Abstract
Despite great efforts to elaborate the physiologic mechanisms in the occurrence development of sepsis, it is still an underlying cause of death in emergency room. Now, it has been identified that excessive systemic inflammation definitely participates in the course of sepsis. The inflammatory response is indeed a host-defense response but in some cases it may cause deterioration to host depending on internal and external factors. In this review we will describe the pathophysiological approach for sepsis studied so far and introduce the therapeutic strategy of this issue.
Key word
sepsis, pathophysiological mechanism, digestive tract, therapy
Introduction
Sepsis has gotten more and more attention in clinical and laboratory researches in recent decades. With the deepening understanding of this disease and the progress of modern medical technology and medical practice, the increasing morbidity of sepsis is reported in literatures[1]..And the increased use of medical equipment, immune suppressor and broad-spectrum have succeeded in prolonging these patients ‘lives but at the same time have created a good number of patients who are also especially vulnerable to infection and this trend probably may go on in the coming future.
There are distinct differences in the incidence of sepsis among all region and countries because of differs between living standard, environments and medical technology, and other factors like the consensus of definition of disorders related to sepsis and so on. Systematic and initially definitions of a sequence of sepsis-related diseases has been proposed about twenty years ago [2], which are refined and completed over time. With correlational researches going, some people suggested that several concepts and definitions should be discarded such as toxemia, pyrexia and bacteremia. Now it is commonly accepted that sepsis may be defined into three hierarchical stages, namely sepsis, severe sepsis and septic shock according to the different condition of diseases [3].
In this context, we have chosen to put our focus on two aspects which are the existing research progress and the future research direction of this disease (Figure 1).
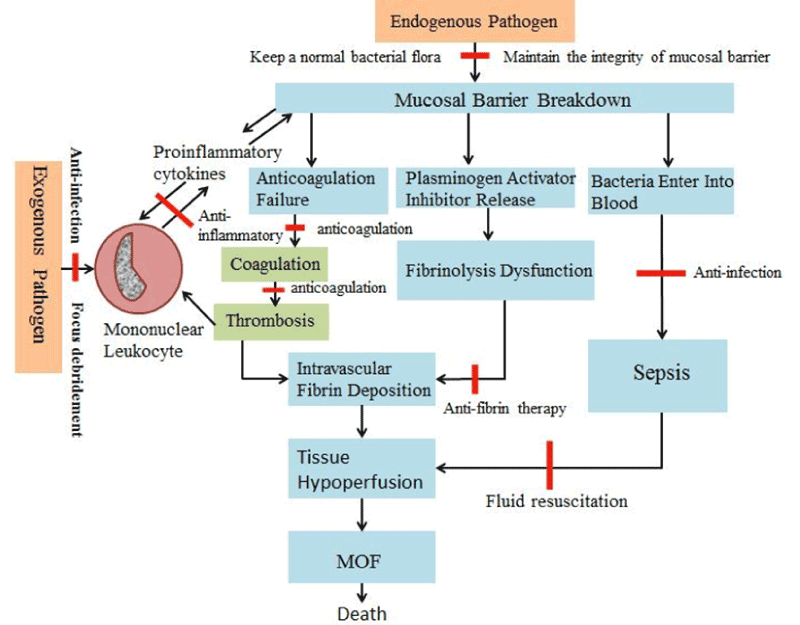
Figure1. Different Mechanism of Sepsis.
Research achievement on mechanisms of sepsis
Although a vast amount of elaborately and profoundly research work have been done, the exact mechanism involved are still mysterious. The manifestations of sepsis and the development of septic shock even multi-organ failure (MOF) are largely due to the pathophysiological effects of inflammatory agents which are released as parts of the systemic immune response [4]. Although the systemic immune response and the release of inflammatory agents are primarily for the protection against pathogens, if the immune response is excessive, uncontrolled release of these agents in turn can have significant negative impact upon the body. The conventional view of sepsis is an anti-inflammatory response to the pathogen, some researchers has described sepsis as the immune system gone haywire [5].However, therapies specific to the inflammatory response have proven non-effective in either anti-inflammatory process or improved survival [6].
Recent researches have elucidated important function of cytokines including tumor necrosis factor (TNF), intercleukin-1, intercleukin-6, intercleukin-8in the course of sepsis, and tried to figure out their applied value in clinic [7]. These relevant molecules act as intercellular signals in either anticrime or paracrine fashion. If the human body suffers from infection or injury, the cytokine cascade will be activated as well as the coagulated and fibrin lytic systems of the body. This process results in acute lung injury/acute respiratory distress syndrome, shock, disseminated intravascular coagulation and fibrinolysis which are the complication of sepsis.
After invading into body, the cellular components released by pathogen, especially the lipopolysaccharide (LPS), a kind of bacterial endotoxin, can induce phagocytosis of macrophages and neutrophil granulocyte, the secretion functions of immune cells and endothelial cells. LPS in macrophages and neutrophil granulocyte will bind with the serum LPS binding protein, then link a surface receptor of antigen presenting celling, i.e., CD4 [8], and this binding stimulate the expression of cytokines, CD80 and CD86 in antigen presenting cells and finally leads to activation of the T cell[9].Besides, IL-6 is also a stimulator for T cells. Activation of the cell results in two kinds of immune response, namely relative immunosuppression led by IL-4, IL-10 and relative immune enhancement led by IL-1, IL-2, TNF, the form will evolve into compensatory anti-inflammatory response syndrome (CARS), and the latter will be systemic inflammatory response syndrome (SIRS). And these findings will reveal new therapeutic strategy.
Researches focused on neutrophil activation have elucidated that this process which results from the action of cytokines is believed to be an important factor in the pathogenic mechanism of sepsis [10]. When the inflammation response becomes systematic, the comprehensive activation of neutrophils tend to form aggregates and become more adherent to endothelial cells, finally cause endothelial cell dysfunction and damage [8]. This course may reduce oxygen diffusion to tissues and impair oxygen metabolism. Activation of neutrophil can also results in production of free oxygen radicals. This is mediated by overexpression of CD11 and CD18, which are two kinds of neutrophil adhesion molecules. This pathological process can lead to endothelial function damaged, the microvasculature injured and ischemia. When organ and tissues get reperfusion after ischemia, the formation of oxygen radicals will generate which may further aggravate the endothelial damage. Increased levels of nitric oxide and its products can be also found in patients with sepsis, these substances will make hypotension occurred. This secondary hemodynamic abnormality, a symbol of the injury to the microvasculature, is the basis for multi-organ failure [11]. So multiple organ failure syndromes including the failure of the kidney, cardiovascular system and so on may be the result of the interweaving of all these alteration in vivo. All these processes are unpredictable and unchecked, so the morbidity and mortality are staying at high level though there are a lot of related researches on this field.
Because of the pathogenic complexity of sepsis, it is increasingly clear that the combined-modality treatment has stronger and faster medications than single therapy. Adjustment of the cytokine effects is as important in reducing mortality as eradication of the focus and hemodynamic stabilization among patients with sepsis.
Duplicate effect of coagulation and inflammation on sepsis
The integration of inflammation and coagulation is so close that cytokines participating entirely in development process of sepsis stimulate thrombin activation and also play an important role in the development of the intravascular coagulation [12]. The inflammatory cytokines activate coagulation and vice versa the activated coagulation cascade may induce the exacerbation of inflammation [13]. Previous researches have showed that similar activation mechanism links these two courses via various kinds of pathways [14]. The complex interaction between the inflammation and coagulation are future complicated by complement system during sepsis which can recognize infectious changes in the organism [15]. Complement including C5a has adverse effects through both inflammation and coagulation. For example, this system can decrease effectiveness of neutrophil, and in turn increase the macrophages’ phagocytic function, meanwhile it can also unbalance the coagulation, and finally lead to an immunodeficiency in patients with sepsis [16]. So sepsis is a result of a delicate network which an over-riding etiology causing host demise. In this way, it is important to recognize these various targets in those systems that will be targeted as therapy to enhance the whole host response to overcome sepsis. There are a lot of animal experiments have shown that attempt at immunomodulation may be useful in reducing the morbidity and mortality of sepsis, however, it is still too early to make recommendations on their regular use in clinical application [17]. Trials on anti-endotoxin monoclonal antibodies have been still unsatisfactory to date [18]. But the use of anti-oxidants like superoxide to prevent injury caused by free oxygen radicals has been proved satisfactory [19]. And the use of nitric oxide synthetase inhibitors also has been shown to have some beneficial effects on sepsis and sepsis-related disease [20]. Now there are more clinical trials have to be done in order to better explicit the use of these substances.
Role of the digestive tract in sepsis
The role of the digestive tract in sepsis is being much more accounted of [21]. The gut is an important focus of infection in sepsis. The micro biota in the digestive tract of the patients is the primary source of endogenous pathogens causing sepsis. The common pathogens are the aerobic gram-negative bacillus like E. coli, Entero bacter and Pseudomonas aeruginosa. It was used to believe that the anaerobic flora is very rarely involved in such an infections situation, however, there have been several reports that this flora can also lead to sepsis [22]; reflecting badly on the colonization resistance of the digestive tract. In septic patients who require prolonged hospitalization, their digestive tract may be affected by the multi-ply resistant strains common in the hospital environment. Bacteria from gut have access to the bloodstream via the intestinal harrier, and this course is referred to translocation [23]. Some researchers thought that the duality of gastrointestinal floras make themselves have the propensity to generate an insidious possibility of feeding intolerance, even ileus and mucosal barrier breakdown which may in turn convert the normally harmless enteric bacteria into harmful pathogens, which so future turn the gut wall into a copious generator of inflammatory mediators that generate the deadly perfect storm of sepsis [24]. Factors in the digestive tract that protect against bacterial translocation include gastric acid, intestinal fluid, the normal flora, avoiding the production of oxygen free radicals that may cause endothelial cell injury, the tight epithelial junctions of the intestinal mucosa and the tissue immunity of the digestive tract. Maintaining the integrity of the intestinal mucosal barrier as well as keeping a normal bacterial flora can help to reduce the possibility of bacterial translocation and the risk of sepsis. It is now believe that total enteral nutrition is an important factor to reserve normal gastrointestinal function [25]. The total parenteral nutrition is more likely to induce bacterial translocation which is associated with an increased incidence of sepsis. There are other factors that also promote normal functioning of the gut including the glutamine dipeptide and superoxide dismutase enzyme which prevent the formation of free oxygen radicals [26,27]. Proton pump inhibitor and H2-antagonists which can reduce gastric acidity may cause bacterial overgrowth and colonization in pharynx oral sand gastric area. Several studies have shown that this situation will easily make organism be vulnerable to nosocomial pneumonia because of the subsequent aspiration of oro pharyngeal gastric contents which can particularly occur in patients who are on ventilators. In this regard, it has been suggested that gastrointestinal antacids such as sucralfate and magnesium chloride may be more suitable protective agent to use for the septic patients since these drugs will not affect gastric acidity [28]. Now this situation is clearly established and some researchers have hold that translocation of bacteria is a more important pathogenesis in nosocomial pneumonia and therefore the prevention of stress ulcers is more important than prevention of bacterial overgrowth [29].
Since a majority of infections are caused by gram negative aerobic bacilli, our ability to improve survival and decrease morbidity for septic patients largely depend on the development of preventative measures as well as post-sepsis therapeutics. Much like other systems, single-target approaches to therapy will likely prove unsuccessful. A therapeutic approach to improve gastrointestinal motility could break the intestinal cycle of sepsis and prevent the development of SIRS and multiple organ failure. Unfortunately, although sepsis induced ileus is a major clinical problem, precious little data exists on specific molecular signaling mechanisms which cause gastrointestinal ileus. Despite some new markers indicating the mucosal damage of the digestive tract in patients with sepsis, there are still few effective methods to prevent and treat the impaired immune defense and microenvironment of gastrointestinal tract in septic patients [30].
Conclusion
In recent years, a better understanding in the pathophysiological mechanism involved in sepsis has led to innovations in the prevention and treatment of sepsis made by a number of clinical trials and animal experiment, some of which have already been mentioned earlier. And researchers never ceased to improve the cognition of sepsis [31]. For all these clear mechanism, a massive effort has been made to integrate fundamental researches into the clinical application [32]. They believed that our attention should not only be paid to modulate functions of immunity and inflammatory system, maintain balanced state between the two, but also to prevent the infection from gastrointestinal tract through maintaining normal gut function, reducing risk of bacterial colonization and translocation, and stop or at least contain the genesis and development of sepsis ultimately. Early antibiotic administration, anticoagulant therapy in sepsis, nursing in the proper posture [33], the promotion of total enteral feeding, the use of antacid may be some of the measures that would help to achieve this. Prevention of infection from exogenous sources through high standards of control of hospital infection remains foremost importance. Hemodynamic stabilization and the application of immune modulator to alleviate the adverse effects of the cytokine cascade are probably as important as antimicrobial therapy in managing the sepsis in clinic. However, the standardized procedures of these agents have yet to be strictly established. There are still problems of patient selection which remains to be sorted out. Some patients are more likely to benefit from certain regimens. With a better understanding of the pathogenic mechanisms involved, it may be possible to select specific strategies for defined groups of patients (Figure 1). In this way, prospects for more effective management of sepsis seem to be better.
References
- Martin JB, Wheeler AP (2009) Approach to the patient with sepsis. Clin Chest Med 30: 1-16, vii. [Crossref]
- Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, et al. (1992) The pathogenesis of sepsis. Annals of Internal Medicine 115: 413–426.
- Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, et al. (1992) Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med 20: 1644-1655.
- Osuchowski MF, Welch K, Siddiqui J, Remick DG (2006) Circulating cytokine/inhibitor profiles reshape the understanding of the SIRS/CARS continuum in sepsis and predict mortality. J Immunol 177: 1967-1974. [Crossref]
2021 Copyright OAT. All rights reserv
- Stone R (1994) Sepsis: an immune system gone haywire. Science 264: 366. [Crossref]
- Riedemann NC, Guo RF, Ward PA (2003) Novel strategies for the treatment of sepsis. Nat Med 9: 517-524. [Crossref]
- Zang XF, Niu SP, Chen W: Combined Inflammatory Cytokines Test in Early Diagnosis of Sepsis inBloodstream Infection Patients Has Clinical Value. J Infection Research 1: 0041-0050.
- De Gaudio AR, Rinaldi S, Chelazzi C, Borracci T (2009) Pathophysiology of sepsis in the elderly: clinical impact and therapeutic considerations. Curr Drug Targets 10: 60-70. [Crossref]
- Medzhitov R, Janeway C (2000) Innate immunity. NEJM 343: 2–4.
- Dellinger RP, Carlet JM, Masur H, Gerlach H, Calandra T, et al. (2004) Surviving Sepsis Campaign guidelines for management of severe sepsis and septic shock. Intensive Care Med 30: 536-555. [Crossref]
- Liu YC, Chang AY, Tsai Y-C (2009) Differential protection against oxidative stress and nitric oxide overproduction in cardiovascular and pulmonary systems by protocol during endotoxemia. Journal of Biomedical Science 16: 119-124.
- Levi M, Nieuwdorp M, van der Poll T, Stroes E (2008) Metabolic modulation of inflammation-induced activation of coagulation. Semin Thromb Hemost 34: 26-32. [Crossref]
- Kountchev J, Bijuklic K, Bellmann R, Wiedermann CJ, Joannidis M (2005) Reduction of D-dimer levels after therapeutic administration of antithrombin in acquired antithrombin deficiency of severe sepsis. Crit Care 9: R596-600. [Crossref]
- Engelmann B, Massberg S (2013) Thrombosis as an intravascular effector of innate immunity. Nat Rev Immunol 13: 34-45. [Crossref]
- Markiewski MM, DeAngelis RA, Lambris JD (2008) Complexity of complement activation in sepsis. J Cell Mol Med 12: 2245-2254. [Crossref]
- Ward PA (2004) The dark side of C5a in sepsis. Nat Rev Immunol 4: 133-142. [Crossref]
- RA B: Systemic inflammatory response syndrome (SIRS): Where did it come from and is it still relevant today? Virulence 5: 20-26.
- Aldridge AJ (2002) Role of the neutrophil in septic shock and the adult respiratory distress syndrome. Eur J Surg 168: 204-214. [Crossref]
- Patil NK, Parajuli N, MacMillan-Crow LA, Mayeux PR, et al. (1992) Inactivation of renal mitochondrial respiratory complexes and manganese superoxide dismutase during sepsis: mitochondria-targeted antioxidant mitigates injury. Am J Physiol Renal Physiol 306: F 734-743.
- Bahar Tunctan , Belma Korkmaz , Ayse Nihal Sari , Meltem Kacan , Demet Unsal (2010) A Novel Treatment Strategy for Sepsis and Septic Shock Based on the Interactions between Prostanoids, Nitric Oxide, and 20-Hydroxyeicosatetraenoic Acid. Anti-Allergy Agents in Medicinal Chemistry (Formerly Cu) 11: 121-150.
- Gosain A, Gamelli RL (2005) Role of the gastrointestinal tract in burn sepsis. J Burn Care Rehabil 26: 85-91. [Crossref]
- Emmanuel Okon, Eliahu Bishburg, Sandra Ugras, Trini Chan, He Wang, et al. (2010) Clostridium perfringens meningitis, Plesiomonas shigelloides sepsis: A lethal combination. The American Journal of Case Reports 14: 70-72.
- Vaishnavi C (2013) Translocation of gut flora and its role in sepsis. Indian J Med Microbiol 31: 334-342. [Crossref]
- Buchholz BM, Bauer AJ (2010) Membrane TLR signaling mechanisms in the gastrointestinal tract during sepsis. Neurogastroenterol Motil 22: 232-245. [Crossref]
- Pontes-Arruda A, Aragão AM, Albuquerque JD (2006) Effects of enteral feeding with eicosapentaenoic acid, gamma-linolenic acid, and antioxidants in mechanically ventilated patients with severe sepsis and septic shock. Crit Care Med 34: 2325-2333. [Crossref]
- Sandini M, Nespoli L, Oldani M, et al.,: Effect of Glutamine Dipeptide Supplementation on Primary Outcomes for Elective Major Surgery. Systematic Review and Meta-Analysis. Nutrients 7: 481-499.
- Brenner T, Hofer S, Rosenhagen C, Steppan J, Lichtenstern C, et al. (2010) Macrophage migration inhibitory factor (MIF) and manganese superoxide dismutase (MnSOD) as early predictors for survival in patients with severe sepsis or septic shock. J Surg Res 1: e163.
- Chang RM, Wen LQ, Chang JX, Fu YR, Jiang ZP, et al. (2013) Repair of damaged intestinal mucosa in a mouse model of sepsis. World J Emerg Med 4: 223-228.
- Tejada Artigas A, Bello Dronda S, Chacón Vallés E, Muñoz Marco J, Villuendas Usón MC, et al. (2001) Risk factors for nosocomial pneumonia in critically ill trauma patients. Crit Care Med 29: 304-309. [Crossref]
- Žurek J, Fedora M (2013) Trefoil factor 1 as a marker of mucosal damage of the gastrointestinal tract in children with sepsis. Biomarkers 18: 338-342. [Crossref]
- R. Phillip Dellinger, Mitchell M. Levy, Jean M. Carlet, et al (2013) Surviving Sepsis Campaign: International guidelines for management of severe sepsis and septic shock. Intensive Care Medicine 39: 165-228.
- Kinasewitz GT, Yan SB, Basson B, Comp P, Russell JA, et al. (2004) Universal changes in biomarkers of coagulation and inflammation occur in patients with severe sepsis, regardless of causative micro-organism [ISRCTN74215569]. Crit Care 8: R82-90. [Crossref]
- Han W, Min W (2009) Effect of Different Body Position on Ventilator-Associated Pneumonia. Chinese Journal of General Practice 24: 89-100.

