Introduction: The role of the cheek fat compartment in aging of the face is nowadays accepted and well described in a lot of publications, but the anatomy and the age-related changes of this compartment are less clear and defined. The authors propose a review on the anatomy of face fat compartments and their age-related changes.
Materials and methods: The authors executed a review of the literature and verified it by the dissection of 14 cadaveric hemifacial specimens. All the main fat compartments described in literature were found in these cadaver dissections. The anatomical localization and the relationships of the fat compartments are described as well as the retaining structures that define them. Based on literature review the age-related modifications of fat compartments were analyzed.
Results: Superficial and deep fat compartments of the cheek were identified: infraorbital fat, superficial medial cheek fat, nasolabial fat, middle cheek fat, lateral temporal-cheek fat, superior and inferior jowl fat, superficially and medial and lateral suborbicular is oculi fat, deep medial cheek fat, buccal fat.
The fat compartments undergo specific modifications due to the aging process. Generally deep compartments undergo hypotrophic changes and whilst superficial compartments undergo hypertrophic or ptotic.
Conclusion: Comprehension of anatomy and of age-related changes of facial fat compartments is important to improve our capability in assessing the aging of the face and planning adequate treatments to correct it.
Midface aging has different causes whose role is still not completely clear. The changes of the anatomical components effected by the aging processes involve all the tissues of the region: skin, fat, ligaments, muscles and bones.
In two interesting papers regarding aging of the bony components of the face,
Pessa et al. [1,2] using computerized tomography, demonstrated a postero-inferior rotation of the skeleton towards the base of the skull. This results in a decrease in the supporting capacity of the bony structures of the overlying soft tissues and consequently a lowering in forward projection of the face.
The part played by bone reabsorption in facial aging and the changes in the facial skeleton have been substantiated and ascertained by other authors too [3], and is always to be taken in consideration, especially in the infraorbital and zygomatic-malar regions, when planning treatment strategies with hyaluronic acid fillers and fat grafting.
In the past it was believed that with aging the muscles of the malar region, in particular the zygomatic muscles, underwent a progressive slackening. In recent years, in the absence of evidence of real muscle relaxation this region, it is thought that the age-related changes the muscle component are of secondary importance and barely relevant. Studies with magnetic resonance imaging show how there are no significant changes to the length and thickness of the muscles in the malar region in relation to aging [4].
The role played by the ligaments in facial aging in general has been described by various authors [5-8] and this is also considered valid for the infraorbital and malar regions where the retaining structures are numerous and anatomically well defined [9,10]. Histopathological studies seem to show a progressive decrease in elastic fibers with aging [11] at the dermal and superficial muscular aponeurotic system (SMAS) level. SMAS is a continuous and organized fibrous network connecting the periosteum, the facial muscles, and other fascia types (such as the parotid fascia), to the dermis. The decrease in the elastic component could be a cause of the reduction in the retaining capacities of the ligaments that are manifested in ptosis of the soft tissues.
Other authors [12] question whether ligament slackening effectively occurs in this way or is simply a consequence of the hypotrophy of the fatty tissue which, through causing a decrease in tension on the ligamentous structures, causes solely an apparent relaxation.
It is widely agreed that the changes arising in the fat component of the midface are among the main causes of visible facial aging. More debatable are the ways in which the fatty tissues change with aging and how these changes manifest and alter the appearance of the face. We shall now analyze the anatomy and the modifications occurring in midface fatty tissue.
A bibliographic search was performed using Pubmed, Lippincott Williams & Wilkins via OvidSP, Nature (NPG), Elsevier Journals (ScienceDirect) databases using the key words anatomy, face, fat, compartment and aging. 117 references were found of which 20 were relevant to with the aims of our study [13-32].
A careful review of all these articles and of others found during the review performed to define the current knowledge of the anatomy of the facial fat compartment and its relation to the aging processes.
A series of 14 hemifacial cadaveric dissection were performed at the Department of Anatomy, University of Malta. In all hemifacial cadaveric specimens, the dissections were performed in order to verify the presence of fat compartments and their correct anatomical localization according to knowledge present in the literature.
The skin was incised along the medial line of the head from trichion to menton, along the hemi-coronal line up to the preaural point, along the jawline, the margins of superior and inferior vermilion and the superior and inferior palpebral sulcus. The skin was first dissected away and removed, exposing in this way the superficial fat compartment and in particular: the infraorbital fat (IF), the superficial middle cheek fat (SMCF), the nasolabial fat (NLF), the middle cheek fat (MCF), the lateral temporal cheek fat (LTCF) and the superior and inferior jowl fat (SJT, IJF). Skin dissection was quite difficult because of a strong adhesion found between the dermis and superficial fat compartments due to the presence of the thick network of fibrous septa of superficial SMAS. The superior margin of the infraorbital fat was identified and, starting from this margin, IF, SMCF and NLF following the SMAS plane were detached by blunt dissection up to zygomaticus major muscle. In this way the orbicularis oculi muscle was exposed and below it the lateral and medial sub-orbicularis oculi fat (L-SOOF, M-SOOF) were located. Caudal to the SOOFs, the deep medial cheek fat (DMCF) was observed. The infero-lateral border of this compartment is formed by the zygomaticus major muscles. Furthermore, using sharp dissection the middle cheek fat was divided from the lateral temporal-cheek fat along the anterior margin of masseter muscle following the masseter ligament. A blunt dissection along the deeper surface of middle fat compartment was then performed, exposing the buccal extension of buccal fat. The dissection proceeded by removing the orbicularis oculi muscle and uncovering the M-SOOF and the medial part of L-SOOF. Sharp dissection alongside the orbicularis retaining ligament reached the pre-periosteal plane and the M-SOOF was detached from the underlying maxillary periosteum up to the zygomatic-cutaneous ligament. Laterally the pre-periosteal dissection was continued, separating the L-SOOF from the periosteum of the zygomatic bone. The dissection extended upwards until the lateral thickening of orbicularis retaining ligament, below the lateral cantus of eyelid; inferiorly it extended to the zygomatic-cutaneous ligament thickening (Mc Gregoor patch) at the level of the zygomaticus major muscle origin. The pre-periosteal dissection of the L-SOOF was found to be easier than that of the M-SOOF as it is less adherent to the periosteum. Cutting along the medial margin of zygomaticus major muscle, the maxillary periosteum was identified, and the deep surface of deep medial cheek fat was dissected away from the underlying pre-periosteal plane extending medially until to the pyriform ligament surrounding the nasal base and inferiorly up to the nasolabial fold adherence.
Comparing the data found in literature and the results of our cadaver dissections an anatomical description of the midface fat compartments and an analysis of their age-related modification was prepared.
All the superficial and deep fat compartments of the cheek usually described in literature have been found in all hemifacial cadaveric specimens. As suggested by [33] clinical observation and laboratory investigation show that the subcutaneous fat of the face is highly partitioned, that it is not a confluent mass, and that exists in distinct anatomical compartments. The fat compartments are determined by fascial membranes that arise from the superficial fascia and insert into the dermis of the skin [17,25].
The midface fat compartments are classified as superficial and deep. It is very important to distinguish between these two different categories. The superficial fat compartments are localized between the skin and the plane of the Superficial Muscular Aponeurotic System (SMAS), that consists of a three-dimensional architecture of collagen, elastic, and muscle fibers as well as fat cells (34-36). The fat tissue of the superficial compartments is found within this fibrotic network. Beneath the SMAS plane, deep to the muscles of facial expression, we find the deep fat compartments extend to and adhere to the periosteum.
Listed below are the fat compartments of the cheek identified by our dissection (Figure 1) (19,37-38).
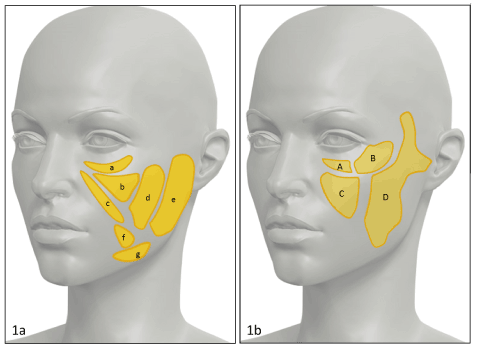
Figure 1. a) Superficial cheek fat compartments: a) Infraorbital fat. b) Medial cheek fat. c) Nasolabial fat. d) Middle cheek fat. e) Lateral cheek fat. f) Superior jowl fat. g) Inferior jowl fat.
b) Deep cheek fat compartments: A) Medial sub-orbicularis oculi fat. B) Lateral sub-orbicularis oculi fat. C) Deep medial cheek fat. D) Buccal fat.
Superficial fat compartments:
- Infraorbital fat (IF);
- Superficial medial cheek fat (SMCF);
- Nasolabial fat (NLF); Middle cheek fat (MCF);
- Lateral temporal-cheek fat (LTCF);
- Superior Jowl fat (SJF);
- Inferior Jowl fat (IJF).
Deep fat compartments:
- Medial Suborbicularis Oculi Fat (M-SOOF);
- Lateral Suborbicularis Oculi fat (L-SOOF);
- Deep medial cheek fat (DMCF);
- Buccal fat (BF).
Anatomy of fat compartments
Superficial fat compartments: Infraorbital fat (IF) (Figure 2): its superior margin corresponds to the tear trough and to the palpebro-malar groove on the skin surface. In fact the superior boundary of this compartment is formed by the orbicularis retaining ligament that originates at 1-2 mm below the margin of orbital cavity and which, after passing through the orbicularis oculi muscle, adheres to the dermis [14,39,40]. Other authors describe this ligament as extending from the periosteum, just outside the orbital rim, to the fascia on the undersurface of the orbicularis oculi muscle [41]. The adhesion of the orbicularis retaining ligament to the above soft tissue contributes to the formation of the tear trough and palpebro malar groove. Cranial to these two grooves, the orbicularis oculi muscle lies directly deep to the skin of eyelid. Caudal to these grooves on the other hand, the orbicularis oculi muscle is separated from the overlying skin by the infraorbital fat.
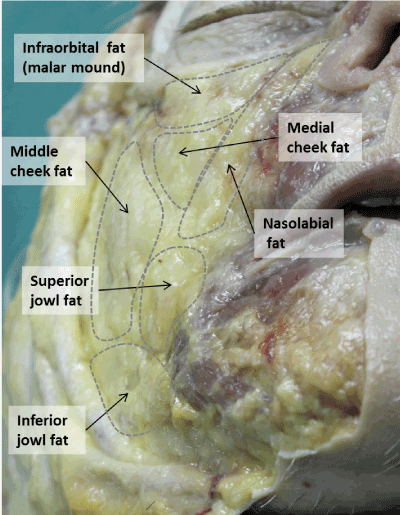
Figure 2.Superficial cheek fat compartments: a) Infraorbital fat. b) Medial cheek fat. c) nasolabial fat. d) Middle cheek fat. e) Lateral cheek fat. d) Superior jowl fat. e) Inferior jowl fat. Red dashed line indicates the margin of malar fat pad constituted by the infraorbital fat, medial cheek fat and nasolabial fat.
The infraorbital fat is inferiorly delimited by the zygomatic cutaneous ligament [42] or zygomatic ligament. Mendelson et al., [9] described zygomatic ligaments medial to the junction of the arch and body of zygoma, located along the origins of the facial expression muscles (the zygomaticus major, zygomaticus minor, and levator labii superioris). At the level of the junction of the arch and body of the zygoma, just lateral to the zygomaticus major muscle origin, this ligament becomes thicker and stronger and is described as the McGregor patch [43].
The fat of this compartment has a higher tendency to retain water. Being frequently the site of persistent edema it often forms the so called malar mound [37,44] .
Superficial medial cheek fat (SMCF) (Figure 2): this is located caudally to the IF from which it is separated by the zygomatic cutaneous ligament. It has a triangular shape and it is wedged between the infraorbital and nasolabial fat. Laterally this compartment is limited by the zygomaticus major muscle and borders, the middle cheek fat. Infero-medial to the superficial medial cheek fat lies the nasolabial fat which extends parallel to the nasolabial fold. The maxillary portion of the bucco-maxillary ligaments divide these two compartments [45].
Nasolabial fat (NLF) (Figure 2): this has an oblong form, lies lateral to the nasal pyramid and cranial to the nasolabial fold. The orbicularis retaining ligament represents the superior border of this compartment [33]. Its supero-lateral boundary is the medial cheek fat and its infero-medial boundary is the nasolabial fold. Its inferior part borders and overlaps the SJF [33].
Middle cheek fat (MCF) (Figure 2): this is located lateral to the medial cheek fat and it is bordered above by the zygomatic ligament [29]. Above this compartment, the ligament is thick and constitutes the McGregor patch [43]. The middle cheek fat does not extend above the inferior margin of the zygomatic arch. Its anterior boundary is the masseter ligament that starts inferior to the McGregor patch and descends vertically along the anterior margin of masseter muscle. This ligament arises from the fascia of the masseter muscle and inserts into the SMAS and overlying dermis of the cheek [29]. The middle cheek fat medially borders the lateral temporal-cheek fat. The subcutaneum parotideomassetericum septum, originating from the SMAS in the region of the parotid gland and running in an anterior and lateral direction into the dermis of the cheek, divides these two compartments [46]. Caudal to the middle cheek fat lies the inferior jowl fat.
There is also the Lateral temporal-cheek fat (LTCF): this is the most lateral compartment of the cheek.
It lies in direct contact with the parotid gland and connects the temporal fat to the cervical subcutaneous fat [33]. The cheek part of this compartment is firmly adherent to the parotid fascia.
At the level of preauricular region the platysma-auricular ligaments forms the posterior border of the lateral temporal cheek fat [45]. A true vertical septal barrier is located anterior to this compartment. This septum was named the lateral cheek septum by Rorich and Pessa [33] as or the subcutaneum parotideomassetericum septum by Pils and Anderhuber [46] .
Superior Jowl fat (SJF) (Figure 2): this is lateral to the modiolus, clinically it appears as the most inferior extension of the nasolabial fold and of the nasolabial fat. Its lateral borders lies against the middle cheek fat and its inferior border against the inferior jowl fat.
Then there is the Inferior Jowl fat (IJF) (Figure 2): this is located below the middle cheek fat and inferior to the superior jowl fat. Its medial boundary is the mandibular ligament and its lateral boundary is the lateral temporal-cheek fat. The inferior boundary is made up by the mandibular septum [24,38].
The first three superficial fat compartments (infraorbital fat, superficial medial cheek fat and nasolabial fat) are often described as a single anatomical structure: the malar fat pad. It has a triangular shape with the base parallel to the nasolabial fold and with the apex near the malar projection (Figure 3). The malar fat pad is loosely adherent to the deep plane (SMAS), but it is firmly adherent to the skin (47). The malar fat pad is supported in its location during youth by multiple fibroelastic fascial septa that extend through the fatty cheek mass originating from the underlying superficial fascia that invests the facial expression muscles to insert into the overlying dermis [11].
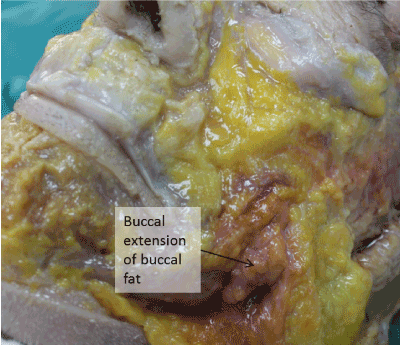
Figure 3. Deep cheek fat compartments: A) Medial sub-orbicularis oculi fat. B) Lateral sub-orbicularis oculi fat. The sub-orbicularis oculi fat compartments are located below the orbicularis oculi muscle. In this anatomic dissection, the SOOFs are visible thanks to the separation of the muscular fibers of orbicularis oculi muscle. C) Deep medial cheek fat. The upper part of DMCF is below the orbicularis oculi muscle. It lies laterally to the zygomaticus major muscle.
Deep fat compartments are: the Medial Suborbicularis Oculi Fat, the Lateral Suborbicularis Oculi Fat, Deep medial cheek fat and Buccal fat.
Medial Suborbicularis Oculi Fat (M-SOOF) (Figure 4): this lies adherent to the periosteum along the orbital rim (Rohrich et al., 2009), below the orbicularis retaining ligament and under the orbicularis oculi muscle. It extends from the medial limbus to the outer cantum. The zygomatic cutaneous ligament separates the M-SOOF from the deep medial cheek fat.
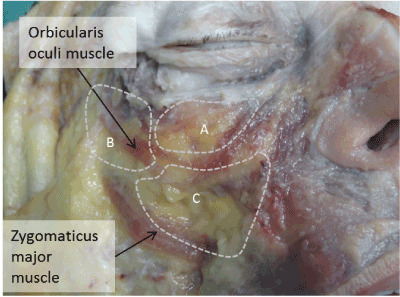
Figure 4. In this anatomical dissection the middle cheek fat has been removed and the buccal extension of buccal fat is clearly visible.
Lateral Suborbicularis Oculi Fat (L-SOOF) (Figure 4): this is located at the lateral orbital rim above the prominence of the zygoma but does not reach above the superior margin of the zygomatic arch and it does not extended above the lateral canthus and the lateral orbital thickening represents the upper limit of L-SOOF. Its medial half is covered by the orbicularis oculi muscle. L-SOOF lies above another more deeply situated fat compartment, therefore it is not in direct contact with the periosteum [30]. Medial to it is the M-SOOF.
Deep medial cheek fat (DMCF) (Figure 4): this is under the SMAS plane and its superior part lies under the orbicularis oculi muscle. Its superior boundary is the zygomatic-cutaneous ligament that divides it from M-SOOF and it medially borders the buccal fat and with the zygomaticus major muscle. The medial boundary is the pyriform ligament surrounding the nasal base and the inferior boundary is the sub–orbicularis orris fat. This fat compartment lies on the periosteum of the maxilla. Between the periosteum and the fat compartment is a potential space, defined as Ristow’s space [19].
Pils et al. [26] divided this compartment in two different layers: one superficial, named malar fat, and another deeper, named premaxillary fat. Other authors [13] describe this compartment as divided into two different parts. One, the medial part, located beneath the nasolabial fat, does not lie immediately on the periosteum of the maxilla but it is bordered posteriorly by another small, triangular compartment. The lateral part is located under the superficial medial cheek fat and lies directly on the maxilla. Probably the Rislow’s space, the premaxillary fat and the triangular fat compartment posterior the medial part, are all the same anatomical structure.
Buccal fat (BF): this is located below the zygoma and anteriorly to the ramus of the mandible surrounding the medial pterygoid and masseter muscles. This fat compartment has a buccal extension (Figure 3) that abuts the medial cheek fat, the deep medial cheek fat, the middle cheek fat, the sub–orbicularis oculi fat, the jowl fat, and the fat of the pre-masseter space. Gierloff et al. [13] in their computed tomography study have observed a hypothetical anatomical boundary between the buccal extension and the buccal fat pad. They have hypothesized that the buccal extension can be regarded as a distinct fat compartment. Other authors share this opinion [27].
Aging of fat compartments
The fat compartments undergo specific changes due to the aging process [20,21]. In some compartments the main changes are volume augmentation; in other the volume reduction or ptotis. The capability to understand these changes is essential in order to make a correct assessment of facial aging.
The main age-related modifications, as indicated by our cadaver dissections and clinical experience, are different in superficial fat compartments compared to the deep ones. This evaluation is confirmed in recent scientific literature concerning the aging process of the face.
In the superficial medial cheek fat, the aging process causes a global volume increase with an inferior volume shift within the fat compartment. The volume increases in the lower two thirds and remains stable in the upper one [13]. Similar changes are observed in nasolabial fat that shows an inferior volume shift of fat tissue. In aged patients, the sagittal diameter of the upper third is smaller and the sagittal diameter of the lower third is higher [13]. These modifications create an overall volume augmentation of lower part of malar fat pad due to the ptosis and caudal migration of fat tissue. For this reason the aging of the malar fat pad can be described generally as ptotic/“hypertrophic”. The ptosis and the volume augmentation of these fat compartments contribute to the increase of the depth of the nasolabial fold [11,18].
The middle cheek fat, is loosely adherent to SMAS plane just like the malar fat pad, and its aging is characterized by ptosis, by caudal migration of fat and by a whole volume augmentation [13]. These modifications produce an increasing of convexity in the central portion of the cheek.
Finally the lateral temporal-cheek fat lies upon and is adherent to the parotid fascia without any deep fat compartment between them. Aging results in a hypotrophic involution of this compartment that does not usually have any tendency to caudal migration, showing a different aging process than the other superficial fat compartments previously described.
In deep fat compartments we find different aging related modifications. The medial and lateral SOOF both lie on periosteum and have an aging characterized by deflation with low tendency to ptosis. This is due to the fact that the reduced weight and the stronger attachment to underlying tissue makes it less likely to ptosis under the effects of gravity. The deflation of medial SOOF produces the formation of the hollow in the infraorbital region. Reduction of the medial SOOF has been noted to increase the orbit cheek crease and the V deformity of the lower lid described by Mendelson et al. [9]. The medial SOOF supports the palpebral tissues of the inferior eyelid, so its reduction in volume increases the relaxation of the tissue of inferior eyelid and of the intraorbital fat. The volume reduction of the lateral SOOF decreases the forward protrusion of the malar area and of the cheekbone, facilitating the ptosis of superficial fat compartments of the cheek.
The deep medial cheek fat undergoes a gradual and global decrease of volume [15,23] and a caudal migration [13]. The volume reduction is greater in the upper two thirds and minor in the lower third where the caudal migration of fat compensates the volume loss [13].
The part of buccal fat that influences the aesthetic of the cheek is its buccal extension. It seems to be mainly characterized by a hypotrophic ageing response. Several authors have observed a lower volume of the buccal extension in older cadaver specimens [13,48]. The deflation of this fat compartment leads consequently to a lack of support for the medial cheek and middle cheek fat, aggravating the descent of these compartments. Other authors [49,50] have observed an antero-inferior protrusion of buccal fat that increases the convexity of cheek and the ptosis of jowl.
Clinical and anatomical observations suggest that, with age, fat compartments could tend to deflation, specifically in the deep compartments, and to volume augmentation and ptosis, especially in the superficial fat compartments [19,51]. Some scientific support for this hypothesis is observed in literature. Gierloff et al. [13] showed a relative volume decrease in the deep cheek compartments of older cadaveric specimens (75–104 years) compared to younger group (54–75 years). These authors introduced in this study the concept of an inferior volume shift within the compartments observed especially in nasolabial and superficial medial cheek fat. These events create the “hypertrophy“ of lower parts of superficial fat compartments that constitute the malar fat pad. A similar hypothesis is proposed by Gosain et al. [52], in their MRI study of the malar fat pad and by Owsley and Roberts [11] in their anatomical analysis of midface aging. They sustain that the facial expression muscle movements related to smiling result in the shrinkage of the base of superficial fat compartments of the malar fat pad and a consequent protrusion of the fat tissue especially in their inferior portion. The continued stress and lengthening of fibrotic septa of the SMAS results in their progressive loosening and the reduction of their retentive capability. With aging the inferior migration of fat tissue becomes permanent and produces a volume augmentation in the lower part of malar fat pad and a consequent increase of depth of the nasolabial fold.
The pattern of facial aging is probably produced by the combination of the different volumetric and morphologic modifications of the various fat compartments. These changes can vary in different patients and can manifest themselves in different ways. The volumetric reduction of deep fat compartments causes the formation of hollows and flattening especially of infraorbital and zygomatic areas; contemporaneously it causes the ptosis of superficial fat compartments due to the loss of support determined by hypotrophy of deep adipose tissue. The compartmental changes secondary to gravity are also influenced by compartmental changes secondary to deflation. These synergistic effects may influence the shape and position of adjacent compartments [22,28]. If the superficial fat compartments are also characterized by volume reduction, it creates an evident skin sagging defined by Rohrich as “pseudoptosis” [19]. If the volume reduction of superficial fat compartments isn’t accentuated and a sufficient amount of fat tissue persists, it creates the downward migration and the volume enhancement at the nasolabial region.
If, instead, the hypertrophy and ptosis of the superficial fat compartments are prevalent, the aging is characterized by volume augmentation especially at inferior part of the malar fat pad. This aspect is combined with the volumetric reduction of infraorbital and zygomatic areas that are mainly caused by the volume reduction of the deep fat compartments (infraorbital fat, deep medial cheek fat and lateral SOOF).
The volumetric modifications of superficial and deep fat compartments appear to be confirmed from the histologic point of view, in a recent study [53] that demonstrated in old cadaveric specimens (47–101 years, mean 71 years) a smaller adipocyte size in the deep medial cheek fat compared to the nasolabial fat; unfortunately in this study these findings were not compared to a younger group and nor was whether these size differences of superficial and deep adipocytes are present in younger subjects when the volumetric compartments change have not yet developed. For a truly controlled study of fat pads age-related changes, it is mandatory to have a younger cohort with which compare the histologic findings in cadavers of elderly people. Such a cohort may come from those having fat removed during reconstructive and cosmetic surgery.
Weight modification and weight differences can influence the volume of fat compartments but it is not well-know to date how this occurs. The clinical observation of submental fat hypertrophy concomitant with deep cheek fat atrophy in overweight patients suggests that weight gain may affect mainly the superficial compartments [30]. Meanwhile, a histologic study on cadavers showed the adipocyte size is increased in both the superficial and deep cheek compartments with higher weight [53].
Wan et al. [16] suggest that the different mechanical environments of the superficial and deep compartments of the midface also contribute to their morphological difference. This is due to the different anatomical location of the two fat layers: superficial fat compartments are located adjacent to the muscles of facial expression, while the deep fat pads lies directly on the periosteum. The continuous compression of the deep fat pads against bone during facial muscle movements and mastication may explain their tendency to selectively hypotrophy [54,55]. The same authors suggest that the proximity of superficial fat pads to the facial muscles may render them more metabolically active, thus requiring a more extensive and vascularized fascial network compared to the deep fat compartments as shown in histologic studies [16,17,25].
The anatomic modifications of the fat compartment of the face are one of the most important causes of facial aging. The causes of such changes are actually only partially understood, and their clinical implications are yet to be completely clarified. The introduction of the compartmentalization concept of adipose tissue of the face has resulted in an important improvement in our capability to assess the aging of the face and the injection technique based on the compartment-specific volume augmentation has improved our ability to treat the aging of midface [31,32]. Further anatomical, physiological, metabolic and histological studies are necessary to continue to better understand the behavior of fat compartments.
An acknowledge is due to the donors for our research.
All authors disclose any potential sources of conflict of interest. “The author(s) declare(s) that there is no conflict of interest regarding the publication of this paper.”
- Pessa JE (2000) An algorithm of facial aging: verification of Lambros's theory by three-dimensional stereolithography, with reference to the pathogenesis of midfacial aging, scleral show, and the lateral suborbital trough deformity. Plast Reconstr Surg 106: 479-488. [crossref]
- Pessa JE, Desvigne LD, Lambros VS, Nimerick J, Sugunan B, et al. (1999) Changes in ocular globe-to-orbital rim position with age: implications for aesthetic blepharoplasty of the lower eyelids. Aesthetic Plast Surg 23: 337-342. [crossref]
- Shaw RB Jr, Kahn DM (2007) Aging of the midface bony elements: a three-dimensional computed tomographic study. Plast Reconstr Surg 119: 675-681. [crossref]
- Gosain AK, Klein MH, Sudhakar PV, Prost RW (2005) A volumetric analysis of soft-tissue changes in the aging midface using high-resolution MRI: implications for facial rejuvenation. Plast Reconstr Surg 115: 1143-1152. [crossref]
- Furnas DW (1989) The retaining ligaments of the cheek. Plast Reconstr Surg 83: 11-16. [crossref]
- Stuzin JM, Baker TJ, Gordon HL (1992) The relationship of the superficial and deep facial fascias: relevance to rhytidectomy and aging. Plast Reconstr Surg 89: 441-449. [crossref]
- Byrd HS, Andochick SE (1996) The deep temporal lift: a multiplanar, lateral brow, temporal, and upper face lift. Plast Reconstr Surg 97: 928-937. [crossref]
- Moss CJ, Mendelson BC, Taylor GI (2000) Surgical anatomy of the ligamentous attachments in the temple and periorbital regions. Plast Reconstr Surg 105: 1475-1490. [crossref]
- Mendelson BC, Muzaffar AR, Adams WP Jr (2002) Surgical anatomy of the midcheek and malar mounds. Plast Reconstr Surg 110: 885-896. [crossref]
- Lucarelli MJ, Khwarg SI, Lemke BN, Kozel JS, Dortzbach RK (2000) The anatomy of midfacial ptosis. Ophthalmic Plast Reconstr Surg 16: 7-22. [crossref]
- Owsley JQ, Roberts CL (2008) Some anatomical observations on midface aging and long-term results of surgical treatment. Plast Reconstr Surg 121: 258-268.
- Donath AS, Glasgold RA, Glasgold MJ (2007) Volume loss versus gravity: new concepts in facial aging. Curr Opin Otolaryngol Head Neck Surg 15: 238-243. [crossref]
- Gierloff M, Stöhring C, Buder T, Gassling V, Açil Y, et al. (2012) Aging changes of the midfacial fat compartments: a computed tomographic study. Plast Reconstr Surg 129: 263-274. [Crossref]
- Sullivan PK, Drolet BC (2013) Extended lower lid blepharoplasty for eyelid and midface. Plast Reconstr Surg 132: 1093-1101. [Crossref]
- Rohrich RJ, Ghavami A, Constantine FC, Unger J, Mojallal A (2014) Lift-and-fill face lift: integrating the fat compartments. Plast Reconstr Surg 133: 756e-767e. [crossref]
- Wan D1, Amirlak B1, Rohrich R1, Davis K1 (2014) The clinical importance of the fat compartments in midfacial aging. Plast Reconstr Surg Glob Open 1: e92. [crossref]
- Rohrich RJ, Pessa JE (2008) The retaining system of the face: histologic evaluation of the septal boundaries of the subcutaneous fat compartments. Plast Reconstr Surg 121: 1804-1809. [Crossref]
- Gierloff M, Stöhring C, Buder T, Wiltfang J (2012) The subcutaneous fat compartments in relation to aesthetically important facial folds and rhytides. J Plast Reconstr Aesthet Surg 65: 1292-1297. [Crossref]
- Rohrich RJ, Pessa JE, Ristow B (2008) The youthful cheek and the deep medial fat compartment. Plast Reconstr Surg 121: 2107-2112. [crossref]
- Dulguerov N, D'Souza A (2011) Update on treatment rationale and options for the ageing face. Curr Opin Otolaryngol Head Neck Surg 19: 269-275. [crossref]
- Farkas JP, Pessa JE, Hubbard B, Rohrich RJ (2013) The Science and Theory behind Facial Aging. Plast Reconstr Surg Glob Open 1. [crossref]
- Gierloff M (2012) Reply: The facial aging debate of deflation versus attenuation: attenuation strikes back. Plast Reconstr Surg 130: 182e. [Crossref]
- Rohrich RJ, Ghavami A, Lemmon JA, Brown SA (2009) The individualized component face lift: developing a systematic approach to facial rejuvenation. Plast Reconstr Surg 123: 1050-1063. [Crossref]
- Reece EM, Rohrich RJ (2008) The aesthetic jaw line: management of the aging jowl. Aesthet Surg J 28: 668-674. [crossref]
- Schaverien MV, Pessa JE, Rohrich RJ (2009) Vascularized membranes determine the anatomical boundaries of the subcutaneous fat compartments. Plast Reconstr Surg 123: 695-700. [crossref]
- Pilsl U, Rosmarin W, Anderhuber F (2014) The premaxillary space: a location for filler injection? Dermatol Surg 40: 301-304. [crossref]
- Pessa JE, Rohrich RJ (2012) Discussion: Aging changes of the midfacial fat compartments: a computed tomographic study. Plast Reconstr Surg 129: 274-275. [Crossref]
- Kretlow JD, Hollier LH Jr, Hatef DA (2012) The facial aging debate of deflation versus attenuation: attenuation strikes back. Plast Reconstr Surg 130: 180e-181e. [Crossref]
- Alghoul M, Codner MA (2013) Retaining ligaments of the face: review of anatomy and clinical applications. Aesthet Surg J 33: 769-782. [crossref]
- Rohrich RJ, Arbique GM, Wong C, Brown S, Pessa JE (2009) The anatomy of suborbicularis fat: implications for periorbital rejuvenation. Plast Reconstr Surg 124: 946-951. [crossref]
- Sandoval SE, Cox JA, Koshy JC, Hatef DA, Hollier LH (2009) Facial fat compartments: a guide to filler placement. Semin Plast Surg 23: 283-287. [crossref]
- Fitzgerald R, Rubin AG (2014) Filler placement and the fat compartments. Dermatol Clin 32: 37-50. [crossref]
- Rohrich RJ, Pessa JE (2007) The fat compartments of the face: anatomy and clinical implications for cosmetic surgery. Plast Reconstr Surg 119: 2219-2227. [crossref]
- Mitz V, Peyronie M (1976) The superficial musculo-aponeurotic system (SMAS) in the parotid and cheek area. Plast Reconstr Surg 58: 80-88. [crossref]
- Har-Shai Y, Bodner SR, Egozy-Golan D, Lindenbaum ES, Ben-Izhak O, et al. (1996) Mechanical properties and microstructure of the superficial musculoaponeurotic system. Plast Reconstr Surg 98: 59-70. [Crossref]
- Ghassemi A, Prescher A, Riediger D, Axer H (2003) Anatomy of the SMAS revisited. Aesthetic Plast Surg 27: 258-264. [crossref]
- Pessa JE, Rohrich RJ (2012) Facial topography. Clinical anatomy of the face. QMP 2012.
- Rees EM, Pessa JE, Rohrich RJ (2008) The mandibular septum: anatomical observations of the jowls in aging-implications for facial rejuvenation. Plast Reconstr Surg 121: 1414-1420. [Crossref]
- Kikkawa DO, Lemke BN, Dortzbach RK (1996) Relations of the superficial musculoaponeurotic system to the orbit and characterization of the orbitomalar ligament. Ophth Plast Reconstr Surg 12: 77-88. [Crossref]
- Wong CH, Hsieh MK, Mendelson B (2012) The tear trough ligament: anatomical basis for the tear trough deformity. Plast Reconstr Surg 129: 1392-1402. [crossref]
- Muzaffar AR, Mendelson BC, Adams WP Jr (2002) Surgical anatomy of the ligamentous attachments of the lower lid and lateral canthus. Plast Reconstr Surg 110: 873-884. [crossref]
- DeFatta RJ, Williams EF 3rd (2009) Evolution of midface rejuvenation. Arch Facial Plast Surg 11: 6-12. [crossref]
- McGregor M (1959) Face Lift Techniques. Presented to the Annual Meeting of the California Society of Plastic Surgeons. Yosemite, California.
- Pessa JE, Garza JR (1997) The malar septum: the anatomic basis of malar mounds and malar edema. Aesthet Surg J 17: 11-17. [crossref]
- Pilsl U, Anderhuber F, Rzany B (2012) Anatomy of the cheek: implications for soft tissue augmentation. Dermatol Surg 38: 1254-1262. [crossref]
- Pilsl U, Anderhuber F (2010) The septum subcutaneum parotideomassetericum. Dermatol Surg 36: 2005-2008. [Crossref]
- Pontius AT, Williams EF 3rd (2005) The extended minimal incision approach to midface rejuvenation. Facial Plast Surg Clin North Am 13: 411-419. [crossref]
- Loukas M, Kapos T, Louis RG Jr, Wartman C, Jones A, et al. (2006) Gross anatomical, CT and MRI analyses of the buccal fat pad with special emphasis on volumetric variations. Surg Radiol Anat 28: 254-260. [Crossref]
- Stuzin JM, Wagstrom L, Kawamoto HK, Baker TJ, Wolfe SA (1990) The anatomy and clinical applications of the buccal fat pad. Plast Reconstr Surg 85: 29-37. [crossref]
- Li WT, Xu DC, Zhong SZ (1993) Applied anatomy of the buccal fat pad transposition for the treatment of soft tissue defects in the maxillofacial region. Chin J Clin Anat 11: 165-170
- Donofrio LM1 (2000) Fat distribution: a morphologic study of the aging face. Dermatol Surg 26: 1107-1112. [crossref]
- Gosain AK, Amarante MT, Hyde JS, Yousif NJA (1996) Dynamic analysis of changes in the nasolabial fold using magnetic resonance imaging: Implications for facial rejuvenation and facial animation surgery. Plast Reconstr Surg 98: 622-636. [Crossref]
- Wan D, Amirlak B, Giessler P, Rasko Y, Rohrich RJ, et al. (2013) The differing adipocyte morphologies of deep versus superficial midfacial fat compartments: a cadaveric study. Plast Reconstr Surg 133: 615e-622e. [Crossref]
- Macchi V, Tiengo C, Porzionato A, Stecco C, Vigato E, et al. (2010) Histotopographic study of the fibroadipose connective cheek system. Cells Tissues Organs 191: 47-56. [Crossref]
- Kahn JL, Wolfram-Gabel R, Bourjat P (2000) Anatomy and imaging of the deep fat of the face. Clin Anat 13: 373-382. [crossref]




