Everyone has become painfully aware that women (and men) with a breast cancer gene(s) have an increased “potential” to develop breast cancer. They also have an increased risk of developing uterine and ovarian cancer and in men, there is an increased potential to develop prostate cancer. One of the first reactions many women have when they are told they have a breast cancer gene or that they have breast cancer, is what do I need to do to get ride of it? Many of them out of that fear and our inability to guarantee better screening than mammography, want the breast(s) removed entirely. Unfortunately, the removal of the breast does not remove all breast tissue as there is still breast tissue connected to the overlying skin.
Absent an accurate quantitative method for detecting breast cancer, one can understand women wanting something done to reduce their risk of dying from breast cancer. Women, who opt for bilateral prophylactic mastectomies, or mastectomy when cancer is present in the breast tissue, believe the mastectomy will totally remove their risk of developing breast cancer in the future. Once a woman has had a mastectomy, like men, there is little significant breast tissue remaining, but it is there. Under these circumstances the development of breast cancer in the remaining breast tissue will be closer to the chest wall and metastatic spread.
A friend of mine, Dr. Henry Lynch is the man who discovered the breast cancer genes. He found two such genes in families whose women had multiple breast cancers. He called these genes BRCA1 and BRCA2. BR is the abbreviation for “breast” and CA is the abbreviation for “cancer.” The first one he discovered was numbered 1 and the second gene number 2. These genes are found on chromosomes 17 and 13 respectively. A representation of these genes is seen in figure 1.
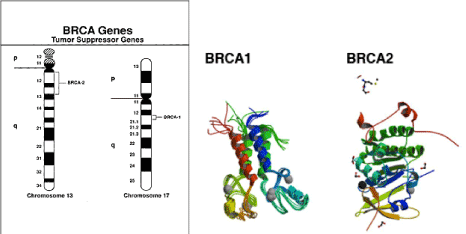
Figure 1. BRCA1 is found on human chromosome 17 and BRCA 2 is found on chromosome 13. Three-dimensional representations are shown.
The function of the “normal” genes is to “suppress”, “inhibit” or “stop” cancers from developing in the first place. In the case of BRCA1 and BRCA2, these genes have become “altered” and no longer do their job. As a result, the genes don’t work properly to “prevent” cancer and if the person for whatever reason develops breast cancer, the “normal” genes won’t be there to stop it. So having BRCA1 and/or BRCA2 doesn’t actually cause cancer, they merely remove one of your safety mechanisms for trying to stop the development of cancer.
Some groups of people have a greater tendency to have these mutations. For example, Ashkenazi Jews have a 1 in 40 frequency of having one of these two mutations, while this is only seen in the U.S. population once in every 400-800 people. Despite the number of people who have these “abnormal” genes, it is still only present in 5 to 10% of all breast cancer cases.
The real problem is one of uncertainty! Women who undergo bilateral prophylactic mastectomy because they have a breast cancer gene are under the misperception that this removes their risk of breast cancer; it does not! Our current diagnostic tests are wrong 35% of the time, so their fear is completely understandable. Fear of developing breast cancer coupled with the misperception that the bilateral prophylactic mastectomy removes their risk of developing breast cancer is the equivalent of two wrongs don’t make a right.
Nothing about mammography has resulted in anyone being so confident in its ability to detect breast cancer that we as physicians are willing to tell you that we can find breast cancer early enough to guarantee your survival. So, fear can easily influence decisions and if I were in the place of a woman with a breast cancer gene, I’m not certain I wouldn’t do the same thing.
Fortunately it’s 2017 and this is not the end of the story. Breast Enhanced Scintigraphy Test (B.E.S.T.)©℗ Imaging recently received it’s patent (FMTVDM-BEST©℗) approval. FMTVDM-BEST©℗ looks for breast cancer in an entirely different way. It was designed to use the characteristics of cancers to make them more easily detected and can accurately quantify these differences. The method brief enhances differences between calcium, normal breast tissue, inflammatory changes in the breast and breast cancer and then measures these differences, allowing (1) differentiation of tissue types, (2) analysis of how rapidly the breast tissue is changing and (3) a determination of whether treatment is working or not. As a result FMTVDM-BEST©℗ can accurately find cancers and pre-cancers missed by mammography and other tests. Because FMTVDM-BEST©℗ is a quantitative test and does not rely on physician interpretation of what s/he sees on the image, it is not plagued by tissue density, clinical interpretation, or calcium deposits.
As shown in figure 2, FMTVDM-BEST©℗ imaging showed that despite this woman having a mastectomy in addition to chemotherapy, she continued to have recurrent breast cancer. These results show how FMTVDM-BEST©℗ imaging can find breast cancers where mammography cannot and how FMTVDM-BEST©℗ can be used to monitor treatment response, allowing for patient tailored treatment decisions, improving clinical outcomes.
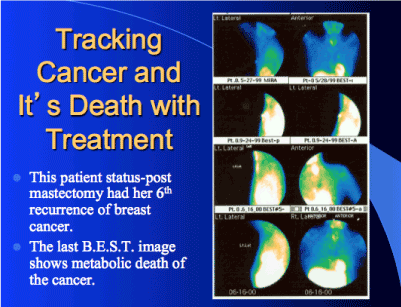
Figure 2. Over the course of time, this patient underwent both mastectomy and chemotherapy. The first and second set of FMTVDM-BEST©℗ images (first and second row) showed the return of her cancer, demonstrated that her treatment, including her mastectomy had not prevented the return of breast cancer. FMTVDM-BEST©℗ imaging resulted in the physician changing her treatment plan tailored to her results (rows 3 and 4), killing the breast cancer.
The results for this patient also clearly show that mastectomy itself cannot guarantee that a woman (or man) will not develop breast cancer. If mastectomy could guarantee this, then there would be no reason for a follow up visit with your doctor after the surgery. Since people can develop recurrent breast cancer after mastectomy, clearly a bilateral prophylactic mastectomy for individuals with a breast cancer gene(s) will not prevent breast cancer from developing?
While genetic testing may be helpful in making life-altering decisions, our prior inability to more accurately detect breast cancer, has undoubtedly caused many women (and men) to make decisions based upon fear, fear that we in Medicine cannot adequately reassure them of the accuracy of our tests, tests which are qualitatively visually driven. FMTVDM-BEST©℗ imaging is the First quantitative method which changes that, allowing people including those with a genetic predisposition toward breast caner, the additional information they need before deciding on a treatment plan, including surgery, chemotherapy, hormonal therapy, dietary and lifestyle changes, or nothing.
Acknowledgements
This study is Funded by the Camelot Foundation 501(c)(3). All authors reviewed and approved of manuscript submission.
Conflicts of interest
No conflicts of interest to note.
2021 Copyright OAT. All rights reserv


