Abstract
Erythema Multiforme Major is an acute inflammatory hypersensitivity reaction usually due to infections and to medications. However, it could be idiopathic in some cases. Pathognomonic target lesions are located symmetrically on extremities and in mucosa. It spontaneously resolves within 1-2 weeks; however, symptomatic care is usually necessary. In this report, we aimed to present a case of erythema multiforme major that necessitate symptomatic treatment.
Keywords
erythema multiforme, hypersensitivity, target lesion
Introduction
Erythema multiforme is acute, inflammatory skin disease and has two clinical forms, minor and major. It occurs as erythema multiforme minor in 90% of the cases. Erythema Multiforme Major, Stevens-Johnson Syndrome and Toxic Epidermal Necrosis are categorized as a common clinical syndrome[1]. Erythema multiforme major is an acute hypersensitive reaction that can be seen at all ages due to medications and infections such as herpes simplex virus and mycoplasma pneumonia[2]. No etiology can be detected in 25-50% of the cases[3]. Macular, papules, urticarial, bullous and purpuric lesions can be noted in patients with erythema multiforme. Especially target-like lesions are pathognomonic[4]. Patients' lesions spontaneously resolve without treatment in 1-2 weeks, but symptomatic treatment might be required[5]. In this report, we aimed to present a case of erythema multiforme major that necessitate symptomatic treatment.
Case report
A fifty-year-old woman referred to our clinic due to rashesin and around her mouth and nose, and on bilateral upper and lower extremities for 2-3 days. Her medical and family history was unremarkable. Except irregular use of a non-steroidal anti-inflammatory drug, she denied use of any other medications. A week before lesions develop, she had had a colposcopy due to suspicious test results of a PAP smear test for malignancy. The skin lesions first developed at the lower extremities and spreaded to upper extremities, to face and oral mucosa.
On physical examination her body temperature was 37°C, heart rate was 80 beatsper minute, blood pressure was 120mmHg systolic and 70mmHg diastolic. Mucosal erosion in oral cavity, crusted plaques on lipsand target lesions on dorsal face of hands and toes were noted (Figure 1-3).
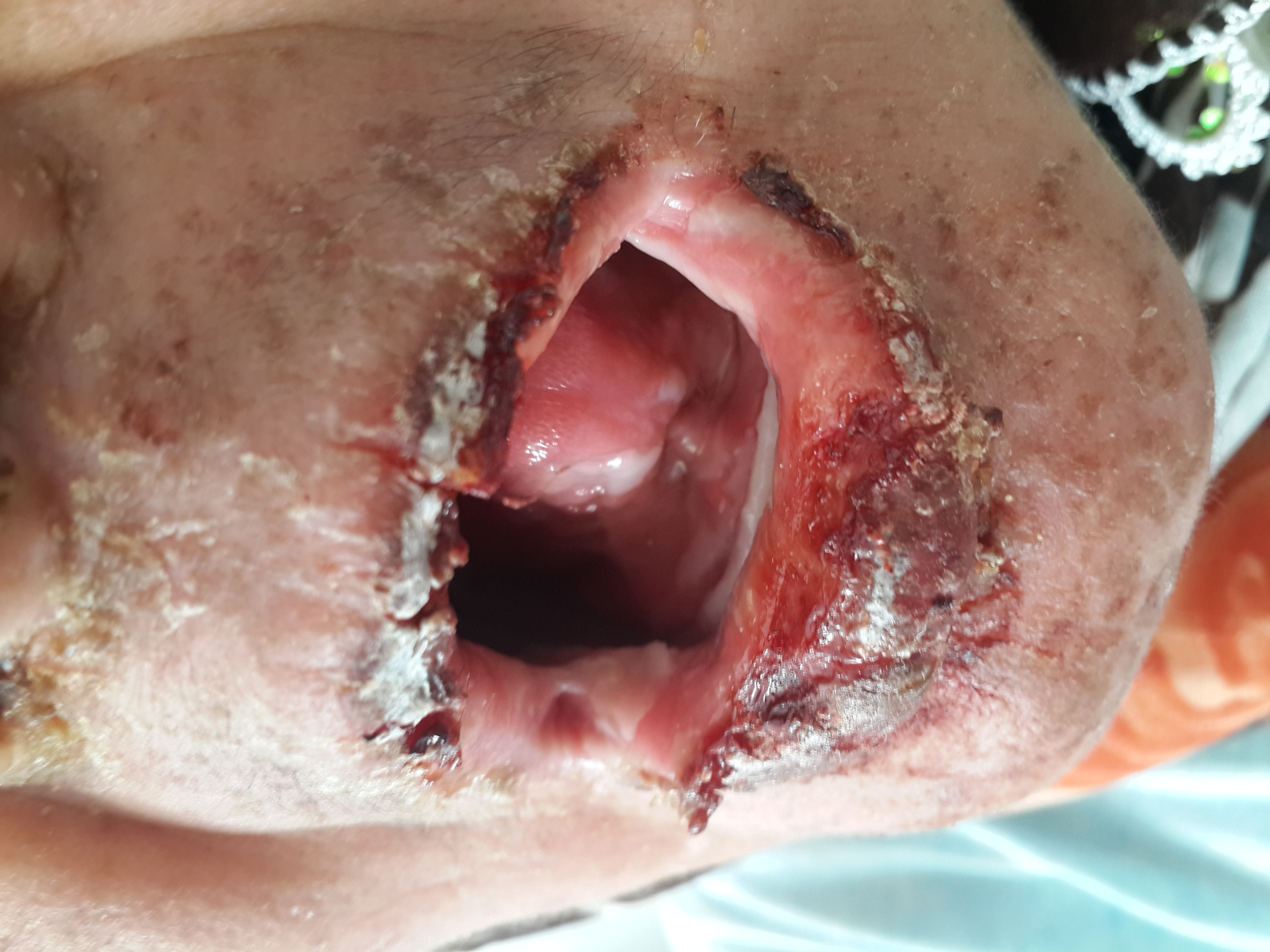
Figure 1. Crusted plaques on lips.
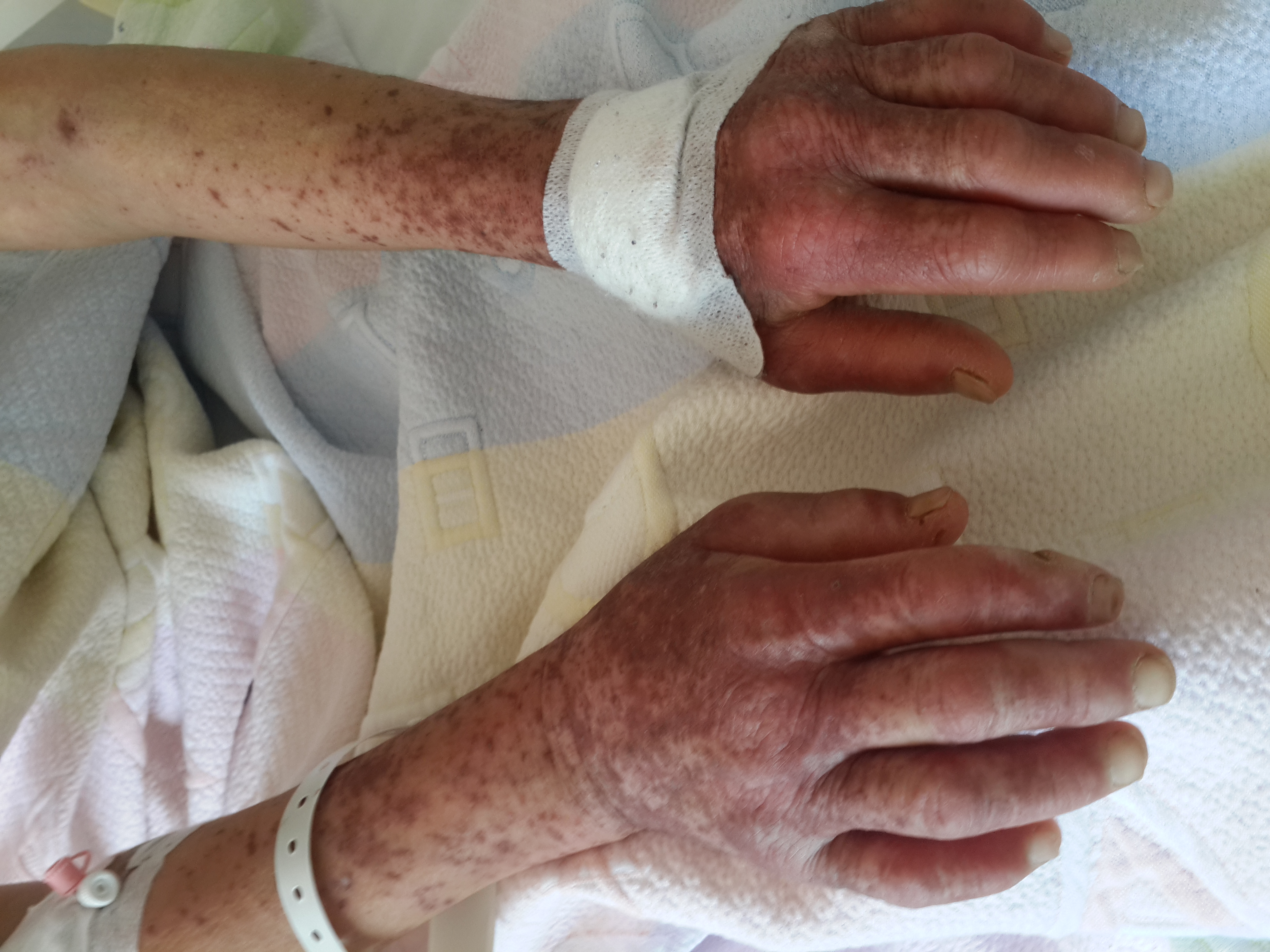
Figure 2. Target lesions on dorsal face of hands.
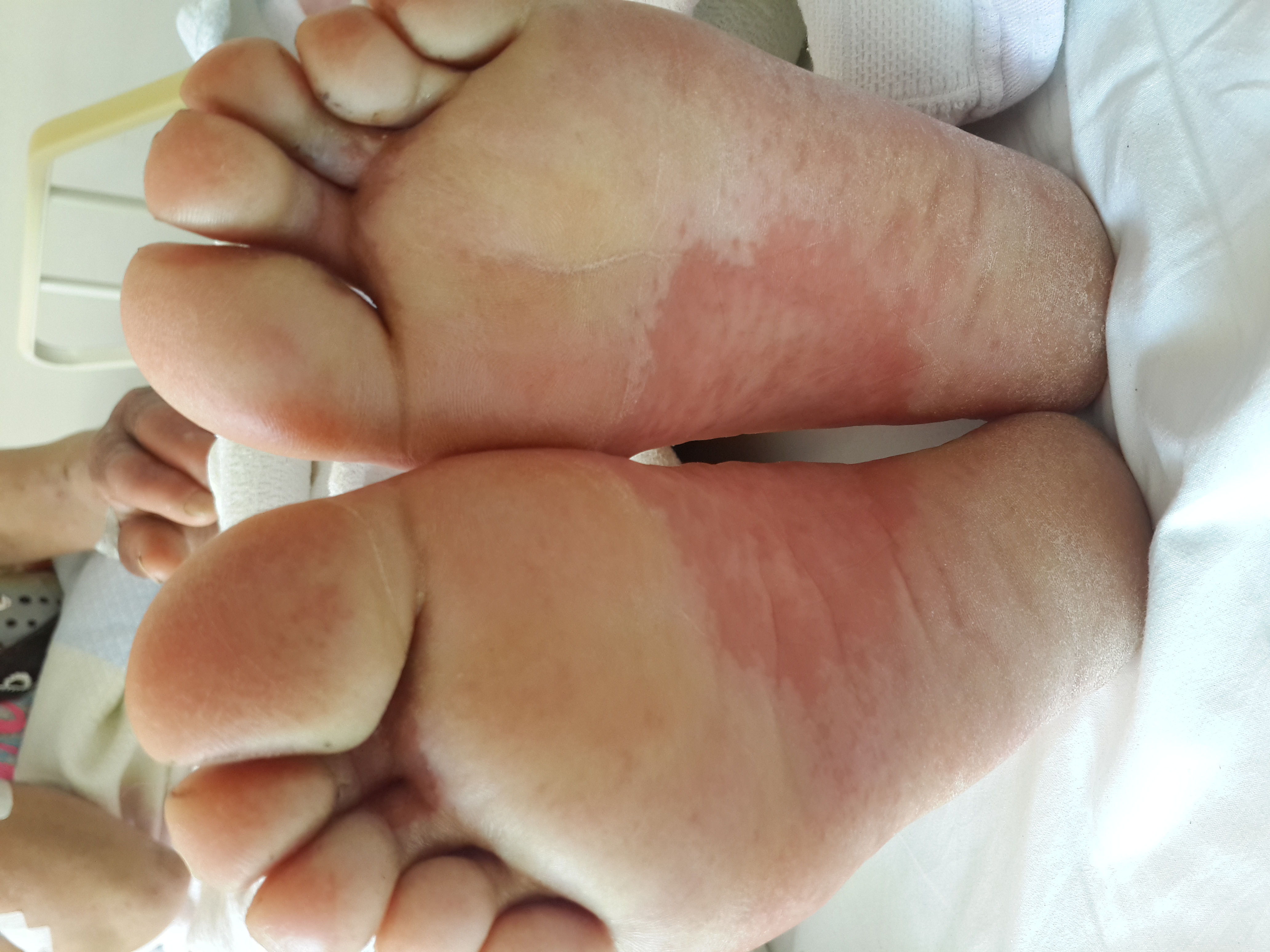
Figure 3. Target lesions on toes.
Biochemistry tests of the serum revealed normal serum electrolytes, serum transaminases and blood urea and creatinine levels. Anemia and leukopenia were prominent in hemogram assay. Erythrocyte sedimentation rate (ESR) and C - reactive protein levels were elevated. After consultation to a Dermatologist, skin biopsy performed and methyl prednisolone 40mg at once. Intravenous antihistamine (Pheniramine 45,5 mg, daily) treatment along with bicarbonate solution for oral mucosa started daily. Pathological evaluation confirmed the diagnosis of Erythema Multiforme.
Since ESR and C-reactive protein levels were elevated, cultures of blood, urine and sputum studied. An empiric amoxicillin/clavulanate1gr twice a day therapy ordered. Intravenous hydration performed after she could drink and eat more effectively per oral. After her general condition and oral and skin lesions improved on 10th day, medications discontinued, and she discharged without event. She has been advised for a control visit within 2 weeks. She was well on control visit, too.
Discussion
Erythema multiforme major is a hypersensitivity reaction with acute onset characterized with symmetric erythematous skin lesions 1. Etiology includes infections and several drugs, however, may be unclear in some cases[2-3]. The etiological cause could not have detected in present case, either.
Target lesions of Erythema Multiforme consisted of three parts; erythematous outer zone, light colored middle zone, vesicular or necrotic central lesion. Large target lesion plaques are formed 72 hours after development of initial small red papules[4]. These lesions show merger tendency and located predominantly on the skin, oral mucosa and around lips. Skin lesions are distributed symmetrically to the extremities. Dorsal and palmar faces of the hand and soles are usually affected [6]. The lesions of present case were in oral mucosa, around the mouth, and on upper and lower extremities. There were also target lesions on the dorsal faces of hands and toes.
Erythema Multiforme Major could be associated with anemia, lymphopenia, leukocytosis, elevated ESR and impaired kidney functions[2]. C-reactive protein and ESR were elevated and anemia and leukopenia were prominent in present case.
ErythemaMultiforme Major resolves spontaneously in about 1-2 weeks. Symptomatic treatment is recommended[5]. In addition to local corticosteroid pomades and antihistamine treatment, intravenous fluid replacement should be considered in patients with deteriorated oral intake due to oral involvement[6]. Topical or systemic antibiotic therapy may be applied for possible secondary infection. Our patient was given symptomatic treatment along with empiric antibiotics.
In conclusion, Erythema Multiforme Major is a toxic hypersensitivity reaction with a rapid course. Symptomatic treatment is usually adequate in management of the lesions of the disease.
References
- 1.Barron SJ, Del Vecchio MT, Aronoff SC (2015) Intravenous immunoglobulin in the treatment of Stevens–Johnson syndrome and toxic epidermal necrolysis: a meta?analysis with meta?regression of observational studies. International journal of dermatology54:108-115.[Crossref]
- 2.Roujeau JC, Stern RS (1994) Severe adverse cutaneous reactions to drugs. New England Journal of Medicine331:1272-1285.[Crossref]
- 3.Roujeau J-C, Kelly JP, Naldi L (1995) Medication use and the risk of Stevens–Johnson syndrome or toxic epidermal necrolysis. New England Journal of Medicine333:1600-1608.[Crossref]
- 4.Farthing PM, Speight PM (2006) Problems and pitfalls in oral mucosal pathology. Current Diagnostic Pathology12:66-74.
- 5.Marinho LHM, Haj M, Pereira LFM (1999) Lip adhesion: An unusual complication of erythema multiforme. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology88:167-169.
- 6.Carder KR (2005) Hypersensitivity reactions in neonates and infants. Dermatologic therapy18:160-175.[Crossref]



