Abstract
Verrucous epidermal nevi are congenital, non-inflammatory cutaneous hamartomas caused by somatic mosaicism. Histologically, epidermal nevi show hyperkeratosis, hypergranulosis, acanthosis, and papillomatosis with or without inflammation. Epidermolytic hyperkeratosis is a rare occurrence. We report a case of an epidermolytic variant of systematized verrucous epidermal nevus, involving large areas of the body.
Key words
verrucous epidermal nevus, VEN, epidermolytic hyperkeratosis, systematized nevus, Blaschko lines
Introduction
Verrucous epidermal nevus (VEN), also known as keratinocytic or non-organoid epidermal nevus, is a congenital, non-inflammatory cutaneous hamartoma composed of keratinocytes. It is manifested as papillomatous papules or plaques, often linear or Blaschkoid in shape. The extent and distribution of the VEN as well as the presence or absence of inflammation determines its subtype: localized VEN, inflammatory linear verrucous epidermal nevus (ILVEN), nevus uniuslateralis, systematized VEN, and ichthyosis hystrix [1].
The term systematized epidermal nevus is used for lesions that are bilateral and excessive. Ichthyosis hystrix is a term used to describe several rare skin disorders in the ichthyosis family of skin disorders characterized by massive spiky or verrucous hyperkeratosis. Histologically, VEN show hyperkeratosis, hypergranulosis, acanthosis, and papillomatosis with or without inflammation. Epidermolytic hyperkeratosis is a rare occurrence [2].
We report a case of an epidermolytic variant of systematized verrucous epidermal nevus, distributed along Blaschko lines.
Case report
A 1-year-old female child presented with widespread, dark-brown, hyperkeratotic, verrucous plaques since she was one month of age. There was no history of blisters or generalized redness at or after birth. Family history was notable for parental consanguinity (third cousins). However, no other family members, including three half sisters were affected by a similar skin condition.
Upon examination, dark-brown, verrucous plaques in Blaschkoid distribution were noted on the trunk and extremities bilaterally (Figure 1a). Over the thorax, linear plaques ran transversely, arranged in streaks and whorls (Figure 1b), as well as linear streaks over both lower limbs. Hyperpigmented velvety plaques were present in the intertriginous areas. The diaper area, and central face, as well as parts of truncus were spared. The hair, nails, and oral cavity were normal. Detailed pediatric, orthopedic and neurological consultations were sought and revealed no abnormalities.
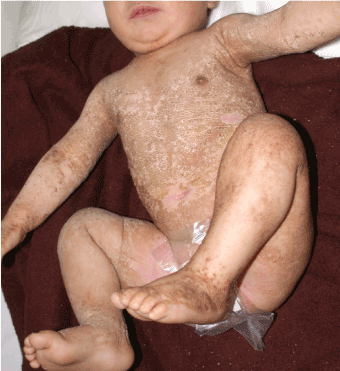
Figure 1a. Bilateral, extensive lesions that cover large areas of the body
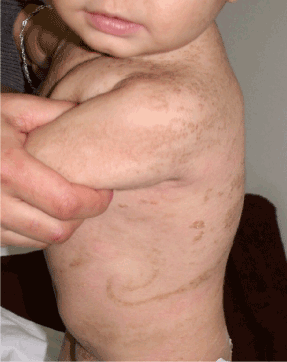
Figure 1b. Verrucous plaque in Blaschkoid distribution
Histo-pathological examination revealed typical features of epidermolytic hyperkeratosis.
A detailed analysis of skin sections revealed a focal epidermolysis in some areas (Figure 2a), while others showed a continuous involvement of the entire horizontal epidermis (Figure 2b). A mild, perivascular, chronic inflammatory cell infiltration was noted in the dermis.
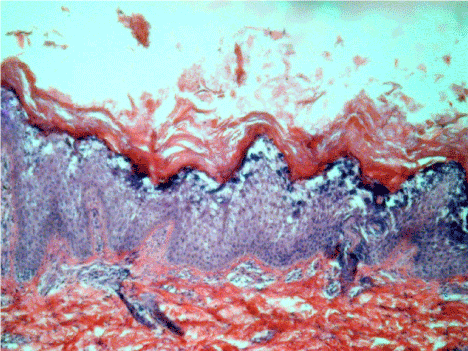
Figure 2a. Massive hyperkeratosis with foci of epidermolysis in the upper spinous layer. Hematoxylin-eosin, original magnification ×200.
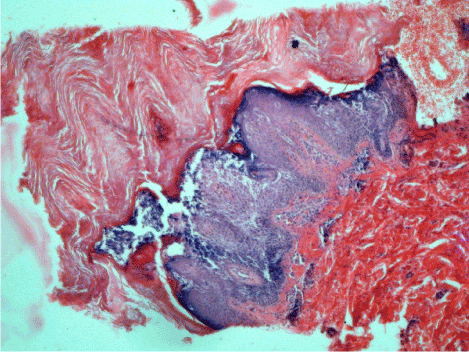
Figure 2b. Epidermolysis continuously involving the entire horizontal epidermis. Hematoxylin-eosin, original magnification ×200.
Based on the clinical and pathological findings the patient was diagnosed with a bilateral systematized epidermolytic verrucous epidermal nevus. Treatment with emollients and mild keratinolytics, such as urea cream and lactic acid lotion resulted in the soothing of the affected skin.
Discussion
Epidermal nevi (EN) are benign hamartomas of the skin arising from the embryonic ectoderm, which are a result of mosaic post-zygotic mutations. Depending on the affected components of the epidermis, they are further divided into non-organoid (keratinocytic) and organoid types.These keratinocytic nevi can be classified histologically into two subtypes: epidermolytic and non-epidermolytic [3].
According to Submoke and Piamphongsant, 62% of EN have a typical hyperkeratosis-papilomatosis-acanthosis configuration, whereas 16% show a feature of Epidermolytic hyperkeratosis [4].
Epidermolytic hyperkeratosisis (EHK) is a pathologic reaction pattern, first described by Ackerman in 1970, characterised by hyperkeratosis, hypergranulosis, and epidermolysis [5].
Through light microscopy, epidermolysis is seen as various sized clear spaces around keratinocyte nuclei (perinuclear vacuolisations) with indistinct peripheral cell boundaries in the upper spinous and granular layers. The boundaries appear to be formed by eosinophilic and basophilic granules [6].
2021 Copyright OAT. All rights reserv
The use of the term epidermolytic hyperkeratosis to describe both the clinical disease and the characteristic histopathologic features caused great confusion in medical literature.
More recently, there are attempts in order to differentiate clinical epidermolytic hyperkeratosis (cEHK) and histologic epidermolytic hyperkeratosis (hEHK). The histology of EHK is seen in a spectrum of clinical conditions including generalized epidermolytic hyperkeratosis, also known as bullous congenital ichthyosiform erythroderma, mosaic cEHK, ichthyosis bullosa of Siemens, and Vorner’s palmoplantar keratoderma
Furthermore, hEHK is seen in a variety of other conditions including melanocytic nevus, basal cell carcinoma, pilar cyst, leukoplakia, epidermolytic acanthoma and nevoid follicular epidermolytic hyperkeratosis, as well as in normal skin and in normal oral mucosa.
According to Ross et al, the pattern of histologic involvement may be a useful predictor of the clinical phenotype of cEHK: the continuous involvement of the entire horizontal epidermis correlates with generalized cEHK, while focal EHK correlates with mosaic epidermolytic hyperkeratosis. Our case revealed both histological patterns, focal and continuous.
Management of VEN is challenging.Topical modalities have shown inconsistent efficacy, and destructive methods, including laser, electrocoagulation, and dermabrasion, have potential permanent complications. Definitive treatment involves full-thickness excision, which may not be possible in extensive lesions [7]. Taking into account the young age of our patient, our main treatment goal was the reduction of hyperkeratosis.
Conclusion
A rare subgroup of epidermal nevi displays histopathological features typical of EHK. Clinicopathologic correlation is essential for diagnosis.
References
- Brandling-Bennett HA, Morel KD (2010) Epidermal nevi. Pediatr Clin North Am 57: 1177-1198. [Crossref]
- Su WP (1982) Histopathologic varieties of epidermal nevus. A study of 160 cases. Am J Dermatopathol 4: 161-170. [Crossref]
- James WD, BergerTG, Elston DM (2011) Epidermal nevi, neoplasm and cysts. Andrews’s diseases of the skin. (11th edition). Saunders Elsevier, Philadelphia, USA: Pp. 658.
- Submoke S, Piamphongsant T (1983) Clinico-histopathological study of epidermalnaevi. Australas J Dermatol 24: 130-136. [Crossref]
- Steele CL, Shea CR, Petronic-Rosic V (2007) Epidermolytic hyperkeratosis within infundibular cysts. J Cutan Pathol 34: 360-362. [Crossref]
- Ross R, DiGiovanna JJ, Capaldi L, Argenyi Z, Fleckman P, et al. (2008) Histopathologic characterization of epidermolytic hyperkeratosis: a systematic review of histology from the National Registry for Ichthyosis and Related Skin Disorders. J Am Acad Dermatol 59: 86-90. [Crossref]
- Lapidoth M, Israeli H, Ben Amitai D, Halachmi S (2013) Treatment of Verrucous Epidermal Nevus: Experience with 71 Cases. Dermatology 226: 342-346. [Crossref]




