Abstract
The uterine rupture during pregnancy is one of the most serious complications, increase morbidity and maternal and fetal mortality. The uterine rupture by percrete placenta is rare. We present the case of a 27 years-old patient gravida 5, which enters by acute abdominal pain of predominance in the hypogastric region, that during its evolution presented hemodynamic compromise and increase of abdominal pain.
Introduction
Uterine rupture is an uncommon but potentially life-threatening obstetrical emergency for both mother and fetus. It occurs mostly during labor in the context of a previous uterine scar. Generally, uterine rupture refers to a complete separation of all uterine layers, including the uterine serosa, and this usually occurs most commonly in the setting of classical cesarean section [1]. The incidence of uterine rupture varies depending on the type and location of the prior uterine incision. The American College of Obstetricians & Gynecologists (ACOG) Practice Bulletin reports a uterine rupture risk of 0.5 to 0.9 percent for women with prior cesarean undergoing trial of labor [2]. However, the overall rate for uterine rupture with previous classical cesarean ranges from 0.6 to 12 percent as cited in the literature.
Case presentation
A 27 years old (gravida 5 parity 4) woman presented to emergency department with compliants of syncope and dyspnea, acute abdominal pain and hemorrhagic shock. On her physical examination, she had a Glascow coma scale of 15, tension arterial of 80/30 mmHg, pulse rate of 130 beats/minute. There was defans and rebound in all abdomen quadrants. Emergency ultrasound was performed in emergency department. USG revealed free fluid in the abdomen. An emergency laparotomy was performed for a probable diagnosis of intra-abdominal hemorrhage and the fetus found floating freely in the peritoneal cavity (Figure 1). Obstetrical hysterectomy was performed (Figures 2 and 3). We confirmed the diagnosis of uterine rupture by percreta placenta. The patient recovered and discharged healthy 5 days after the operation, while the fetus could not survive.
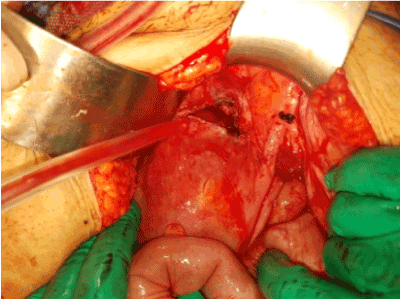
Figure 1. Diagnosis of intra-abdominal hemorrhage and fetus
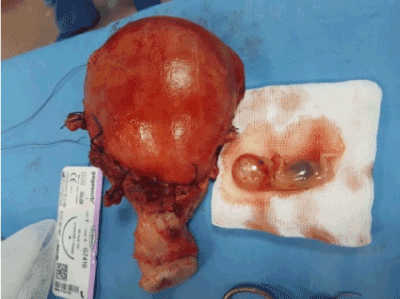
Figure 2. Obstetrical hysterectomy
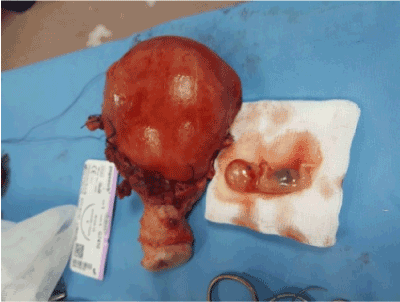
Figure 3. Obstetrical hysterectomy
Discussion
Spontaneous uterine rupture due to placenta percreta is a rare obstetric emergency with an estimated incidence of 1/5,000 pregnancies [3]. Placenta percreta accounts for 5% of all placental invasion anomalies [4]. Previous Caesarian section is the most common predisposing factor of abnormal placentation. The other risk factors are placenta previa, submucous myoma, endometritis, Asherman’s Syndrome, increased maternal age, uterine curettage [5]. In our case the patient had 4 Caesarian operations.
Spontaneous uterine rupture due to placenta percreta is rare. But it can be life threatening for both mother and fetus. The main cause of that in such cases is hemorrhage, disseminated intravascular coagulation and shock. The clinical spectrum of disease vary from abdominal pain to shock. in our case, the patient had hipovolemic shock. Intraabdominal hemorrhage due to placenta percreta can mimick many conditions. The differantial diagnosis includes intraabdominal solid organ rupturu (such as hepatic or splenic rupture), ovarian cyst rupture, heterotopic pregnancy.
Antenatal ultrasound is the technique of choice used to establish the diagnosis and guide clinical management as it is cost-effective and popular. If the ultrasound findings are suspicious or the placenta is located on the posterior wall, magnetic resonance imaging can be performed.It provides crucial information on the vascularization of the anatomic planes and of the degree of invasion, modifies the surgical strategy [6]. The differantial diagnosis constitutes a particular challenge for clinician as massive blood can be life threatening to patient. In our case, ultrasonography performed in emergency department. But the diagnosis was confirmed in the peroperative period.
Placenta percreta can be managed in two ways, first is surgical removal of the uterus and the surrounding tissues and another is conservative therapy including localized resection of the placental implantation site, over sewing, blunt dissection and packing tecniques. The choice between hysterectomy and conservative therapy is dependent on the severity of the placenta percreta and associated complications [7]. Hysterectomy is considered to be the gold standard approach in a hemodynamically unstable patient with massive intraperitoneal bleeding [8].
Conclusion
Placenta percreta induced spontaneuos uterine rupture is difficult to diagnose. The possibility of uterine rupture should always be kept in mind when a patient admitted to emergency department with compliants of syncope and dyspnea, acute abdominal pain and hemorrhagic shock.
Consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Conflict of interests
The authors declare that they have no conflict of interests.
References
- [1] Landon MB (2010) Predicting uterine rupture in women undergoing trial of labor after prior cesarean delivery. Semin Perinatol 34: 267–271. [Crossref]
- [2] American College of Obstetricians and Gynecologists (2010) ACOG Practice bulletin no. 115: vaginal birth after previous cesarean delivery. Obstet Gynecol 116: 450–463. [Crossref]
- [3] Gardeil F, Daly2021 Copyright OAT. All rights reservin pregnancy reviewed. Eur J Obstet Gynecol Reprod Biol 56: 107–110. [Crossref]
- [4] Roeters AE, Oudijk MA, Heydanus R, Bruinse HW (2007) Pregnancy outcome after intra-abdominal bleeding due to placenta percreta at 14 weeks of gestation. Obstet Gynecol 109: 574–576. [Crossref]
- [5] Oyelese Y, Smulian JC (2006) Placenta Previa, placenta accreta and vasa previa. Obstet Gynecol 107: 927-41. [Crossref]
- [6] Marcos HB, Semelka RC, Woravattaanakul S (1997) Normal Placenta: Gadolinium-Enhanced, Dynamic MR imaging. Radiology 205: 493-498. [Crossref]
- [7] Kazandi M (2003) Placenta Percreta: Report of Two Cases and Review of the Literature. Clin Exp Obstet Gynecol 30: 70-72. [Crossref]
- [8] Sparic R, Mirkovic L, Ravilic U, Janjic T (2014) Obstetric complications of placenta previa percreta. Vojnosanit Pregl 71: 1163-6. [Crossref]



