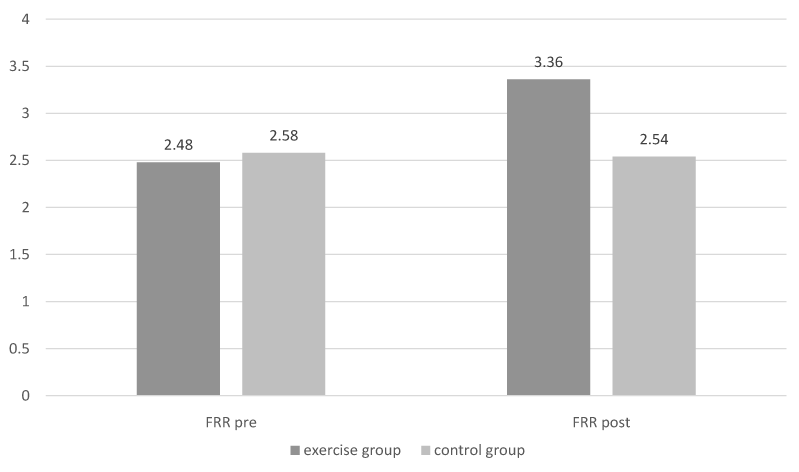Abstract
Purpose: The aim of the current study was to investigate the differences of erector spinae EMG activity measurements on patients presenting NSLBP, after the implementation of a 3-week trunk stabilization exercise program.
Methodology: Fifty AKMI Metropolitan College (AMC) students with NSLB were recruited and were randomly assigned to either an exercise group or a control group. Information regarding LBP prevalence were obtained by using the Nordic Questionnaire. The participants in the exercise group performed a trunk stabilization program consisting of 6 low load activation exercises, for a duration of 3 weeks and with a frequency of 5 times per week. Electromyographic (EMG) activity of erector spinae was recorded bilaterally, using surface EMG, during four different phases in the beginning of the study and 3 weeks later.
Results: Significant differences were revealed on the EMG activity for the exercise group’s pre and post measurements as well as exercise post and control post in the full trunk flexion position (p< 0.0001). Similarly, significant differences for the exercise group pre and post measurements in FRR (p< 0.0001) were observed.
Conclusions: The findings of the current study indicate that a 3 week stabilization exercise can facilitate the reduction of full flexion position and the improvement of FRP by amending erector spinae muscular alterations in patients with NSLBP.
Key words
electromyography, erector spinae, low back pain, exercise
Introduction
Low Back Pain (LBP) is considered a common disabling condition, which is increasingly confronted in Western societies, and is related to work absence, and consequently, loss of productivity [1]. For the majority of LBP cases, a precise diagnosis is not feasible, yet are classified as ‘non-specific low back pain’ [2]. Non-specific low back pain (NSLBP) is defined in the literature as pain localized in the lumbar region, which is not attributed to a specific underlying cause or pathology [3]. It is documented that NSLBP presents a lifetime prevalence of approximately 80% [3]. In spite of intensive research, the accurate causes of LBP are still unclear, whereas the recurrence rates of LBP patients who have received treatment reach approximately 70% [4]. Unfortunately, the exact reasons liable for the recurrence of symptoms are not known, and results are inconclusive [1].
It is postulated that alterations in recruitment patterns, and consequently postural control impairments of trunk muscles, constitute a plausible contributor concerning the persistence of symptoms and the recurrence of LBP [5-7]. Biomechanical studies have documented the association of paravertebral muscles with the generation of spinal stabilization, as well as postural control, whereas erector spinae in particular is described as a critical muscle group, which facilitates spinal function [8]. It has been advocated that significant differences, concerning muscle activation, exist between LBP patients and asymptomatic participants in static [9] dynamic [10] and isometric tasks [11] when conducting EMG measurements in the lumbar musculature.
Furthermore, additional differences between sides are evident in patients presenting LBP [10,12]. More specifically, the main finding of the relevant studies is the existence of an increased activity pattern of erector spinae muscle, which is explained by LBP patients’ necessity for additional spine stabilization and overall postural control [13]. The particular requirement is a consequence of the alterations in trunk muscles’ force, and, ultimately, the inability to correct perturbing forces [10]. The theory which predominates and has been proposed in the literature regarding the formation of this compensatory activity pattern, is attributed to motor disorganization, preceded by a previous low back pain incident [14,15].
It has been found that motor retraining can facilitate the reversibility of the adaptive changes in the motor cortex by amending muscular alterations [16]. Evidence from current research indicates that exercise provides beneficial effects for patients with sub-acute or chronic NSLBP [17]. Moreover, it has been indicated that exercises targeting restoring trunk muscles’ coordination can lead to the reduction of pain and disability in patients presenting NSLBP [18].
Additionally, the study of Tsao et al. [6] advocates that motor training of the paraspinal muscles leads to an increase of deep trunk muscles’ contribution in functional tasks for patients with unilateral NSLBP. Nevertheless, the study presented a small sample size, and the outcomes were based on a single session of exercise.
What remains currently questionable is whether repeated sessions of a stabilization exercise program can facilitate changes in EMG activity patterns of erector spinae muscle in patients with NSLBP. Therefore, the purpose of the present study is to investigate the effects of a three week stabilization exercise program, aiming on the restoration of trunk muscles’ coordination, on the EMG pattern of erector spinae in NSLBP patients.
Methodology
Participants
A total number of 65 AKMI Metropolitan College (AMC) students were recruited for the trial from November to December 2015. The individuals participated voluntarily in the study, and were contacted through a moderator email sent from the research team. All participants were informed about the purpose, the risk and the procedure of the research. Prior to the initiation of the study, each participant signed a consent form; however 15 students were excluded, since they met the exclusion criteria. The study was approved by The University Ethics Panel of AMC and completed in accordance with the Declaration of Helsinki for studies involving human subjects.
Data concerning low back pain prevalence as well as functional impairment was gathered by using the Nordic Low Back Pain Questionnaire [19], which has been recognized by previous studies for its validity [20]. Eligibility criteria included the presentation of a low back pain incident during the last 12 months, an age range of 20-35 years, absence of functional impairment and BMI normal values (18.5-24.9). Exclusion criteria included pregnancy, a history of back surgery, signs of underlying nerve root pain or serious spinal pathology (i.e., numbness/paraesthesia, pain radiating below the knee etc.), low back pain in the last 7 days prior to the assessment, neurologic deficits, malignancy, diabetes, symptoms of vertigo, excessive scoliosis or structural deformity and current pain in the hip, knee or ankle joint.
The 50 participants (23 males, 27 females) who met the inclusion criteria were then randomly allocated either to an exercise group (15 male, 10 female) or a control group (8 males, 17 females) (Figure 1). Both groups consisted of non - specific low back pain (NSLBP) patients who were asymptomatic (i.e., pain free) prior to assessment. The randomization of the patients was conducted with the use of opaque sealed envelopes. The researchers who were involved in the exercise group or the outcome assessments had no access to the above mentioned procedure, and the main assessors were blinded to group allocation.
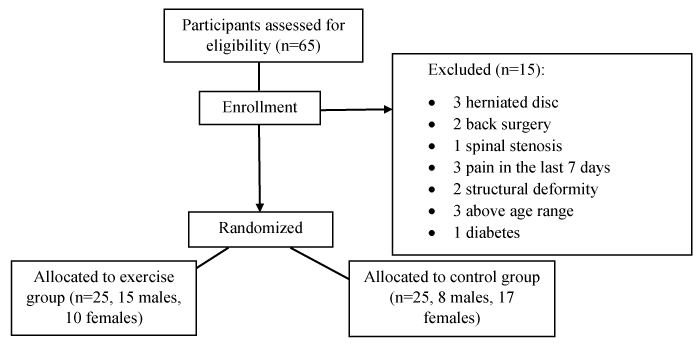
Figure 1. Flow chart of subject screening and allocation
Instrumentation
A two channel portable MyoTrac Infiniti EMG device (Thought Technology TTL T9855, Canada) was utilized to record the muscle activity of erector spinae muscle. After cleaning the skin with alcohol, two pre-gelled disposable pairs of 26 mm diameter silver silver – chloride (Ag/AgCl) surface electrodes (PG10C, FIAB SpA, Vicchio Firenze, Italy) were applied on both erector spinae muscles at L3-L4 spinal level (approximately 2,5-3 cm lateral to spine and at 3 cm of electrode center to center distance). The electrodes were applied parallel to the erector spinae muscles in a bipolar configuration. One reference electrode for each pair was applied on the anterior superior iliac spines (ASIS) as advised in a previous report [21]. The preamplifiers’ sensitivity of EMG was 1 μV and the bandwidth was 20-500 Hz. The device recorded the raw EMG signals, converted them into digital, and then presented absolute values. Data were exported to a Laptop (Acer), stored and later analyzed with the BioGraph Infiniti Software (Thought Technology TTL T9855, Canada).
EMG Protocol
The subjects were informed about the testing procedure and their right to withdraw from the trial at any time. The testing procedure was conducted in the AKMI Metropolitan College Laboratory with a constant temperature of 21°C. The specific testing protocol was adopted from previous relevant studies [21,22]. The participants were required to remove their clothing down to the underwear and, raise their t-shirts in order for the testing region to be exposed. After the application of the electrodes in the lumbar region, the main assessors explained briefly the procedure and demonstrated the positions, which the subjects had to assume.
The initial positioning, required the subjects to stand upright with their hips and knees stabilized in an extended position. Their feet were placed shoulder width apart and the position was marked in order to ensure consistency between trials. Furthermore, in order to limit the probability of an aftereffect caused by altered head positioning, subjects were requested to keep their eyesight fixed on a mark. Prior to the testing procedure each subject was advised to assume the positions of the testing protocol so as to guarantee the completion of the task within time epoch. When correct positioning was ensured, the following four positions were analysed by SEMG. The four positions included the standing position, bending as far forward as possible, the full flexed position, and return to standing. All positions were maintained for two seconds.
During the second phase, namely the stooping position, the patients were asked to tuck their chin to their chest in order to avoid the influence that head alterations have been documented to have during EMG measurements [22]. For every participant, data from three trials were gathered, and an average measurement of the three was recorded. In order to ensure the avoidance of EMG amplification differences, variables such as weight, height and BMI of participants were considered and data were normalized as has been stated in relevant studies [22]. Electromyographic signals from both sides of the lumbar region were averaged, and results from each participant were imprinted into the four phases of the testing task.
As it has been proposed in Wallborn et al.’s research [22], the flexion relaxation response was calculated by dividing the maximum EMG value for one second in flexion position by the maximum EMG value in full flexion position.
Exercise protocol
The exercise protocol was especially designed for the current study by synthesizing stabilization exercises, which have been previously described and investigated for their effectiveness [23-25]. The first session was performed on an individual basis with the supervision of a researcher, whereas the anatomy and the importance of these muscles for spinal function were explained to the patients. The next sessions were performed at home with no equipment required. All participants in the exercise group received an instructional booklet, for the correct implementation of the program, as well as a self-report exercise diary in order to monitor their adherence.
Briefly, the protocol included low load activation exercises, targeting the trunk stabilizers, in low load positions (i.e., supine position, 4-point kneeling). More specifically the exercises consisted of the drawing manoeuvre, the birddog, the deadbug, the one leg supine bridging, the camel arch and dorsal raises. Every exercise was performed for three sets of 10 repetitions with 10 seconds hold whereas the resting time was 10 seconds between sets. The frequency of the program was set at five times per week, the duration was three weeks, and every session lasted approximately 45 minutes. Based on a previous study [24] the compliance was defined by the 80% of sessions (12 sessions) for every individual.
Statistical analysis
For the assessment of intra- rater reliability of the tests, 6 participants (3 from exercise group, 3 from control group) were selected. Pearson’s correlations were used for EMG data, and descriptive characteristics for the characterization of the sample. Normality of distribution for each variable was analysed using the Shapiro – Wilk method. Multivariate analysis of variance (MANOVA) was carried out in order to evaluate and compare the EMG values for the 4 phases of the task, as well as the demographic characteristics of both groups. One –way ANOVA was used to compare the flexion relaxation ratio (FRR). The alpha significance value for the statistical tests was set at 0.05. The statistical analysis was conducted by utilizing the SPSS statistical software version 22.0 (IBM Corp., Armonk, NY, USA).
Results
Participants
From the 50 participants who fulfilled the inclusion criteria, seven withdrew from the study. More specifically, four subjects who were initially assigned to the exercise group, were not compliant with the exercise program, whereas contact with three participants who were assigned in the control group was not attainable. Therefore, data were statistically analysed for 43 participants (21 exercise group, 22 control group).
Intra-rater reliability of EMG data
The reliability coefficients (r) deriving from the between measurements correlations, presented a good level of reliability since they ranged from 0.7 to 0.8 and significance p values were documented to be 0.05.
Analysis of anthropometric characteristics
MANOVA (2 × 4) was conducted in order to identify possible significant differences on the anthropometric characteristics such as age, weight, height and body mass index (BMI) between the two groups. The statistical analysis presented that there were no significant differences in the aforementioned characteristics (p>0.05). Therefore, the process of controlling the amplification of the EMG, as described above, was redundant (Table 1).
Variables |
Exercise Group
M ± SD |
Control Group
M ± SD |
Age (years) |
24,67 ± 5,02 |
23,50 ± 4.29 |
Weight (kg) |
71,48 ± 13.47 |
66,0 ± 12.59 |
Height (cm) |
176,52 ± 10.51 |
172,0 ± 8.79 |
BMI (kg/m2) |
22,73 ± 2.14 |
21,93 ± 2.22 |
Table 1. Anthropometric characteristics of subjects
EMG group differences: Standing, flexion, full flexion and extension
The statistical analysis conducted with MANOVA (2 × 4), revealed that there were no significant differences on the combined dependent variable of EMG activity measurements, between the two groups (p<0,0001). Analysis of variables utilizing Bonferroni for the multiple comparisons detected that the two groups did not differ during standing (p>0.05), flexion (p>0,05) and extension (p>0,05) positions, either in the pre or post measurements. However, a significant difference was observed between the exercise pre and post measurements characterized by a reduction in the full flexion position (p<0.0001) and, between the exercise post and the control post measurements, with the mean values of the exercise group being lower than those of control in the full flexion (p<0.001). Figure 2 is a graphic representation of EMG activity measurements of erector spinae for each group, during the four phases of the task that was tested (Table 2).
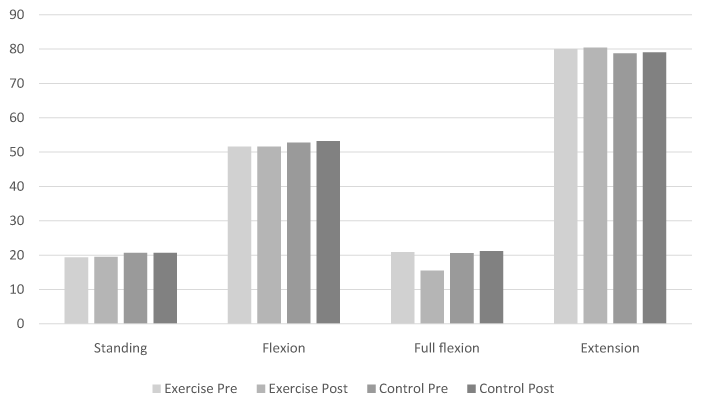
Figure 2. Graphic representation of EMG activity measurements of erector spinae during standing, flexion, full flexion and extension for each group (pre – post).
Variables |
Exercise Group Pre (μV ± SD) |
Control Group Pre (μV ± SD) |
Exercise Group Post (μV ± SD) |
Control Group Post (μV ± SD) |
Standing |
19,33 ± 1.83 |
20,71 ± 1,97 |
19,49 ± 1.35 |
20,70 ± 1.70 |
Flexion |
51,60 ± 3.5 |
52,75 ± 8.13 |
51,60 ± 3.26 |
53,22 ± 8.41 |
Full flexion |
20,87 ± 1.71 |
20,57 ± 3.05 |
15,52 ± 1.19 |
21,19 ± 3.32 |
Extension |
80,05 ± 2.68 |
78,77 ± 9.09 |
80,42 ± 1.83 |
79,02 ± 8.05 |
Table 2. EMG activity measurements of erector spinae during the phases of standing, flexion, full flexion and extension for both groups (pre and post).
EMG group differences: Flexion relaxation ratio (FRR)
The One-way ANOVA revealed that there were significant differences for the flexion relaxation ratio (FRR) between groups for pre and post measurements (p<0.0001). Multiple comparison of the variables by employing Bonferroni post hoc test, exhibited that the mean FRR for exercise pre measurements was significantly lower than the relevant mean of exercise post measurements (p<0.0001). Furthermore, the mean FRR measurements of the exercise group in comparison to the control group post measures was documented to be significantly higher. (p<0.0001). Figure 3 is a graphic representation of FRR measurements for the erector spinae for each group (Table 3).
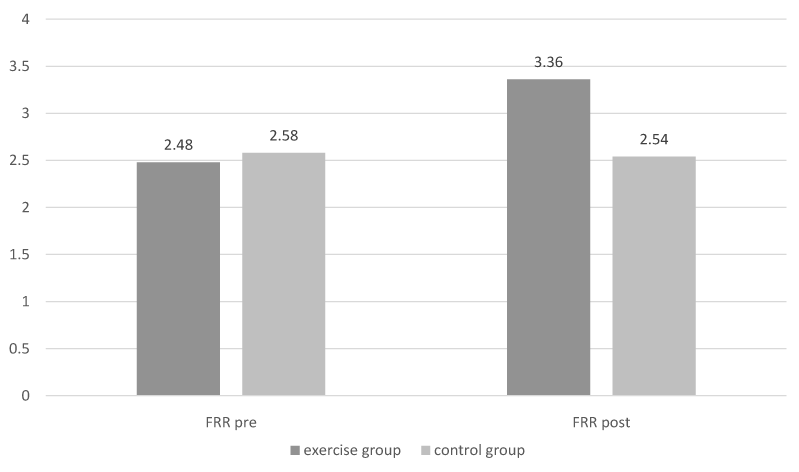
Figure 3. Graphic representation of Flexion relaxation ratio (FRR) differences between groups (pre – post).
Variables |
Exercise Group Pre (M ± SD) |
Control Group Pre (M± SD) |
Exercise Group Post (M ± SD) |
Control Group Post (M ± SD) |
FRR |
2,48 ± 0.18 |
2,58 ± 0.38 |
3,36 ± 0.12 |
2,54 ± 0.45 |
Table 3. FRR measurements for both groups, pre and post
Discussion
Methodological issues
A prerequisite prior to discussing the findings of the current study, is to address the existence of some methodological issues. The present investigation recruited a convenience sample which consisted of AMC students eligible for participation. The demographic characteristics of the participants had significantly lower mean compared to other relevant studies investigating EMG activity of the lumbar musculature. Furthermore, the participants recruited were asymptomatic and without functional impairments. Consequently, the comparability with patients presenting chronic low back pain and functional impairments is rendered difficult.
Low back pain prevalence was acquired by utilizing the Nordic LBP questionnaire, which does not include variables such as pain intensity and duration of symptoms in its assessment. Thus, there is a possibility to produce different results concerning LBP prevalence. Exclusion of specific spinal pathology was based on participant’s self- report, and by the investigator’s observation. (i.e., structural deformity). Moreover, the compliance of the exercise group participants was based on the self -report of the subjects, thus the reliability of the results cannot be fully ensured. No follow up measurements were conducted in order to investigate if the differences persisted.
EMG differences: Standing, flexion, full flexion, extension positions and flexion relaxation phenomenon (FRP)
The findings of the present study provide evidence regarding the positive effect of stabilization exercises targeting trunk muscles, during standing, flexion, full flexion and extension positions as well as FR response. The results revealed that there were no significant differences concerning standing, flexion and extension positions for both groups in either pre or post measurements. Nevertheless, research evidence investigating the differences on EMG activity of erector spinae in the above three positions has not been conducted. On the contrary, our results showed a significant difference in pre and post measurements for the full trunk flexion and FR response. Flexion relaxation response is considered a phenomenon, which refers to the muscular activity pattern of erector spinae during the trunk flexion [26]. It is indicated that during trunk flexion the passive elements of the spine present a tension. When this tension reaches a specific point, the central nervous system deactivates the erector spinae muscle [9]. In patients with LBP the flexion relaxation phenomenon is documented to be absent. Relevant research evidence has proposed that the altered activity pattern of erector spinae constitutes an adaptation of the neuromuscular system in order to provide spinal stability, since deep trunk muscles present delayed activation [6,26]. Overall, past injury, pain and neuromuscular changes concerning afferent receptors constitute the main factors leading to motor reorganization [14,15]. Therefore the results of the present study concerning the first measurements of EMG activity can be explained through these series of changes, since an absence of FRP, and an increased activity in full flexion position were observed in both groups.
Regarding the second measurements, which showed a significant improvement in terms of FRR and lower values in full trunk flexion for the exercise group, the results can be interpreted based on the effects that the stabilization exercise program had in those patients. It is postulated in relevant studies that stabilization exercises can facilitate the ability of achieving FRP by restoring motor control and coordination of the patients, and, thus, the altered activity patterns [16,18]. All the above outcomes of the study are in agreement with other researches which found that the implementation of an exercise program for a period of 12 weeks, led to a reduction in full flexion activity and improvement of FR response [21,27]. Additionally, another study concluded that after a period of 7 weeks performing stabilization exercises, the 94% of the patients were able to achieve the EMG silence of the erector spinae [26]. Nonetheless, the patients of the above studies recruited chronic low back pain patients (CLBP) as well as the exercise program duration was longer in comparison to the current investigation.
An additional contributing factor for the explanation of the absence of FRP is the muscular stiffness, and the reduction of hamstring flexibility, due to LBP [28]. It is indicated that hamstring stiffness results in heightened erector spinae muscle activity as a compensatory measure in order to control spinal instability [9]. Nevertheless, in the current study the hamstring flexibility was not assessed, it can be considered as a plausible explanation concerning erector spinae altered activation. Finally, although the present investigation revealed an improvement in FRR for the exercise group, future studies examining further the impact of exercise, is imperative.
Conclusion and clinical implications
The findings of the cu2021 Copyright OAT. All rights reserv trunk stabilization exercise program can have a positive impact on the improvement of FRR in NSLBP patients. No significant differences were observed between the two groups during standing, flexion and extension positions in pre or post measures. Nevertheless, full trunk flexion decreased significantly in the post measurements of the exercise group while FR response was improved. As there was no other research examining the effects of exercise in EMG activity measurements for NSLBP patients after the implementation of an exercise program; therefore the clinical implication of the study is that a stabilization exercise program implemented for at least a period of 3 weeks can reverse motor reorganization, and ultimately change the heightened activity patterns of erector spinae in NSLBP patients. Future research should examine the effects of a longer duration exercise program, and the persistence of exercise effects in a long term.
References
- MacDonald D, Moseley GL, Hodges PW (2009) Why do some patients keep hurting their back? Evidence of ongoing back muscle dysfunction during remission from recurrent back pain. Pain 142: 183-188. [Crossref]
- O'Sullivan P (2005) Diagnosis and classification of chronic low back pain disorders: maladaptive movement and motor control impairments as underlying mechanism. Man Ther 10: 242-255. [Crossref]
- Smith BE, Littlewood C, May S (2014) An update of stabilisation exercises for low back pain: a systematic review with meta-analysis. BMC Musculoskelet Disord 15: 416. [Crossref]
- van Dieën JH, Selen LP, Cholewicki J (2003) Trunk muscle activation in low-back pain patients, an analysis of the literature. J Electromyogr Kinesiol 13: 333-351. [Crossref]
- Panjabi MM (2003) Clinical spinal instability and low back pain. J Electromyogr Kinesiol 13: 371-379. [Crossref]
- Tsao H, Druitt TR, Schollum TM, Hodges PW (2010) Motor Training of the Lumbar Paraspinal Muscles Induces Immediate Changes in Motor Coordination in Patients With Recurrent Low Back Pain. J Pain 11: 1120-1128. [Crossref]
- Massé-Alarie H, Flamand VH, Moffet H, Schneider C (2013) Peripheral Neurostimulation and Specific Motor Training of Deep Abdominal Muscles Improve Posturomotor Control in Chronic Low Back Pain. Clin J Pain 29: 814-823. [Crossref]
- Hashemirad F, Talebian S, Hatef B, Kahlaee AH (2008) The relationship between flexibility and EMG activity pattern of the erector spinae muscles during trunk flexion-extension. J Electromyogr Kinesiol 19: 746-753. [Crossref]
- Dankaerts W, O'Sullivan P, Burnett A, Straker L (2006) Altered patterns of superficial trunk muscles activation during sitting in nonspecific chronic low back pain patients: importance of subclassification. Spine 31: 2017-2023. [Crossref]
- Mazis N (2014) Does a History of Non Specific Low Back Pain Influence Electromyographic Activity of the Erector Spinae Muscle Group During Functional Movements? Journal of Novel Physiotherapies 4: 1-11.
- Sung PS, Lammers AR, Danial P (2009) Different parts of erector spinae muscle fatigability in subjects with and without low back pain. Spine J 9: 115-120. [Crossref]
- Kim MH, Yoo WG, Choi BR (2013) Differences between two subgroups of low back pain patients in lumbopelvic rotation and symmetry in the erector spinae and hamstring muscles during trunk flexion when standing. J Electromyogr Kinesiol 23: 387-393. [Crossref]
- Hodges PW (2001) Changes in motor planning and feedforward postural responses of the trunk muscles in low back pain. Exp Brain Res 141: 261 – 266. [Crossref]
- Tsao H, Galea MP, Hodges PW (2008) Reorganization of the motor cortex is associated with postural control deficits in recurrent low back pain. Brain 131: 2161-2171. [Crossref]
- Tsao H, Hodges PW (2008) Persistence of improvements in postural strategies following motor control training in people with recurrent low back pain. J Electromyogr Kinesiol 18: 559-567. [Crossref]
- Hodges PW, Moseley GL (2003) Pain and motor control of the lumbopelvic region: effect and possible mechanisms. J Electromyogr Kinesiol 13: 361-370. [Crossref]
- Hayden JA, van Tulder MW, Malmivaara AV, Koes BW (2005) Meta-analysis: exercise therapy for nonspecific low back pain. Ann Intern Med 142: 765-775. [Crossref]
- Macedo LG, Maher CG, Latimer J, McAuley JH (2009) Motor control exercise for persistent, nonspecific low back pain: a systematic review. Phys Ther 89: 9-25. [Crossref]
- Kuorinka I, Jonsson B, Kilbom A, Vinterberg H, Biering-Sørensen F, et al. (1987) Standarized Nordic questionnaires for the analysis of musculoskeletal symptoms. Appl Ergon 18: 233-237. [Crossref]
- Mitchell T, O'Sullivan PB, Burnett AF, Straker L, Rudd C (2008) Low back pain characteristics from undergraduate student to working nurse in Australia: a cross-sectional survey. Int J Nurs Stud 45: 1636-1644. [Crossref]
- Marshall P, Murphy B (2006) Changes in the flexion relaxation response following an exercise intervention. Spine (Phila Pa 1976) 31: E877-883. [Crossref]
- Wallbom AS, Geisser ME, Koch J, Haig AJ, Guido C, et al. (2009) Lumbar flexion and dynamic EMG among persons with single level disk herniation pre- and postsurgery with radicular low-back pain. Am J Phys Med Rehabil 88: 302-307. [Crossref]
- Koumantakis GA, Watson PJ, Oldham JA (2005) Trunk muscle stabilization training plus general exercise versus general exercise only: randomized controlled trial of patients with recurrent low back pain. Phys Ther 85: 209-225. [Crossref]
- Hebert JJ, Fritz JM, Thackeray A, Koppenhaver SL, Teyhen D (2015) Early multimodal rehabilitation following lumbar disc surgery: a randomized clinical trial comparing the effects of two exercise programmes on clinical outcome and lumbar multifidus muscle function. Br J Sports Med 49: 100 – 106. [Crossref]
- Kim S, Kim H, Chung J (2014) Effects of Spinal Stabilization Exercise on the Cross- Sectional Areas of the Lumbar Multifidus and Psoas Major Muscles, Pain Intensity, and Lumbar Muscle Strength of Patients with Degenerative Disc Disease. J Phys Ther Sci 26: 579-582. [Crossref]
- Neblett R, Mayer TG, Gatchel RJ, Keeley J, Proctor T, et al. (2003) Quantifying the lumbar flexion-relaxation phenomenon: theory, normative data, and clinical applications. Spine (Phila Pa 1976) 28: 1435-1446. [Crossref]
- Marshall PW, Murphy BA (2008) Muscle activation changes after exercise rehabilitation for chronic low back pain. Arch Phys Med Rehabil 89: 1305-1313. [Crossref]
- Halbertsma JP, Göeken LN, Hof AL, Groothoff JW, Eisma WH (2001) Extensibility and stiffness of the hamstrings in patients with nonspecific low back pain. Arch Phys Med Rehabil 82: 232-238. [Crossref]