015). The prognostic role of various indices and ratios of Doppler velocimetry in patients with pre-eclampsia. Clin Exp Hypertens 37: 57-62. [Crossref]
- Bahado-Singh RO, Kovanci E, Jeffres A, Oz U, Deren O, et al. (1999) The Doppler cerebroplacental ratio and perinatal outcome in intrauterine growth restriction. Am J Obstet Gynecol 180: 750-756. [Crossref]
- Odibo AO, Riddick C, Pare E, Stamilio DM, Macones GA (2005) Cerebroplacental Doppler ratio and adverse perinatal outcomes in intrauterine growth restriction: evaluating the impact of using gestational age-specific reference values. J Ultrasound Med 24: 1223-1228. [Crossref]
- Gramellini D, Folli MC, Raboni S, Vadora E, Merialdi A (1992) Cerebral-umbilical Doppler ratio as a predictor of adverse perinatal outcome. Obstet Gynecol 79: 416-420. [Crossref]
- Murata S, Nakata M, Sumie M, Sugino N (2011) The Doppler cerebroplacental ratio predicts non-reassuring fetal status in intrauterine growth restricted fetuses at term. J Obstet Gynaecol Res 37: 1433-1437. [Crossref]
- Spinillo A, Gardella B, Bariselli S, Alfei A, Silini EM, et al. (2014) Cerebroplacental Doppler ratio and placental histopathological features in pregnancies complicated by fetal growth restriction. J Perinat Med 42: 321-328. [Crossref]
- DeVore GR (2015) The importance of the cerebroplacental ratio in the evaluation of fetal well-being in SGA and AGA fetuses. Am J Obstet Gynecol 213: 5-15. [Crossref]
- Warshak CR, Masters H, Regan J, DeFranco E (2015) Doppler for growth restriction: the association between the cerebroplacental ratio and a reduced interval to delivery. J Perinatol 35: 332-337. [Crossref]
- Khalil A, Thilaganathan B (2017) Role of uteroplacental and fetal Doppler in identifying fetal growth restriction at term. Best Pract Res Clin Obstet Gynaecol 38: 38-47. [Crossref]
- Simeone S, Marchi L, Canarutto R, Pina Rambaldi M, Serena C, et al. (2016) Doppler velocimetry and adverse outcome in labor induction for late IUGR. J Matern Fetal Neonatal Med 1-6.
- Muresan D, Rotar IC, Stamatian F (2016) The usefulness of fetal Doppler evaluation in early versus late onset intrauterine growth restriction. Review of the literature. Med Ultrason 18: 103-109. [Crossref]
- Triunfo S, Crispi F, Gratacos E, Figueras F (2016) Prediction of delivery of small for gestational age neonates and adverse perinatal outcomes by feto-placental Doppler at 37 weeks' gestation. Ultrasound Obstet Gynecol 49: 364-371. [Crossref]
- Tanis JC, Boelen MR, Schmitz DM, Casarella L, van der Laan ME, et al. (2016) Correlation between Doppler flow patterns in growth-restricted fetuses and neonatal circulation. Ultrasound Obstet Gynecol 48: 210-216. [Crossref]
- Nassr AA, Abdelmagied AM, Shazly SA (2016) Fetal cerebro-placental ratio and adverse perinatal outcome: systematic review and meta-analysis of the association and diagnostic performance. J Perinat Med 44: 249-56. [Crossref]
- Baschat AA, Gembruch U (2003) The cerebroplacental Doppler ratio revisited. Ultrasound Obstet Gynecol 21: 124-127. [Crossref]
- Morales-Rosello J, Khalil A, Morlando M, Hervas-Marin D, Perales-Marin A (2015) Doppler reference values of the fetal vertebral and middle cerebral arteries, at 19-41 weeks gestation. J Matern Fetal Neonatal Med 28: 338-43. [Crossref]
- Ebbing C, Rasmussen S, Kiserud T (2007) Middle cerebral artery blood flow velocities and pulsatility index and the cerebroplacental pulsatility ratio: longitudinal reference ranges and terms for serial measurements. Ultrasound Obstet Gynecol 30: 287-296. [Crossref]
- Low JA, Pickersgill H, Killen H, Derrick EJ (2001) The prediction and prevention of intrapartum fetal asphyxia in term pregnancies. Am J Obstet Gynecol 184: 724-730. [Crossref]
- Khalil AA, Morales-Rosello J, Morlando M, Hannan H, Bhide A, et al. (2015) Is fetal cerebroplacental ratio an independent predictor of intrapartum fetal compromise and neonatal unit admission? Am J Obstet Gynecol 213: 54.e1-10. [Crossref]
- Morales-Roselló J, Khalil A, Morlando M, Bhide A, Papageorghiou A, et al. (2015) Poor neonatal acid-base status in term fetuses with low cerebroplacental ratio. Ultrasound Obstet Gynecol 45: 156-161. [Crossref]
- Khalil A, Morales-Rosello J, Townsend R, Morlando M, Papageorghiou A, et al. (2016) Value of third-trimester cerebroplacental ratio and uterine artery Doppler indices as predictors of stillbirth and perinatal loss. Ultrasound Obstet Gynecol 47: 74-80. [Crossref]
- Prior T, Mullins E, Bennett P, Kumar S (2013) Prediction of intrapartum fetal compromise using thecerebroumbilical ratio: A prospective observational study. Am J Obstet Gynecol 208: 124.e1-e6. [Crossref]
- Liu J, Song G, Zhao G, Meng T (2016) The Value of the Cerebroplacental Ratio for the Prediction of Intrapartum Fetal Monitoring in Low-Risk Term Pregnancies. Gynecol Obstet Invest 82: 475-480 [Crossref]
- Akolekar R, Syngelaki A, Gallo DM, Poon LC, Nicolaides KH (2015) Umbilical and fetal middle cerebral artery Doppler at 35-37 weeks' gestation in the prediction of adverse perinatal outcome. Ultrasound Obstet Gynecol 46: 82-92. [Crossref]
- Bakalis S, Akolekar R, Gallo DM, Poon LC, Nicolaides KH (2015) Umbilical and fetal middle cerebral artery Doppler at 30-34 weeks' gestation in the prediction of adverse perinatal outcome. Ultrasound Obstet Gynecol 45: 409-20. [Crossref]
- http://medicinafetalbarcelona.org/




