Abstract
A 55-year-old man was scheduled to get a L4-5 decompression surgery due to spinal stenosis. He received occipitocervical fusion because of traffic accident in 1999 and he had cleft palate of 3*5 cm and his nasal opening also showed abnormality. As there was a concern about the difficult airway, awake intubation using fiberoptic bronchoscope was considered. After the patient was sedated, oral fiberoptic intubation was attempted. But, unexpectedly when the bronchoscope fell into the nasal cavity through cleft palate, it became difficult to get a view and thus it was also difficult to find a normal structure. After about 5 minutes of attempt, his sedation deepened and his oxygen saturation gradually decreased to less than 90%. After oxygen saturation was secured 100% with assisted ventilation, intubation was attempted by using Glidescope. It was difficult to get a proper view and insert endotracheal tube, but intubation was successful when the second attempt was conducted. After then, 100 mg of propofol and 50 mg of esmeron were administered and general anesthesia was performed by using desflurane. After about 1 hour, surgery ended and the patient’s spontaneous respiration was recovered sufficiently. After observing him obeying our command, his tube was removed. He was transferred to a recovery room and when all of his vital signs were observed to be stable, he was instructed to leave the room.
Key words
occipitocervical fusion, cleft palate, fiberoptic intubation, glidescope
Introduction
Occipitocervical fusion is carried out in case of occipitocervical junction instability such as antlanto-axial fracture or dislocation. After the procedure, the movements of cervical vertebrae are limited, which may make endotracheal intubation difficult. Awake fiberoptic endotracheal intubation (FOI) is one of the most frequently chosen procedures when a difficult intubation by direct laryngoscopy is expected [1]. But, in case of patients with cleft palate, an unanticipated difficulty can be caused by the anatomical defect during FOI. In this case, we are to report the difficulties in airway management experienced by the patients with both occipitocervical fusion and cleft palate.
Case report
A 55-year-old man was scheduled to get a L4-5 decompression surgery due to spinal stenosis. He received occipitocervical fusion because of traffic accident in 1999 and so his occipitocervical joint was almost immobilized and his mouth opening was limited to moderate degree. And he had cleft palate of 3*5 cm and his nasal opening also showed abnormality (Figure 1). In the radiograph, his tongue base was displaced posteroinferiorly, thus covering the epiglottis, which narrowed the oropharyngeal space (Figure 2).
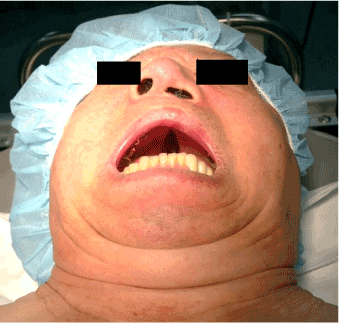
Figure 1. General appearance with mouth opening. Cleft palate and nasal opening deformity are observed.
As there was a concern that it would be difficult to keep airway patent when the muscle relaxation led to the loss of spontaneous respiration, awake intubation was considered. Fiberoptic bronchoscope, which may give less pain and stimulation to patients compared to the direct laryngoscope, was preferentially selected, and oral fiberoptic intubation was conceived to be appropriate due to abnormal nasal opening. Besides bronchoscope, for immediate use in case of FOI failure, I-gel, Glidescope, light wand, and laryngeal mask airway (LMA) were prepared. Continuous intravenous infusion began with dexmedetomidine of 1 mcg/kg/min and remifentanil of 0.5 mcg/kg/min, and during sedation, arterial line was secured for hemodynamic monitoring and arterial blood gas analysis. Topical anesthesia of pharynx was carried out using 5% lidocain spray, and oxygen was supplied through nasal canulae. After about 10 minutes, he became sedated, but when he was called, he could open his eyes, and thus intubation was attempted using fiberoptic bronchoscope. But, unexpectedly, when the bronchoscope fell into the nasal cavity through cleft palate, it became difficult to get a view and thus it was also difficult to find a normal structure.
To prevent the tip of the scope from being trapped, bronchoscope was inserted with endotracheal tube, but due to cleft palate and narrowed oropharyngeal space, it was difficult to operate. After about 5 minutes of attempt, his sedation deepened and his oxygen saturation gradually decreased to less than 90%. As he was still able to cooperate, assist ventilation was conducted using oxygen mask to have him take a deep breath for about 1 min. Oxygen saturation was secured 100% and after a sufficient time passed, intubation was attempted by using Glidescope. It was difficult to get a proper view and insert endotracheal tube, but intubation was successful when the second attempt was conducted (Figure 3). After then, 100 mg of propofol and 50 mg of esmeron were administered and general anesthesia was performed by using desflurane. After about 1 hour, surgery ended and the patient’s spontaneous respiration was recovered sufficiently. After observing him obeying our command, his tube was removed. He was transferred to a recovery room and when all of his vital signs were observed to be stable, he was instructed to leave the room.
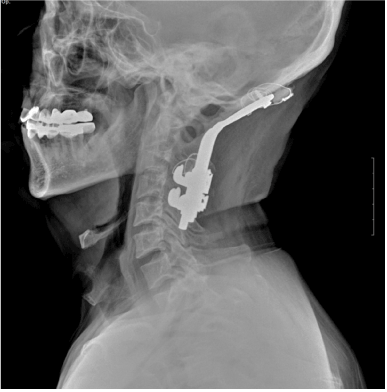
Figure 2. Radiograph of the side of the cervical vertebral portion. Immobilized occipitocervical junction and tongue base are overridden on the upper side of the hyoid bone.
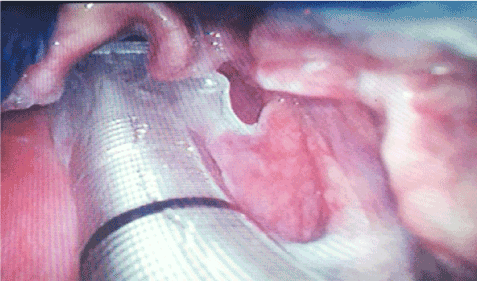
Figure 3. Intubation using Glidescope
Discussion
Cleft lip and/or cleft palate are the most common congenital anomalies in the oral and maxillofacial region. The overall incidence of orofacial clefting is about one in 700 live births, and the incidence of isolated cleft palate is approximately 0.5 per 1,000 live births [2]. If oral fiberoptic intubation is attempted into a patient in a supine position by using bronchoscope, the range of manipulation is limited to the tip of bronchoscope and more proximal part slides along the hard palate and enters the pharynx and larynx. But, in this patient’s case, the scope fell into the nasopharynx through cleft palate and so it was difficult to find a normal structure. Also, as shown in the photo, his nasal opening was also severely deformed and so nasal fiberoptic intubation was also hardly possible. It is conceived to be relatively free from the disturbance caused by cleft palate if attempting oral FOI in a sitting position, but it would be difficult to say that it is always a favorable method. It depends on operator’s preference and degree of skill. It is necessary to be careful for patients with cleft palate accompanied during intubation by using bronchoscope and it is also necessary to consider the other options sufficiently in preparation for failures.
Fixation of occpitocervical junction can cause life-threatening upper airy obstruction and, even after the procedure, can be a big obstacle to an anesthesiologist [3,4]. In this case, the angle between laryngeal and pharyngeal axes was steep, mouth opening was restricted, and mandible pressurized the upper side of the epiglottis when he opened his mouth, which restricted the space and visibility significantly. This caused a significant difficulty in every step of endotracheal intubation.
Occipitocervical fusion was conducted in upper cervical spine, and as the larynx was located underneath it, neck flexion, although chin up wouldn’t be possible, would be a little helpful for getting a view and carrying out intubation. Also, as the space for tube handling in both oral cavity and orpharyngeal area is significantly limited, it is necessary to pay much attention to making appropriate curvature with a tube by using stylet before attempting intubation. In preparation for the worst, help can be sought from a man of experience to carry out endotracheal intubation with readiness for emergency invasive airway access. In the patient whose upper airway obstruction is highly anticipated, extubation with a tube exchanger might be a good choice [4].
Despite this bad condition, Glidescope is very helpful equipment. Although the blade designed thick when camera lens was installed gave a difficulty to manipulation due to a narrow mouth opening, it was possible to get a proper view that could have been impossible if using direct larygoscope. The combination of dexmedetomine and remifentanil had the effect of strong sedation and pain control. During a series of process of manipulating Glidescope blade, getting a proper view, and attempting intubation, the patient showed the level of consciousness enough to hold eye contact, but did not show gag reflex or big pain. But, temporarily, his oxygen saturation dropped and thus it was considered that it would be necessary to pay a little more attention to the adjustment of dosage.
In summary, awake fiberoptic intubation is one of the best procedures for a difficult airway, but may face unexpected difficulty if it is accompanied with cleft palate. In this case, awake intubation using Glidescope under sedation can be a good alternative.
References
- Sdrales LM, Miller RD, Sdrales LM (2013) Miller’s anesthesia review. Maryland Heights. MO: Elsevier/Saunders.
- Goodacre T, Swan MC (2008) Cleft lip and palate: current management. Paediatr Child Health 18: 283–292.
2021 Copyright OAT. All rights reserv
- Matsushita K, Morikawa K, Sumie M, Sakaguchi Y, Hoka S (2013) [Acute upper airway obstruction after extubation due to excessive anteflexion of the neck with occipitocervical fusion]. Masui 62: 168–171. [Crossref]
- Tagawa T, Akeda K, Asanuma Y, Miyabe M, Arisaka H, et al. (2011) Upper airway obstruction associated with flexed cervical position after posterior occipitocervical fusion. J Anesth 25: 120–122. [Crossref]



