Case report
The patient, male, 51 years old. Due to visual disorder 7 years, trunk and lower extremity weakness with numbness 3 years, recurrence 5 days. His right eye vision suddenly drops 7 years ago, the onset of visual loss serious after 3 months; the eye vision suddenly drops 5 years ago, considering primary bilateral optic atrophy (ONA) at that time. No improvement with the conventional therapy, no automatic recovery or improvement on vision for long time. The brain and spinal cord were examined at that time. The double lower limbs were weakness and numbness of the patients appeared three years ago, Involving trunk gradually, with incontinence of urine and stool. Being treated in the local hospital and considered acute myelitis (AM). It appears nipples, numbness and weakness below the bilateral breasts level after catching cold five days ago, which was very difficult as standing and walking, with headache in changing pastual position. No previous history of injury and poisoning and familial history no similar disease.
Physical examination: The patient was lucid and clear thinking, his computing power, memory and orientation was good. His bilateral cornea was mild cloudy and pupil was round about 4mm in diameter with dull in light reflection. The binocular vision has little light and Fingers on his chest was not identified, but open or close the eyes was good. Fundus examination revealed bilateral optic atrophy, optic papilla changed obviously, optic disc showed grayish white, retinal artery had thin and narrow. Mouth no skew, loll centered, reflex is abating, shrug normal. Mild difficulty breathing, heart rate 90 beats / min, rhythm and tidy, no heart murmur. abdominal flat, no tenderness. Muscle tension of double upper limbs was normal and muscle tension of double lower limbs was reducing. The muscle strength of left upper limb was grade 3 and the right upper limb grade 2, double lower limbs grade 1. Algesia was decreasing obviously below the second thoracic plane in bilateral thoracolumbar, there was a chest hypoalgesia transition zone. The right Babinski sign is positive sign suspicious, double lower limbs mild muscle atrophy.
Auxiliary examination
Random blood sugar: 5.6mmol/L, urine protein is slightly higher in routine urine, total white blood cells slightly higher. The routine and enhanced MRI examination in spinal cord showed abnormal signal at thoracic and lumbar spinal cord (Figures 1&2), especially T5-11 thoracic intramedullary had swelling and gadolinium enhanced, considering a spinal inflammatory lesion. On the other hand, head MRI examination showed there were some scattered abnormal signal in white matter junction area below the left frontal and parietal and bilateral basal ganglia, with T1 lower signal and T2 higher signal (Figures 3&4). Cerebrospinal fluid (CSF) examination showed the pressure was 130mm H2O, the total cell number increased, the mononuclear cell (MNC) is 52×106/L. The protein electrophoresis of oligoclonal bands (OB) was positive, while serum OB was negative. Visual evoked potential (VEP) and somatosensory evoked potential (SEP) examination was abnormal, as the P100 latency and amplitude decreased mainly.
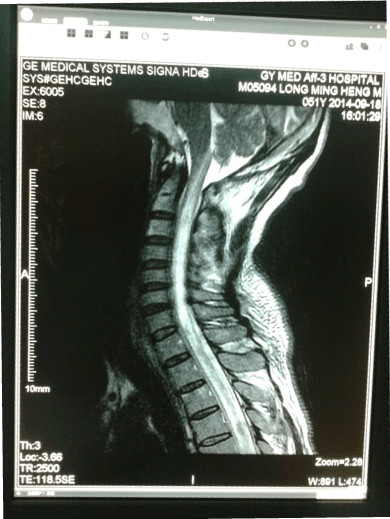
Figure 1. MRI-T1--Some abnormal signal at thoracic and lumbar spinal cord were found
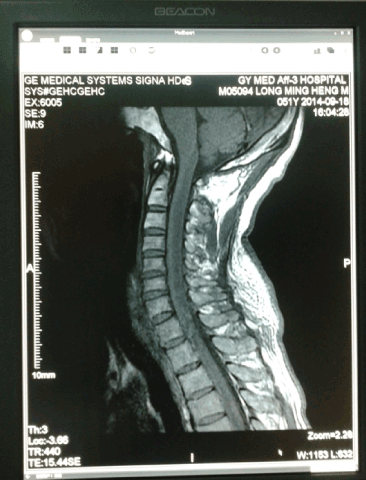
Figure 2. MRI-T1--Some abnormal signal at thoracic and lumbar spinal cord were found
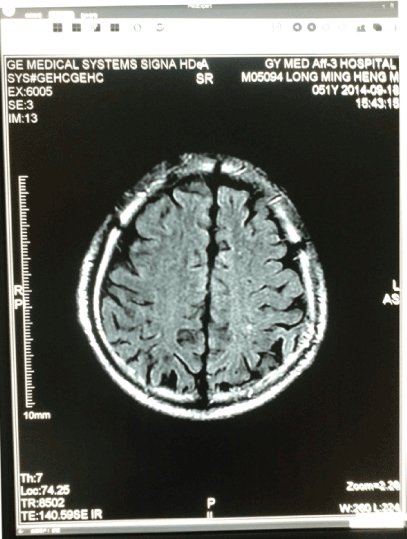
Figure 3. Head MRI-T1show some scattered abnormal signal spots
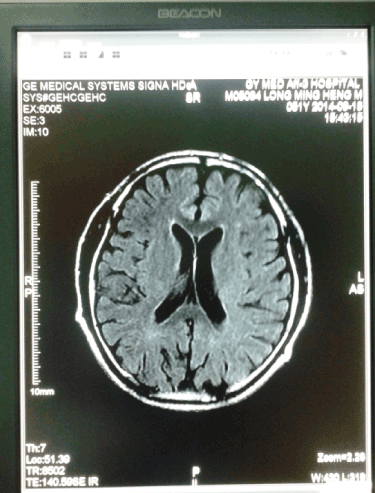
Figure 4. Head MRI-T2 show some scattered abnormal signal spots
Admission diagnosis: 1, neuromyelitis optica (NMO; 2, multiple sclerosis (MS)). After admission he was given intermittent oxygen inhalation, ECG monitoring, bladder irrigation, retention catheterization, prevent bedsore, hemiplegia limb function training. Edaravone, ginkgo leaf extract, Vit B1, Vit B12, Vit D, etc. for treatment. Acyclovir was used for antiviral and cefoperazone sulbactam for anti-inflammatory therapy, and the high-dose intravenous methylprednisolone pulse therapy for 5 days, but invalid. The requirement of automatic discharge was asked from this patient after admission ten days. At that time, vital signs were stable, but no restoration of limb function.
Discussion
MS is an autoimmune disease in the white matter of vicinity of the brain and spinal cord with demyelination inflammation. MS with the spinal cord type is a MS which occurs injury in the spinal cord not in brain. If the injury occurs in the spinal cord and optic nerve the MS is usually diagnosed as NMO. Yet it remains some debate for NMO is a subtype of MS or an independent disease. Mezer etc. assessed macromolecular tissue volume (MTV) by quantitative neuroimaging and thought that MTV had not only good sensitivity for the diagnosis MS but also can analyzed the cognitive function by the change of pathological effects in patients [1]. The routine head and spinal cord MRI, adding history, symptoms, signs and other auxiliary examination was finished for differential diagnosis of MS and NMO in this case.AM refers to a disease from nonspecific inflammation caused by spinal cord demyelinating lesions which have some pathological changes such as myelin swelling, demyelination, axonal degeneration, peripheral lymphocyte proliferation, vascular inflammation cell infiltration. Influenza, Measles, chickenpox, Measles, mumps, EB virus, Cytomegalovirus and Mycoplasma such as pathogens may be associated with the occurrence of this disease. The patient had an upper respiratory infection before admission and the typical clinical manifestations, adding some lesions found as spinal cord MRI, it seems to be more support for diagnosis of acute myelitis. However, there were obvious decrease at vision of right and left eye and abnormal fundus condition in this patient over 7 years ago and 5 years ago. It may have the intrinsic relation that he was suffering from ONA and later AM, so the final diagnosis as NMO is more reasonable, just a special NMO. Cock etc. has detected 4 cases of NMO (Devic syndrome) in mitochondrial DNA (mtDNA) mutation, any positive results are not found in 3460bp, 11778bp, 14484bp and other multiple sites, they reasoned that mtDNA mutations are not important in the pathogenesis of NMO [2]. This case did not detect any gene mutation, but it is not thought that gene mutation analysis is not important for diagnosis of NMO or MS. The common causes of ONA have retrobulbar neuritis, hereditary optic neuropathy, orbital tumors and intracranial tumor compression, ocular injury, neurotoxin, papillitis, papilla edema, retinal vein inflammation, retinal pigment degeneration, central retinal artery occlusion, membrane quinine poisoning, ischemic optic neuropathy, glaucoma, tuberculous meningitis, NMO, arachnoid phlogistic in the optic chiasm etc. Primary ONA generally refers to the cause is unknown, at least so far unknown exact etiology of ONA. If this patient was diagnosed as primary ONA, then the subsequent AM should be as an independent disease, but this patient was diagnosed as AM 3 years ago, vision loss is still in progress and optic nerve atrophy symptoms is still under development and aggravation, and the vision almost completely lost at that time. The longitudinal lesions up to 5 vertebral segments together with swelling and gadolinium enhanced also support this diagnosis for NMO. In addition, some abnormal signals in brain MRI, scattered under white matter and unlike the vascular distribution of the ischemic lesions, are found in this patient after admission, the number of cells increased and oligoclonal bands positive in CSF, VEP and SEP abnormal found, all support the diagnosis of MS in brain instead of encephalitis. Combining with a variety of symptoms and disease development the coexistence of NMO and MS are quite sure. Notably, NMO and MS are rarely existing in one patient, and sometimes the coexistence of spinal cord MS and regular MS condition is seen, as the difference of mechanism between NMO and MS is obvious but the difference of mechanism between spinal cord type MS and regular MS is a little.
Why coexist NMO and MS in one case? The possible reason is his patient has the atopic constitution, not only the relatively hyperthyroidism in cellular immune but also the relatively strong generation at water channel protein antibody belongs to the IgG category as this antibody is an indicator for diagnosing NMO with relative specificity [3]. Liu etc. have collected 138 patients from China mainland, and MS and NMO in the differential diagnosis is studied. There are 60 cases with MS, 73 cases with NMO and 5 cases with alike MS of the NMO-IgG antibody positive. They found that a comprehensive analysis for head MRI, evoked potentials and laboratory data (such as OB value, CD4+/CD8+) have been able to differentiate MS from NMO effectively. If no lesion in head MRI it is necessary, that the longitudinal extension of the spinal cord lesion (LESCLs) are found in MRI of the spinal cord for diagnosing NMO definitely [4]. Those five patients specifically listed with NMO-IgG antibody positive are similar to this case to some extent. This patient coexists both NMO and MS at same time, which suggest that part of the common genetic molecular pathway in mechanism of NMO and MS may undergo. The classic therapy is high-dose methylprednisolone pulse therapy (MPPT) for NMO. Recently Araki et al treated 7 NMO patients by using an interleukin 6 receptor antagonist tocilizumab (TCZ) [5]. It has been found that the neuropathic pain and fatigue were reduced and motor function was improved after one year for treatment. This case was treated with MPPT for 5 days, together with other symptomatic and supportive treatments, but the effect was poor, which suggest that this is a very special case of NMO again.
References
- Mezer A, Yeatman JD, Stikov N, Kay KN, Cho NJ, et al. (2013) Quantifying the local tissue volume and composition in individual brains with magnetic resonance imaging. Nat Med 19: 1667-1672. [Crossref]
- Cock H, Mandler R, Ahmed W, Schapira AH (1997) Neuromyelitis optica (Devic’s syndrome): no association with the primary mitochondrial DNA mutations found in Leber hereditary optic neuropathy. J Neurology Neurosurgery and Psychiatry 62:85-87. [Crossref]
- Zhang XH, Xu XH (2007) Diagnosis of multiple sclerosis and neuromyelitis optica. Zhonghua Yi Xue Za Zhi 87: 2739-2740. [Crossref]
- Liu Y, Zhao G, Yu H, Lyu C, Li Z, et al. (2014) Differentiation of neuromyelitis optica from multiple sclerosis in a cohort from the mainland of China. Chin Med J (Engl) 127: 3213-3218. [Crossref]
- Araki M, Matsuoka T, Miyamoto K, Kusunoki S, Okamoto T, et al. (2014) Efficacy of the anti-IL-6 receptor antibody tocilizumab in neuromyelitis optica: A pilot study. Neurology 82: 1302-1306. [Crossref]




