Abstract
Background: Iatrogenic endometriosis and leiomyomatosis are potential complications of minimally invasive gynecologic surgery associated with morcellation performed during either laparoscopic myomectomy or laparoscopic supracervical hysterectomy for benign indications.
Case(s): We present three cases of iatrogenic dissemination of benign endometrial and/or myometrial tissue due to power morcellation in which two cases were managed surgically, one requiring laparatomy and a bowel resection, and one was managed medically.
Conclusion: Power morcellation may result in seeding and implantation of benign viable endometrial and myometrial tissue during laparoscopic surgery for benign indications. Hence, patient selection and extensive counseling related to the risks and benefits of this surgical approach are crucial given the potentially serious complications of disseminated endometrial and/or myometrial tissue after morcellation.
Key words
iatrogenic endometriosis, leiomyomatosis, morcellation, power morcellation, laparoscopy
Teaching points
- Power morcellation may result in seeding and implantation of benign viable endometrial and myometrial tissue during laparoscopic surgery with potentially serious long-term complications.
- Patients who suffer from complications of uncontained morcellation can be managed both surgically and medically, as appropriate to their clinical status and presenting symptoms.
- Careful patient selection and extensive patient counseling regarding the risks and benefits of this surgical approach is vital given the potential complications related to the spread of uterine tissue, both benign and malignant.
Introduction
Uterine leimyomas or fibroids are the most common type of tumors of the female reproductive system. In 2012, it was estimated that 200,000 hysterectomies and 30,000 myomectomies were performed for fibroid-related symptoms in the United States [1]. Minimally invasive surgery may include the use of intra-abdominal manual or power morcellation to remove the uterine corpus or leiomyoma from the abdomen. The use of power morcellation, first introduced in 1995, involves reduction of a solid tissue specimen into smaller pieces using a hand held laparoscopic morcellation device and removal of the subsequent dissected specimen through existing incisions. Risks associated with morcellation during a laparoscopic hysterectomy or myomectomy include injuries to the vasculature, small and large bowel, bladder, ureter, fallopian tubes and omentum. Complication rates are estimated to be 0.02-0.07% [2-3]. While a tremendous amount of attention has recently focused on the potential for unintended morcellation of occult leiomyosarcoma, it is important to recognize that the iatrogenic dissemination of fragments of benign tissue following power morcellation appears to be the most common complication. Although the estimated incidence of parasitic myomas after hysterectomy with power morcellation is reported to be less than 1%. [4], Resultant complications can be severe. In this series, we present four cases of iatrogenic dissemination of benign endometrial and myometrial tissue secondary to uterine power morcellation.
Cases
Case #1: Surgical management
Patient presentation: A 46-year-old African American female, gravida one para one, presented with “throbbing, crampy,” cyclical abdominal pain. Her surgical history was remarkable for a supracervical hysterectomy for uterine fibroids, with uncontained power morcellation two years prior. Her past medical history was significant for asthma, anemia and diverticulitis. The patient had no known history of endometriosis. Her family history was negative for any known gynecologic, breast or gastrointestinal malignancies. At presentation, a CT scan of the abdomen and pelvis, noted three opacities. The first mass-like opacity abutted the lateral wall of the descending colon in the anterior peritoneal surface and measured 25 mm x 20 mm. Also identified were a second lesion, medial to the descending colon and measuring 32 mm x 32 mm, as well as a third, more inferior and anterior lesion measuring 25 mm x 34 mm (Figure 1). An ultrasound-guided left lower quadrant mass biopsy was consistent with endometriosis and pathology results revealed a benign glandular element, hemosiderin laden macrophages, and an endometrial stromal component with the presence of benign-appearing smooth muscle, consistent with endometriosis.
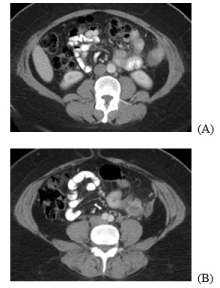
Figure 1. CT Abdomen/Pelvis of multiple symptomatic endometriomas in 46 year old following laparoscopic hysterectomy (A-B).
Surgical course: The decision was made to proceed with an diagnostic laparoscopy. Intra-abdominal survey revealed an endometrioma adherent to the anterior abdominal wall at the T 10 level in the left mid-clavicular line with tethering of the omentum and small bowel. Another endometrioma was identified at the T 8 level, also in the mid-clavicular line. Further endometriomas were noted to be adherent to the small bowel and descending colon. Due to the degree of adhesions and the extent of the endometriomas, complete laparoscopic resection was not possible and a midline vertical laparotomy was performed. Intraoperative exploration revealed endometriomas to be invading and encompassing several segments the descending colon as well as the anterio-lateral abdominal wall. Given the extensive adhesive disease, a colonic resection with end-to-end anastomosis and bilateral salpingo-oophorectomy was performed.
Pathology: Pathology results revealed [i] a segment of resected colon measuring 12 x 9 cm with multiple firm subserosal nodules measuring 2 to 4.5 cm in diameter and [ii] an abdominal wall nodule measuring 2.5 x 5 x 2 cm that were positive for severe endometriosis.. No adenomatous dysplasia or malignancy was detected.
Post-operative course: The patient’s post-operative course was complicated by re-admission for a pelvic abscess. A transvaginal pelvic drain was placed and with cultures showing Candida albicans and Bacteroides fragilis. The patient completed an appropriate seven day course of antibiotics. On hospital day 6, the patient was noted to have worsening leukocytosis and thus repeat imaging was performed which showed an anterior abdominal wall collection of gas and fluid as well as a left upper quadrant collection of extra-luminal gas and fluid suspicious for an anastomotic leak. However, the patient improved clinically and was discharged home in stable condition after regaining bowel function. At her six week post-operative visit, the patient was noted to have resolution of her symptoms and was doing well.
Case #2: Surgical management
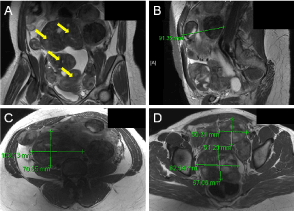
Patient presentation: The patient is a 41-year-old woman, gravida two para two, who presented for fertility counseling and management of symptomatic fibroids. Her history was significant for a previous laparoscopic myomectomy with power morcellation, four years earlier. Her family history was negative for any gynecologic malignancies. Pre-operative transabdominal and transvaginal ultrasound, as well as subsequent MRI of the pelvis, noted a 16-week size, enlarged uterus with multiple intramural, subserosal and pedunculated fibroids and moderate free fluid (Figure 2A-B). The largest noted fibroid measured 10.3 x 7.1 cm (Figure 2C). Three fibroids additional along the posterior wall measuring 4.3 x 3.3 cm, 5.6 x 5.1 cm and 8.3 x 6.7 cm, were found to exert a mass effect on the bladder and rectum (Figure 2B,D). A pre-operative Pap smear demonstrated no intraepithelial lesions or malignancy.
2021 Copyright OAT. All rights reserv
Figure 2. A/P (A), sagittal, (B) and C/S views (C-D) of multiple parasitic, symptomatic fibroids (yellow arrows) in a 41-year-old woman.
Surgical course: The patient underwent an exploratory laparotomy and abdominal myomectomy prior to moving forward with fertility treatment. Intra-operative findings were notable for multiple pedunculated, parasitic fibroids located on the fundus, including on the anterior and both lateral uterine surfaces, the anterior surface of the pelvis, the anterior abdominal wall, the right broad ligament, and the bowel. Extensive pelvic adhesions to the bowel and bladder were also noted.. One uterine fibroid was enveloped in bowel and a second posterior cervical fibroid was encased in the right broad ligament. The decision was made not to remove these fibroids due to the patient’s desire for future fertility and the risk of resultant hysterectomy. A total of 18 fibroid clusters comprised of 25 fibroids were removed.
Pathology: Final pathology consisted of 18 fibroid clusters ranging from 0.6 x 0.5 x 0.3 cm to 12.5 x 8.0 x 6.0 cm. Some clusters demonstrated hyaline degeneration. The fragments weighed a total of 818 grams.
Post-operative course: At her follow-up visit, the patient was recovering well in spite of a palpable posterior fundal fibroid.
Case #3: Medical management
Patient presentation: The patient is a 40-year-old African American, gravida one para one, who presented with a history of 2-3 days of monthly spotting and bilateral lower quadrant abdominal pain. Her past medical history was significant for a laparoscopic supracervical hysterectomy with uncontained power morcellation for an enlarged fibroid uterus and transfusion dependent menorrhagia. Other surgical history was remarkable for a cholecystectomy. The patient had no history of endometriosis and her family history was significant for a paternal grandmother with ovarian cancer. Her exam was remarkable for a palpable, mobile, non-tender 5 cm supracervical mass. CT scan of the abdomen and pelvis demonstrated a large cluster of cystic lesions in the left lower quadrant measuring 10.1 x 9.0 x 5.5 cm and 1.7 x 4.2 cm in the right lower quadrant respectively consistent with possible peritoneal carcinomatosis (Figure 3). A soft tissue mass was also noted within the cul-de-sac, measuring 5.0 x 7.8 cm possibly representing cervical malignancy. CA-125 levels were noted to be elevated at 117 U/mL. The patient had a repeat Pap smear of the cervix which was negative for intraepithelial lesion or malignancy and negative for high risk human papilloma virus (HPV).
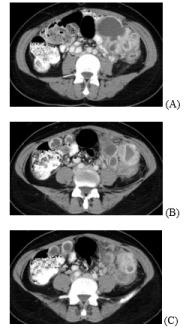
Figure 3. CT of Abdomen/Pelvis of clusters of endometriomas in 40-year-old following laparoscopic supracervical hysterectomy (A-C).
Medical management: A peritoneal cyst biopsy with aspiration was performed. Cyst contents were chocolate brown in color, favoring an endometrioma. Pathology results revealed benign mesothelial cells, acute and chronic inflammation, few granulomas, macrophages and blood. The patient was started on continuous combined oral contraceptives given the likelihood that the cysts were endometriomata. At her follow-up visit, the patient was noted to have resolution of her symptoms and was doing well.
Discussion
Over the last few decades, minimally invasive gynecologic surgery has become the approach of choice for many patients requiring gynecologic surgery. With the advent of robotic surgery and formal residency training in advanced laparoscopic skills, uterine sparing laparoscopic surgeries such as a myomectomy or minimally invasive removal of the uterus has become a common procedure. Primary benefits include decreased size of incision, quicker recovery relative to a laparotomy, minimal blood loss, lower risk of infection and same day discharge to home [4]. Known risks include occult injury to vasculature or bowel at time of initial entry. This study highlights an increasingly recognized concern relating to extraction of large tissue in fragments after morcellation. Much attention has recently been placed on inadvertent morcellation of malignant tissue as recently reported in a few cases [5]. In this case series, we focus on the tissue dissemination risks that may be associated with morcellation of benign tissue such as uterine leiomyomas and entire uterine specimen with the underlying endometrium [6]. While such risks are predominantly associated with power morcellation, any type of uncontained morcellation renders the patient to intraabdominal disbursement of tissue fragments and associated risks.
Minimally invasive gynecologic surgery: The advantages of minimally invasive gynecologic surgery, such as vaginal hysterectomy or laparoscopic hysterectomy, over abdominal hysterectomies are well documented. A Cochrane review in 2009 assessed 34 hysterectomy studies involving 4,495 women and found that the benefits of minimally invasive hysterectomy included a quicker return to normal activities (MD 13.6 days), lower intra-operative blood loss (MD 45 cc), smaller drop in hemoglobin (MD 0.55 g/dl), shorter hospital stay (MD 2.0 days), and fewer wound or abdominal wall infections (OR 0.31) at the cost of increased urinary tract (bladder or ureter) injuries (OR 2.41) and longer operative time (MD 20.3 minutes) [4]. Similarly, benefits of a laparoscopic myomectomy versus open myomectomy include a decreased blood loss, fewer fever, wound or abdominal wall infections and a more rapid recovery.6 Furthermore, patients who undergo abdominal hysterectomy have three times the risk of mortality compared to those who have laparoscopic hysterectomy [7].
Tissue morcellation: Minimally invasive gynecologic surgery often require the use of intra-abdominal morcellation to remove large tissue specimen. During the process of uncontained morcellation, tissue particles may be dispersed into the peritoneal cavity and abdominal wall. Viable tissue fragments may attach to intrabdominal peritoneal surfaces to develop into nodular foci. With benign tissue this leads to diffuse peritoneal leiomyomatosis, endometriosis, adenomyosis, or adenomyomatosis. In cases of unrecognized malignant tissue, resultant pathology includes leiomyosarcoma, endometrial carcinoma or endometrial stromal sarcoma [7]. Therefore, laparoscopic morcellation has recently come under scrutiny regarding risks of mortality due to inadvertent morcellation of a malignant lesions and what benefits of a minimally invasive procedure outweigh associated risks [8].
Importantly we highlight in this study, the need to recognize potential complications that may arise from morcellation of even benign tissue. We present three cases of iatrogenenic dissemination of benign endometrial and myometrial tissue due to uterine morcellation. Despite the absence of occult malignancy, as these case studies demonstrate, there can be significant morbidity resulting from the primary procedure and route of tissue extraction. Surgeons considering a minimally invasive surgical approach without en bloc tissue removal even in benign cases should be aware of the potential complications associated with iatrogenic dissemination viable tissue. Such risks are further enhanced with the use of power morcellation. Further studies, many of which are ongoing, are needed to understand whether tissue containment systems can mitigate the risks of benign tissue implantation during morcellation. Hence, in addition to a complete pre-operative evaluation, careful patient selection and extensive patient counseling are of crucial importance if considering morcellation of any kind.
IRB approval
The Partners Healthcare Institutional Review Board deemed this study exempt.
Financial support
RMA is supported by the Agency for Healthcare Research and Quality (AHRQ), and Patient-Centered Outcomes Research Institute (PCORI) through COMPARE-UF (Comparing Options for Management: Patient-Centered Results for Uterine Fibroids).
References
- Cardozo ER, Clark AD, Banks NK, Henne MB, Stegmann BJ, et al. (2012) The estimated annual cost of uterine leiomyomata in the United States. Am J Obstet Gynecol 206: e1-e9. [Crossref]
- American Association of Gynecologic Laparoscopists (AAGL) (2014) AAGL practice report: Morcellation during uterine tissue extraction. J Minim Invasive Gynecol 21: 517-530. [Crossref]
- Senapati S, Tu FF, Magrina JF (2015) Power morcellators: A review of current practice and assessment of risk. Am J Obstet Gynecol 212: 18-23. [Crossref]
- Nieboer TE, Johnson N, Lethaby A, Tavender E, Curr E, et al. (2009) Surgical approach to hysterectomy for benign gynecological disease. Cochrane Database Syst Rev 3: CD003677. [Crossref]
- Winner B, Porter A, Velloze S, Biest S (2015) Uncontained Compared with Contained Power Morcellation in Total Laparoscopic Hysterectomy. Obstet Gynecol 126: 834-838. [Crossref]
- Van der Meulen JF, Pijnenborg JM, Boomsma CM, Verberg MF, Geomini PM, et al. (2016) Parasitic myoma after laparoscopic morcellation: a systematic review of the literature. BJOG 123: 69-75. [Crossref]
- American College of Obstetricians and Gynecologists (2014) Power Morcellation and Occult Malignancy in Gynecologic Surgery: A Special Report. ACOG.
- Park JY (2012) The impact of tumor morcellation during surgery on the prognosis of patients with apparently early uterine leiomyosarcoma. Gynecol Oncol 124: 173. [Crossref]


 2021 Copyright OAT. All rights reserv
2021 Copyright OAT. All rights reserv
