Abstract
Introduction: Malposition and displacement of IUDs is an important drawback of all conventional intrauterine devices which rely sole on size for uterine retention.
Areas covered: This expert opinion examines the prevalence, side effects, diagnosis and management of the malplaced or displaced hormonal or copper-releasing IUD. Strategies for avoidance of malposition with IUDs/IUSs are given.
Expert opinion: Malposition and displacement of an IUD should be corrected particularly if associated with side effects such as abnormal bleeding and pain and if optimal protection against pregnancy cannot be guaranteed. Ultrasonography and hysteroscopy are the best and most practical methodologies to diagnose malposition and the possible existence of uterine anomalies. A displaced IUD can be repositioned either blindly, under ultrasonographic guidance or during hysteroscopy if there is no discrepancy between the size of the IUD and the width of the uterine cavity. Frameless IUDs which lack the conventional transverse arm and which rely on different means of uterine retention have the ability to be used in both small and large uterine cavities of varied shapes and appear to be the method of choice particularly in women with very narrow uterine cavities.
Introduction –The problem
Prevalence of interval, post-abortion and postpartum malposition and displacement
The optimal position of a copper or hormone-releasing IUD is in the upper fundal portion of the uterine cavity. Clinical studies have shown that in order to achieve maximal clinical effectiveness location of the device near the fallopian tubes is critical and is the rationale as to why some copper releasing devices have additional copper releasing components on the transverse crossarms. Malposition occurs if the IUD is not positioned in the fundus uteri (Figure 1). This can be caused by anatomical reasons (e.g., a too small uterine cavity, congenital or acquired malformation/distortion of the uterine cavity). In addition if the device is ill fitting, the uterus continuously attempts to expel the foreign body especially during menstruation where uterine forces can be quite severe. Inexperienced providers may release the IUD in the uterine cavity without taking care to make contact with the uppermost fundal wall or failing to confirm proper placement with sonographic or other visualization techniques.
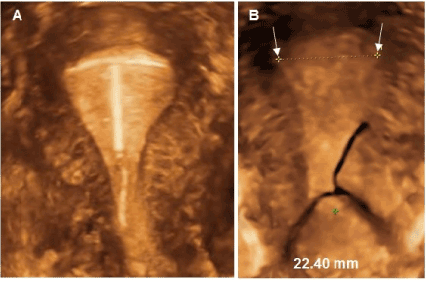
Figure 1: A) 3D ultrasound of T-shaped IUD in sufficiently large endomentrial cavity; B) 3D ultrasound of conventional T-shape in average size uterine cavity with maximum width of 22.40 mm.
The issue of full uterine expulsion of IUD is well appreciated and represents the pinnacle of malpositioning. Fortunately for most women the incidence is typically low (<5%) but of significant impact in the women in which it does occur. In contrast to total expulsion, displacement of an IUD occurs when an IUD which was believed to be appropriately placed in the uterus is found to be still retained within the uterus but malpositioned at follow-up examination. In the past, issues surrounding displacement, embedment and perforations were dismissed because the device was still retained within the uterus. With the advent and routine use of office ultrasound the ability to monitor IUD placement and positioning is greatly enhanced.
Displacement can take many forms: the IUD frame can rotate on its axis or transversely with the retentions arms unfolded or extended in any position. The arms of the displaced IUD often become embedded or can even perforate the uterine wall. There are many degrees of severity and not all patients with displaced and embedded IUDs report symptoms [1]. The leading conventional T-shape devices such as LNG releasing systems and copper devices have 5 year continuation rates, when adjusted for conception requests, of only 50% and 40% respectively bringing into question the long term tolerability of these devices. An IUD that is too large for the uterine cavity will exert pressure on the uterine wall; the uterus will usually react with heavy symmetrical or asymmetrical contractions displacing the IUD and possible embedment. The malpositioning and embedment may actually serve to prevent full IUD expulsion but will likely cause some degree of discomfort to the patient. Partial expulsion is present if the IUD is visible or can be felt at the external cervical os, or if the IUD stem is located in the cervix on ultrasonographic examination.
The precise incidence of malposition is not known but may be higher than what is generally thought due to the more frequent use of 3D ultrasonography. The use of 2D ultrasound affords the physician minimal information given its singular planar view. 3D ultrasound affords a clear assessment of the uterine cavity and simultaneously a full image of the IUD itself. A prospective study, employing 3D ultrasound conducted in 413 women undergoing levonorgestrel (LNG)-IUS (Mirena, Bayer, Germany) insertion or replacement suspected embedment of one or both arms 6 weeks after insertion of the LNG-IUS in more than 50% [2].
If not identified at the first follow-up examination, IUDs can become displaced over time. Braaten et al. studied retrospectively all ultrasound reports from a 5.5-year period and identified 10.4% displaced IUDs, the majority of which were in the lower uterine segment or cervix [3]. Malposition, displacement, partial and total expulsion occurs more frequently after post-abortal insertion of an IUD. A review showed expulsion rates between 0.8% and 17.3% at 8 weeks, up to 5 years after insertion, respectively [4]. It is becoming more apparent that in all women with an IUD, if the device is not expelled, health care providers should assess proper location of the IUD at follow-up or during routine gynecological visits.
Even higher rates of displacement of IUDs are to be expected following second trimester and postpartum IUD insertion [5]. The higher expulsion rates are obviously due to the size difference between the IUD and the uterine cavity, the latter being too large for the IUD. In contrast most interval inserted IUDs that are malpositioned or become displaced are due to a too small cavity eliciting uterine contraction impacting on the IUD.
Is contraceptive failure higher when the IUD is malpositioned or displaced?
IUDs that are malpositioned or have become displaced over time do not necessarily cause a higher risk of pregnancy. However, this depends on the type of the IUD. Copper IUDs are more likely to result in contraceptive failure if they are dislocated than levonorgestrel-releasing IUDs, particularly if the IUD is dislocated in the lower uterine segment or the cervix. Findings from a case control study, in which 318 women with pregnancies with TCu380A IUDs in place were compared with 300 controls also using the TCu380A IUD, revealed a 64% rate of IUD malpositioning among the pregnant cases, compared with an 11% rate among the nonpregnant controls (P<.05) [6]. In contrast, in a 5-year randomized comparative study involving 151 women with an intracervical LNG-IUS compared with 147 women who had the LNG-IUS placed in the fundus there was no difference in failure rates between the two groups [7]. During the first year, two pregnancies occurred in each group. Two of these were ectopic, one in each group. The other two occurred after unnoticed expulsions. Thereafter, no pregnancies occurred. The cumulative gross rate for pregnancy was 1.3 and the Pearl Index at 5 years was 0.425. This study suggests that the LNG-IUS is also effective even if the hormone is not released in the fundus of the uterus. A LNG-IUS prevents pregnancy primarily through the hormonal impact on the cervical glands and the endometrium. As long as the LNG-IUS remains within the cavity it seems that it will provide adequate protection.
Does a malpositioned or displaced IUD cause more side effects?
A study conducted in China in 130 patients with a history of failed IUD removal found that 128 among them were embedded. Half of the patients were asymptomatic and the remaining 50% complained of pain and menstrual disorders [1]. Benacerraf et al.evaluated 167 consecutive patients with an IUD using 3D ultrasonography. Twenty-eight (16.8%) of them had malpositioned IUDs with the arms embedded within the myometrium on coronal view. Of these 28 women, 75% with abnormally located IUDs presented with bleeding and pain complaints compared with 34% of those women with normally positioned IUDs (P=.0001). Twenty of the 21 women with malpositioned IUDs reported improvement in their symptoms after IUD removal. In this study, the type of IUD was not specified. A higher proportion of symptomatic women (e.g., bleeding and pain) were also found in a case-controlled study in which women with malpositioned IUDs were compared with women with normally positioned IUDs. This study included both copper and levonorgestrel-releasing IUD [8].
Another study reported on the 2D and 3D evaluation of 239 women fitted with an IUD. One hundred and eighty had a copper IUD and 59 a levonorgestrel IUD of those who complained of abdominal pain and bleeding. In this group there was no statistical difference between the copper and levonorgestrel IUD regarding malposition, clinical indication for ultrasound examination, or presenting symptomatology. Approximately 75% of the IUDs were properly positioned. In the overall study group, 46% presented with complaints of pain and 14% with complaints of bleeding for which an evaluation was requested. In a significant number of these complaints, 23% and 38%, respectively, the IUD was found to be malpositioned. Bleeding disturbances were found to be more predictive of malposition [9].
Is there an association of malposition and subsequent expulsion of the IUD?
In a Chinese study, 852 women were enrolled to receive a TCu380A, and 860 women received the MLCu375. The aim of the study was to evaluate the relationship between the dimensions of the endometrial cavity and intrauterine device expulsion or removal for displacement [10]. The study demonstrated that when the length of the MLCu375 exceeded the uterine cavity length by 10 mm or more, the expulsion rate increased significantly (P >.01). The study also found that women with a transverse diameter of the uterine cavity in the fundus that is greater than the width of the IUD had a higher risk of expulsion or displacement. This was the case for MLCu375 users with transverse width ≥ 27 mm and for TCu380A users with transverse width ≥ 37 mm, respectively. The inverse relationship between a too large device and a significantly smaller uterine cavity width was not evaluated in this study. The study suggested that the transverse diameter might be a better index than the axial length for studying the association between uterine cavity dimensions and side effects of IUD. The study also suggested that the transverse diameter of the uterine cavity should be considered when deciding which IUD model to use.
IUDs that are too big for the small cavity, if not expelled, may embed resulting in patient discomfort, bleeding and may even advance to perforations [11-14]. Severe uterine distortion (e.g., fibroids) or a congenital malformation (e.g., uterus arcuatus or bicornus) may preclude the proper positioning of an IUD and cause displacement and migration of the IUD in and through the wall of the uterus.
Total expulsion of a conventional framed IUDs occurs in 5–10% of women during the first year of use, with 1–2% per year thereafter. Full IUD expulsion occurs most often during the first months after insertion and is mainly due to spatial incompatibility with a too small uterine cavity. These women usually complain of pain which lasts for more than 3 days after insertion with some continuing for 6 weeks [15]. The uterus is capable of generating 50 N (Newton) of myometrial force or more depending on internal pressure and surface area. If the IUD is not fully expelled, embedment and/or secondary perforation of the IUD may occur. The imbalance between the size of the IUD and that of the uterine cavity can result in the production of asymmetrical uterine forces, which can increase patient discomfort especially while menstruating [16]. Hubacher’s review of copper IUDs revealed that nulliparous women experience higher rates of total expulsion and removals for bleeding and/or pain compared with parous women [17]. However, in a recent study IUD expulsion rates of the Mirena LNG-IUS and TCu380A were not increased in nulliparous women (8.4 per 100 women at 36 months), but 18.8 expulsions per 100 women were observed in adolescents aged 14–19 [18]. Although full expulsions are serious when they do occur, malpositioning and partial embedment likely occurs more frequently and has greater impact on patient comfort and thus continuation rates. Previous studies have found higher rates of expulsion in women with heavy menstrual bleeding and in women with uterine leiomyomas [19]. An association was also found between adenomyosis and IUD malpositioning which may be due to abnormal uterine contractility and heavy menstrual bleeding in these women.
Although the large majority of displacements are in the lower uterine segment of the uterus or in the cervix, migration upwards towards the fundus may occur especially during the first few months after insertion [20,21]. This “fundal-seeking” behavior is caused by upward forces from the myometrial promontories in adequately fitting devices.
The main reason for displacement and expulsion of an IUD postabortion and postpartum is the great disparity between the size of the uterine cavity and that of the IUD. Many examples are given in the literature as was reported in the Chinese study referred to above [5,22]. IUDs are found to be placed lateralized in the uterine cavity, inverted or obliquely causing side effects, embedment or expulsion.
Malpositioned and displaced IUDs cause early removal
To fully understand the implications of shape and size of IUDs one needs to go back several decades and revisit much of the early work on IUD design and development. Research conducted in the US found that there is a great individual variation in the size and shape of the human uterus which is probably greater than variations in the size and shape of the human foot [23]. Some thirty years ago, researchers had shown that uterine cavities vary a great deal in shape, size and adaptation potential contrary to what is implied in numerous medical articles. The length of the IUD may not be its most important dimension, unless it exceeds the length of the cavity and/or the stem of the IUD has a pointed tip. Its width has an even greater influence on its performance and acceptability. Kurz, in Germany measured the transverse diameter of the endometrial cavity at the fundus in 795 parous and nulliparous women [24]. The mean value and standard deviation in nulliparous women were 23.1 ± 3.1 mm. Remarkably, the mean value in parous women, with increasing parity up to parity 3, did not differ very much. In 62 women with parity 2, the mean value and standard deviation were 25.7 ± 3.5 mm. In many women the classic V–shape cavity is absent with many having narrow, cylindrical (or more correctly prolate ellipsoid) uterine cavities. This is why many women, especially nulliparous women, complain and request removal of IUDs that are simply too large. By modifying the T-shaped IUDs (by trimming the ends of the horizontal arm) Kurz was able to achieve significantly higher acceptability and continuation rates, and fewer expulsions in women who experienced discomfort.
The majority of women using conventional IUDs discontinue use long before the end of the lifespan of the IUD [25]. The average use of copper IUDs is only approximately 36 months whilst the lifespan is 10 years for the TCu380A IUD. The 5-year continuation rate can be as low as 40% [26]. For the LNG-IUS (Mirena), removal rates for medical reasons of 35–40% at 5 years have been reported which included malposition and displacement of the LNG-IUS [27,28]. In the CHOICE study, continuation rates at 5 year were 51.7% for the LNG-IUS and 55.9% for the TCu380 IUD, respectively [29]. Many of the reasons for patient discontinuation is a consequence of the uterine incompatibility of conventional T-shape devices.
Management and avoidance of malposition and displacement of IUDs
How to manage a malpositioned or displacement of an IUD
Partially expelled IUDs should be removed and replaced with a suitable IUD but many women will, understandably, be reluctant to try another IUD. Women with cramping pain and bleeding, consulting within hours, days or weeks after insertion of an IUD should be suspected to have a malpositioned IUD. 2D and especially 3D ultrasound examination will usually show the IUD to be in an improper position. The coronal 3D-rendered image will demonstrate the total IUD and its position in the uterine cavity. It is important to know if the cavity width is large enough, or is too large for the IUD. Measuring the width of the uterine cavity with 2D will indicate if the IUD is suitable and if repositioning of the IUD by ultrasound guidance or hysteroscopically has a chance to be successful. In case of gross discrepancy, the IUD should be removed as repositioning may only be temporarily and recur. The patient could be offered a new, more suitable IUD, if available, or immediate initiation of another, highly effective method of contraception. Complaints will usually disappear if the women is fitted with a properly fitting IUD.
We agree that women with a LNG-IUS have a lower risk of unintended pregnancies than women with a copper IUD if the IUD is not properly positioned within the uterine cavity. Asymptomatic patients with displaced LNG-IUS can be managed expectantly; however, the risk of pregnancy is likely to be higher with malpositioned devices. It is wise to verify if the displaced IUD remains in place or tends to become expelled. Some may actually move upwards as a consequence of uterine movement. If however the patient should become symptomatic, she may be offered replacement of a better tolerated/suitable IUD or another effective contraceptive.
Copper IUDs perform best if the copper is high up in the uterine cavity, within millimeters from the uterine fundus. It is recommended to remove all low-load, low-lying (>3 mm from the fundus) copper IUDs as adequate protection cannot be guaranteed. Unfortunately it is impossible to quantify the risk of pregnancy from device malpositioning as this depends on other factors such as age and frequency of intercourse. The health care provider may recommend leaving the IUD in place if all the copper is contained within the uterine cavity and if the patient is asymptomatic and at lower risk. However, if the risk appears higher than the risk of short-acting contraceptive methods, the IUD should be replaced, especially in highly fertile young women.
The management of grossly embedded IUDs is challenging especially if most of the frame of the IUD is embedded or if a portion of the IUD has perforated the uterine wall. In these cases hysteroscopic removal, sometimes combined with laparoscopy may be necessary (Figure 2).
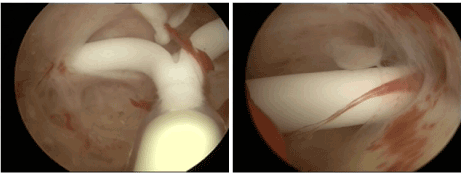
Figure 2: A) Hysteroscopic view of IUD with both arms embedded for 5 mm in the uterine wall; B) Close view of left arm embedded in the uterine wall causing abnormal bleeding and pain. Pain is sometimes only present during sexual intercourse.
How to avoid IUD malposition and displacement
Most current copper T-shaped IUDs and the Mirena LNG-IUS have a transverse arm length of 32 mm. The new smaller version of Mirena LNG-IUS, Jaydess/Skyla, has a transverse arm length of 28 mm. Incompatibility between the IUD and the endometrial cavity will provoke uterine contraction in an attempt to expel the IUD. The impact of uterine forces can be significant if the transverse arm of the IUD/IUD is significantly greater than the fundal transverse diameter [16]. These forces can compress, distort, displace, and expel the IUD, particularly if the IUD is not capable of adaptive changes [30]. In a Finnish study conducted in 165 nulliparous women the mean width of the uterine cavity, measured by ultrasonography, was 24.4 mm, ranging from 13.8 to 35.0 mm. In 2/3 of these young women the transverse width was less than this distance [31]. Without the aid of ultrasonic measurements physicians may be routinely, unknowingly inserting devices of sizes approaching 32 mm in uteri much too small to accommodate them. In other cases, the IUD may be too small for a big uterine cavity [10]. We recommend, therefore assessment of the patient’s uterine cavity size prior to selecting an appropriate IUD [15]. 3D ultrasonography is by far the easiest and cheapest method to also diagnose uterine anomalies or other gynecological conditions which may affect IUD/uterus compatibility. Overall, about 5.5% of uterine anomalies are diagnosed in an unselected population. Arcuate uteri are the most common abnormalities affecting 3.9% of all women. Subseptate or septate uteri have a prevalence of 2.3%. Bicornuate uteri are uncommon (0.4%) and 0.1% of cases present with a unicornuate uterus. The prevalence of uterus didelphys is approximately 0.3% in an unselected population [31,32].
If 3D is not available 2D may very well be appropriate to measure the width of the cavity with precision, especially when performed premenstrually. Gel Instillation Sonography (GIS) is easily and quickly accomplished and can be done any time during the menstrual cycle.
The frameless IUD
The frameless, anchored, copper-releasing and levonorgestrel-releasing intrauterine device has been the subject of considerable technical and clinical research over the past 20 years [33]. The Frameless copper system is currently available in the EU in the form of GyneFix® (Contrel Europe, Belgium). The device lacks a transverse arm, is flexible within the uterine cavity, has a transverse width of <3 mm and is retained via a novel uterine anchoring technique. The insertion technique and the anchor itself has been proven to be a valid concept to suspend active pharmaceutical agents in the interval, postabortion, and postpartum uterus, resulting in improved IUD retention or almost complete absence of expulsion if the procedure was correctly performed [34]. Frameless copper and frameless LNG-IUSs could be the optimal design from a dimensional point of view. The design of the frameless copper IUD, due to its absence of a horizontal crossarm and its flexibility, explains its adaptation to uterine cavities of every size and shape (Figure 3). These characteristics eliminate the ability of the uterus to exert expulsive forces on the frameless IUD devices, in contrast to that seen with the framed T-shape designed IUDs. Consequently, the frameless IUD offers several important advantages as the risk of malposition of the IUD is unlikely unless the uterine cavity is distorted or if the cavity is not accessible. In addition, the correct position of the anchor can be verified by ultrasound (Figure 3). Expulsion or displacement are rare as the anchor securely retains the IUD in the uterine cavity. The design characteristics of the frameless IUD would be attractive as a first choice method for many women, especially for those with a small (e.g. nulliparous women) or too big cavity, and for women who have experienced problems with framed IUDs. The device has been successfully inserted in many women with transverse uterine widths below 10-15 mm. The one-dimensional design of the frameless IUD explains its high acceptability and high continuation of use. An interesting observation is that continuation rates (adjusted for removal for conception request) after the first year with the frameless GyneFix 200 IUD and the frameless LNG-IUS remain high (over 90% at 5 years) due to the low rates of removal for bleeding and pain, whereas these rates reduce by up to 10% each year with conventional T-shaped IUDs yielding continuation rates of only 40 to 50% at 5 years [35].
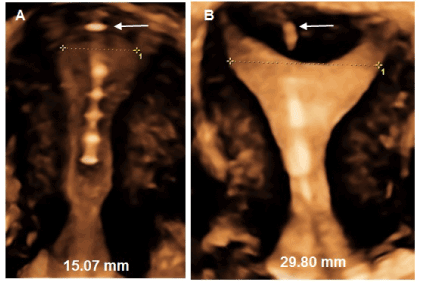
Figure 3: A) 3D ultrasound of the frameless copper IUD in a less than average uterine cavity; B) idem in a greater than average uterine cavity. The correct position of the anchor can be verified by 2D or 3D ultrasound (see arrows).
Conclusion
Malpositioning of IUDs is likely more common than previously believed. Although its impact on effectiveness can never be adequately determined it likely plays a role in overall patient tolerability and long term IUD utilization. The availability of office based 2D and 3D ultrasound systems affords the physician and patient an inexpensive, noninvasive means to monitor IUD placement and uterine compatibility.
Considering the size (width) of uterine cavities in young fertile nulliparous and parous women requesting long-acting contraception, the selection of an appropriate IUD is challenging as most conventional IUDs are too big for many uterine cavities. Studies which measured the width of the uterine cavity ubiquitously show that the uterine cavities are small (narrow) and cannot accommodate a standard size IUD optimally. Clinicians are therefore faced with problems occurring in women with ill-fitted IUDs such as malposition of the IUD at insertion and displacement during use of the IUD.
Alternatives to the conventional T-shape IUD design, such as the intrauterine ball (IUB) and the frameless intrauterine devices hold significant clinical advantages in that they are the only devices currently available which will fit any size uterine cavity. However, improving the IUD-cavity relationship and consequently IUD tolerance may not be enough if expulsion rates are too high, as is currently still the case with the IUB [36].
Displacement and expulsion of IUDs inserted after termination of pregnancy and postpartum can be avoided using the same or a modified anchoring technology.
Expert opinion
Key findings
Intrauterine contraception has become a very important long-acting reversible contraceptive method, as an epidemiological study showed that short-acting methods, such as the pill, the dermal patch, and the vaginal ring, requiring daily attention, had a high failure rate due to incorrect and inconsistent use [37]. A major advantage of long-acting hormonal and non-hormonal methods is that they do not need specific action at the time of coitus. IUDs and intrauterine systems are particularly attractive, as they act locally, avoiding systemic effects. They also have the highest continuation of use of all contraceptives, and thus protect up to 20 times better than pills, patches, and rings to prevent pregnancy [38].
Malposition can be caused by anatomical reasons, lack of skill and inexperience of the provider but the main reason is probably attributable to disparity between the IUD and the uterine cavity. A malpositioned IUD which may originally be located in the upper part of the uterine cavity may become misplaced, usually in the lower uterine segment. Both malpositioned and displaced IUDs will likely embed, causing early discontinuation, if the IUD is not expelled. Misplaced and partially embedded IUDs may still be effective. However, they constitute a risk for unintended pregnancy and should therefore be removed, even if asymptomatic, especially if the IUD is lying in the lower segment of the uterine cavity.
Frameless IUDs have significant potential advantages over framed IUDs, as they fit in cavities of every size and shape (“one size fits all”). As the technique of anchoring is new, health care providers need to learn the correct procedure. A recent publication explains how providers can become proficient to insert and how to check the proper position of the frameless IUD after insertion and at follow-up [39]. Due to the absence of a plastic frame, measuring the size of the uterine cavity is unnecessary which is cost-saving.
The challenge
A T-shaped IUD should be selected based on the prior knowledge of the transverse width of the uterine cavity which matches best the measured distance. IUDs that adapt to the width of the uterine cavity without distorting the cavity could also solve problems of incompatibility. Frameless IUDs hold promise as no considerations of uterine width or shape is necessary. Clinical evidence suggests that interval, post-abortal and postpartum IUD displacement and expulsion can be minimized by anchoring the IUD to the fundus of the uterus.
Declaration of interest
Dirk Wildemeersch, MD, PhD, has been involved in the optimization of new, innovative, drug delivery systems for use in the uterus. He is currently advisor in devising new concepts in controlled release for contraception, gynecological treatment, and prevention of infectious diseases. Thomas Hasskamp, Norman Goldstuck: nil.
References:
2021 Copyright OAT. All rights reserv
- Chen X, Guuo Q, Wang W, Huang L (2015) Three-dimensional ultrasonography versus two dimensional ultrasonography for the diagnosis of intrauterine device malposition. Int J Obstet Gynecol 128: 157–159. [Crossref]
- Van Schoubroeck D, Van den Bosch T, Ameye L, Veldman J, Hindryckx A, et al. (2013) Pain and bleeding pattern related to levonorgestrel intrauterine system (LNG-IUS) insertion. Eur J Obstet Gynecol Reprod Biol 171: 154-156. [Crossref]
- Braaten K, Goldberg AB (2012) Malpositioned IUDs: When you should intervene (and when you should not). OBG Management 24: 39–46.
- Wildemeersch D, Goldstuck ND (2015) Expulsion and continuation rates after postabortion insertion of framed IUDs versus frameless IUDs – review of the literature. J Contracept 6: 87–94.
- Wildemeersch D, Goldstuck ND, Hasskamp T (2016) Current status of frameless anchored IUD for immediate intracesarean insertion. Dev Period Med 20: 7–15.
- Inal MM, Ertopçu K, Ozelmas I (2005) The evaluation of 318 intrauterine pregnancy cases with an intrauterine device. Eur J Contracept Reprod Health Care 10: 266-271. [Crossref]
- Pakarinen P, Luukkainen T (2005) Five years' experience with a small intracervical/intrauterine levonorgestrel-releasing device. Contraception 72: 342-345. [Crossref]
- Braaten KP, Benson CB, Maurer R, Goldberg AB (2011) Malpositioned intrauterine contraceptive devices: risk factors, outcomes, and future pregnancies. Obstet Gynecol 118: 1014-1020. [Crossref]
- Moschos E, Twickler DM (2011) Does the type of intrauterine device affect conspicuity on 2D and 3D ultrasound? AJR Am J Roentgenol 196: 1439-1443. [Crossref]
- Liang H, Li L, Yuan W, Zou Y, Gao ES, et al. (2014) Dimensions of the endometrial cavity and intrauterine device expulsion or removal for displacement: a nested case-control study. BJOG 121: 997-1004. [Crossref]
- Teal SB, Sheeder J (2012) IUD use in adolescent mothers: retention, failure and reasons for discontinuation. Contraception 85: 270–274. [Crossref]
- Rasheed SM, Abdelmonem AM (2011) Complications among adolescents using copper intrauterine contraceptive devices. Int J Gynaecol Obstet 115: 269–272. [Crossref]
- Kaislasuo J, Suhonen S, Gissler M, Lähteenmäki P, Heikinheimo O (2013) Uterine perforation caused by intrauterine devices: clinical course and treatment. Hum Reprod 28: 1546-1551. [Crossref]
- Shipp TD, Bromley B, Benacerraf BR (2010) The width of the uterine cavity is narrower in patients with an embedded intrauterine device (IUD) compared to a normally positioned IUD. J Ultrasound Med 29: 1453-1456. [Crossref]
- Wildemeersch D, Hasskamp T, Goldstuck N (2016) Side effects of intrauterine devices are often related to disproportion with the endometrial cavity-is there a role for pre-insertion ultrasound? Eur J Obstet Gynecol Reprod Biol 201: 215-217. [Crossref]
- Goldstuck ND, Wildemeersch D (2014) Role of uterine forces in intrauterine device embedment, perforation, and expulsion. Int J Womens Health 6: 735-744. [Crossref]
- Hubacher D (2007) Copper intrauterine device use by nulliparous women: review of side effects. Contraception 75: S8-11. [Crossref]
- Madden T, McNicholas C, Zhao Q, Secura GM, Eisenberg DL, et al. (2014) Association of age and parity with intrauterine device expulsion. Obstet Gynecol 124: 718-726. [Crossref]
- Zhang J, Feldblum PJ, Chi IC, Farr MG (1992) Risk factors for copper T IUD expulsion: an epidemiologic analysis. Contraception 46: 427-433. [Crossref]
- Morales-Roselló J (2005) Spontaneous upward movement of lowly placed T-shaped IUDs. Contraception 72: 430-431. [Crossref]
- Faundes D, Bahamondes L, Faundes A, Petta CA (1998) T-shaped IUD move vertically with endometrial growth and involution during the menstrual cycle. Contraception 57: 413–415. [Crossref]
- Gupta S, Shashiprateek, Sinha R, Shyamsunder S, Mittal MK (2014) Association of the position of the copper T380A as determined by ultrasonography following its insertion in the immediate postpartum period with subsequent complications: an observational study. J Obstet Gynecol India 64: 349–353. [Crossref]
- Hasson HM (1980) Uterine geometry and IUD performance. In: Hafez ESE, van Os WAA, eds. Medicated intrauterine devices: Physiological and clinical aspects. Boston: Martinus Nijhoff Publishers 11–21.
- Kurz KH (1984) Cavimeter uterine measurements and IUD clinical correlation. In: Zatuchni GI, Goldsmith A, Sciarra JJ, eds. Intrauterine contraception: Advances and future prospects. Philadelphia: Harper & Row 142–162.
- Moreau C, Trussell J, Rodriguez G, Bajos N, Bouyer J (2007) Contraceptive failure rates in France: results from a population-based survey. Hum Reprod 22: 2422-2427. [Crossref]
- Sivin I, Greenslade F, Schmidt F, et al. The copper T 380 intrauterine device. A summary of scientific data. New York (NY): The Population Council; 1992. ISBN 0-87834-064-5.
- Sivin I, El Mahgoub S, McCarthy T (1990) Long-term contraception with the levonorgestrel 20 mcg/day (LNg 20) and the copper T380Ag intrauterine devices: a five-year randomized study. Contraception 42: 361–378.
- Andersson K, Odlind V, Rybo G (1994) Levonorgestrel-releasing and copper-releasing (Nova T) IUDs during five years of use: a randomized comparative trial. Contraception 49: 56–62. [Crossref]
- Diedrich JT, Madden T, Zhao Q, Peipert JF (2015) Long-term utilization and continuation of intrauterine devices. Am J Obstet Gynecol 213: 822. [Crossref]
- Wildemeersch D, Hasskamp T, Goldstuck N (2015) Intrauterine devices that do not fit well cause side effects, become embedded, or are expelled and can even perforate the uterine wall. J Minim Invasive Gynecol 22: 309-310. [Crossref]
- Chan YY, Jayaprakasan K, Zamora J, Thornton JG, Raine-Fenning N, et al. (2011) The prevalence of congenital uterine anomalies in unselected and high-risk populations: a systematic review. Hum Reprod Update 17: 761-771. [Crossref]
- Jurkovic D1, Gruboeck K, Tailor A, Nicolaides KH (1997) Ultrasound screening for congenital uterine anomalies. Br J Obstet Gynaecol 104: 1320-1321. [Crossref]
- Wildemeersch D, Pett A, Jandi S, Hasskamp T, Rowe P, et al. (2013) Precision intrauterine contraception may significantly increase continuation of use: a review of long-term clinical experience with frameless copper-releasing intrauterine contraception devices. Int J Women’s Health 5: 215–225. [Crossref]
- Wildemeersch D, Goldstuck N (2015) Expulsion and continuation rates after postabortion insertion of framed IUDs versus frameless IUDs – review of the literature. J Contracept 6 87–94.
- Wildemeersch D, Jandi S, Pett A, Nolte K, Hasskamp T, et al. (2014) Use of frameless intrauterine devices and systems in young nulliparous and adolescent women: results of a multicenter study. Int J Womens Health 6: 727–734. [Crossref]
- Wiebe E, Trussell J (2016) Discontinuation rates and acceptability during 1year of using the intrauterine ball (the SCu380A). Contraception 93: 364-366. [Crossref]
- Trussell J (2011) Contraceptive failure in the United States. Contraception 83: 397-404. [Crossref]
- Winner B, Peipert JF, Zhao Q, Buckel C, Madden T, et al. (2012) Effectiveness of long-acting reversible contraception. N Engl J Med 366: 1998-2007. [Crossref]
- Wildemeersch D, Hasskamp T (2016) How to become Proficient with Insertion of Frameless IUDs? Obstet Gynecol Int J 4: 2–9.



