Abstract
The purpose of this study was to report an intervention process for promoting the wearing of eyeglasses and to examine the effects of intervention for 1.5 years upon fixation duration with and without eyeglasses in a child with severe motor and intellectual disabilities. The subject was an 11-year-old boy with quadriplegia, mental retardation, and epilepsy. He was recommended wearing of eyeglasses for correction of nearsightedness and astigmatism. When the subject wore eyeglasses for the first time, he immediately removed them and refused to wear eyeglasses. A step-by-step approach was used with eyeglasses without corrective lenses for 7 months, for correction of nearsightedness for 5 months, and for correction of nearsightedness and astigmatism for 6 months, to allow a gradual adjustment to wearing eyeglasses. Intervention was through use of physical contacts and activities in a darkened and separate room, to ease into the wearing of eyeglasses. After the longitudinal habilitation to eyeglass wear, the subject could wear eyeglasses for 60 minutes. He spent a great deal of time watching television during the day and could move to look for a toy. The fixation length with eyeglasses was, therefore, significantly longer than without eyeglasses. The refusal to wear eyeglasses decreased after repeated graded interventions, and the subject could wear the eyeglasses longer than before intervention. After wearing eyeglasses, the patient may have been able to recognize his surroundings better than before.
Key words
eyeglasses fixation, prescription, profound intellectual multiple disabilities, severe motorand intellectual disabilities
Introduction
Individuals with severe motor and intellectual disabilities (SMID) often have profound motor dysfunctions and severe mental disabilities. Visual functions in persons with SMID have been assessed for optimization of their visual environments by interprofessional collaborations (i.e., ophthalmologists, orthoptists, occupational therapists, speech pathologists, physical therapists, teachers, and pediatricians) at our institute for developmental disabilities. Within our team, occupational therapists and pediatricians have mainly evaluated the client's health, body functions and structure, activity, and participation in daily living situations. Ophthalmologists and orthoptists have assessed the patient's detailed visual functions. A high prevalence of ophthalmological abnormalities was reported in children with mental retardation or cerebral palsy [1,2].
When a client has serious intellectual disabilities, it is difficult to evaluate their visual function [3], and for them to wear or continue wearing eyeglasses [4]. Therefore, an interprofessional approach and a long-term intervention are needed. Interventional approaches for promoting the wearing of prescription eyeglasses in mentally retarded clients have been reported [4]. Few studies have focused on the use of different fixation durations with and without eyeglasses, as the effects of the correction with eyeglasses are often associated with longitudinal interventions by the care staff. The purpose of this study was therefore to report an intervention process for promoting the wearing of eyeglasses, and to examine the effects of the intervention for 1.5 years of follow-up on fixation duration with and without eyeglasses in a child with SMID.
Case presentation
The subject of this study was an 11-year-old male with quadriplegia, mental retardation, and epilepsy that were sequelae of acute encephalopathy. The participant's family provided informed consent, and the study was approved by the institutional ethics committee of the International University of Health and Welfare. The study conformed to the tenets of the Declaration of Helsinki. At the age of 11 months, the patient developed acute encephalopathy secondary to pyrexia fever, dehydration, and convulsion with subsequently significant cerebral atrophy (Figure 1). The participant's birth weight was 1,768 g (gestational weeks: 38) because of intrauterine growth restriction. The subject was placed in an institution for developmental disabilities when 2-years-old. The subject still lives in the same institution, and spends a great deal of time at self-stimulatory behaviors that are dependent upon touch and auditory sensations. These behaviors include sitting alone, without speaking or communicating verbally. The subject has undergone specialized therapies, including occupational therapy, physical therapy, special needs education, and pedagogic stimulation several times a week. According to the assessments of the ophthalmologist and orthoptist, he had intermittent exotropia, nearsightedness, and astigmatism. Therefore, eyeglasses for correction of nearsightedness and astigmatism were recommended. Occupational therapists practiced for the purpose of promoting the wearing eyeglasses. Orthoptists assessed the visual function.
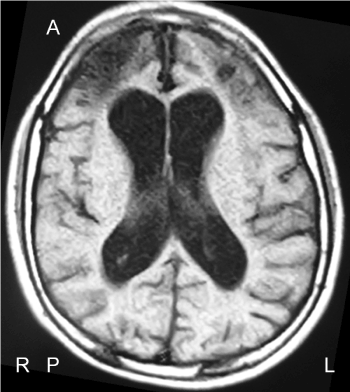
Figure 1. Magnetic resonance imaging of the patient (A: anterior, P: posterior, R: right, L: left).
Stage 1 (7 months duration)
When the subject wore eyeglasses for the first time, he immediately took them off and refused wearing of eyeglasses. Occupational therapists then used eyeglasses without corrective lenses for the purpose of adjusting gradually to wearing eyeglasses during occupational therapy sessions. He could not pursue an object. He did not show an interest in a cartoon on a notebook computer monitor and often touched the monitor or threw the notebook computer. Therefore, the occupational therapists intervened using touch and auditory sensations. Occupational therapists have also attempted to lessen the patient's stress of wearing eyeglasses through use of physical contacts or music in the darkened room. Under the supervision of the occupational therapists, the patient tried the use of eyeglasses in a darkened room, which was easier for observing a television show or a light, to be interested in and use vision. The visual acuity of each eye with or without eyeglasses could not be recorded, but binocular visual acuity without eyeglasses was 0.037, as determined by Teller acuity cards (TACs) [5]. When the occupational therapist requested, the patient could wear eyeglasses for 1 to 3 minutes. The duration was measured by occupational therapists using timepieces. However, once the occupational therapist left the room, the subject immediately removed the eyeglasses.
Stage 2 (5 months duration)
Eyeglasses were used for correction of nearsightedness [Right (R): −5.0D, Left (L): −5.0D] once the subject could wear eyeglasses without corrective lens for several minutes during occupational therapy sessions. When he wore the eyeglasses for correction for the first time, he looked slowly around. The patient could pursue an object for a few seconds. Occupational therapy sessions were changed separate room to allow the subject to concentrate on the visual stimuli. Patient monitor touching or throwing of objects was decreased when wearing corrective eyeglasses. Therefore, the occupational therapists intervened using toys, which needed to look at hands, and directly in using spoon at the time of a meal. Occupational therapists promoted that his attention using vision was able to turn to hands. He could look at a picture book for several seconds and could notice a toy at 1 meter distance. Subsequent opportunities to wear eye glasses were also increased during his special needs education sessions. His visual acuity was recorded in each eye without eyeglasses, and was right eye: 0.037 and left eye: 0.056, as assessed using the TAC [5]. The patient could eventually wear corrective eyeglasses for 20 minutes or longer, especially during a meal.
Stage 3 (6 months duration)
Occupational therapists finally used eyeglasses for correction of nearsightedness and astigmatism (R: −2.5D, C −2.5D Ax 180°; L: 2.5D, C −2.5D Ax 180°). He could pursue an object for 10 seconds. Occupational therapy sessions continued, using a cartoon and a picture book as visual stimuli in a separate room. The occupational therapists intervened using toys, which needed to use tools. The number of times he removed the eyeglasses was reduced when he was engaged in playing with a toy, or when someone was interacting with him. Visual acuity could be recorded in each eye with and without eyeglasses using TAC [5] (right and left eyes with eyeglasses: 0.15 and 0.07, right and left without eyeglasses: 0.07 and 0.05, respectively). While wearing the eyeglasses, the subject could move to look for a toy, and he showed increased vision and increased eye-hand coordination. He could eventually continue wearing the eyeglasses for 60 minutes, and then spent a great deal of time watching television.
Differences with and without eyeglasses
After long-term habilitation to wearing eyeglasses for 1.5 years, fixation duration in two conditions [without and with eyeglasses (R: −2.5D, C −2.5D, Ax 180°; L: −2.5D, C −2.5D, Ax 180°)] was monitored. The patient sat in his wheelchair that he used every day. In the task, a cartoon with sounds on a notebook computer monitor was displayed for 15 s, followed for 20 s, and then repeated five times. First and seventh authors measured the fixation duration using timepieces on visual recording. To statistically compare fixation duration for the cartoon with and without eyeglasses, the t-test was used. Statistical analysis was performed with SPSS Statistical Packages version 21 (IBM Corp., Armonk, NY, USA). With and without eyeglasses, fixation time was 12.6 ± 2.9 s and 7.4 ± 3.8 s (mean ± standard deviation), respectively. The fixation length with eyeglasses was significantly longer than without eyeglass [t (8) = 2,419, p = 0.042)] (Figure 2).
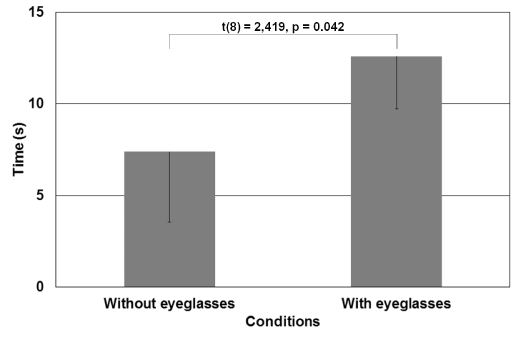
Figure 2. Difference of fixation duration (bar: mean value; error bar: standard deviation among cycles 1–5) in two conditions, with and without eyeglasses.
Discussion
This is one of the first studies to evaluate different fixation durations with and without eyeglasses in an individual with SMID associated with longitudinal habilitation intervention by the occupational therapist. After habilitation for 1.5 years, the subject could continue wearing eyeglasses and the time of fixation duration with eyeglasses to experimental tasks was longer than without eyeglasses. Occupational therapists used physical contacts and activities in a darkened room to ease the subject into wearing eyeglasses. Occupational therapists also allowed him to concentrate on visual stimuli while in a darkened room. The subject's refusal to wear eyeglasses decreased after repeated graded interventions, and he could wear the eyeglasses for longer than before intervention. When wearing eyeglasses, this patient may be more able to recognize external stimuli than without eyeglasses. The correction of acuity with eyeglasses to the elongation of the fixation length enabled to move to look for a toy, to increase vision, to increase eye-hand coordination, to spend a great deal of time watching television.
A step-by-step approach was used with eyeglasses without corrective lenses for 7 months, for correction of nearsightedness for 5 months, and for correction of nearsightedness and astigmatism for 6 months. Occupational therapists considered the characteristics of the sensory processing in early times. The subject spent a great deal of time at self-stimulatory behaviors that are dependent upon touch and auditory sensations. Therefore, the occupational therapists intervened using touch and auditory sensations at stage 1. The patient's stress of wearing eyeglasses reduced through intervention with these senses. Next the intervention using the vision was performed aggressively. The occupational therapists intervened using toys, which needed to look at hands at stage 2 and, which needed to use tools at stage 3. It is useful for care staffs to evaluate and use the characteristics of the sense processing at intervention.
Using functional near infrared spectroscopy, a previous study showed that continuous instruction from the care staff resulted in an individual with quadriplegia, mental retardation, and epilepsy acquiring new upper extremity motions that caused changes in prefrontal brain activation [6]. Using eye tracking technology, we recently reported fixation duration changes in an individual with Rett syndrome associated with longitudinal habilitation intervention by the care staff [7,8]. The participants in the study had SMID. This finding suggests that continuous intervention from the care staffs and family members results in acquiring new upper/lower extremity motions or learning abilities e.g. selection, anticipation, or understanding, for individuals with SMID.
We wanted to use many quantitative data to make our claim convincing. However, quantitative data was limited in occupational therapy records. Therefore, we were using as many quantitative data as possible. The use of quantitative data is important to explain objective results. Not only qualitative but also quantitative date were included to know the subject's changes.
Future study should be done to identify the short term or daily detailed effects of intervention care. Care staffs should routinely evaluate an individual's abilities, adjust intervention plans, and evaluate intervention outcomes. There is a need for multidisciplinary teams involving physicians, psychologists, and therapists in the assessment of children with cortical visual impairment [9]. It is necessary to collaborate interprofessionally to define the optimal visual environment for SMID clients in a manner that is consistent with their visual functions.
Acknowledgments
This study was supported by Grant-in-Aid number 22330260 for Scientific Research from the Japan Society for the Promotion of Science.
Conflicts of interest
The authors have no conflicts of interest for the submission of this manuscript.
Author contributions
The 1st and 7th authors monitored fixation duration. The 2nd, 3rd, 4th, 5th, 6th, and 9th authors established and carried out the longitudinal habilitation protocol. The 8th and 10th authors assessed visual function.
References
- Mwanza JC, Nkidiaka CM, Kayembe DL, Maillet CY, Mukau EJ, Tuela MR (2000) Ophthalmologic abnormalities in mentally retarded. Bull Soc Belge Ophtalmol 277: 75–78. [Crossref]
- Pennefather PM, Tin W (2000) Ocular abnormalities associated with cerebral palsy after preterm birth. Eye 14: 78–81. [Crossref]
- Kwok SK, Ho PC, Chan AK, Gandhi SR, Lam DS (1996) Ocular defects in children and adolescents with severe mental deficiency. J Intellect Disabil Res 40: 330–335.[Crossref]
- DeLeon IG, Hagopian LP, Rodriguez-Catter V, Bowman LG, Long ES, Boelter EW (2008) Increasing wearing of prescription glasses in individuals with mental retardation. J Appl Behav Anal 41: 137–142. [Crossref]
- Teller DY, Morse R, Borton R, Regal D (1974) Visual acuity for vertical and diagonal gratings in human infants. Vision Res 14: 1433–1439.[Crossref]
- Hirano D, Taniguchi T, Takeda K, Arai K, Takiguchi S (2009) Physiological changes of an individual with severe motor and intellectual disabilities as a result of care staff intervention: a near-infrared spectroscopy case study. Brain topography and multimodal imaging. Kyoto University Press, Kyoto, 249–252.
- Hirano D, Hayashi K, Onose Y, Ishii M, Miyauchi M, et al. (2015) Fixation duration changes in Rett syndrome after habilitation intervention. Int J Phys Med Rehabil 3: 1000271.
- Hirano D, Taniguchi T (2015) Application of eye-tracker to individuals with Rett syndrome: a systematic review. Int J Phys Med Rehabil 3: 1000292.
- Matsuba CA, Jan JE (2006) Long-term outcome of children with cortical visual impairment. Dev Med Child Neurol 48: 508–512. [Crossref]


