A 51-year-old man was referred to us with a diagnosis of chronic hepatitis, secondary to hepatitis C infection after receiving blood transfusion at splenectomy for traffic accident at 16-year age. He had undergone ultrasonographic examination, and a homogeneous and slight hyperechoic mass, measuring 18 × 20 mm in diameter, was detected in liver segment IV (Figure 1). Contrast-enhanced computed tomography (CT) scan showing a marked hyper-attenuation of the lesion during the hepatic arterial phase and a fast wash-out during the venous phase, mimicking hepatocellular carcinoma (HCC) (Figure 2).
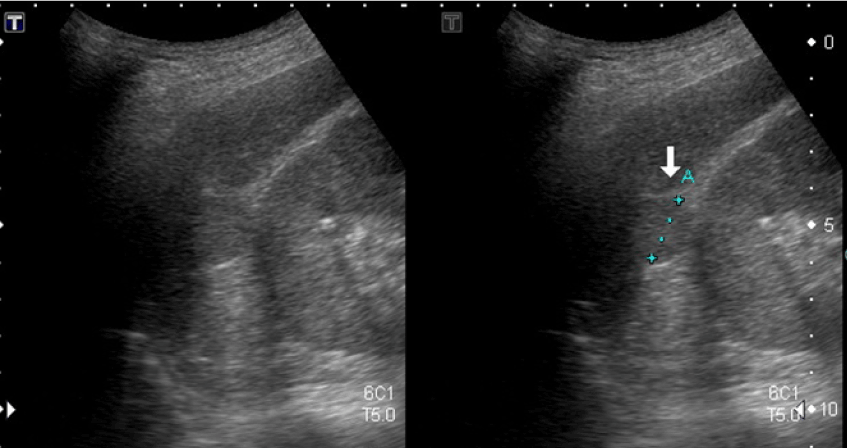
Figure 1. Abdominal ultrasonography revealed a slight hyperechoic homogeneous mass 18x20 mm in size in segment IV of the liver.
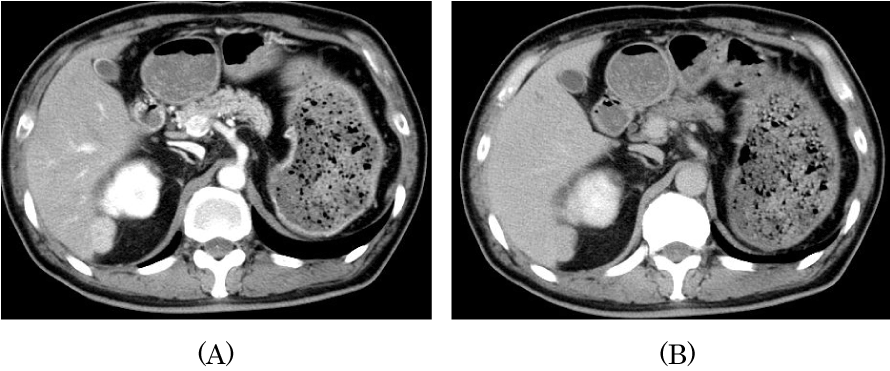
Figure 2. (A) Computed tomography scan showing a hyper-attenuation of the lesion during the hepatic arterial phase. (B) Computed tomography scan showing a wash-out during the venous phase.
2021 Copyright OAT. All rights reserv
There are no typical radiological features of intrahepatic splenosis and it is usually difficult to distinguish this condition from other liver tumors. We performed an echo-guided tumor biopsy. Histopathology showed a splenic tissue containing lymphocytes and myeloid cells in sinusoids surrounded by fibrous capsule (Figure 3). We confirmed the diagnosis of hepatic splenosis.
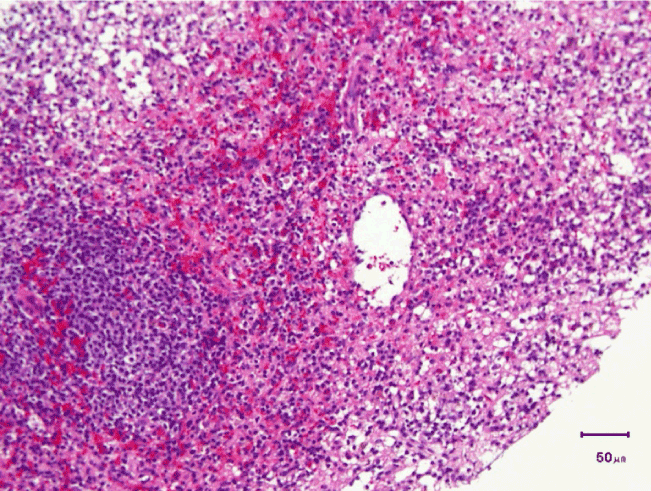
Figure 3. Histopathology showed a splenic tissue containing lymphocytes and myeloid cells in sinusoids surrounded by fibrous capsule.
Splenosis was firstly reported by Buchbinder and Lipkoff in 1939 [1]. Although it is believed to occur in up to 67% of cases with splenic trauma the true incidence cannot be estimated as it is usually an incidental finding during surgical exploration or autopsy [2]. Splenosis is thought to be uncommon, but the incidence is probably underreported since the majority of patients are asymptomatic. Distinguishing the etiology of hepatic nodular lesions is important because it significantly alters therapeutic procedures.
Typical imaging modalities such as US, CT or MRI will not differentiate splenosis from other entities and a histologic specimen needs to be obtained to reach definitive diagnosis.
In most cases, correct diagnosis was only possible on histological examination after a laparotomy and open liver resection [3,4].
A missed diagnosis of hepatic splenosis can have a significant negative impact on patient's management [5].
We performed tumor biopsy and diagnosed hepatic splenosis mimicking hepatocellular carcinoma in a patient with chronic hepatitis C.
In conclusion, considering patients past history of splenectomy or splenic trauma should add splenosis to the list of possible differential diagnosis to avoid unnecessary surgical intervention.
All authors have contributed significantly, and that all authors are in agreement with the content of the manuscript. The study was approved by the local ethics committee in accordance with the 1975 Declaration of Helsinki, and the authors declare that they do not have any current financial arrangements or affiliations with any organization that may have a direct interest in their work.
- Buchbinder JH, Lipkoff CJ (1939) Splenosis: multiple peritoneal splenic implant following abdominal injury. Surgery 6: 927-930.
- Vuysere SD, Steenbergen WV, Aerts R, Hauwaert HV, Beckevoort DV, et al. (2000) Intrahepatic splenosis: imaging features. Abdom Imaging 25: 187-189. [Crossref]
- Lee JB, Ryu KW, Song TJ, Suh SO, Kim YC, et al. (2002) Hepatic splenosis diagnosed as hepatocellular carcinoma: report of a case. Surg Today 32: 180-182. [Crossref]
- Khosravi MR, Margulies DR, Alsabeh R, Nissen N, Phillips EH, et al. (2004) Consider the diagnosis of splenosis for soft tissue masses long after any splenic injury. Am Surg 70: 967-970. [Crossref]
- Di Costanzo GG, Picciotto FP, Marsilia GM, Ascione A (2004) Hepatic splenosis misinterpreted as hepatocellular carcinoma in cirrhotic patients referred for liver transplantation: report of two cases. Liver Transpl 10: 706-709. [Crossref]



