A 33-year-oldCaucasian male presented to the emergency department with lower extremity edema, dyspnea, and orthopnea. A transthoracic echocardiogram demonstrated an ejection fraction of 10% with global hypo kinesis, biventricular dilatation, and moderate mitral regurgitation. A right heart catheterization demonstrated a pulmonary capillary wedge pressure of 40mmHg and reduced cardiac index of 1.7. Coronary angiography revealed no evidence of obstructive coronary artery disease. An extensive infectious and rheumatologic workup was negative. During the clinical admission for NYHA class 4 heart failure, the patient developed flash pulmonary edema causing hypoxic respiratory failure and he was subsequently intubated requiring pressors. He received aggressive IV diuresis with ionotropic support and was eventually weaned off ionotropic support and started on metoprolol and enalapril for afterload reduction. After marked improvement of his cardiovascular hemodynamics, he could be extubated. Upon further questioning, the patients admitted to using anabolic androgenic steroids for the past year. After an extensive negative workup, the underlying etiology of the cardiomyopathy was postulated to be due to Anabolic Androgenic Steroids abuse. At 10-month cardiology follow-up, continuation of standard medical therapy for systolic heart failure, and complete cessation of anabolic androgenic steroids usage, the patient remained asymptomatic with significant improvement of his ejection fraction to 45%.
anabolic androgenic steroids, acute heart failure
Acute heart failure is defined as the onset of symptoms or signs of heart failure (HF) in a patient with no prior history of heart failure. It is uncommon to have acute decompensated heart failure in patients without concomitant acute coronary syndromes [1]. Acute decompensated heart failure broadly represents new or worsening symptoms or signs of dyspnea, fatigue or edema that lead to hospital admission or unscheduled medical care and that are consistent with an underlying worsening of left ventricular function [2]. It is estimated that 5.7 million Americans greater than 20 years of age have HF [3]. Currently there are 870,000 new HF cases diagnosed annually [3]. It is projected that the prevalence of HF will increase 46% from 2012 to 2030, resulting in greater than 8 million people over 18 years of age with heart failure [4]. Symptoms of HF are the result of severe pulmonary congestion due to elevated left ventricular filling pressures which can occur with or without low cardiac output. Acute HF can occur in patients with preserved or reduced ejection fraction [3]. Usual causes are conditions such as coronary heart disease, hypertension, valvular heart disease, atrial arrhythmias, and/or noncardiac conditions (including renal dysfunction, diabetes, anemia) [3].
A 33-year-old Caucasian male with a past medical of asthma presented from an outside hospital with progressive lower extremity edema, dyspnea initially on exertion then at rest, and orthopnea. Patient stated that his symptoms began 2 weeks prior to admission. Previous to this, the patient was an active weight-lifter and attended the gym 6 days per week. At presentation, vitals were blood pressure 145/90, heart rate of 133 beats per minute, respiratory rate of 35-40, oxygen saturation of 95% on 2liters nasal cannula and he was afebrile. On physical exam, the patient was in respiratory distress with accessory muscle use, and paradoxical breathing. Lung exam was remarkable for diffuse rales and his legs had 2 plus pitting edemas bilaterally up to both his knees.
Laboratory investigations demonstrated elevated erythrocyte sedimentation rate and D-Dimer. His infectious work-up included cytomegaly virus, ebsteinbarr virus, human immunodeficiency virus, respiratory viral panel, hepatitis virus B/C, coxsackie A virus, parvovirus B19 and blood cultures which were all negative. Urine drug screen was negative. His rheumatological work-up included anti-nuclear antibody, anti-smooth muscle antibody and anti-mitochondrial antibody and all were within normal limits. His troponins trended were all negative. Other investigations including blood count, thyroid-stimulating hormone, liver function, cholesterol levels, ferritin were all within normal limits.
Chest x-ray demonstrated that his heart was enlarged with diffuse patchy opacities and pulmonary vascular cephalization consistent with moderate pulmonary edema. Electro-cardiogram demonstrated sinus tachycardia with a heart rate of 125 beats per minute (Figure 1). A (TTE)from an outside hospital demonstrated acute systolic heart failure with left ventricular ejection fraction of10% with global hypo kinesis with no evidence of hypertrophic obstructive cardiomyopathy. A repeat TTE on hospital day 4 demonstrated an ejection fraction of less than 25%, severe global hypo kinesis of the left ventricle consistent with a cardiomyopathy, moderate bi-atrial/biventricular dilation and moderate mitral valve regurgitation (Figure 2, Figure 3). Cardiac catheterization was performed on hospital day the right heart catheterization showed elevated pulmonary capillary wedge pressure of 40mmHg and reduced cardiac index of 1.7 whereas the left heart catheterization was negative for coronary artery disease. A cardiac magnetic resonance imaging was not suggestive of infiltrative diseases.

Figure 1. EKG demonstrating sinus tachycardia with a rate of 125. Normal axis, PR, QRS, and QT intervals. Left ventricular hypertrophy, septal wall infarct of age undetermined age, and inverted T wave abnormality in V5-V6 which could signify lateral ischemia.
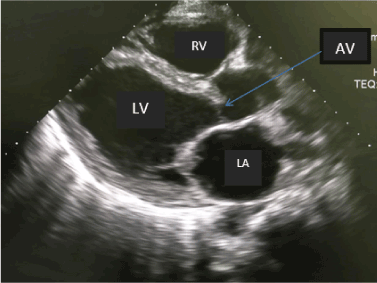
Figure 2. Parasternal long axis viewfrom TTE. This echo images showed a mildly dilated Left atrium (LA) and a mildly left ventricle (LV). Aortic valve(AV), Right ventricle(RV).
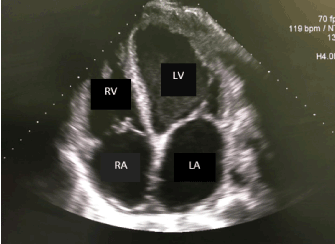
Figure 3. Four chamber view of TTE. Echo image demonstrates biatrial and biventricular dilation. Right atrium(RA), Left atrium (LA), left ventricle (LV), Right ventricle(RV).
Given his worsening clinical status, the patient was scheduled to be transferred to a tertiary center for urgent evaluation for placement of a mechanical left ventricular assistance device, but he decompensated the evening prior. His chest x-ray demonstrated worsening pulmonary edema. He then became lethargic, tachypneic, and was intubated due to flash pulmonary edema causing hypoxic respiratory failure. He was stabilized on norepinephrine and milrinone drips and was transferred to a tertiary facility. Ultimately, his norepinephrine and milrinone drips were weaned off and he was transitioned to an oral heart failure regimen including: metoprolol and enalapril afterload reduction as part of his HF management. The etiology of his cardiomyopathy was unclear but the patient endorsed that he also had been using anabolic androgenic steroids (AAS)for one year, which was supplied by a friend from his gym. Thus, in light of his otherwise extensive, negative workup, it was postulated that the abuse of AAS was the likely cause of his cardiomyopathy. At the time of hospital discharge, he had NYHA class 2 CHF symptoms and he was able to ambulate without any difficulty. He was instructed not to resume taking AAS.
At 10-month cardiology follow-up with continuation of standard medical therapy for systolic heart failure and complete cessation of AAS usage, the patient remained asymptomatic with significant improvement of his ejection fraction to 45%. He currently has NYHA class 1 symptoms.
The use of Anabolic Androgenic Steroids (AAS) has been linked to causing myocardial infarction, sudden cardiac death, ventricular fibrillation with exercise, atrial fibrillation, cardiac tamponade, and development of dilated cardiomyopathy [5]. AAS like other endogenous steroids influence left ventricular hypertrophic response through the androgen receptor. Androgen receptors are found on skeletal muscle and also on cardiac myocytes. They cause alterations in heart structure, including left ventricular hypertrophy, dilation which can cause impaired contraction and relaxation [6]. Anabolic steroids can induce an unfavorable enlargement and thickening of the left ventricle, which loses its diastolic properties with the mass increase [7]. AAS can also cause hypertension, dyslipidemia, and impaired fasting glucose [8]. The effect of anabolic androgenic steroids on the cardiovascular system has been well described in the literature; however, the knowledge of these effects amongst amateur sports participants is poor [9]. A qualitative, cross-sectional, observational study using an anonymous online questionnaire completed by amateur sports participants enrolled in competitive sports teams at an Irish university demonstrated that one-third of respondents personally knew someone that uses anabolic steroids, however 59% of participants were never advised about their health effects [9]. The majority (59%) of respondents obtained their nutritional advice from Internet sites or friends and only 26% of respondents knew about the blood pressure and cholesterol effects of anabolic steroid use [9].
The knowledge of the cardiac risks associated with the use of AAS amongst sports participants is generally poor [9]. Efforts must be made to educate coaches and gym facilities about the harmful effects of certain performance enhancing drugs.
None
- Allen LA, O'Connor CM (2007) Management of acute decompensated heart failure. CMAJ 176: 797-805. [Crossref]
- Felker GM, Adams KF Jr, Konstam MA, O'Connor CM, Gheorghiade M (2003) The problem of decompensated heart failure: nomenclature, classification, and risk stratification. Am Heart J 145: S18-25. [Crossref]
- Mozaffarian D, Benjamin EJ, Go AS, Arnett DK, Blaha MJ, et al. (2015) Heart disease and stroke statistic--2015 update: a report from the American Heart Association. Circulation 2015;131: e29-e322. [Crossref]
2021 Copyright OAT. All rights reserv
- Heidenreich PA, Albert NM, Allen LA, Bluemke DA, Butler J, et al. (2013) Forecasting the impact of heart failure in the United States: a policy statement from the American Heart Association. Circ Heart Fail 6:606-619. [Crossref]
- Ahlgrim C, Guglin M (2009) Anabolics and cardiomyopathy in a bodybuilder: case report and literature review. J Card Fail 15: 496-500. [Crossref]
- Figueredo VM (2011) Chemical cardiomyopathies: the negative effects of medications and nonprescribed drugs on the heart. Am J Med 124: 480-488. [Crossref]
- De Piccoli B, Giada F, Benettin A, Sartori F, Piccolo E (1991) Anabolic steroid use in body builders: an echocardiographic study of left ventricle morphology and function. Int J Sports Med 12: 408-412. [Crossref]
- [No authors listed] (1987) American College of Sports Medicine position stand on the use of anabolic-androgenic steroids in sports. Med Sci Sports Exerc 19: 534-539. [Crossref]
- S. Y Naqvi, G. Flaherty. (2016) Knowledge, and Attitudes of Amateur Sports Participants Regarding the Cardiac Risks Associated with the Use of Anabolic-Androgenic Steroids. IOSR Journal of Sports and Physical Education 36-44.



