A male patient was brought in by ambulance to the Accident and Emergency department as a trauma call following an alleged self-stabbing to the head with a kitchen knife. The patient underwent both primary and secondary survey with additional input from Ophthalmology, Oral and Maxillofacial Surgery and Otolaryngology.
Detailed examination revealed an isolated penetrating incision injury with 2-inches of a serrated kitchen knife to the right temporal region. The right globe was soft to palpation, pupillary reflexes to light and accommodation both intact, and minimal proptosis was noted. However, reduced lateral movements of the right globe were evident.
The patient’s medical history was unremarkable. A corroborative social history revealed the patient was a frequent cannabis user and had become increasingly introverted and isolated in the weeks preceding the injury.
A CT angiogram taken confirmed a penetrating injury through the right intra-conal compartment, with the tip of the serrated blade lying within the right ethmoidal sinus. Probable transection of the right lateral and medial rectus muscles was reported with additional impingement of the optic nerve.
Following radiographic imaging, the patient was immediately taken to emergency theatres under the joint care of Ophthalmology and Oral and Maxillofacial Surgery, for exploration of the right orbit and lateral orbitotomy to remove the knife (Figures 1 and 2).
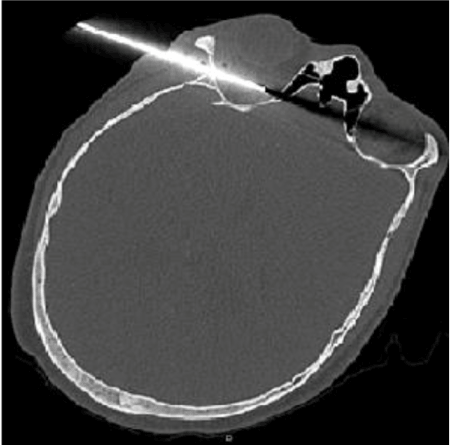
Figure 1. Axial view of the CT Head showing the knife penetrating the right lateral wall of the orbit and transecting the medial rectus muscle
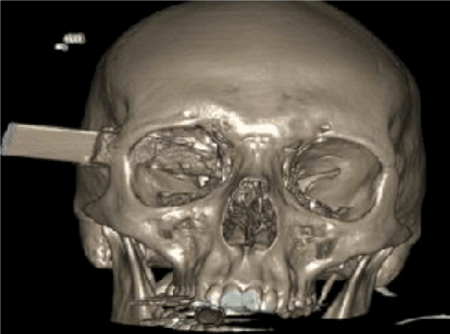
Figure 2. 3D reconstruction of the CT Head
Post operatively visual prognosis of the affected eye was initially deemed poor, with a visual acuity of 6/18 compared with 6/4 on the left. A diagnosis of post traumatic optic neuropathy was given. The patient was reviewed regularly by the Oral and Maxillofacial, Ophthalmology and Psychiatric teams post-operatively and was eventually transferred to an inpatient Psychiatric unit.
On 3-month Ophthalmology follow-up, the visual acuity had improved to 6/9 in the right eye but evidence of inferior hemifield loss resulting from direct trauma to the optic nerve was noted.
Post-operative psychiatric evaluation revealed diagnoses of anxiety and severe depression. The patient is currently subject to a Community Treatment Order.
Learning points
- Penetrating intra-conal injuries are associated with significant morbidity and mortality and often require a multidisciplinary approach to management [1].
- Lateral orbitotomy is a useful surgical technique for achieving adequate access to the orbit to aid in removal of foreign bodies and orbital tumours [2].
Trauma Team, University Hospital Aintree.
Ophthalmology Department, University Hospital Aintree.
- MacEwen C, Fullarton G (1986) A penetrating orbitocranial stab wound. British Journal of Ophthalmology 70: 147-149.
- Evans B, Mourouzis C (2009) Lateral orbitotomy: A useful technique in the management of severe traumatic disruption of the lateral orbital skeleton. International Journal of Oral and Maxillofacial Surgery 38: 984-987.


