resuscitation, oxygen, SpO2, premature infants
Premature infants < 32 weeks’ gestation often require resuscitation during fetal to neonatal transition, which includes administration of supplemental oxygen. Hyperoxia is one of the important generators of reactive oxygen species (ROS) and excess ROS is kept in check by antioxidant defense mechanisms. Premature infants have reduced antioxidant defense mechanisms at birth and hence are at risk for toxic effects of oxygen [1]. Supplemental oxygen in premature infants contributes to development of bronchopulmonary dysplasia (BPD) [2], retinopathy of prematurity [3] and brain injury [4]. The awareness of oxygen toxicity in premature infants has led to strategies such as limiting oxygen exposure at birth, use of antioxidants and administering room air at neonatal resuscitation to reduce free radical formation and to optimize long term outcomes.
Numerous studies have defined the percentiles of oxygen saturation as a function of time from birth in uncompromised babies born at term [5,6]. Neonatal resuscitation guidelines in 2010 for the first time recommended the targeted preductal saturations (SpO2) at resuscitation in the first 10 minutes after birth [7]. The SpO2 guidelines were applicable for both term and premature infants, to be achieved by initiating resuscitation with air or blended oxygen and titrating the oxygen concentration to achieve an SpO2 in the target range using pulse oximetry [7]. Oxygen concentration is increased to100%O2 in a bradycardic (heart rate < 60/min) infant after 90 seconds of resuscitation with a lower concentration of oxygen, until the heart rate recovers to normal. The 2015 NRP guidelines maintained the same saturation targets, recommended against using high O2 concentrations of 65% to 100%O2 and to initiate resuscitation with 21% to 30%O2 [8].
The three studies that administered 30%O2 as one of the oxygen resuscitation groups is summarized in Table 1. Escrig et al was the first to demonstrate that 30%O2 can safely be used to resuscitate premature neonates, which can then be adjusted to infant’s needs reducing the oxygen load on the infant [9]. Vento et al. later demonstrated that 30%O2 for resuscitation, causes less oxidative stress, inflammation and decreases the risk of BPD10. However, a recent study with 30%O2 did not find differences in oxidative stress markers or BPD among the two resuscitation groups [11] (Table 1). This may be related to differences in target saturations among the groups in the first 10 minutes; changes in oxygen load from differences in the high oxygen resuscitated group (90%O2 [10] versus 65%O2 [11]) at resuscitation and finally from varying definitions of BPD at 36 weeks (physiologic or clinical) among the groups [10,11]. Despite using diverse target saturations in the first 10 minutes, all the three studies demonstrate the feasibility of administering 30%O2 at resuscitation in premature infants. The oxygen concentration was titrated upwards to meet SpO2 targets in all studies: to 40% [11], 45%9 or 55%O2 [10] by 5 minutes of birth. The studies indicate that 30%O2 can be used as a starting point to resuscitate a premature infant. The clinical outcomes need to be confirmed, as all these studies used varying target saturations in the first 10 minutes.
Table 1.Studies That Administered 30% O2 as the Initial Gas at Resuscitation in Premature Infants.
| Study |
Methods / Groups |
Results / Conclusions |
Escrig et al. 2008
(≤ 28 wks GA) |
30%O2 (n=19; lox grp) vs. 90%O2 (n=29; hox grp)
Target spo2 – FiO2 adjustment based on HR; spo2 between 85-90 |
FiO2 ↑ stepwise to ̴ 45% in LOX; ↓ to 45%O2 in HOX for a spo2 of around 85% at 5-7 minutes in both groups. No difference in morbidity including BPD and ROP. No deaths < 28 days in both groups.
|
| Vento et al. 2009
(24 – 28 wks GA) |
30%O2 (n=37; lox grp) vs. 90%O2 (n=41; hox grp)
Target spo2 – preductal spo2 of 75% at 5 min and 85% at 10min |
FiO2 ↑ stepwise to ̴ 55% at 5min; lower incidence of BPD & less markers of oxidative stress (urine / GSSG/GSH) in the LOX group. |
| Rook et al. 2014
(<32wks GA) |
30%O2 (n=99; lox grp) vs. 65%O2 (n=94; hox grp)
Target spo2 – FiO2 ↓ for spo2 > 94%; FiO2 ↑ for HR < 100/min before 10 min |
FiO2 ↑ stepwise to ̴ 40% by 7min in LOX; FiO2 ↓ to ~ 40% by 11min in HOX group; No difference in oxidative stress markers or BPD between groups |
Five studies that administered 21%O2 as one of the oxygen resuscitation groups is summarized in Table 2. In the three studies wherein the infants were resuscitated in 21%O2 [12-14], room air failed to maintain the targeted SpO2 and almost all infants required supplemental oxygen. However, resuscitation in 100%O2 resulted in hyperoxic infants with SpO2>95% [13]. Oxygen titration strategy after initial resuscitation with 100%O2 resulted in higher number of infants achieving targeted saturations [13]. The studies imply, that if premature infants were initially resuscitated with 21%O2, then careful attention should be placed to heart rate and SpO2, so that the oxygen can be titrated upwards to achieve saturations as per neonatal resuscitation guidelines.
Table 2. Studies That Administered 21% O2 as the Initial Gas at Resuscitation in Premature Infants.
| Study |
Methods / Groups |
Results / Conclusions |
| Wang et al. 2008
(23-32 wks GA)
|
21%O2 (n=18) vs. 100%O2 (n=23)
Target SpO2 – 100% O2 grp: FiO2 ↓ for spo2 >95% at 5min. 21% grp - ↑ FiO2 for spo2 < 70% at 3min or for spo2 < 85% at 5min (↑ to 50% X 30 secs; no response ↑ to 75% X 30 secs; no response - ↑100% O2) |
All infants resuscitated in the RA received O2 ≤ 3 min; Resuscitation with RA failed to achieve targeted spo2 by 3 minutes; recommend not to use RA for resuscitation of premature neonates. |
Dawson et al. 2009
(<30 weeks GA)
| 21%O2 (n=105) vs. 100%O2 (n=20)
Target SpO2 – 80 to 90%; FiO2 ↓ by 10% if spo2 > 90; FiO2 ↑ for spo2 <70% at 5min or spo2 <90% at 5min + HR < 100 |
97/105 (92%) in the 21%O2 group were subsequently treated with supplemental O2 at 5.05 (4-5.5) min. |
Rabi et al. 2011
(< 32 wks GA)
| 21%O2 (Low O2 strategy; titrate up; n=34); 100%O2 and then wean (mod. O2 strategy) (n=34); 100% O2 (high O2 strategy; n=37);
Target spo2 – FiO2 adjusted 20%O2 q 15 secs to achieve spo2 of 85-92% |
Titrating down from 100% O2 was more effective at maintaining spo2 in the range of 85 – 92 and these infants spent nearly twice as long in the target range as infants resuscitated in 21%O2. |
Kapadia et al. 2013
(24 – 34 wks GA)
| 21%O2 (n=44; lox grp) vs. 100%O2 (n=44; hox grp)
Target SpO2 – 21%O2 grp: NRP guidelines; 100%O2 grp: FiO2 adjusted by 10% to target spo2 of 85-94 |
Lox decreased oxygen load by half; had less oxidative stress at one hour of age and reduced incidence of BPD |
| Kumar et al. 2014
(24-32 wks GA)
|
21%O2 (n=6) vs. 40%O2 (n=7) vs. 100%O2 (n=5)
Target spo2 – First 10 min of birth no change in FiO2 and spo2 were blinded; 10-30 min: spo2< 85% ↑FiO2 and spo2> 95% ↓ FiO2 10% q 60secs |
Defined the natural evolution of spo2 in three different O2 concentrations in the first 10 minutes; 21%O2 had spo2 below the NRP-LL in the first 5 min; 40%O2 mostly within the NRP limits; 100% O2 leads to higher total O2 exposure and systemic oxidant stress |
Studies conducted with 21%O2 as one of the resuscitation group, had the same drawbacks as the studies conducted with 30%O2 resuscitation group. No two resuscitation studies conducted so far (including 21%O2 and 30%O2 resuscitation groups; (Table 1,2) had similar saturation targets in the first 10 minutes after birth. Neonatal resuscitation program (NRP) guidelines recommends that the goal in babies resuscitated at birth, whether born at term or preterm, should be an oxygen saturation value in the interquartile range of preductal saturations measured in healthy term babies following vaginal birth at sea level [7]. The guidelines recommend preductal SpO2 of 60%-65% at 1 min; 65%-70% at 2nd min; 70%-75% at 3rd min; 75%-80% at 4th min and 80%-85% at the end of 5 minutes. The SpO2 values between 5 and 10 minutes of life should be 85% – 95% [7]. These targets should be achieved by initiating resuscitation with a low oxygen concentration (21%O2 – 30%O2) and to titrate the O2 to achieve an SpO2 in the target range using pulse oximetry [8]. The guidelines also recommend against initiating resuscitation of premature infants with high supplementary oxygen concentration (65%O2 - 100%O2) [8]. Limiting oxygen exposure at resuscitation by starting low (21%O2 – 30%O2) and titrating the oxygen concentration upwards to target the above saturation limits in the first ten minutes after birth, not only decreases the oxygen load but may also decrease the risk for BPD [10].
The 2010 guidelines states that the saturation data are extrapolations from term infants [7]. The lack of induction of anti-oxidant enzyme systems soon after birth [15] along with generation of ROS by hyperoxia, makes it highly likely that the suggested SpO2 targets in the first 10 minutes after birth are ‘relatively hyperoxic’ for premature infants. The physiology of oxyhemoglobin curves is different in term and premature infants [16-18]. Maintaining similar saturations in both term and preterm infants may lead to higher oxygen delivery, higher oxidant load and downregulation of hypoxia inducible factor (HIF-1) and vascular endothelial growth factor (VEGF) expression in premature infants. HIF-1 expression is tightly linked to O2 concentration in vivo and hyperoxia or even normoxia in the developing lung rapidly induce HIF degradation and hence VEGF expression [19]. Future studies should address SpO2 ranges in premature infants, particularly in the first 10 minutes after birth. The question is, what is the natural evolution of SpO2 in premature infants resuscitated in room air in the first ten minutes after birth and how do they compare to the limits set by NRP?
This was addressed in a small pilot study in infants < 32 weeks GA, randomized to 21%, 40% or 100%O2 and resuscitated as per 2005 NRP guidelines [20]. Oxygen groups and SpO2 were unmasked at 10 minutes of age and FiO2 adjusted to maintain SpO2 of 85%-95% for the next 20 minutes. The study was stopped at 30% enrollment following publication of the 2010 NRP guidelines, which is a limitation. The mean SpO2 values were 50%, 53% and 69% at 1 min; 77%, 83% and 95% at 5 min and 92%, 92% and 98% at 10 min in 21%O2, 40%O2 & 100%O2 groups respectively (Figure 1) [20]. Resuscitation of premature infants with 100%O2 resulted in SpO2 values above the upper limit of the 2010 NRP guidelines (Figure 1 – red line; open diamonds); 40%O2 resuscitated group had mean SpO2 values below the NRP lower limit in the first five minutes and within the NRP defined SpO2 target range from 6 to 10 minutes (Figure 1 – blue line; open circles); 21%O2 resuscitated group had mean SpO2 values bordering the NRP lower limit in the first five minutes and within the NRP defined SpO2 target range from 6 to 10 minutes (Figure 1 – green line; closed squares). Similarly, there were no differences in SpO2 at 10 and 30 minutes after birth among the groups [20]. Infants in 21%O2, 40%O2 and 100%O2 groups were weaned to 24.8% (±5), 27.9% (±6) and 38% (±20) O2 respectively at 30 minutes of age (Figure 2) [20]. Despite aggressive weaning, FiO2 administered was significantly higher in the 100%O2 group to maintain the target SpO2 until 30 minutes of age; however, there was no significant difference in FiO2 between 40%O2 and 21%O2 groups during the weaning process (Figure 2). The novelty of this study was in administering a fixed concentration of oxygen and blinding the study gas for the first 10 minutes irrespective of the SpO2. This pilot study does demonstrate that resuscitation with 21%O2 is feasible and the evolution of SpO2 in the first 10 minutes following 21%O2 resuscitation are fairly close to NRP saturation limits.
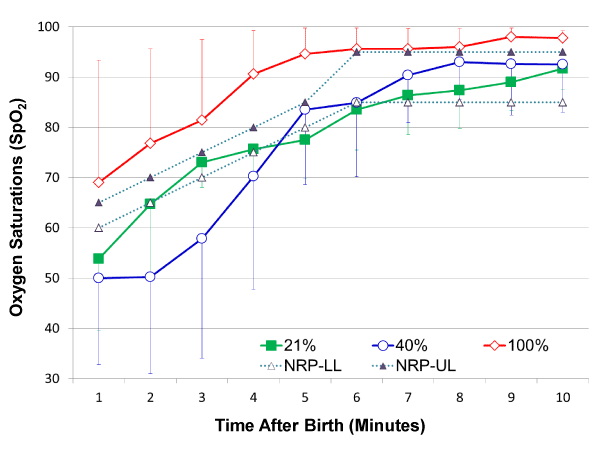
Figure 1. Oxygen saturations (SpO2) in premature infants < 32 weeks GA during the first 10 minutes after birth in the three resuscitated groups. The concentration of oxygen was constant for the first 10 minutes at 21% O2 [-◼-; green]; 40% O2 [-○-; blue] and 100% O2 [-◊-; red] in the three groups. Each time point represents mean ± SD. SpO2 significantly increased over time in the first 10 minutes after birth in all infants (P < 0.0001 mixed model ANOVA). Upper (…▲…) and lower (…Δ…) SpO2 limits (NRP 2010 guidelines) are superimposed on the SpO2 curves of the three O2 resuscitated groups. SpO2 in the 100% O2 group was above NRP-upper limit; resuscitation with 21% or 40% O2 maintained SpO2 within the NRP range from 5 to 10 minutes of life.
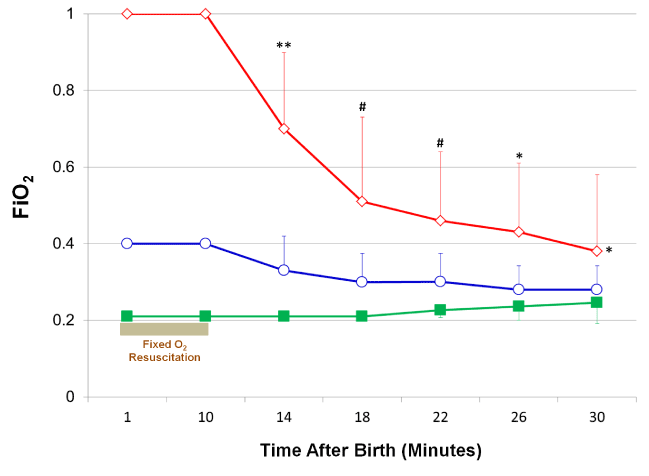
Figure 2. FiO2 in the first 30 minutes after birth in the three oxygen resuscitated groups. Oxygen concentration was constant during resuscitation for the first 10 minutes after birth at 21% O2 [-■-; green]; 40% O2 [-○-; blue] and 100% O2 [-◊-; red] in the three groups. FiO2 was adjusted from 10 to 30 minutes of age for a target SpO2 of 85 – 95. FiO2 was significantly higher in the 100% O2 group to maintain the target SpO2 from 10 to 30 minutes of age (*p < 0.02 versus 40% O2 & 21% O2 groups; Mixed model repeated measure); **p < 0.0001; #p < 0.002; *p < 0.02 versus 40% O2 & 21% O2 groups; ANOVA.
Despite the lack of evidence regarding the appropriate SpO2 ranges at resuscitation in premature infants, particularly in extremely low birth weight infants, studies suggest that using high oxygen concentration at resuscitation is not beneficial [21]. Resuscitation guidelines released last year recommend against using high oxygen concentrations (65%O2 - 100%O2) and to administer 21%O2 – 30%O2 to initiate resuscitation. Administering low oxygen concentrations has not been conclusively proven to improve outcomes. Nonetheless, it decreases the oxygen load exposed in the first 30 minutes after birth contributing to improvement in oxidative stress markers in these infants [10,20].
In a non-asphyxiated premature or term infant administering low concentration of oxygen and titrating it based on saturation limits is prudent at the present time. However, in an asphyxiated infant, whether term or preterm, the oxygen resuscitation guidelines are not clear-cut. It is recommended that oxygen concentration be increased to 100%O2 in a bradycardic / asystolic infant, until heart rate recovers to normal [7]. The key determinant of neonatal resuscitation is more likely to be the heart rate rather than oxygenation. Reperfusion-reoxygenation may lead to additional injury beyond that generated by hypoxia-ischemia alone. Free radicals are produced when myocardium is perfused following ischemia, injuring myocytes & endothelial cells. The release of free radicals, in combination with ischemia deplete intracellular antioxidant activity, rendering myocardium extremely vulnerable to further insult. Weaning and titrating the oxygen concentration to defined saturation targets with pulse oximetry in place is probably the best course at this time. Research into the critical role of heart rate and the myocardial oxygen dynamics at resuscitation, its responses to oxygenation and ultimately on long-term neurodevelopmental outcomes will determine the oxygen concentration after birth.
- Saugstad OD (1990) Oxygen toxicity in the neonatal period. Acta Paediatr Scand 79: 881-892. [Crossref]
- Jobe AH, Ikegami M (1998) Mechanisms initiating lung injury in the preterm. Early Hum Dev 53: 81-94. [Crossref]
- Ashton N, Ward B, Serpell G (1954) Effect of oxygen on developing retinal vessels with particular reference to the problem of retrolental fibroplasia. Br J Ophthalmol 38: 397-432. [Crossref]
- Mickel HS, Vaishnav YN, Kempski O, von Lubitz D, Weiss JF, et al. (1987) Breathing 100% oxygen after global brain ischemia in Mongolian Gerbils results in increased lipid peroxidation and increased mortality. Stroke 18: 426-30. [Crossref]
- Dawson JA, Kamlin CO, Vento M, Wong C, Cole TJ, et al. (2010) Defining the reference range for oxygen saturation for infants after birth. Pediatrics 125: e1340-7. [Crossref]
- Kamlin CO, O'Donnell CP, Davis PG, Morley CJ (2006) Oxygen saturation in healthy infants immediately after birth. J Pediatr148: 585-589. [Crossref]
- Kattwinkel J, Perlman JM, Aziz K, Colby C, Fairchild K, et al. (2010) Neonatal resuscitation: 2010 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care. Pediatrics 126: e1400-1413. [Crossref]
- Perlman JM, Wyllie J, Kattwinkel J, Wyckoff MH, Aziz K, et al. (2015) Part 7: Neonatal Resuscitation: 2015 International Consensus on Cardiopulmonary Resuscitation and Emergency Cardiovascular Care Science With Treatment Recommendations. Circulation 132: S204-241.
- Escrig R, Arruza L, Izquierdo I, Villar G, Saenz P, et al. (2008) Achievement of targeted saturation values in extremely low gestational age neonates resuscitated with low or high oxygen concentrations: a prospective, randomized trial. Pediatrics 121: 875-881. [Crossref]
- Vento M, Moro M, Escrig R, Arruza L, Villar G, et al. (2009) Preterm resuscitation with low oxygen causes less oxidative stress, inflammation, and chronic lung disease. Pediatrics 124: e439-449. [Crossref]
- Rook D, Schierbeek H, Vento M, Vlaardingerbroek H, van der Eijk AC, et al. (2014) Resuscitation of preterm infants with different inspired oxygen fractions. J Pediatr 164: 1322-1326. [Crossref]
- Dawson JA, Kamlin CO, Wong C, te Pas AB, O'Donnell CP, et al. (2009) Oxygen saturation and heart rate during delivery room resuscitation of infants <30 weeks' gestation with air or 100% oxygen. Arch Dis Child Fetal Neonatal Ed 94: F87-91. [Crossref]
- Rabi Y, Singhal N, Nettel-Aguirre A (2011) Room-air versus oxygen administration for resuscitation of preterm infants: the ROAR study. Pediatrics128: e374-381. [Crossref]
- Wang CL, Anderson C, Leone TA, Rich W, Govindaswami B, et al. (2008) Resuscitation of preterm neonates by using room air or 100% oxygen. Pediatrics 121: 1083-1089. [Crossref]
- Frank L, Sosenko IR (1987) Development of lung antioxidant enzyme system in late gestation: possible implications for the prematurely born infant. J Pediatr 110: 9-14. [Crossref]
- Finne PH, Halvorsen S (1972) Regulation of erythropoiesis in the fetus and newborn. Arch Dis Child 47: 683-687. [Crossref]
- Von Kohorn I, Ehrenkranz RA (2009) Anemia in the preterm infant: erythropoietin versus erythrocyte transfusion--it's not that simple. Clin Perinatol 36: 111-123. [Crossref]
- Dudell G, Cornish JD, Bartlett RH (1990) What constitutes adequate oxygenation? Pediatrics 85: 39-41. [Crossref]
- Yu AY, Frid MG, S2021 Copyright OAT. All rights reserval. (1998) Temporal, spatial, and oxygen-regulated expression of hypoxia-inducible factor-1 in the lung. Am J Physiol 275: L818-826. [Crossref]
- Kumar HSV, Carrion V, Wynn KA, Nielsen L, Reynolds AM, et al. (2014) Oxygen resuscitation and oxidative stress biomarkers in premature infants. Research and Reports in Neonatology 4: 91-99.
- Davis PG, Tan A, O'Donnell CP, Schulze A (2004) Resuscitation of newborn infants with 100% oxygen or air: a systematic review and meta-analysis. Lancet 364: 1329-1333. [Crossref]


