placenta invasion anomalies, placenta accreata
Placenta invasion anomalies are important conditions as they may cause severe morbidity and mortality. The incidence of abnormal placentation is described in various ratios such as 1/540 to 1/93000 birth rates [1,2]. In recent years, it has been reported that placenta invasion anomalies have increased tenfold and especially the cases in which placenta invades the surrounding tissues are on the increase. The increasing rate of cesarean has been blamed for this situation [3]. With this case report, we aim to report the case about a 36 year old woman who was undergone a G2P1 caesarean section without prenatal visits, who was admitted to emergency department with active vaginal bleeding, and after ultrasonographic evaluation placenta previa was detected and it was suspected whether invasion anomaly accompanied it, for whom an emergency caesarean section was planned after obtaining informed consent and who was hysterectomized by detecting placenta accreta during the operation.
Though the etiology of abnormal placental invasion is not known for certain, it has been presumed that it occurs with the myometrial invasion of the placenta due to the lack of placental barrier function as a result of the disruption of the basal decidua [4]. When chorionic villies adhere to myometrial surface, it is called placenta accreata only when there is no myometrium infiltration, when there is myometrium infiltration, it is called placenta increta, and if there is infiltration into seosa and sometimes into adjacent organs by infiltrating the whole myometrium, it is called placenta percreta. Among placenta invasion anomalies, the incidence of placenta accreta has been reported to be 84%, placenta increta 13%, placenta percreta 30% [5]. Plasenta invasion anomalies constitute the most common indication of postpartum hysterectomy that may result in severe morbidity and mortality [6]. On average 3000-5000 ml blood loss, massive transfusion and as a result of this several complications such as disseminated intravascular coagulopathy, hydration, acute respiratory distress syndrome, infection, ureter and intestine injury, laceration of the bladder can be seen [7]. Therefore, controlling the abnormalities of placental invasion is crucially important in the prevention of morbidity and mortality.
The patient who was 36 years old, had no follow-up, had 34 weeks pregrancy and who had to have a caesarean section due to breech presentation in the 40th week was admitted to the emergency with active painless vaginal bleeding. Placenta previa was detected in the ultrasonographic examination and monitoring the locunae in plasenta on the uterine front wall and the thickness of myometrium’s being less than 1cm aroused suspicion about possible comorbidity of invasion abnormalities. Having informed the patient and her relatives, and receiving approvals, an immediate caesarean section was planned. The patient’s Hb values were detected 10.3 g/dl. Blood center, intensive care and anesthesia teams were informed. The patient, for whom 4 erythrocyte suspension (ES) and four fresh frozen plasma were prepared, was opened two vascular access. She was taken to surgery in the lithotomy position. The abdomen was entered with a median incision under the umblicus. When abnormal placental invasion on the uterine wall, on and above former incision line, was detected with hypervascularisation, the infant weighing 2600 gr was delivered healthily by means of incision from uterine fundus without hurting plasenta. Total hysterectomy was performed with the start of bleeding. It was observed that bladder was adhered to uterus, however, there was no placental infiltration. After vascularised areas on the bladder and the abdomen were checked for bleeding, the operation was completed by putting a drain in the abdomen. As postoperative Hb: 6,2 g/dl was detected, the patient was observed closely by giving 4 unit ES and 2 unit fresh frozen plasma. She was discharged healthily on the fourth postoperative day. The result was reported as placenta accreta in the hystopathological examination which was carried out by pathology (Figure 1).
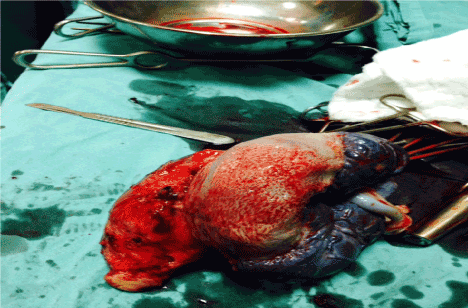
Figure 1. Postoperative Cesarean Hysterectomy Material.
Placenta previa, previous caesarean section, endometrial dilatation curettage, mother aged over 35 are risk factors for abnormal placental invasion [3]. In our case, advanced maternal age and previous caesarean delivery are risk factors. In the studies, in placenta previa cases, where there is no uterine surgery, the rate of placenta accreta was reported to be 5%. The risk ratio for those who had one or two caeserean sections is respectively 24% and 50% and even 67% for those who had four or more operations [8].
The prediction of abnormal placental invasion in antepartum period is the most important factor that affects prognosis. Knowing the diagnosis beforehand reduces mortality and morbidity by enabling the operation to be planned in elective conditions before the delivery and to be handled by experienced surgical and anesthesia team. It has been revealed that peripartum blood loss and transfusion amount are significantly lower in planned caesarean hysterectomy than in emergency operations [9,10]. Furthermore, the completion of the preparation of the blood product in the preoperative period prevents the development of disseminated intravasculer coagulation by enabling transfusion to be performed rapidly. It is also important to determine the proper type of incision before the operation.
Besides clinical findings, transabdominal, transvaginal and doppler ultrasonography are used in the diagnosis. Magnetic resonance imaging ( MRI) is another method that can be used in addition to ultrasound in the cases of obese patients and fundal or posterior placenta [3]. MRI gives information about where placenta is located and the depth of invasion in adjacent organs [11].
In the ultrasonographic examination, placental lacunae, hypoechoic area loss in the retroplacental area, irregularities in bladder- uterine serosa complex, myometrium thickness' being less than 1 cm and protrusion of the placenta into bladder are the symptoms that suggest abnormalities of placental invasion [3,12].
With color doppler ultrasound, high- speed turbulent flow in lacunae, hyper- vascularization in bladder- uterin serosa complex and interruption in retroplacental blood flow suggest placenta accreta [5].
There are two procedures to handle invasion abnormalities, which are surgical and conservative. Classic and definite treatment of abnormalities of placental invasion is postpartum hysterectomy. Supracervical hysterectomy has some advantages such as less blood loss, fewer visceral organ injuries and shorter operation and hospital stay. In total hysterectomy, especially the risk of ureter injury is higher. However, the cases in which placenta accreta accompanies, as placenta is placed in cervix and lower uterine segment, bleeding mostly takes place in these areas. Therefore, total hysterectomy should he preferred for this kind of cases [6]. In surgical approach, the abdomen is entered into with a median incision under the umblicus. In the entrance to uterus, classical median incision that is opened at least 2 cm superior of the placenta location should be preferred. In the cases, when the vascularization is increased and suggests deep placental invasion, hysterectomy takes place after the delivery. Before closure of the abdomen, drain is routinely placed. Hemodynamically unstable patients should be monitored in the intensive care unit. In the postoperative period, patients vital signs, hemorrhage and diuresis should be monitored closely, in the 2nd - 4th and 24th hours following surgery, patients should be evaluated with complete boold count and coagulation parameters. From a technical point of hysterectomy, problems are bladder' s adherence to uterus due to previous operation and the increase of vascularization which developed as a secondary to placental invasion behind bladder. As a result of these during the dissection, bladder injury and excessive bleeding may occur between bladder and uterus. Moreover, performing partial cystectomy by resecting posterior bladder wall may be necessary in the placenta percreta cases when bladder is densely adherent and can't be separated.
Alternatively during pre- operative period, prophylactic perioperative intravascular balloon occlusion or hypogastric artery embolization might be applied in order to prevent bleeding in the patients for whom placenta accreta is being considered [5].
In a case report, Canonico et al. [13] suggest conservative approach for cases which are selected by combining many surgical treatments with prohylactic catheterization of descending aorta by transhumeral or transfemoral access. However, the efficiency and credibility of these methods should be debated. Further studies need to be carried out.
2021 Copyright OAT. All rights reserv
As for conservative approach, it has been performed in recent years to reduce morbidity and surgical complications and protect fertility. Conservative approach was identified by Arulkumaran et al. [14] in 1986 for the first time. They reported that placenta disposal took place on the 11th postpartum day by using 50mg methotrexate treatment intravenously every other day with a total dose of 250 mg.
Yee et al. [15] suggested that uterus was incised from fundus to placenta without any harm and placenta involution occurred at different times varying between 6 weeks to 8 months when uterus and abdomine were closed and placenta was left its place after the clamping of the umbilical cord in the cases when there was no bleeding . With conservative approach, complications such as vaginal bleeding, infection and disseminated intravascular coagulation can be detected and patients may need to be hysterectomized [16]. For this reason, more randomized controlled studies about conservative approach must be carried out.
Consequently, the frequency of abnormalities of placental invasion has been increasing in parallel with the increasing cesarean birth rate [17].
Cesarean hysterectomy which is the classical treatment of the invasion abnormalities is an operation of high morbidity. Therefore, in preoperative period, the patients who are suspected to have abnormal placental invasion in clinical and ultrasonographic terms should be led to comprehensive tertiary centers with necessary equipment, for further evaluation and treatment. Operation should be carried out in a planned way by an experienced team.
This is highly important as it saves lives. It is also a great advantage to be able to give the patient information about hysterectomy and to obtain informed consent before the operation.
- Fox H (1972) Placenta accreata, 1945-1969a. Obstet Gynecol Surv 27: 475-490.
- Breen JL, Neubecker R, Gregori CA, Franklin JE Jr (1977) Placenta accreta, increta, and percreta. A survey of 40 cases. Obstet Gynecol 49: 43-47. [Crossref]
- Thia EW, Lee SL, Tan HK, Tan LK (2007) Ultrasonographical features of morbidly-adherent placentas. Singapore Med J 48: 799-802. [Crossref]
- Thia EW, Tan LK, Devendra K, Yong TT, Tan HK, et al. (2007) Lessons learnt from two women with morbidly adherent placentas and a review of literature. Ann Acad Med Singapore 36: 298-303. [Crossref]
- Chou MM (2004) Prenatal diagnosis and perinatal management of placenta previa accreata: Part, present and future. Taiwanese J Obstet Gynecol 43: 64- 71.
- Rossi AC, Lee RH, Chmait RH (2010) Emergency postpartum hysterectomy for uncontrolled postpartum bleeding: a systematic review. Obstet Gynecol 115: 637-644. [Crossref]
- Shrivastava V, Nageotte M, Major C, Haydon M, Wing D (2007) Case-control comparison of cesarean hysterectomy with and without prophylactic placement of intravascular balloon catheters for placenta accreata. Am J Obstet Gynecol 197: 402: e1-e5
- Mok M, Heidemann B, Dundas K, Gillespie I, Clark V (2008) Interventional radiology in women with suspected placenta accreta undergoing caesarean section. Int J Obstet Anesth 17: 255-261. [Crossref]
- O'Brien JM, Barton JR, Donaldson ES (1996) The management of placenta percreta: conservative and operative strategies. Am J Obstet Gynecol 175: 1632-1638. [Crossref]
- Tikkanen M, Paavonen J, Loukovaara M, Stefanovic V (2011) Antenatal diagnosis of placenta accreta leads to reduced blood loss. Acta Obstet Gynecol Scand 90: 1140-1146. [Crossref]
- Ng MK, Jack GS, Bolton DM, Lawrentschuk N (2009) Placenta percreta with urinary tract involvement: the case for a multidisciplinary approach. Urology 74: 778-782. [Crossref]
- Chan BC, Lam HS, Yuen JH, Lam TP, Tso WK, et al. (2008) Conservative management of placenta praevia with accreta. Hong Kong Med J 14: 479-484. [Crossref]
- Canonico S, Arduini M, Epicoco G, Luzi G, Arena S, et al. (2013) Placenta Previa Percreta: A Case Report of Successful Management via Conservative Surgery. Case Rep Obstet Gynecol 2013: 702067. [Crossref]
- Arulkumaran S, Ng CS, Ingemarsson I, Ratnam SS (1986) Medical treatment of placenta accreta with methotrexate. Acta Obstet Gynecol Scand 65: 285-286. [Crossref]
- Yee YH, Kung FT, Yu PC, Hsu TY, Cheng YF (2008) Successful conservative management of placenta previa totalis and extensive percreta. Taiwan J Obstet Gynecol 47: 431-434. [Crossref]
- Timmermans S, van Hof AC, Duvekot JJ (2007) Conservative management of abnormally invasive placentation. Obstet Gynecol Surv 62: 529-539. [Crossref]
- Morlando M, Sarno L, Napolitano R, Capone A, Tessitore G, et al. (2013) Placenta accreta: incidence and risk factors in an area with a particularly high rate of cesarean section. Acta Obstet Gynecol Scand 92: 457-460. [Crossref]

