Lupus vulgaris is the commonest form of cutaneous tuberculosis accounting for about 75% of the cases. Clinical dermatologists need to be aware of the myriad clinical presentations of this condition as it can be misdiagnosed especially when the index of suspicion is low. It is important to make a diagnosis and promptly treat as it can be disfiguring and destructive.
Tuberculosis (TB) is one of the oldest known diseases with evidence of the disease being found in the vertebrae of the Neolithic man in Europe and in Egyptian mummies. It was not until 1882 that Robert Koch discovered the causative agent Mycobacterium tuberculosis [1]. Though improved living standards, the BCG vaccine and standardised chemotherapy have greatly reduced the disease burden of tuberculosis, in the current era of HIV, co-infection with tuberculosis (incidence 17.4%) is still a major concern especially in developing countries [2].
Lupus vulgaris (LV) is the commonest form of cutaneous TB accounting for 75% of the cases. It was first described by Erasmus Wilson in 1865 who compared the clinical appearance of the lesions to the ravages of a wolf [3,4]. Various clinical forms of the disease have been reported, many of which are close mimics of other common dermatoses in the tropics [5]. This, and its association with systemic TB make it essential to have a clear understanding of LV.
LV, also referred to as “tuberculosis luposa” and “tuberculosis luposa cutis” is more common in males with a male to female ratio of 6.8:1 [6,7]. Though the disease generally begins before puberty, it has been reported to occur as early as 18 months of age [8]. Due to the asymptomatic nature and slow progression of the lesions, the patients present late; The duration of illness varying between 3 months to 50 years before medical help is sought [9,10]. LV is more common in the tropics among the lower socioeconomic group. The clinical presentation also varies with the geographic location. In Europe, over 80% of the lesions occur on the head and neck, particularly on the nose and cheek [11], Whereas in the tropics lesions are noticed more commonly on the extremities and buttocks. This difference has been attributed to the increased environmental temperature encountered in the tropics and cultural practice sitting on the ground and walking bare feet [4].
Though the commonest causative organism is M. tuberculosis, few reports of lupus vulgaris associated with M. bovis, especially M. bovis spp caprae [12], Bacillus Calmette- Guerin [13,14] and M. xenopi [15] have been reported. The mode of infection is thought to be exogenous or endogenous inoculation following minor trauma including tattooing [16,17] and ear piercing [18]. Multiple reports of the occurrence of LV following BCG vaccination have been documented [13].
LV starts as a soft brownish red papule or nodule that gradually expands by involution in one area with expansion in another, gradually progressing over a period of many years to form a well-defined skin-coloured to erythematous plaque with an “apple jelly nodule” appearance on diascopy [19]. The plaque is characterised by evidence of healing and atrophic scarring in some areas interspersed between areas of activity giving a wolf bitten appearance. The lesions are usually located on the buttocks, thighs and occasionally on the face [20]. Lesions involving the genitalia [21,22], nasal mucosa [23-25] and auricular cartilage are rare but associated with severe disfigurement [4]. Other uncommon sites include the oral mucosa [26], larynx [27] and conjunctiva [28]. Ocular involvement with extension to the globe [29], occurrence at the site of BCG vaccination [14] and in the vicinity of scrofuloderma [30] and lesions in a “necklace distribution” have also been reported [31]. Indurated plaques of LV on the earlobes causing “turkey ears” is a recently described sign of LV [32]. An eczematous variant, “Lupus vulgaris erythematoides “has been described [33]. Though the lesions are mostly unilateral, cases with bilateral earlobe involvement and disseminated lesions have also been reported [34-36].
The commonly encountered clinical variants include classic plaque or keratotic type, hypertrophic, ulcerative, atrophic and planar [37]. Of these, the keratotic type is the most common whereas ulcerative and atrophic forms are the least common [38]. Bhutto et al. [20] described four major types of lupus vulgaris:
- 1. Psoriasiform type: Single or multiple flat plaques varying in size and shape with annular, oval or irregular borders on a non erythematous base. The lesions are covered with thick silvery scales resembling psoriasis. Lesions commonly occur on the legs, knees and back (Figure 1).
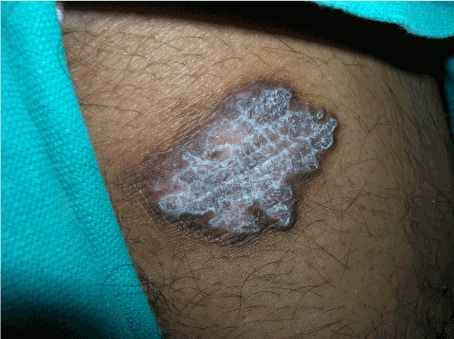
Figure 1. Psoriasiform lupus vulgaris: Solitary plaque with silvery scaling
- 2. Nodular type: Multiple nodules with the classically described “apple jelly” appearance surrounding a single larger plaque with a clear or sometimes atrophic centre. These lesions are frequently located on the thighs and hips (Figure 2).
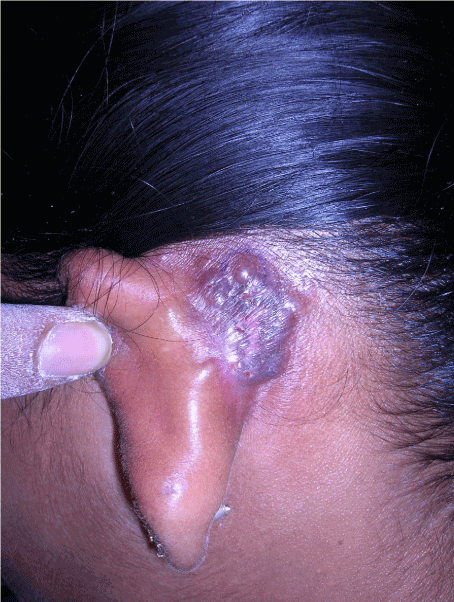
Figure 2. Nodular lupus vulgaris on the retroauricular area
- 3. Papular type: Small reddish-brown to skin-coloured papules. The lesions closely resemble cutaneous leishmaniasis and are seen mostly on the cheek and rarely on the nose and abdomen.
- 4. Erythematous type: Erythematous plaques of 2-5 cm with irregular margins with minimal scaling on the surface, clinically resembling eczema. The affected sites include the face, hips and arms (Figure 3).
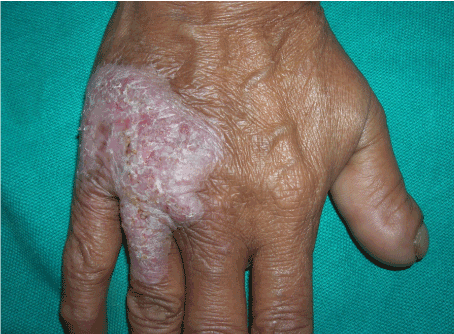
Figure 3. Erythematous plaque type of lupus vulgaris on the dorsum of the hand
Other unusual presentations include sporotrichoid lesions [39], annular lesions [40-42], disseminated lesions [34-36], giant lesions [37] (Figure 4) and lesions mimicking granulomatous folliculitis [43].
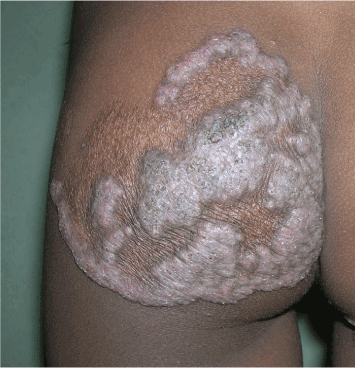
Figure 4. Giant plaque of lupus vulgaris on the gluteal region
Although regional lymphadenopathy is not uncommon [44], in rare cases when the lymph nodes have been destroyed due to intense tissue reaction, the patients develop lymphedema. LV associated with esthiomene has been documented [45].
The association of LV with systemic TB is seen in 10-30% cases [38]. Concomitant active TB elsewhere involving the lungs, bones, liver and other organs can be demonstrated in only 10% to 30% of the cases, and approximately only one half of the cases have history of past infection [46]. Papulonecrotic tuberculids [36], scrofuloderma [30,47], TBVC [6] and lichen scrofulosorum [48] have been reported to coexist with LV. Miliary TB has been rarely associated with LV and is hypothesised to occur following a drop in the patient’s immune status [44].
Various malignancies have been reported to occur in long standing cases of LV including SCC in 8% cases [49] and BCC [50,51]. One case of LV associated with Non Hodgkin’s Lymphoma has been reported [52].
In the immunocompromised host
Though lupus vulgaris is uncommon in the immunocompromised host, both solitary and disseminated lesions have been reported. The clinician must be aware that multiple forms of TB can occur concomitantly in such situations and the patient must be investigated and treated accordingly [53].
Differential diagnosis
LV mimics various other tropical dermatoses and can often be misdiagnosed clinically as TBVC, leishmaniasis, Hansen’s disease, syphilis and deep fungal infections e.g. actinomycetoma Madhura mycosis, sporotrichosis and chromomycosis [20,38,39]. Lesions on the face may be mistaken for DLE in view of the atrophic scarring [4]. Early lesions resemble a Spitz nevus or a haemangioma [54]. Other common dermatoses that need to be excluded are psoriasis [55-57], eczema [33], sarcoidosis, porokeratosis [58], hypertrophic lichen planus, lichen simplex chronicus [59], tinea corporis [41] and blastomycosis [60]. Lesions may mimic squamous cell carcinoma and lead to a diagnostic dilemma especially in long standing lesions as SCC is known to develop in 1-2% of cases over a period of 10-30 years [61].
Lesions on the nasal mucosa may mimic other granulomatous lesions including lepromatous leprosy, Wegener’s granulomatosis and syphilis with destruction of the nasal cartilage and deformity [24].
The diagnosis of LV requires a full workup including a detailed history and a thorough physical examination. Due to its myriad forms, a high index of suspicion is the key to making the diagnosis. Laboratory investigations should aim at both confirming the diagnosis of lupus vulgaris and excluding other foci of tuberculosis.
In LV the tuberculin test or Mantoux skin test becomes positive 2-10 week s following infection and has a sensitivity between 33% and 96% and specificity of 62.50% with a cut-off of 10 mm. In unvaccinated populations, the sensitivity is close to 97% [62]. Fine needle aspiration cytology, though not commonly used in the diagnosis of LV, shows cohesive epithelioid cell granulomas with or without chronic inflammatory infiltrate in 89%; however, Acid Fast Bacilli (AFB) can be demonstrated only in 22.2% cases [63]. Interferon –gamma release assays performed on whole blood, like Quantiferon- Gold and T- SPOT have been rapidly gaining popularity due to their high specificity and speed even though the sensitivity in cutaneous TB is average [64].
A biopsy is considered the pillar for identification of cutaneous TB [65]. The sample can be utilized for the following tests:
- 1. Tissue smears
- 2. Histopathology
- 3. Bacteriological cultures
- 4. PCR
Tissue smears do not demonstrate bacilli but help exclude other mimics e.g. leishmaniasis. Cultures have a higher sensitivity (up to 90%) and may detect as few as 10-100 bacilli/ml. However, the delay of 3 to 6 weeks required for culture results currently limits their use in the diagnosis of tuberculosis. Though the Lowenstein- Jensen medium, one of the oldest and time tested media is still in use, newer popular media for the culture of M. Tuberculosis include biphasic (MB-Check; Nippon Roche Co., Ltd., Tokyo, Japan) and radiometric (BACTEC; Nippon Becton Dickinson Co., Ltd., Tokyo, Japan) liquid-based culture systems and egg-based media (3% Ogawa and Ogawa K). Mycobacterial growth is better on an egg-based medium, but quicker on agar medium. Liquid systems allow for rapid growth (1–3 weeks), while growth on solid media can take from 3 to 8 weeks. The BACTEC- MGIT 960 and BACTEC460TB are of the most popular tests.
The MycoDot test, which is a lipoarabinomannan (LAM) antigen ELISA has a positivity of 85% and the sensitivity and specificity of 26-81% and 92-100% respectively.
Currently, though PCR appears to be the most useful in multibacillary forms of CTB, its utility in the paucibacillary forms like LV is limited [54]. In one report of AFB-negative specimens, the overall sensitivity of PCR was found to be 50 to 72 percent [66]. In a study by Suthar et. al, none of the patients showed a positive reaction on mRNA PCR test. DNA PCR is more useful with a sensitivity of 25% and a specificity of 73.7%. Hence, the results of PCR should be interpreted cautiously in the light of clinical and histological findings [67]. Though the value of genotyping has been established in various other forms of TB especially in this era of drug resistance, it has not been well studied in lupus vulgaris.
Definite laboratory confirmation requires either a positive culture of tubercle bacilli or from guinea pig inoculation, but these are not essential for routine clinical diagnosis [64].
The characteristic histology of LV is of a well formed granuloma without caseation with absent AFB. The epidermis may be atrophic or hypertrophic, with acanthosis, papillomatosis and pseudoepitheliomatous hyperplasia. The epidermal changes will vary based on the clinical presentation. Well defined tuberculoid granulomas composed of Langerhans giant cells and mature epitheliod cells with a dense lymphocytic infiltrate with plasma cells located in the mid dermis is characteristic. Occasionally the granulomas may be sarcoidal or mixed. Caseation is rare and may occur within small foci of the granuloma (Figure 5). AFB are infrequently detected. A deep biopsy is highly recommended to visualise the entirety of the granuloma. Due to the paucibacillary state, the Zeil Nielsen stain has limited utility [54].
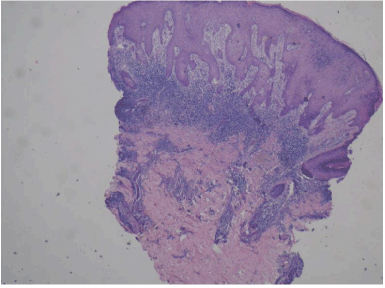
Figure 5. Histology of lupus vulgaris: well formed tuberculoid granulomas without caseation (H&E 10x)
Histological differential diagnoses include sarcoidosis, tuberculoid leprosy, deep fungal infection, and foreign body reaction [68].
Over the years, various treatment modalities have been tried for LV including mercury [69], potassium iodide [70], arsenic [71] and vitamin D2 [72]. In 1903, Niels Ryberg Finsen was awarded the Nobel Prize for his invention of light therapy for skin tuberculosis (lupus vulgaris). The mechanism of action has been hypothesised to be by the production of singlet oxygen through radiation of porphyrins with light leading to destruction of the mycobacteria [73].
Surgical excision and flap reconstruction has been successfully attempted with no recurrence on long term follow up. Though the advantage of this therapeutic approach is that there is quick eradication of the disease avoiding the unsightly wolf bitten scar, it is not a recommended modality of treatment as microscopic spread to the lymph nodes and other sites will not be treated. Recurrences have been reported with such an approach [74].
Earlier reports indicate that lupus vulgaris has been treated with Isoniazid alone [75,76]. But this may lead to the emergence of drug resistant strains of M tuberculosis especially if extracutaneous sites are involved and should be discouraged.
As controlled trials are lacking for the treatment of cutaneous TB, the recommendations from trials on pulmonary and other extracutaneous forms of TB have been incorporated into the treatment guidelines. Currently, the treatment of all types of tuberculosis is by the directly Observed Treatment Short Course (DOTS) strategy, which is implemented by World Health Organization (WHO) [77]. Most DOTS regimens have thrice-weekly schedules (Monday-Wednesday-Friday). For cutaneous tuberculosis the recommended treatment involves an intensive phase consisting of Rifampicin (R-450 mg), Isoniazid (H-600 mg) Ethambutol (E-1200mg) and Pyrazinamide (Z-1500 mg) are administered for three days in a week for 2 months. This is followed by the continuation phase in which R-450 mg and H-600 mg given three days in a week as a continuation phase for 4 months [78]. This strategy has been found to be efficacious with most cases responding well by the end of the intensive phase with no reported relapses [64,78]. Depending on the clinical response, the duration of treatment can be extended. For children and adults who weigh less than 30 kg, these drugs are administered according to their body weight.
Lupus vulgaris is the commonest form of cutaneous TB with diverse clinical manifestations. It is important to make a diagnosis and promptly treat as LV can be disfiguring and destructive.
- Patra AC, Gharami RC, Banerjee PK (2006) A profile of cutaneous tuberculosis. Indian J Dermatol 51:105-107.
- Selwyn PA, Sckell BM, Alcabes P, 2021 Copyright OAT. All rights reserv992) High risk of active tuberculosis in HIV-infected drug users with cutaneous anergy. JAMA 268: 504-509. [Crossref]
- Fariña MC, Gegundez MI, Piqué E, Esteban J, Martín L, et al. (1995) Cutaneous tuberculosis: a clinical, histopathologic, and bacteriologic study. J Am Acad Dermatol 33: 433-440. [Crossref]
- Behera B, Devi B, Patra N (2010) Mutilating lupus vulgaris of face: an uncommon presentation. Indian J Dermatol Venereol Leprol 76: 199-200. [Crossref]
- Marcoval J, Servitje O, Moreno A, Jucglà A, Peyrí J (1992) Lupus vulgaris. Clinical, histopathologic, and bacteriologic study of 10 cases. J Am Acad Dermatol 26: 404-407. [Crossref]
- Padmavathy L, Lakshmana Rao L, Pari T, Ethirajan N, Krishnaswamy B (2008) Lupus vulgaris and tuberculosis verrucosa cutis (TBVC)--a clinical, pathological and epidemiological study of 71 cases. Indian J Tuberc 55: 203-209. [Crossref]
- Umapathy KC, Begum R, Ravichandran G, Rahman F, Paramasivan CN, et al. (2006) Comprehensive findings on clinical, bacteriological, histopathological and therapeutic aspects of cutaneous tuberculosis. Trop Med Int Health 11: 1521-1528. [Crossref]
- Tutanc M (2012) The youngest patient of lupus vulgaris; A cutaneous tuberculosis case report. Pak J Med Sci 28: 533-535.
- Acharya KM, Ranpara H, Dutta R, Mehta B (1997) A clinicopathological study of 50 cases of cutaneous tuberculosis in Jamnagar District. Indian J Dermatol Venereol Leprol 63: 301-303. [Crossref]
- Uttawichai P, Igarashi T, Kawana S (2009) Case of lupus vulgaris diagnosed 50 years after onset. J Dermatol 36: 103-105. [Crossref]
- Ghislain E (1957) Lupus vulgaris of buttocks with unusual distribution in a case of renal tuberculosis. Arch Belg Dermatol Syphiligr 13: 260-261. [Crossref]
- Meyer S, Naumann L, Landthaler M, Vogt T (2005) Lupus vulgaris caused by Mycobacterium bovis ssp. caprae. Br J Dermatol 153: 220-222. [Crossref]
- Tan HH, Seow CS (2002) A review of cutaneous granulomas and lupus vulgaris following BCG vaccination in a skin hospital in Singapore. Ann Acad Med Singapore 31: 663-665. [Crossref]
- Farsinejad K, Daneshpazhooh M, Sairafi H, Barzegar M, Mortazavizadeh M (2009) Lupus vulgaris at the site of BCG vaccination: report of three cases. Clin Exp Dermatol 34: e167-169. [Crossref]
- Kiehl P, Eicher U, Vakilzadeh F (1992) A lupus-vulgaris like atypical mycobacteriosis caused by Mycobacterium xenopi (lupus xenopi). Hautarzt 43: 569-575. [Crossref]
- Ghorpade A1 (2003) Lupus vulgaris over a tattoo mark--inoculation tuberculosis. J Eur Acad Dermatol Venereol 17: 569-571. [Crossref]
- Ghorpade A (2006) Tattoo inoculation lupus vulgaris in two Indian ladies. J Eur Acad Dermatol Venereol 20: 476-477. [Crossref]
- Kumar P, Mondal A, Lal NR, Gharami RC (2014) Lupus vulgaris in a child: a complication of ear piercing. Indian J Dermatol Venereol Leprol 80: 97. [Crossref]
- Findlay GH (1987) Bacterial Infections. (1stedn). The Dermatology of Bacterial Infections. Blackwell Scientific, London 71-83.
- Bhutto AM, Solangi A, Khaskhely NM, Arakaki H, Nonaka S (2002) Clinical and epidemiological observations of cutaneous tuberculosis in Larkana, Pakistan. Int J Dermatol 41: 159-165. [Crossref]
- Jaisankar TJ, Garg BR, Reddy BS, Riba B, Ramarao AP (1994) Penile lupus vulgaris. Int J Dermatol 33: 272-274. [Crossref]
- Nimisha E, Gupta G2 (2014) Penile lupus vulgaris: a rare presentation of primary cutaneous tuberculosis. Int J STD AIDS 25: 969-970. [Crossref]
- Eskelund GM (1951) Vitamin D2 therapy of lupus vulgaris of the nasal mucosa. Nord Med 45: 236-238. [Crossref]
- Kaur S, Thami GP, Singhal SK (2003) Lupus vulgaris causing nasal perforation: not a thing of the past. Indian J Dermatol Venereol Leprol 69: 182-183. [Crossref]
- Piatti A (1955) Lupus vulgaris of mucosa and nasal cutis. Arch Ital Otol Rinol Laringol 66: 407-415. [Crossref]
- Laskaris GC, Nicolis GD (1981) Lupus vulgaris of the oral mucosa. Report of 4 cases associated with asymptomatic pulmonary tuberculosis. Dermatologica 162: 183-190. [Crossref]
- Reznik IE (1967) Lupus tuberculosis of the larynx in a child. Vestn Otorinolaringol 29: 113-114. [Crossref]
- Cook CD, Hainsworth M (1990) Tuberculosis of the conjunctiva occurring in association with a neighbouring lupus vulgaris lesion. Br J Ophthalmol 74: 315-316. [Crossref]
- El-Ghatit AM, El-Deriny SM, Mahmoud AA, Ashi AS (1999) Presumed periorbital lupus vulgaris with ocular extension. Ophthalmology 106: 1990-1993. [Crossref]
- Duttaroy DD, Jagtap J, Bansal U, Duttaroy B (2007) Picture of the month--quiz case. Scrofuloderma with lupus vulgaris. Arch Pediatr Adolesc Med 161: 1211-1212. [Crossref]
- Morais P, Ferreira O, Nogueira A, Bettencourt H, Azevedo F (2010) A nodulo-ulcerative lesion on the nose. Dermatol Online J 16: 11. [Crossref]
- Küçükünal A, Ekmekçi TR, Sakız D (2012) "Turkey ear" as a cutaneous maniestation of tuberculosis. Indian J Dermatol 57: 504. [Crossref]
- Vazquez-Lopez F, Fueyo-Casado A, Gonzalez-Lara L (2013) Lupus Vulgaris Erythematoides: report of a patient initially misdiagnosed as dermatitis. Dermatol Online J 19: 18187. [Crossref]
- Bayramgürler D, Sayan M, Aktürk AS, Bilen N, Aslan N, et al. (2007) Disseminated lupus vulgaris presenting with different atypical lesions. J Dermatol 34: 849-851. [Crossref]
- Garg T, Ramchander, Shrihar R, Gupta TP, Aggarwal S (2011) Disseminated lupus vulgaris. Skinmed 9: 125-126. [Crossref]
- Senol M, Ozcan A, Aydin A, Karincaoglu Y, Sasmaz S, et al. (2000) Disseminated lupus vulgaris and papulonecrotic tuberculid: case report. Pediatr Dermatol 17: 133-135. [Crossref]
- Sacchidanand S, Sharavana S, Mallikarjun M, Nataraja HV (2012) Giant lupus vulgaris: A rare presentation. Indian Dermatol Online J 3: 34-36. [Crossref]
- Singal A, Sonthalia S (2010) Cutaneous tuberculosis in children: the Indian perspective. Indian J Dermatol Venereol Leprol 76: 494-503. [Crossref]
- Khandpur S, Nanda S, Reddy BS (2001) An unusual episode of lupus vulgaris masquerading as sporotrichosis. Int J Dermatol 40: 336-339. [Crossref]
- Werschler WP, Elgart ML, Williams CM (1990) Progressive asymptomatic annular facial skin lesions. Cutaneous tuberculosis (lupus vulgaris). Arch Dermatol 126: 1227-1230. [Crossref]
- Heo YS, Shin WW, Kim YJ, Song HJ, Oh CH (2010) Annular lupus vulgaris mimicking tinea cruris. Ann Dermatol 22: 226-228. [Crossref]
- Gönül M, Kiliç A, Külcü Cakmak S, Gül U, Koçak O, et al. (2007) Annular lupus vulgaris: an unusual case undiagnosed for five years. Eur J Dermatol 17: 83-85. [Crossref]
- Hruza GJ, Posnick RB, Weltman RE (1989) Disseminated lupus vulgaris presenting as granulomatous folliculitis. Int J Dermatol 28: 388-392. [Crossref]
- Schulz KH (1957) Disseminated miliary cutaneous tuberculosis & lupus vulgaris in generalized lymph node & pulmonary tuberculosis. Z Haut Geschlechtskr 23: 147-154. [Crossref]
- Naik RP, Srinivas CR, Balachandran C, Narayan PK, Ramnarayan K, et al. (1987) Esthiomene resulting from cutaneous tuberculosis of external genitalia. Genitourin Med 63: 133-134. [Crossref]
- Campanelli CD, Santoro AF, Webster CG, Lee JB (2001) Symmetrically distributed orange eruption on the ears: a case of lupus vulgaris. Cutis 67: 311-314. [Crossref]
- AliaÄŸaoÄŸlu C, Atasoy M, Karakuzu A, Cayir K, MelikoÄŸlu M (2006) Rapidly developing giant sized lupus vulgaris on the chest associated with bilateral scrofuloderma on the neck. J Dermatol 33: 481-485. [Crossref]
- Sehgal VN, Srivastava G, Sharma VK (1987) Lupus vulgaris, caries of the spine and lichen scrofulosorum--an intriguing association. Clin Exp Dermatol 12: 280-282. [Crossref]
- Motswaledi MH, Doman C (2007) Lupus vulgaris with squamous cell carcinoma. J Cutan Pathol 34: 939-941. [Crossref]
- Vora NS, Dave JN, Mukhopadhyay A, Roy K, Patel N, et al. (1995) Basal cell carcinoma in a long standing case of lupus vulgaris. Indian J Dermatol Venereol Leprol 61: 109-110. [Crossref]
- Kate MS, Dhar R, Borkar DB, Ganbavale DR (2009) Longstanding lupus vulgaris with basal cell carcinoma. Indian J Pathol Microbiol 52: 588-590. [Crossref]
- Harrison PV, Marks JM (1980) Lupus vulgaris and cutaneous lymphoma. Clin Exp Dermatol 5: 73-77. [Crossref]
- Dlova NC1 (2010) Lupus vulgaris in an HIV-positive patient. Skinmed 8: 296. [Crossref]
- Pai VV, Naveen KN, Athanikar SB, Dinesh US, Divyashree A, et al. (2014) A clinico-histopathological study of lupus vulgaris: A 3 year experience at a tertiary care centre. Indian Dermatol Online J 5: 461-465. [Crossref]
- Reich A, Kobierzycka M, Cisło M, Schwartz RA, Szepietowski JC (2006) Psoriasiform lupus vulgaris with 30 years duration. Scand J Infect Dis 38: 556-558. [Crossref]
- Padmavathy L, Rao LL, Ethirajan N, Dhanlaklshmi M (2008) Psoriasiform lupus vulgaris. Indian J Tuberc 55: 97-99. [Crossref]
- Fine RM, Meltzer HD (1970) Psoriasiform lupus vulgaris: a case report. Int J Dermatol 9: 273-277. [Crossref]
- Sudip Das GB (2004) Porokeratosis Masquerading As Lupus Vulgaris. Int J Dermatol 49: 212.
- Pandhi D, Reddy BS (2001) Lupus vulgaris mimicking lichen simplex chronicus. J Dermatol 28: 369-372. [Crossref]
- Gilchrist TC, Stokes WR (1898) A case of pseudo-lupus vulgaris caused by a blastomyces. J Exp Med 3: 53-78. [Crossref]
- Hagiwara K, Uezato H, Miyazato H, Nonaka S (1996) Squamous cell carcinoma arising from lupus vulgaris on an old burn scar: diagnosis by polymerase chain reaction. J Dermatol 23: 883-889. [Crossref]
- Frankel A, Penrose C, Emer J (2009) Cutaneous tuberculosis: a practical case report and review for the dermatologist. J Clin Aesthet Dermatol 2: 19-27. [Crossref]
- Kathuria P, Agarwal K, Koranne RV (2006) The role of fine-needle aspiration cytology and Ziehl Neelsen staining in the diagnosis of cutaneous tuberculosis. Diagn Cytopathol 34: 826-829. [Crossref]
- Santos JB, Figueiredo AR, Ferraz CE, Oliveira MH, Silva PG, et al. (2014) Cutaneous tuberculosis: diagnosis, histopathology and treatment - part II. An Bras Dermatol 89: 545-555. [Crossref]
- Hernández Solis A, Herrera González NE, Cazarez F, Mercadillo Pérez P, Olivera Diaz HO, et al. (2012) Skin biopsy: a pillar in the identification of cutaneous Mycobacterium tuberculosis infection. J Infect Dev Ctries 6: 626-631. [Crossref]
- Akoglu G, Karaduman A, Boztepe G, Ozkaya O, Sahin S, et al. (2005) A case of lupus vulgaris successfully treated with antituberculous therapy despite negative PCR and culture. Dermatology 211: 290-292. [Crossref]
- Suthar C, Rana T, Singh UB, Singh M, Ramesh V, et al. (2013) mRNA and DNA PCR tests in cutaneous tuberculosis. Indian J Dermatol Venereol Leprol 79: 65-69. [Crossref]
- Saritha M, Parveen BA, Anandan V, Priyavathani MR, Tharini KG (2009) Atypical forms of lupus vulgaris - a case series. Int J Dermatol 48: 150-153. [Crossref]
- Adamson HG (1920) on the treatment of lupus vulgaris by the liquid acid nitrate of mercury. Br Med J 2: 123-124. [Crossref]
- Costa RO, Macedo PM, Carvalhal A, Bernardes-Engemann AR (2013) Use of potassium iodide in dermatology: updates on an old drug. An Bras Dermatol 88: 396-402. [Crossref]
- Beatty J (1928) Treatment of Lupus Vulgaris. Br Med J 1: 47-48. [Crossref]
- Dowling GB (1957) The present status of vitamin D2 in the treatment of lupus vulgaris. Dermatologica 115: 491-495. [Crossref]
- Kenez J (1964) Finsen and lupus vulgaris. Orv Hetil 105: 2382-2385. [Crossref]
- Rees TD (1957) Surgical repair of lupus vulgaris. Plast Reconstr Surg (1946) 20: 147-154. [Crossref]
- Van KetelW (1965) Treatment And Follow-Up Of Lupus Vulgaris With Isoniazid Only. Ned Tijdschr Geneeskd 109: 849-851. [Crossref]
- Dowling GB, Waddington E, Howell RG, Rees DL (1953) Six cases of lupus vulgaris treated with isoniazid. Proc R Soc Med 46: 163-172. [Crossref]
- World Health Organisation (1993) Treatment of tuberculosis: Guidelines for national Programmes: 1-43.
- Rama Rao GR; Sridevi, Narayan BL, Amareswar A, Sandhya S (2011) Directly observed treatment short course and cutaneous tuberculosis: our experience. Indian J Dermatol Venereol Leprol 77: 330-332. [Crossref]





