Background
According to the National Bureau of Economics Research, Canada spends far less of its gross domestic product on health care (10.4% versus 16% in the U.S.) yet performs better than the U.S. on infant mortality rate and life expectancy [1]. Lowering healthcare utilization and costs are important goals for primary care and subspecialty providers. In March 2012, the Agency for Healthcare Research and Quality (AHRQ) published a meta-analysis of the utility of lab testing in musculoskeletal pain evaluation and screening of rheumatic diseases in children and adolescents2. The review analyzed 28 pediatric articles and concluded that current evidence does not support the use of antinuclear antibody (ANA) and rheumatoid factor (RF) testing as a screening for rheumatic diseases in the primary pediatric care setting. Despite this and other articles with similar recommendations, it seems that inappropriate use of these labs continues to be a persistent problem in pediatrics [2-4]. Referring pediatric patients to rheumatology for positive labs with a normal exam and complaints of intermittent joint pain generates multiple unnecessary referrals that prolong wait times for new patients with active pathology. Additionally, new patients are seen with severe joint damage and contractures that are not referred earlier as their “arthritis labs are negative.” This practice may waste a significant amount of money annually and contributes to higher healthcare utilization [5].
In order to quantify this problem, we choose to review the healthcare utilization and costs for children and adolescents with juvenile idiopathic arthritis (JIA) in the Texas Children’s Hospital (TCH) Health Plan during January 1 to December 31, 2011. JIA is the most common rheumatic disease of childhood and it is also one of the more frequent chronic illnesses in childhood that cause short and long term disability [6,8]. JIA is defined in children that are younger than 16 years old and have persistent joint pain and swelling for at least 6 weeks [6]. A positive ANA has long been associated with several inflammatory rheumatic diseases [5,7]. Although it is included among classification criteria for diseases like systemic lupus erythromatosus and other inflammatory connective tissue diseases, it is not specific to these conditions [5,7]. A positive ANA in absence of arthritis, malar rash, or cytopenias is of no clinical significance [5,7]. In patients with JIA a positive ANA can be found in about 18-77% of patients [1,6]. However, after a patient has been diagnosed by a pediatric rheumatologist with JIA, this test is used to predict patients’ risk for uveitis and determines the interval for their ophthalmologic evaluations [1,6].
JIA shares many clinical features and ICD-9 code with adult rheumatoid arthritis. They even share the same ICD-9 code. In adults, a positive test for RF is 97% specific and has a predictive value for 80%7. Yet JIA pathophysiology, presentation, and lab assessment is not identical to its adult counterpart. In children, a positive RF is found in only about 5-10% of children clinically diagnosed with polyarticular disease [1,3,6]. Taking this into consideration, a primary care provider should refer a child or adolescent for evaluation if he or she meets the above criteria and infection and malignancy have been excluded [5,6]. Lab studies are only confirmatory in JIA and have no place in screening schema. We hypothesized that lab utilization practices seen in outpatient rheumatology clinic would correlate with significant annual cost for an individual health plan.
Methods
We reviewed administrative claims data from January 1 to December 31, 2011 for TCH Health Plan members’ ages 0-17 years old to identify unique members with the arthritis-related ICD-9 codes (Table 1) and CPT codes for ANA (86038 and 86039) and RF (86431). The TCH Health Plan is a health maintenance organization (HMO) that serves exclusively children with Medicaid or the Children’s Health Insurance Program (CHIP). This was done to describe the use of these labs across the TCH Health Plan. Data capture for unique members with diagnosis code 714.xx (JIA diagnosis code) was collected to include other health service data, such as: service provider specialty, radiology and laboratory services, and cost for ANA and RF. We set out to identify coding patterns for primary care providers when using the ICD-9 code 714.xx for the first and second diagnoses. Available charts for members with JIA diagnosis code were reviewed by a pediatric rheumatologist to assess for correct use of the code and appropriateness of referral. This project was approved by the Baylor College of Medicine IRB.
Table 1. Arthritis-related codes
ICD-9 code |
Description |
696.xx |
Psoriatic arthropathy |
713.xx |
Arthropathy |
714.xx |
Inflammatory arthropathy, juvenile idiopathic arthritis, rheumatoid arthritis |
715.xx |
Osteoarthrosis |
716.xx |
Kaschin-Beck disease, osteoarthropathy |
720.xx |
Unspecified inflammatory spondylopathy, ankylosing spondylopathy |
737.xx |
Synovitis and tenosynovitis |
726.xx |
Rheumatism unspecified |
Results
Claims analyses for 1,574 members with rheumatologic diagnosis codes were identified and reviewed. A multitude of patients had multiple autoimmune lab tests performed and some members had labs repeated up to five times (i.e. a member with intermittent knee swelling and pain that resulted in a diagnoses of torn a meniscus after seeing multiple providers including primary care, ER, and orthopedic providers) (Table 2). Fifty nine percent of the ANA and 76% of the RF test were ordered by primary care physicians.
Table 2. Utilization rates of ANA and RF testing among pediatric health plan members Jan 1- Dec 31 2011 by associated diagnosis code
|
Test |
Associated Dx Code |
ANA claims % of test ordered |
RF claims % of test ordered |
Non Arthritis |
1,202 |
89% |
672 |
85% |
Arthritis |
155 |
11% |
116 |
15% |
714.xx |
67 |
43% |
47 |
41% |
Other arthritis |
88 |
57% |
69 |
59% |
TOTALS |
1357 |
100% |
788 |
100% |
Taking in consideration the total annual costs for the insurance plan laboratory evaluation, this gives an average cost of $313 for each ANA claim and $98 for each RF claim (Table 3).
Table 3. Total claims and costs for ANA and RF testing among Pediatric Health Plan Members Jan 1-Dec 31 2011 by associated diagnosis code
Unique Members |
ANA |
RF |
Associated Dx Code |
n |
% |
Cost |
n |
% |
Cost |
Non Arthritis |
1,316 |
87% |
$381,731.90 |
700 |
84% |
$64,779.89 |
Arthritis |
191 |
13% |
$90,318.11 |
129 |
16% |
$16,056.19 |
714.xx M |
81 |
42% |
$37,562.00 |
54 |
42% |
$6,383.03 |
Other arthritis |
110 |
58% |
$52,756.11 |
75 |
58% |
$9,673.16 |
TOTALS |
1507 |
100% |
$472,050.01 |
829 |
100% |
$80,836.08 |
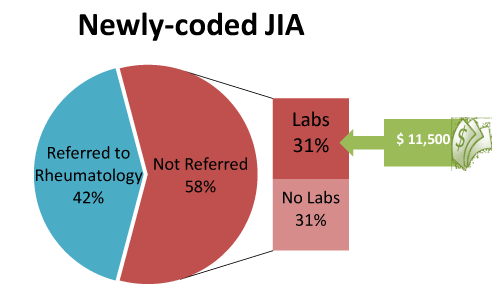
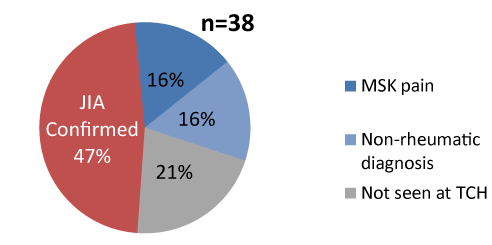
Further analyses identified 174 unique members with diagnosis code for JIA (714.xx). These members had 81 claims for ANA and 54 claims for RF. Chart review of these 174 JIA members showed that approximately 47% (n=83) of them were already established patients at TCH and 58% (n=91) had a newly coded diagnosis of JIA. Only 42% (n=38) of the newly coded members were referred to rheumatology sub-specialist for evaluation. Of the newly coded members 30% (n=27) were not referred. Of these groups, ANA and RF tests were ordered for n=28 patients but did not lead to a subsequent referral to a TCH pediatric rheumatologist (Figure 1). The reminding 42% (n=38) of the newly coded JIA group where referred to a pediatric rheumatology subspecialist a diagnosis of JIA was confirmed in 47% of them (Figure 2). Of these referred children, 10% (n=4) initially had a negative ANA and their referrals were delayed (range 6-18 months). This delay may have contributed to the progression of severe joint deformity and disability documented in their medical record upon presentation to rheumatology sub-specialist.
Discussion
We describe a preliminary pilot study. That assesses the frequency and expenditures associated with ANA and RF testing among members of an insured pediatric population. We supplemented claims date with clinical chart review of children with JIA ICD-9 code to assess appropriate use and potential impact of lab studies on a timely rheumatology referral and clinical course. Although there is currently insufficient evidence to support the use of RF and/or ANA as screening or diagnostic tests in children with suspected JIA, we found that these tests continue to be utilized for this purpose by pediatric primary care providers. Analyzing of the administrative claims and charts, documented that the code for JIA was often inappropriately assigned to order x-rays and magnetic resonance imaging (i.e. patient with brain cancer or an HIV patient with complains of bone or joint pain). Fifty nine percent of the ANA and 76% of the RF test were ordered by primary care physicians. As hypothesized, ANA/RF testing was frequently and repetitively inappropriately utilized by primary care providers. The cost of unnecessary ANA claims is difficult to assess as ANA is also used for evaluation of other autoimmune conditions, beyond the scope for this study. However, a pediatric primary care provider should never use a RF to screen for arthritis in children and adolescents. This could save about $61,435.42 (76% of $80,836.08) a year to the TCH health plan (small urban health plan). Furthermore, the inappropriate use of these labs of screening for rheumatologic conditions contributed to observe delays in referrals (range 6-18 months) of four patients that presented with severe joint disease, disability, and deformity.
There are limitations to our data collection and conclusions. Retrospective reviews of claims databases pose a series of methodological challenges, some of which are unique to this data source. Issues include clinical relevance, reliability of validity of data and data linkages. Also, chart review was not done in a systematic way and some important data was not recorded effectively. Other limitations included sample selection, and variable definitions. We limited to table 1codes for ANA and RF and did not take into account other bundled or reflex tests, which may have overlooked subjects for inclusion, or affected the valuation of associated costs. Our study chart review were restricted to members with diagnosis code JIA, 714.xx and not all members getting lab testing; this resulted in the identification of potential sampling bias and perhaps incomplete understanding of lab and referral patterns. Finally, given the high volume of patients and associated claims received each year, we limited the scope of inquiry to a “snap-shot” of claims data during a 1-year period. Although looking at health care cost data from one year is thought to be sufficient to identify major sources for health care expenditures, more stable estimates would be obtained by combining health care claims data for 24 or more months. We believe cost and inappropriate utilization patterns are probably even underestimated by our design limitations. Our findings emphasize the need for continuing educational efforts to disseminate guidelines and recommendations for diagnostic testing in children with suspected JIA and other musculoskeletal complaints. Not only for the unnecessary cost to our health care, but also to prevent morbidity to children and adolescents that have delayed referrals for having negative ANA/RF test.
Future directions
As our preliminary evaluation revealed apparent overuse and misuse of ANA and RF testing, further work is planned to address methodological issues. Specifically, we will examine claims for a period of more than a year, include CPT codes associated with bundled test, and will extend our chart review to primary and secondary diagnosis codes for other JIA-related conditions. We will evaluate the predictive value of ANA and RF testing for rheumatologic complaints, as well as the impact on delay in care and increased costs associated with testing by examining test results. We will complete an extended claims analysis and chart review that will involve revisiting study variable definitions, and development of a standardized data collection tool. We have submitted an IRB amendment to permit this expanded evaluation, and are refining our methodology so to develop a project timeline to enable robust re-analysis and dissemination of results.
We feel these refinements will enhance the validity of our analysis and interpretation. We then may be able to identify target populations of providers for which reimbursement modules, clinical guidelines, and subsequent educational activities can be developed to reduce healthcare costs and ultimately improve quality of care and patient outcomes.
2021 Copyright OAT. All rights reserv
References
- Comparing the U.S. and Canadian Health Care Systems. [www.nber.org/bah/fall07/w13429.html]
- Wong KO, Bond K, Homik J, Ellsworth JE, Karkhaneh M, et al. (2012) Antinuclear antibody, rheumatoid factor, and cyclic-citrullinated peptide tests for evaluating musculoskeletal complaints in children. AHRQ Comparative Effectiveness Reviews 50: 1-31. [Crossref]
- Smith JA (2009) Testing for Rheumatological Diagnoses in Children. Eur Paediatr Rev 3: 30-34. [Crossref]
- Correll CK, Spector LG, Zhang L, Brinstadt BA, Vehe RK (2014) A137: Appropriateness of rheumatology lab studies and referrals among general pediatricians. Arthritis & Rheumatology 66: S180.
- Breda L, Nozzi M, De Sanctis S, Chiarelli F (2010) Laboratory testing in the diagnosis and follow-up of pediatric rheumatic diseases: an update. Semin Arthritis Rheum 40: 53-72. [Crossref]
- Cassidy J, Petty RE (2011) Textbook of pediatric rheumatology (6th edn). Chronic arthritis in childhood 13: 211-235.
- Meyer O (2003) Evaluating inflammatory joint disease: how and when can autoantibodies help? Joint Bone Spine 70: 433-447. [Crossref]
- Sacks JJ, Helmick CG, Luo Y, Ilowite NT, Bowyer S (2007) Prevalence of and annual ambulatory health care visits for pediatric arthritis and other rheumatologic conditions in the United States in 2001-2004. Arthritis Rheum 57: 1439-1445. [Crossref]
- Helmick CG, Felson DT, Lawrence RC, Gabriel S, Hirsch R, et al. (2008) Estimates of prevalence of arthritis and other rheumatic conditions in the United States. Arthritis Rheum 58: 15-25. [Crossref]
- Harrold LR, Salman C, Shoor S, Curtis JR, Asgari MM, et al. (2013) Incidence and prevalence of juvenile idiopathic arthritis among children in a managed care population, 1996-2009. J Rheumatol 40: 1218-1225. [Crossref]
- van Rossum M, van Soesbergen R, de Kort S, ten Cate R, Zwinderman AH, et al. (2003) Anti-cyclic citrullinated peptide (anti-CCP) antibodies in children with juvenile idiopathic arthritis. J Rheumatol 30: 825-828. [Crossref]