Abstract
Tuberous sclerosis complex (TSC) is a common neurocutaneous syndrome inherited as autosomal dominant pattern affecting virtually every organ systems of the body resulting in a variety of hamartomatous lesions. Classically, it is described as clinical triad of adenoma sebaceum, mental retardation and seizures. Angiomyolipoma (AML) is the commonest benign mesenchymal renal neoplasm composed of fat, vascular and smooth muscle components. It can present sporadically or may be associated with tuberous sclerosis complex.
We report a rare case of spontaneous giant pseudoaneurym with hematoma formation in a renal angiomyolipoma of a 25 year old female associated with TSC who presented with right flank pain and tenderness for 5 day and fever for 2 days. The patient underwent emergency selective renal angiography with embolisation to stop intrarenal bleed and prevent future rebleed.
Giant pseudoaneurysm in a renal angiomyolipoma associated with tuberous sclerosis complex is rare. Transarterial embolization may at times be required to stop the bleed or prophylactically to prevent chances of intralesional pseudoaneurysmal rupture. Surgery may be indicated when vascular interventional facilities are not available.
Key words
angiomyolipoma, angiography, embolisation, tuberous sclerosis, ultrasound
Introduction
Tuberous sclerosis complex (TSC) is a common neurocutaneous syndrome inherited as autosomal dominant pattern affecting cellular differentiation, proliferation, and migration early in development, resulting in a variety of hamartomatous lesions. Classically, it is described as clinical triad of adenoma sebaceum, mental retardation and seizures. It may affect virtually every organ system of the body, most commonly the brain, skin, eyes, heart, kidneys, and lungs.
Angiomyolipomas (AMLs) are the most common benign mesenchymal renal lesions derived from perivascular epithelioid cells and composed of fat, vascular and smooth muscle elements besides spindle cells. It can occur sporadically or may be associated with tuberous sclerosis. According to study by JA Cook et.al., angiomyolipoma is the commonest benign renal lesion, occurring in 49% of patients, out of them 91% and 84% are multiple and bilateral respectively [1].
We present here a case of spontaneous giant pseudoaneurysm and hematoma formation in a renal angiomyolipoma (AML) associated with TSC.
Case report
A twenty five years old female patient was referred for transabdominal ultrasonography with chief complains of right flank pain for five days, multiple episodes of vomiting and fever for two days. She has five siblings without any stigma of TSC. On examination, she had external stigma such as adenoma sebaceum on face, multiple shagreen patches and periungual fibromas (Figures 1A-D) along with pallor and right flank tenderness.
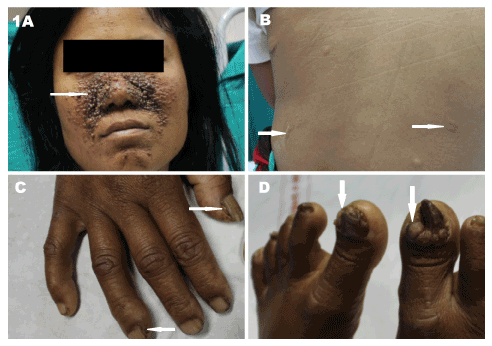
Figure 1. Twenty five years female patient with tuberous sclerosis presenting with right flank pain, fever and anemia showing the following external stigmatas A. Facial adenoma sebaceum (white arrow). B. Shagreen patches (white arrows). C. Subungual fibromas in the hand (white arrows). D. Subungual fibromas in the feet (white arrows).
Ultrasound was performed using 4-5.5 MHz curvilinear transducer (Logiq P5, GE Milwaukee US) which showed an enlarged right kidney with multiple heteroechoic mass lesions in both kidneys (Figures 2A & 2B). The largest lesion in right kidney showed a central anechoic and peripheral thick hyperechoic area (Figures 2A & 2C). On color Doppler, the central anechoic area measured 4.3 cm x 3.8 cm and displayed "swirling to and fro" color flow (Figure 2 C&D).
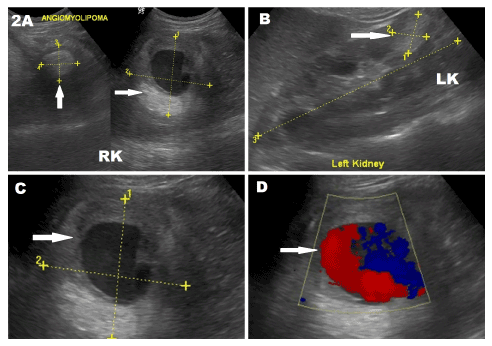
Figure 2. Ultrasonography of the right kidney of twenty five years female patient with tuberous sclerosis presenting with right flank pain, fever and anemia showing renal angiomyolipomas. A. Scan showing enlarged right kidney with two echogenic angiomyolipomas (white arrows), the larger one in the mid pole showing internal round hypoechoic centre. B. Scan showing left kidney showing an echogenic angiomyolipoma (arrow) in lower pole. C. Magnified view of the lesion in the mid pole of the right kidney showing central anechoic area. D. Color Doppler of the right renal lesion showing a large central anechoic area with turbulent ying yang flow suggests pseudoaneurysm (arrow).
On the same day, cross-sectional imaging of the brain and abdomen were performed using 128 multislice computed tomography (CT) SOMATOM Definition AS (Siemens AG, Germany) and 1.5 Tesla MAGNETOM Avanto (Siemens AG, Germany) magnetic resonance imaging (MRI). Plain brain CT scan showed multiple calcified subependymal nodules (Figure 3A). MRI revealed multiple T2 hyperintense cortical tubers (Figure 3B). Contrast enhanced CT scan of abdomen revealed multiple heterodense renal mass lesions in bilateral kidneys with areas of soft tissue and fat attenuation components (HU= -45 to -80) suggestive of multiple AMLs. The largest AML in right mid portion kidney measured 9 cm x 8 cm x 9 cm and showed a central round nonenhancing area of pseudoaneurysm measuring 4.3 cm x 3.8 cm x 4.9 cm suggestive of spontaneous thrombosis. Minimal ascites was noted. Rest of the abdomen was unremarkable (Figure 3C).
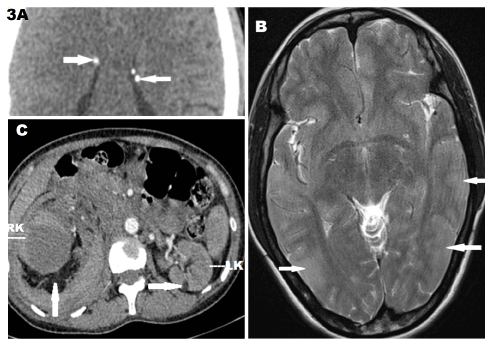
Figure 3. Cross sectional imaging of twenty five years female patient with tuberous sclerosis presenting with right flank pain, fever and anemia showing A. Multiple calcified subependymal nodules (white arrows) in plain CT brain. B. Multiple hyperintense cortical tubers (white arrows) onT2WI MRI. C. Bilateral angiomyolipomas seen as fat-dense lesions in bilateral kidneys (white arrows) with largest in right mid pole. Non enhancing central component in the right renal lesion suggest thrombus.
Based on above findings, diagnosis of giant pseudoaneurysm and hematoma formation in an AML of the right kidney associated with TSC was made.
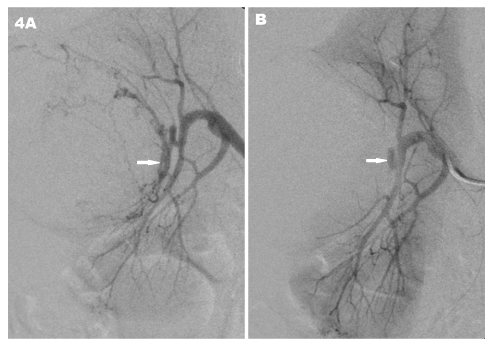
As the patient was severely anemic she was transfused with multiple packed red cell units. Following stabilization,urgent digital subtraction angiography (DSA) was performed on BV Endura C-arm X-ray machine (Philips, Holland). Selective right renal angiography showed a large tumor blush with enlarged feeders from mid polar segmental arteries with no pseudoaneurysm as it was thrombosed (Figure 4A). Embolization was performed after selective catheterization of the feeder with 1.8F Microferret catheter (Cook, USA) using PVA 200 particles (Cook, USA) to prevent future risk of rebleed (Figure 4B).
. <strong>B. </strong>Post embolization showing complete obliteration of supplying segmental arteries (white arrow).</p>
<h2>Discussion</h2>
<p>On sonography, the angiomyolipoma appears heteroechoic with hyperechoic components similar to renal sinus fat due to presence of detectable amount of fat. Presence of fat can be confirmed on CT and MRI. In addition CT can rarely show calcification. Fatty components shows hyperintensity on T1WI MRI with signal loss on fat saturated sequences [2-4]. Minimal fat content can easily be detected by using opposed phase MR imaging which produces characteristic fat-water interface black line also called as the "India ink artifact" [4].</p>
<p>The blood vessels in AML are tortuous and thick walled with absence supportive elastic tissue which predisposes to the formation of intralesional pseudoaneurysm. Renal angiomyolipoma can bleed spontaneously, especially if they are larger than 3.5 cm in diameter, producing intrarenal or extrarenal hemorrhages in the form of retroperitoneal hematoma, hematuria or both [5].</p>
<p>TSC-associated angiomyolipoma tend to be multiple,large in size and more likely to cause spontaneous haemorrhage than the sporadic forms [6]. Tumor and aneurysm diameters have been used as a criterion for predictors of rupture and hence the need of prophylactic treatment. There is increased incidence of pseudoaneurysm formation in angiomyolipomas larger than 4cm and increased possibility of rupture if the pseudoaneurysm is 5 mm or large [7]. Only a few cases of large pseudoaneurysm associated with TSC is described in the literature [8,9]. In our case the angiomyolipoma (including hematoma) and the pseudoaneurysm were quite large measuring 9 cm x 8 cm x 9 cm and 4.3 cm x 3.8 cm x 4.9 cm respectively.</p>
<p>Most angiomyolipomas being a benign and asymptomatic can be managed conservatively with regular follow up imaging. Intervention is required when there is suspicion of malignancy or a large pseudoaneurysm formation which has risk of spontaneous haemorrhage. It can be treated by minimally invasive radiological procedures such superselective renal embolization [5,10]. We performed selective embolization to prevent future rebleed within the large angiomyolipoma. On rare occasions, it may require partial or complete nephrectomy when bleeding cannot be controlled especially if embolization facility is not available.</p>
<h2>Conclusion</h2>
<p>Whenever there are multiple angiomyolipoma in kidney, the diagnosis of tuberous sclerosis complex must be ruled out. There is an increased incidence of pseudoaneurysm formation within AMLs associated with TSC or when lesion size is larger than 4 cm. Larger the aneurysm size, greater are the chances of rupture and fatality. Treatment,such as prophylactic transarterial superselective embolization of angiomyolipoma, is performed to decrease the risk of spontaneous hemorrhage when angiomyolipoma has already bled or exceeds the size criteria.</p>
<h2>Acknowledgements</h2>
<p>We thank the staffs of the Department of Radiology and Imaging at NEIGRIHMS, Shillong, Meghalaya.</p>
<h2>References</h2>
<ol>
<li>Cook JA, Oliver K, Mueller RF, Sampson J (1996) A cross sectional study of renal involvement in tuberous sclerosis. <em>J Med Genet</em> 33: 480-484. <a href=)
[Crossref]
Casper KA, Donnelly LF, Chen B, Bissler JJ (2002) Tuberous Sclerosis Complex: Renal imaging findings. Radiology 225: 451-456. [Crossref]
Maizlin ZV, Gottlieb P, Simon YC, Strauss S (2002) Various Appearances of Multiple Angiomyolipomas in the Same Kidney in a Patient without Tuberous Sclerosis. J Ultrasound Med 21: 211-213. [Crossref]
Israel GM, Hindman N, Hecht E, Krinsky G (2005) The Use of Opposed-Phase Chemical Shift MRI in the Diagnosis of Renal Angiomyolipomas. AJR Am J Roentgenol 184: 1868-1872. [Crossref]
Van Baal JG, Smits NJ, Keeman JN, Lindhout D, Verhoef S (1994) The evolution of renal angiomyolipomas in patients with tuberous sclerosis. J Urol 152: 35-38. [Crossref]
Nelson CP, Sanda MG (2002) Contemporary diagnosis and management of renal angiomyolipoma. J Urol 168: 1315-1325. [Crossref]
Yamakado K, Tanaka N, Nakagawa T, Kobayashi S, Yanagawa M, et al. (2002) Renal Angiomyolipoma: Relationships between Tumor size, Aneurysm Formation, and Rupture. Radiology 225: 78-82. [Crossref]
Choh NA, Choh SA, Yousuf R, Jehangir M (2009) A giant aneurysm arising from renal angiomyolipoma in tuberous sclerosis. Arch Dis Child 94: 47-48. [Crossref]
Lapeyre M, Correas JM, Ortonne N, Balleyguier C, Helenon O (2002) Color-Flow Doppler Sonography of Pseudoaneurysms in Patients with Bleeding Renal Angiomyolipoma. AJR Am J Roentgenol 179: 145-147. [Crossref]
De Luca S, Terrone C, Rossetti SR (1999) Management of renal angiomyolipoma: a report of 53 cases. BJU Int 83:215-8. [Crossref]