Introduction
Schema therapy (ST) was originally developed in 1994 by Jeffrey Young to treat personality disorders (PD) and has been adapted for a number of psychiatric disorders [1,2]. ST is an integrative therapy, combining cognitive, behavioral, psychodynamics and experiential strategies [3]. Although the theory of this therapeutic approach has evolved significantly, the same is not true for investigations into its clinical effectiveness. This is partially due to difficulties inherent to the research process involving long-term psychotherapy treatments and populations with characterological symptoms.
Recent years have seen an increasing number of studies on the clinical effectiveness of ST for PD [4-9] and other pathologies [1,2], though research is still scarce considering the treatment’s popularity. These studies are necessary for the development and maturation of a therapeutic approach, since they identify critical areas that require additional investigation.
A systematic review of research on the clinical effectiveness of ST was recently conducted, analyzing studies published until January 2011[10]. The authors included only studies that investigated the clinical effectiveness of ST and involved more than 10 therapeutic sessions. This last factor is relevant because profound schematic changes are unlikely to occur in a short-term intervention. The total sample consisted of12 studies, indicating favorable results for the clinical effectiveness of this therapeutic approach.
Considering the importance of tracking the development of ST, this paper presents a systematic review of clinical effectiveness studies published from February 2011 to February 2015. Taking into account the rapid expansion of electronic publishing, a systematic review is important because it summarizes results. This methodology gathers published data in order to identify, select, summarize and evaluate evidence that is relevant to clinical issues [11]. The present study aims at identifying the clinical effectiveness of ST.
However, it is important to note that the recommendations stemming from a review depend on the quality of the studies analyzed [11]. Therefore, in addition to including only studies that met the inclusion criteria, this review aimed at qualifying the publications based on the Scottish Intercollegiate Guidelines Network – SIGN [12].
Method
We performed a systematic review of studies on the clinical effectiveness of Schema Therapy (ST). Papers published from February 2011 to February 2015 were identified using the following key words: “schema therapy” and “treatment and/or efficacy”. Inclusion criteria were: (a) studies that showed evidence of ST treatment, (b) published in English, Portuguese or Spanish, (c) any diagnosis, including co-morbidities, (d) individual or group treatment. We excluded: (a) studies with participants younger than 18 years old, (b) research involving treatment in fewer than 10 sessions, and (c) case studies with three participants or fewer. The articles included were then organized and analyzed according to the disorder investigated.
In addition to the aforementioned criteria, the level of evidence was also qualified in order to extend discussion to the methodological competence of each paper reviewed. Based on the systematic review mentioned before [10], scores were calculated according to a checklist from the Scottish Intercollegiate Guidelines Network – SIGN[1] [12].
Results
A total of 3,200 abstracts were identified, with 31 remaining after exclusion criteria were applied. Of these, only 9 addressed the treatment effectiveness of ST and met the inclusion criteria. One compared ST to cognitive-behavioral therapy (CBT) in the treatment of depression [13] and another investigated ST’s effectiveness in treating chronic depression patients [14]. The remaining seven articles evaluated ST in different samples of personality disorders [4,5,9,15-18].
A combined individual and group ST for the treatment of borderline personality disorder was investigated by some researches [5], whereas others evaluated the effects of ST on inpatients [16]. A study analyzed the effects of ST on a group of personality disorders (cluster C or B) [9], while another investigated its effects on elderly patients [18]. Van Vresswijk et al. examined the relationship between group ST and changes in symptoms, schemas and modes in a heterogeneous psychiatric sample (patients with long-term Axis I and/or personality disorders) [17]. Another authors compared the effectiveness of 50 ST sessions inclarification-oriented therapy and treatment as usual in a 323-patient sample exhibiting six types of personality disorder (avoidant, dependent, obsessive-compulsive, paranoid, histrionic, and narcissist) [4]. Finally, the effectiveness of ST for narcissist, antisocial, borderline or paranoid patients who had been forcibly institutionalized for committing crimes was examined [15]. Figure 1 shows the selection process for papers in the sample and table summarizes each study.
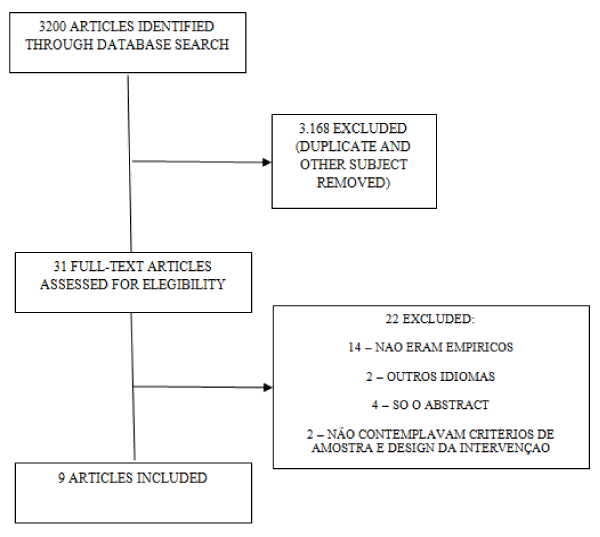
OBS: 14 – not empirical; 2 – other languages; 4 – only abstract available; 2 – did not include sample criteria and intervention design
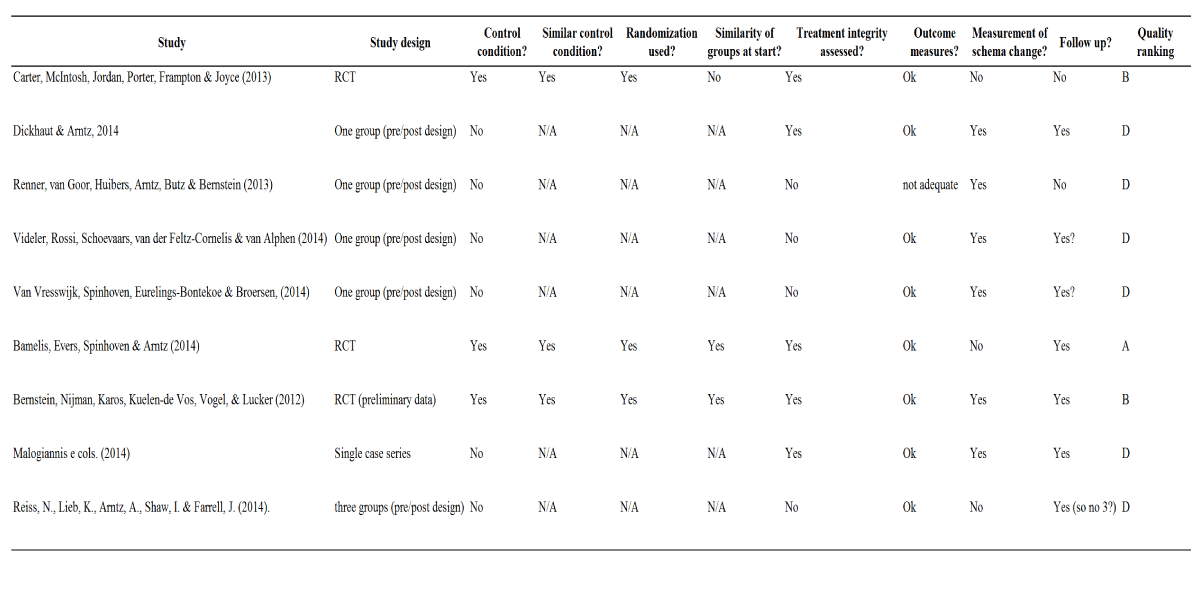
Discussion
Several considerations can be put forward regarding publications on ST. First, it is important to note the growing number of papers published in Europe, where ST has been the first choice treatment for PD patients in the last 15 years. In a review by Masley et al., of the 12 papers included in the sample, seven were European, specifically from the Netherlands and Norway [10]. The first authors of the other five studies were American (three) and Australian (two). In our review, only one study was from New Zealand, while eight were European, more specifically, from Dutch.
Although initial studies focused on personality disorders (especially borderline), over the last 5 years other clinical conditions have been investigated. Research has emerged on disorders not of personality, such as eating disorders, post-traumatic stress disorder, and depression, expanding the application of this approach and enriching the range of evidence-based treatments.
This review focuses initially on findings regarding the effectiveness of ST in treating depression disorder, followed by studies that evaluated its effectiveness for personality disorders.
Depression
Although the effectiveness of Cognitive Behavioral Therapy (CBT) for depression is well documented, in some cases the results obtained are not maintained over long periods [19]. This decline is relevant in the study of ST, since the characteristics of depressed patients may explain the failure to maintain therapeutic results over time.
The effectiveness of CBT were compared to ST in the treatment of depressive patients [13]. A sample of 100 patients diagnosed with depression was subjected to weekly CBT and ST sessions over six months, followed by monthly sessions for another six months. The results indicated that ST was neither superior nor inferior to CBT. Both treatment modalities achieved the same remission and recovery rates. Considering the intensive and comprehensive nature of the Schema Therapy approach, as well as its effectiveness in treating chronic problems, the authors expected to find lasting changes in the population treated with ST. However, recent studies have shown that ST must be applied over an extended period in order to be effective and achieve its treatment goals. It appears that six months of weekly therapy followed by an additional six months of monthly sessions does not meet the required treatment time. Indeed, when referring to chronic depression several authors have suggested more intensive treatment, reporting that effectiveness increases with the number of sessions [14-20]. Given that this study is the first randomized clinical trial to compare two treatments for depression [13], we suggest that future research include the structure and duration of treatment.
Malogiannis et al. analyzed the duration of therapy and its effectiveness in 12 chronically depressed patients. Treatment took place over 60 sessions, of which 55 were weekly and the last 5, twice-weekly [14]. Patients were assessed four times: baseline (8 weeks prior to intervention), introduction to ST and bond with therapist (session 12 to 16), during treatment, and six months later (follow-up). After treatment, five patients showed reduced symptoms. During the follow-up period only one relapsed, while two others who had initially only improved recovered fully.
The authors suggest that the inclusion of limited reparenting in a comforting setting in the introductory phase (different from the standard structure, in which this phase consists solely of appraisal) is related to the visible positive outcomes [14]. Another point emphasized was the temporary worsening of patients` symptoms during the intermediary phase, in which techniques for schematic changes were used, followed by positive outcomes. According to the authors, all patients with positive outcomes exhibited this pattern of deterioration followed by recovery during treatment.
During the follow-up, the authors found reduced schematic levels of impaired autonomy and/or performance, over vigilance or inhibition, disconnection/rejection, which may be associated with sustained results during these six months. Although hypothetical, this data strengthens the argument that long-term ST can achieve significant levels of cognition (schematic structures), thereby maintaining the clinical improvement obtained [14].
In general, both studies favored ST for depressive disorders. Despite the less robust design of the study by Malogiannis and colleagues [14], which lacks randomization, a control group and significant sample size, preliminary data suggest that ST is effective for chronic depression. In the other investigation, 68% of patients were diagnosed for chronic depression, also indicating the effectiveness ST for this type of disorder [13].
Personality disorders
Studies that evaluate the effectiveness of ST for personality disorders (PD) still focus on borderline personality disorder (BPD) and have confirmed its effectiveness for this population [6-8,21,22]. In the present paper, two of the articles reviewed investigated the use of ST for BPD. One was a pilot study in an outpatient setting and the other was conducted in a hospital; both included individual and group treatment.
The pilot study evaluated combined individual and group ST for BPD [5]. Two groups of patients with BPD were treated weekly over two years in individual and group sessions. Individual sessions were designed according to the Arntz and van Genderen (2009) (mentioned in [5]) protocol and aimed at supporting group sessions. Group therapy was based on the format designed by Farrell [23]. Symptoms, early maladaptive schemas (EMS) and schema modes were evaluated every six months for two and a half years. BPD manifestations decreased significantly and 77% of participants recovered after 30 months.
These results corroborate the effectiveness of ST in combined individual and group treatment and support the findings of Farrell and colleagues, who reported positive results in group therapy [6]. Nevertheless, the small sample size was a limitation and restricted confidence intervals. Therefore, future studies could examine the effectiveness of ST for group treatment, as well as combined individual and group treatment.
The other study investigated the effects of treatment during hospitalization for 92 BPD patients in three pilot studies, combining individual and group treatment [16]. Results showed that ST during hospitalization can reduce symptoms of severe BPD.
These and previous studies found favorable results for ST in the treatment of severe BPD [5-8,16,22]. Positive results were also found with severe borderline patients not suited to outpatient treatment. The authors found that treatment during hospitalization can offer benefits, although results should be viewed with caution since data are preliminary and the study exhibited methodological limitations [16].
Research on personality disorders other than BPD is still scarce and, when available, often evaluates more than one disorder, making it difficult to identify differences difficult due to sample size. In this review, five studies evaluated the effectiveness of ST in heterogeneous samples of personality disorders.
Videller et al. were the first to investigate the effects of ST on a group of elderly patients with chronic mood disorder or adjustment disorder comorbid with personality disorder or personality disorder traits [18]. The sample consisted of 31 patients aged 60 to 78 years, submitted to 18 weekly 90-minute ST sessions and two additional follow-up sessions. In the first phase (sessions 1 to 9), patients were educated about their three main dysfunctional schemas and modes, and in the second phase (sessions 10 to 20) they were encouraged to respond to situations that activated their schemas in a more adaptive manner. Comorbid disorders were: personality disorder not otherwise specified (6 patients), dependent PD (3 patients), paranoid PD (1 patient) and PD traits (12 patients). Data confirmed the effectiveness of group ST for elderly patients, both in reducing symptoms and changing early maladaptive schemas. Furthermore, changes in the severity of schema from the start to the middle of treatment predicted final symptom improvement.
Another study investigated the effect of group ST on a population of young adults with PD or PD traits [9]. Participants were 26 adults with a first diagnosis of cluster B or C, or PD traits alone. The group ST protocol used consisted of 18 structured weekly sessions, focusing on psychoeducation and cognitive techniques [24]. The results indicated a substantial decline in general stress symptoms from pre- to post-treatment. EMSs, schema modes and coping styles decreased; however, the decline in EMSs did not remain significant when stress symptoms were controlled. The finding of stable EMSs was also reported in previous studies, reinforcing the idea that long treatment periods are needed to achieve deeper change [14,20,21]. Nevertheless, data reveal preliminary evidence of group ST effectiveness in this population.
It is important to underscore the different age groups included in the above studies [9,18], since EMSs may differ in terms of flexibility and maturation according to age. Although both studies found the short-term group schema approach to be effective for populations with PD or PD traits, the effect size of the study by Renner et al. [9] was greater than the one observed on the other investigation [18]. The authors suggest that greater flexibility and potential for EMS changes in young adults could explain these findings.
Van Vresswijk et al. investigated the relationship between short-term group ST and changes in symptoms, schemas and modes, in a heterogeneous sample of patients with long-term axis I disorders and/or PD characteristics [17]. The short-term ST group underwent 18 weekly 90-minute sessions, followed by two follow-up sessions in the first and second months after treatment. Findings indicated that 46.8% of participants recovered from initial symptoms and 12% showed improvement. Thus, similarly to previous studies [9,18], short-term ST may be associated with a clinically significant improvement in a population with long-term axis I disorders and/or PD characteristics. The schematic domain “other-directedness" was a significant predictor of treatment success. The results also suggested co-occurrence of schema and symptom changes through a mutual reinforcement process.
Another investigation compared the effectiveness of 50 ST sessions with clarification-oriented psychotherapy and TAU in a sample of 323 patients with six types of personality disorders (avoidant, dependent, obsessive-compulsive, paranoid, histrionic, and narcissistic) [4]. A multicenter randomized controlled trial was conducted between 2006 and 2011 in 12 mental health institutions. With respect to therapists, one group was initially trained through lectures, while the other was given practical exercises. A significantly higher number of patients submitted to ST recovered compared to those who underwent other types of psychotherapy. During follow-up, these patients also exhibited fewer mood changes and better social and general functioning. Additionally, therapists trained using practical exercises achieved a better result when compared to those trained through lectures. The dropout rate was found to be lower in schema approaches only when compared to treatment–as-usual. It is important to note that findings remained the same for all types of personality diagnoses.
ST has only been recently developed for cluster C PD and empirical evidence on its effectiveness is still limited. Recent developments suggest that, for this population, schematic modes should be prioritized over schemas [25]. This is because the problems presented by patients are easily understood in terms of related modes, making it easier for therapists to identify and address these during sessions. Although it did not focus solely on cluster C PD patients, the multicenter randomized controlled trial (RCT) conducted by [4] was the first such study to demonstrate the superiority of ST for this population when compared to clarification-oriented psychotherapy or TAU. In discussing the findings, the authors highlight use of the mode model and experiential techniques as essential elements.
A three-year RCT aimed to investigate ST effectiveness for patients convicted of crimes and hospitalized in institutions aimed at rehabilitation and social reintegration [15]. The authors presented preliminary data from 30 patients (from a total sample of 102) with antisocial, borderline, narcissistic or paranoid personalities, submitted to three years of ST or treatment as usual. Results, although still partial and non-significant, reveal that ST is effective at reducing relapse risk and promoting social reintegration.
Although their findings are preliminary, favorable results were reported for the application of ST in a difficult-to-manage population including patients with antisocial personality and high psychopathy scores [15]. A plausible explanation for this outcome is the intensive and long-term nature of ST. Patients underwent ST twice a week and this was reduced to weekly sessions only in the third year, when they entered the social reintegration stage. Another relevant aspect is the therapist’s ability to form a genuine emotional connection, overcoming the patient’s emotional barriers and reaching their most vulnerable emotions. In addition, treating the forensic population using the mode model and reducing the use of maladaptive coping modes seems to be an effective strategy to mitigate antisocial behaviors.
Final considerations
This review shows an overall increase in the number of studies on the clinical effectiveness of ST in different psychiatric populations, particularly by European researchers. A larger number of studies examining the schema approach in other PD (in addition to BPD) are underway, including cluster C PD and antisocial PD. Furthermore, studies investigating other modalities and contexts of ST application, such as group and inpatient treatment, have broadened the research area and enabled the development of more specialized protocols tailored to specific populations.
Nevertheless, although empirical support for ST is growing, RCTs are still rare, preventing broader generalizations. Some points should be considered when conducting these studies [26]: (1) the population under study should be described in detail, and (2) the study design should include a control group, apply psychometric instruments and allow broader generalizations. In addition, due to methodological differences in ST application (frequency, intensity, techniques used/prioritized), some direct comparisons cannot be made. In this respect, future research should strive to meet these requirements to ensure that scientific studies on the clinical effectiveness of ST are better designed.
[1]For further information, see [10].
References
2021 Copyright OAT. All rights reserv
- Cockram DM, Drummond PD, Lee CW (2010) Role and treatment of early maladaptive schemas in Vietnam Veterans with PTSD. Clin Psychol Psychother 17: 165-182. [Crossref]
- Simpson SG, Morrow E, van Vreeswijk M, Reid C (2010) Group schema therapy for eating disorders: a pilot study. Front Psychol 1: 182. [Crossref]
- Thimm JC (2010) Personality and early maladaptive schemas: a five-factor model perspective. J Behav Ther Exp Psychiatry 41: 373-380. [Crossref]
- Bamelis LL, Evers SM, Spinhoven P, Arntz A (2014) Results of a multicenter randomized controlled trial of the clinical effectiveness of schema therapy for personality disorders. Am J Psychiatry 171: 305-322. [Crossref]
- Dickhaut V, Arntz A (2014) Combined group and individual schema therapy for borderline personality disorder: a pilot study. J Behav Ther Exp Psychiatry 45: 242-251. [Crossref]
- Farrell JM, Shaw IA, Webber MA (2009) A schema focused approach to group psychotherapy for outpatients with borderline personality disorder: a randomized controlled trial. J Behav Ther Exp Psychiatry 40: 317-328. [Crossref]
- Giesen-Bloo J, van Dick R, Spinhoven P, van Tilburg W, Dirksen C, et al. (2006) Outpatient psychotherapy for borderline personality disorder: randomized trial of schema-focused therapy vs transference-focused psychotherapy. Arch Gen Psychiatry 63: 649-658. [Crossref]
- Nadort M, Arntz A, Smit JH, Giesen-Bloo J, Eikelenboom M, et al. (2009) Implementation of outpatient schema therapy for borderline personality disorder with versus without crisis support by the therapist outside office hours: a randomized trial. Behav Res Ther 47: 961-973. [Crossref]
- Renner F, van Goor M, Huibers M, Arntz A, Butz B, et al. (2013) Short-term group schema cognitive-behavioral therapy for young adults with personality disorder features: associations with change in symptomatic distress, schemas, schema modes and coping styles. Behaviour Research and Therapy 51: 487-492.
- Masley SA, Gillanders DT, Simpson SG, Taylor MA (2012) A systematic review of the evidence base for Schema Therapy. Cogn Behav Ther 41: 185-202. [Crossref]
- Harris JD, Quatman CE, Manring MM, Siston RA, Flanigan DC (2014) How to write a systematic review. Am J Sports Med 42: 2761-2768. [Crossref]
- Harbour R, Miller J (2001) A new system for grading recommendations in evidence based guidelines. BMJ 323: 334-336. [Crossref]
- Carter JD, McIntosh VV, Jordan J, Porter RJ, Frampton CM, et al. (2013) Psychotherapy for depression: a randomized clinical trial comparing schema therapy and cognitive behavior therapy. J Affect Disord 151: 500-505. [Crossref]
- Malogiannis IA, Arntz A, Spyropoulou A, Tsartsara E, Aggeli A, et al. (2014) Schema therapy for patients with chronic depression: a single case series study. J Behav Ther Exp Psychiatry 45: 319-329. [Crossref]
- Bernstein DP, Nijman HLI, Karos K, Kuelen de Vos M, Vogel V, et al. (2012) Schema Therapy for forensic patients with personality disorders: design and preliminary findings of a multicenter randomized clinical trial in the Netherlands. International Journal of Forensic Mental Health 11: 312-324.
- Reiss N, Lieb K, Arntz A, Shaw IA, Farrell J (2014) Responding to the treatment challenge of patients with severe BPD: results of three pilot studies of inpatient schema therapy. Behav Cogn Psychother 42: 355-367. [Crossref]
- Van Vresswijk MF, Spinhoven P, Eurelings-Bontekoe EHM, Broersen J (2014) Changes in symptom severity, schemas and modes in heterogeneous psychiatric patient groups following short-term schema cognitive-behavioral group therapy: a naturalistic pre-treatment and post-treatment design in an outpatient clinic. Clinical Psychology and Psychotherapy 21: 29-38.
- Videler AC, Rossi G, Schoevaars M, van der Feltz-Cornelis CM, van Alphen SP (2014) Effects of schema group therapy in older outpatients: a proof of concept study. Int Psychogeriatr 26: 1709-1717. [Crossref]
- Fournier JC, DeRubeis RJ, Shelton RC, Hollon SD, Amsterdam JD, et al. (2009) Prediction of response to medication and cognitive therapy in the treatment of moderate to severe depression. J Consult Clin Psychol 77: 775-787. [Crossref]
- Cuijpers P, van Straten A, Schuurmans J, van Oppen P, Hollon SD, et al. (2010) Psychotherapy for chronic major depression and dysthymia: a meta-analysis. Clin Psychol Rev 30: 51-62. [Crossref]
- Klein DN (2008) Classification of depressive disorders in the DSM-V: proposal for a two-dimension system. J Abnorm Psychol 117: 552-560. [Crossref]
- Nordahl HM, Nysaeter TE (2005) Schema therapy for patients with borderline personality disorder: a single case series. J Behav Ther Exp Psychiatry 36: 254-264. [Crossref]
- Farrell J (2012) Introduction for group schema therapy. In: The Wiley-Blackwell Handbook of Schema Therapy: Theory, Research and Practice. Van Vreeswijk M, Broersen J, Nadort M (Eds.), Chichester, United Kingdom, Wiley-Blackwell, 2012: 337-339.
- Broersen J, van Vreeswijk M (2012) Schema therapy in groups: a short-term schema CBT protocol. In: The Wiley-Blackwell Handbook of Schema Therapy: Theory, Research and Practice. Van Vreeswijk M, Broersen J, Nadort M (Eds.), Chichester, United Kingdom, Wiley-Blackwell: 373-81.
- Arntz A (2012) Schema therapy for cluster C personality disorders. In: The Wiley-Blackwell Handbook of Schema Therapy: Theory, Research and Practice. Van Vreeswijk M, Broersen J, Nadort, M (Eds.), Chichester, United Kingdom, Wiley-Blackwell, 2012: 397–414.
- Bamelis L, Bloo J, Bernstein D, Arntz A (2012) Effectiveness studies. In: The Wiley-Blackwell Handbook of Schema Therapy: Theory, Research and Practice. Van Vreeswijk M, Broersen J, Nadort M (Eds.), Chichester, United Kingdom, Wiley-Blackwell, 2012: 495-510.


