Abstract
Missed hollow viscus injuries increase the mortality rate in trauma patients specifically in polytraumatized patients. A 18 years old young male patient suffered a high velocity (ca.50 km/h, 31mi/h) car crash with deployment of the airbags. The hemodynamically stable patient did not suffer any intracranial injuries but complained about severe pain in the lower abdomen. The primary survey was misleading. CT demonstrated minimal accumulation of free intraabdominal fluid. Due to persistently severe pain, the patient was taken to the operating room for diagnostic laparoscopy followed by exploratory laparotomy. Jejunal perforation was detected and was surgically treated.
In conclusion, following blunt abdominal trauma, operative management is even recommended in patients who present with significant abdominal pain but minimal or absence of pathological findings in abdominal CT-scan imaging.
Key words
abdominal injuries, small intestine perforation, computed tomography
Introduction
Blunt abdominal trauma may injure all sections of the gastro- intestinal tract, and lesions may vary in their clinical presentation. More than half of all blunt intestinal injuries are found in the small intestinal, with equal involvement of the jejunum and ileum. The second most frequent location of injury is the colon. Colonic injuries are predominately localized in the descending colon [1]. In trauma patients, missed hollow viscus injuries result in extravasation of bowel content, and cause abdominal inflammation and early sepsis. If missed, septic complications may even develop into life- threatening septic shock. The presented case is nothing tremendly new, however, should be ever kept in mind.
Case presentation
An 18 year- old male patient, who suffered blunt abdominal trauma, was admitted to the trauma bay. The Glasgow Coma Scale was 15, and the patient complained about severe pain in the lower abdomen. The patient always remained hemodynamically stable. The delay until admission to the emergency department (ED) was 47 minutes. The primary survey demonstrated skin bruises over the pelvis, and pain in the lower abdomen (Figure 1). The Focused Assessment with Sonography for Trauma (FAST) did not show any free intraabdominal fluid or lacerations in parenchymatous organs. The laboratory parameters and vital signs are presnten in Table 1. Immediately after the FAST, whole body CT- scan including liver and spleen as well as arterial and venous phase was performed showing discrete accumulation of free fluid in the Douglas space but no sign of pneumoperitoneum (Figure 2). Initially, non- operative management and close monitoring was applied. However, repeated clinical examinations revealed persistent abdominal tenderness and guarding, and therefore, diagnostic laparoscopy was indicated and performed.
Table 1. Depicted are the laboratory and vital parameters at admission in the ED in an alphabetical order. Parameters under or over-exceeding the normal laboratory range are highlighted in bold. INR: International Normalized Ratio.
Parameters |
Value at admission |
Blood pressure |
147/75 mmHg |
Creatinine |
90 µM |
Glucose |
6.7 mM |
INR |
1.1 |
Lactate |
0.8 mM |
Pancreatic amylase |
49 U/L |
Potassium |
3.8 mM |
Pulse rate |
110 bpm |
Respiratory rate |
14 /min |
Sodium |
137 mM |
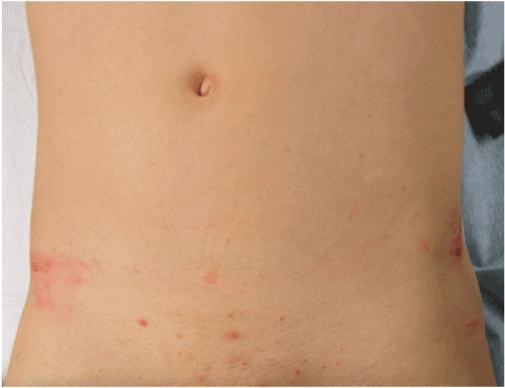
Figure 1. The primary survey revealed skin bruises over the pelvis (asterisk).
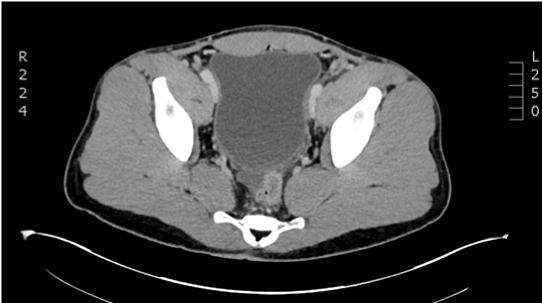
Figure 2. Abdominal CT-scan immediately following admission to the trauma bay demonstrated minimal fluid accumulation in the Douglas space (asterisk).
Immediately after the FAST, whole body CT- scan including liver and spleen as well as arterial and venous phase was performed showing discrete accumulation of free fluid in the Douglas space but no sign of pneumoperitoneum (Figure 2). Initially, non- operative management and close monitoring was applied. However, repeated clinical examinations revealed persistent abdominal tenderness and guarding, and therefore, diagnostic laparoscopy was indicated and performed.
Laparoscopy revealed turbid fluid in the Morrison pouch (Figure 3), and it was decided to convert to open exploration using midline laparotomy. A small rupture of the Jejunum approximately 1 m aboral to the ligament of Treitz (Figure 4) was detected. Therapeutically, segmental resection followed by end-to end anastomosis to restore intestinal continuity was performed. In addition, it was decided to postpone definite abdominal closure and to apply temporary laparostomy using negative pressure sealing. A second- look procedure including irrigation of the abdominal cavity was performed after two days, followed by definite abdominal closure after 4 days.
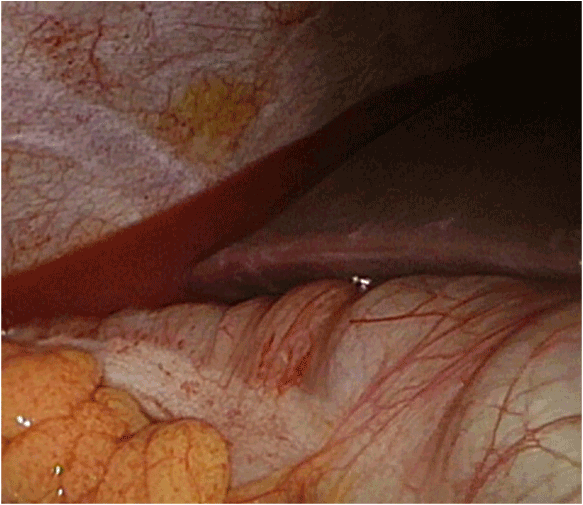
Figure 3. Laparoscopic view to the Morrison pouch. Turbid bloody fluid is observed in the Morrison pouch (asterisk). Liver at upper right and the right colonic flexure at the bottom.
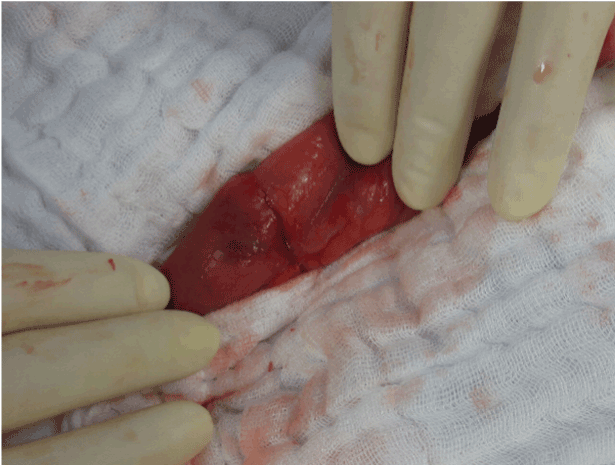
Figure 4. Intraoperative view of the jejunal perforation approximately 1 m aborally to the ligament of Treitz.
Discussion
This young patient suffering isolated jejunal perforation due to bland abdominal trauma admitted in hemodynamically stable conditions was on the edge of decision to operate or not to operate. The indication to perform laparoscopic surgery was made due to persistent abdominal pain shedding a light on the complications in consciousness less patients. In patients treated for blunt abdominal trauma, hollow organ and mesenteric injuries are found in 3–15% [2,3]. These injuries represent 16% of all cases in blunt abdominal trauma, and are the third most common abdominal injuries after liver and splenic injuries [4]. Accurate diagnosis of intestinal lesions can be difficult and thus, may cause detrimental therapeutic delay. Lawson et al., reviewed trauma patients for delayed diagnosis and observed that bowel injuries were most commonly missed, and thus concluded, that blunt abdominal trauma had to be addressed with high suspicion for adverse consequences [5]. The presence of abdominal skin bruising may be indicative for visceral organ injuries. Several studies have pointed out, that bruising in a seat belt pattern was associated with intra-abdominal injury in 20–60% of cases [6]. The risk of perforated bowel injury increased by a 2.4 factor whenever seat belt bruising was detected [7]. In contrast, isolated findings of bruising without associated abdominal pain or guarding, was associated with low risk of intra-abdominal injury [8]. Thorough physical examination should repeatedly assess abdominal tenderness and guarding, but these signs are non-specific and may be observed with all abdominal injuries. The presence of other radiological lesions associated with the seatbelt syndrome (e.g. thoracic and or lumbar spinal fractures, as well as abdominal aortic lesions) are very suspicious and may be indicative for intestinal injuries. For diagnostic studies, FAST (Focused Assessment with Sonography for Trauma) may be utilized in unstable patients. However, FAST offers very limited sensitivity, and thus is not be beneficial in detecting intestinal and mesenteric injuries [9]. For hemodynamically stable trauma patients, CT is the most effective imaging study for detection of intestinal and mesenteric lesion, and the radiologic signs are well defined (Figure 3) [10].
However, some injuries that require prompt surgical intervention may present without clear pathological imaging findings. Specifically, lesions of the small intestine (jejunum, ileum, duodenum) may not present the typical signs of intestinal wall injury including thickening of the bowel wall, fluid extravasation or free abdominal air. In contrast, detection of colonic ruptures may be more obvious, since theses lesions regularly present with free abdominal air. The choice of treatment is difficult, with two opposing strategies: diagnostic laparotomy versus non- operative management. Sometimes, the clinical presentation and radiological pattern of intestinal or mesenteric injury is straight forward, leading to treatment without delay. In cases of doubt, whenever CT imaging studies are not conclusive and clinical symptoms persist or aggravate, it is recommended to systematically perform surgical exploration for the least suspicion of intestinal or mesenteric injury, and thus, as a general advice, non- operative management cannot be recommended in these patients. Patient prognosis is dependent on early detection and the time interval between the time of injury and the time of therapeutic intervention. Many studies have demonstrated direct relation between delay time and post-operative morbidity with a threshold varying from 5 to 8 hours [11,12]. In the study with the largest number of patients, Fakhry et al. reported that mortality for isolated trauma of the intestine significantly increased when the delay interval exceeded 8 hours [13]. The importance of this case report lies in the divergent findings between clinics and CT, assuming a blunt abdominal trauma in combination with cranio-cerebral trauma (the multiple injured patient) the clinical findings could not be evaluated in such a case and the perforation might be missed leading to mentioned complications. However, the limitations in this case lie in patient’s excellent clinical response, if the patient would have been unconscious the injury might been missed.
Conclusion
Be suspicious of intestinal perforation in male patients even when only very little free fluid is present on abdominal CT and set the operative indication generously especially in patients with additive cranio-cerebral injuries. There might still be the indication for deep peritoneal lavage in such trauma cases in male and in female patients with persistent abdominal pain.
References
- Swaid F, Peleg K, A2021 Copyright OAT. All rights reserv2014) Concomitant hollow viscus injuries in patients with blunt hepatic and splenic injuries: An analysis of a National Trauma Registry database. Injury 45: 1409-1412. [Crossref]
- Watts DD, Fakhry SM, EAST Multi-Institutional Hollow Viscus Injury Research Group (2003) Incidence of hollow viscus injury in blunt trauma: an analysis from 275,557 trauma admissions from the East multi-institutional trial. J Trauma 54: 289-294. [Crossref]
- Bruscagin V, Coimbra R, Rasslan S, Abrantes WL, Souza HP, et al., (2001) Blunt gastric injury. A multicentre experience. Injury 32: 761-764. [Crossref]
- Stuhlfaut JW, Lucey BC, Varghese JC, Soto JA (2006) Blunt abdominal trauma: utility of 5-minute delayed CT with a reduced radiation dose. Radiology 238: 473-479. [Crossref]
- Lawson CM, Daley BJ, Ormsby CB, Enderson B (2011) Missed injuries in the era of the trauma scan. J Trauma 70: 452-456. [Crossref]
- Borgialli DA, Ellison AM, Ehrlich P, Bonsu B, Menaker J, et al., (2014) Association between the seat belt sign and intra-abdominal injuries in children with blunt torso trauma in motor vehicle collisions. Acad Emerg Med 21: 1240-1248. [Crossref]
- Fakhry SM, Watts DD, Luchette FA, EAST Multi-Institutional Hollow Viscus Injury Research Group (2003) Current diagnostic approaches lack sensitivity in the diagnosis of perforated blunt small bowel injury: analysis from 275,557 trauma admissions from the EAST multi-institutional HVI trial. J Trauma 54: 295-306. [Crossref]
- Sokolove PE, Kuppermann N, Holmes JF (2005) Association between the “seat belt sign” and intra-abdominal injury in children with blunt torso trauma. Acad Emerg Med 12: 808-813. [Crossref]
- Nural MS, Yardan T, Güven H, Baydin A, Bayrak IK, et al., (2005) Diagnostic value of ultrasonography in the evaluation of blunt abdominal trauma. Diagn Interv Radiol 11: 41-44. [Crossref]
- Brofman N, Atri M, Hanson JM, Grinblat L, Chughtai T, et al., (2006) Evaluation of bowel and mesenteric blunt trauma with multidetector CT. Radiographics 26: 1119-1131. [Crossref]
- Malinoski DJ, Patel MS, Yakar DO, Green D, Qureshi F, et al., (2010) A diagnostic delay of 5 hours increases the risk of death after blunt hollow viscus injury. J Trauma 69: 84-87. [Crossref]
- Faria GR, Almeida AB, Moreira H, Barbosa E, Correia-da-Silva P, et al., (2012) Prognostic factors for traumatic bowel injuries: killing time. World J Surg 36: 807-812. [Crossref]
- Fakhry SM, Brownstein M, Watts DD, Baker CC, Oller D (2000) Relatively short diagnostic delays (< 8 hours) produce morbidity and mortality in blunt small bowel injury: an analysis of time to operative intervention in 198 patients from a multicenter experience. J Trauma 48: 408-414. [Crossref]




