Virchow-Robin spaces (VRs) are perivascular spaces that surround small arteries as they enter the brain parenchyma. Rarely, VRs look strikingly enlarged, “tumefactive”, having an unusual cystic configuration and causing mass effect. Here we report incidental revealed isolated “tumefactive” VRs developed unilaterally in the left Basal Ganglia (BG).
A 86-year-old man underwent brain MRI to evaluate a mild cognitive impairment. MRI revealed a multi-cystic non-enhancing lesion developed in the entire left caudate nucleus (CN) and lenticular nucleus (LN) and causing a slight mass effect on the frontal horn of the lateral ventricle and on the insula. All the cysts were rounded and had 2-3mm of diameter. The cysts-contents were iso- intense to CSF on T1 and T2/FLAIR sequences (Figure 1a-1d). On these sequences, because of mass effect, the internal capsule could not be identified. High Resolution (HR) 3D-T1 images demonstrated that the internal capsule was preserved (Figure 1e) but did not reveal more VRs. The lesion had no restriction diffusion.
There was not abnormal signal intensity in the neighboring white matter and no dilated VRs were detected in the remaining brain. T2/FLAIR sequences revealed an extensive leucopathy and T2-GRE showed multiple bilateral cortical microbleeds but no hemorrhage in the BG (Figure 1f and 1g). The diagnosis of cerebral amyloid angiopathy (CAA) finally retained.
Furthermore, Brain-CT did not reveal calcifications (Figure 1h). These findings remained stable on 2-years CT and MRI follow-up.
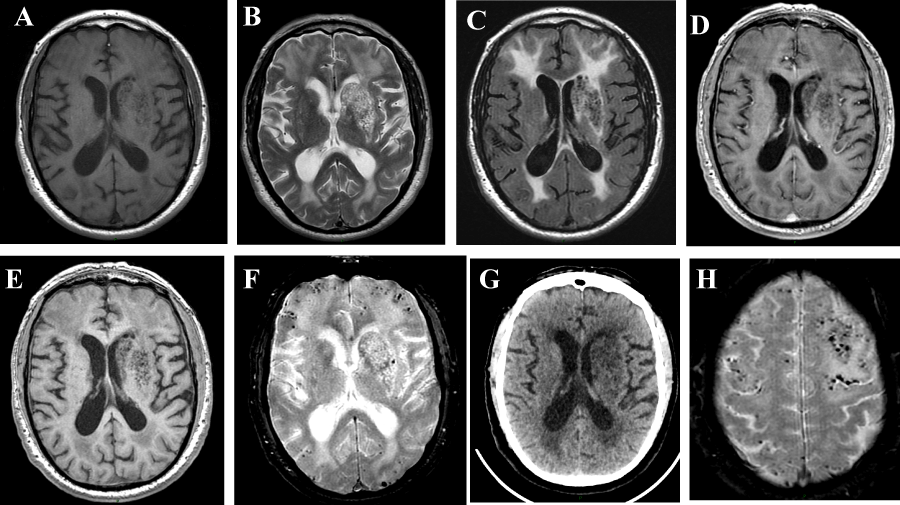
Figure 1. Brain MRI and CT in a 86-year-old man with mild cognitive impairment MRI: T1 (a), FLAIR (b) and T2SE (c) sequences show a cluster of CSF-like cysts developed in the left Basal Ganglia: caudate nucleus and lenticular nucleus, predominantly in the putamen. FLAIR/T2 images demonstrate extensive leucopathy. The cysts do not enhance after gadolinium injection (d). High Resolution (HR) 3D T1 image better defines the limits, showing that the internal capsule is free of cysts (e).
GRE-T2 sequence reveals multiple cortical microbleeds in the fronto- -temporo- parieto – occipital region (f-g). Non-contrast Brain-CT does not reveal calcifications (h).
VRs are usually normal findings on MRI of healthy people, but are more frequently found in older patients.
They are classified into 3 types; type 1occurs in the BG, along the lenticulo-striate arteries, type 2 are in the CSO and type 3 is in the midbrain.
Dilated or “Enlarged” VRs have 1 – 5mm in diameter and are associated with cardiovascular risks factors, dementia, hypertension, atherosclerosis, small-vessel disease and CAA [1-3]. They typically occur in two locations: the BG, along with the lenticulo-striate arteries, and in the white matter (WM) of the centrum semi-ovale (CSO). VRs in the BG are usually associated with WM VRs.
Rarely, VRs are markedly enlarged. They may cause mass effect and can become symptomatic, even after several years [4]. These “giant” VRs are usually localized in the mesencephalo-thalamic region, but have also been reported in the CSO, dendate nucleus, corpus callosum and cingulate gyrus [5].
Rarely, as in the present case, they can occur at an atypical location. Only 1 case of bilateral giant VRs of the BG has been previously reported, manifesting as chorea [6].
These abnormal VRs usually contain cysts of various shape and size [7-10]. If in our case, the numerous foci fulfilled the criteria of VRs, another unusual feature is the presence of a cluster of VRs of the same size (2-3mm of diameter) and shape, and causing mass effect. Furthermore the reported case underlines the interest to evaluate dilated VRs using HR 3DT1 imaging.
When enlarged or giant VRs exhibit bizarre configuration by their pattern of distribution they may be misdiagnosed as other pathologic processes, such as a cystic neoplasm. However, cystic brain tumors have cyst-contents that usually are not iso-intense to CSF and often have solid components which may enhance after contrast, and are surrounded by edema.
In the current case, enlarged, tumefactive VRs, although in an usual location and with unilateral development, had a bizarre configuration and furthermore produced mass effect.
The presence of multiple cysts, a typical location along the path of a penetrating vessel, CSF-like signal of the cysts, no signal changes in adjacent brain tissue and the lack of calcifications and contrast-enhancement are important criteria to establish an accurate diagnosis and to avoid unnecessary invasive diagnosis.
The authors have no conflict of interest and have not any source of support.
- Patankar TF, Mitra D, Varma A, Snowden J, Neary D, et al. (2005) Dilatation of the Virchow-Robin space is a sensitive indicator of cerebral microvascular disease: Study in elderly patients with dementia. AJNR Am J Neuroradiol 26: 1512-1520. [Crossref]
- Groeschel S, Chong WK, Surtees R, Surtees R, Hanefeld F (2006) Virchow-Robin spaces on magnetic resonance images: normative data, their dilatation, and a review of the literature. Neuroradiology 48: 745-754. [Crossref]
- Charidimou A, Jaunmuktane Z, Baron JC, Burnell M, Varlet P, et al. (2014) White matter perivascular spaces: An MRI marker in pathology-proven cerebral amyloid angiopathy? Neurology 82: 57-62. [Crossref]
- Fujimoto K, Kuroda J, Hide T, Hasegawa Y, Yano S, et al. (2012) Giant tumefactive perivascular spaces that expanded and became symptomatic 14 years after initial surgery. Surg Neurol Int 3: 127. [Crossref]
2021 Copyright OAT. All rights reserv
- Salzman KL, Osborn AG, House P, Jinkins JR, Ditchfield A, et al. (2005) Giant tumefactive perivascular spaces. AJNR Am J Neuroradiol 26: 298-305. [Crossref]
- Zacharia TT (2011) Giant tumefactive perivascular spaces manifesting as chorea bilaterally. J Neuroimaging 21: 205-207. [Crossref]
- Shiratori K, Mrowka M, Toussaint A, Spalke G, Bien S (2002) Extreme, unilateral widening of Virchow-Robin spaces: Case report. Neuroradiology 44: 990-992.
- Rohlfs J, Riegel T, Khalil M, Iwinska-Zelder J, Mennel HD, et al. (2005) Enlarged perivascular spaces mimicking multicystic brain tumors. Report of two cases and review of the literature. J Neurosurg 102: 1142-1146. [Crossref]
- Mölzer G, Robinson S (2014) Case 202: Extensive unilateral widening of Virchow-Robin spaces. Radiology 270: 623-626. [Crossref]
- Kumar A, Gupta R, Garg A, Sharma BS (2015) Giant mesencephalic dilated virchow robin spaces causing obstructive hydrocephalus treated by endoscopic third ventriculostomy. World Neurosurg 84: 2074.e11-4. [Crossref]

