Introduction: There is a strong relationship between infectivity with Human Immunodeficiency Virus (HIV) and Herpes Simplex Virus (HSV); however the process leading to chronic herpetic lesions in HIV is still under investigation.
Case report: There is evidence that patients receiving highly active antiretroviral therapy (HAART) may be more prone to chronic ulcers than those not receiving therapy. We present a case of a 35-year-old HIV-infected African American woman with a chronic herpetic ulcer of over 2 years duration, and suggest that her anti-retroviral therapy is enabling her immune system to mount an ongoing attack against the herpes virus resulting in a chronic non-healing ulcer.
Conclusion: Immune reconstitution inflammatory syndrome (IRIS) should be considered when a patient on HIV therapy presents with a chronic herpetic lesion.
Chronic herpetic genital ulcerations have become more prevalent since the start of the Human Immunodeficiency Virus (HIV) epidemic and the relationship between these two viruses is increasingly important. Although more cases of chronic herpetic ulcers are being described in HIV infected individuals, the mechanism behind this ongoing tumor-like inflammation has yet to be fully determined [1]. In this case report we describe an abnormally prolonged vulvar ulcer and explore the impact that the HIV therapy may have on the clinical manifestation.
A 35-year-old African American woman with known vertically transmitted HIV infection diagnosed at age 16 presented to the gynecologists with a chief complaint of a non-healing vulvar ulcer of over 2 year duration. Examination revealed a 4x4cm non-tender and non-pruritic vulvar ulcer with indurated borders (Figure 1). Areas of depigmentation, atrophic labia minora, small stenotic vaginal introitus and a scar on the clitoris are also visible on the external genitalia. In June 2014 absolute CD4+ count was 490-1740 cells/uL and Herpes Simplex Virus (HSV) immunostain of the ulcer was positive. Patient was on highly active antiretroviral therapy (HAART) during this time. Patient was instructed to avoid sexual intercourse and she was put on Acyclovir 400 mg PO three times daily and acyclovir cream. The ulcer healed and she was left on acyclovir 400 mg PO daily as suppressive therapy and is responding well.
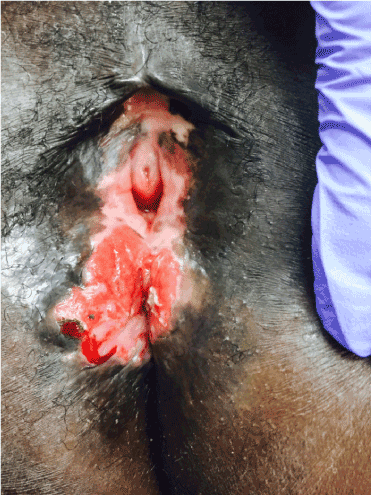
Figure 1. Chronic vulvar herpetic ulcer in HIV-infected patients on HAART.
This case report is unique, even among the other cases of chronic herpetic vulvar ulcers in an HIV-infected patient, due to the prolonged duration of the ulcer of over 2 years. In a report on 29 cases of chronic (greater than 1 month) genital ulcers in HIV patients, the etiology was Herpes in the majority of cases [2] and other studies found that co-infection in certain populations is as high as 50% to 90% [3]. Since the introduction of HAART, mortality rate has decreased but it has lead to a new phenomenon known as immune reconstitution inflammatory syndrome (IRIS), in which clinical deterioration occurs soon after the initiation of HAART due to the return of the body’s ability to effectively mount an immune response against a pathogen [4].
Although this patient’s HAART therapy is protecting her against opportunistic infections, emerging evidence has shown that it increases the likelihood of genital herpes. A retrospective cohort study of 1,551 HIV-infected patients showed that after controlling for the confounders of age, gender and CD4 counts, patients receiving HAART for less than 6 months had a higher incidence of active genital herpes than those not receiving therapy [5]. Because IRIS is the result of the restoration of an immune response against a causative agent, definitive treatment is the removal of the agent. Reports have demonstrated complete elimination of chronic herpetic ulcers following treatment with oral acyclovir [6,7]. IV foscarnet or IV valacyclovir are effective in situations where acyclovir had been unsuccessful at eliminating the ulcer [7]. Our patient responded well to PO acyclovir; Figure 2 is eight weeks after initiation of treatment. The patient was left on prophylactic dose without recurrence in over one year.
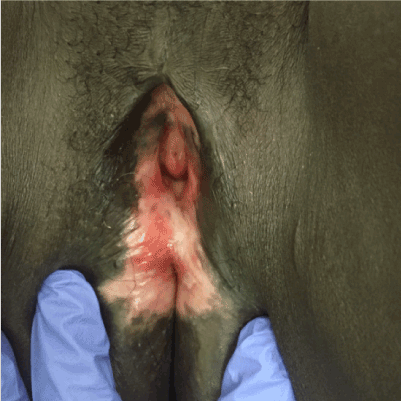
Figure 2. Herpetic lesion eight weeks after initiation of treatment with Acyclovir.
This is an original case report of interest to dermatologists, gynecologists, infectious disease and general physicians. In short, IRIS should be considered a possible cause of healing delay in patients on HAART with chronic vulvar herpetic lesions. Physicians should educate their patients who are on HAART about the possibility of a prolonged presentation of genital ulcers, and the importance of early identification and treatment of the causative organism.
Funding: This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Disclosures: Jeffrey B. Morris, Eric L. Maranda, Christopher Mancuso and Jose A. Carugno declare that they have no conflict of interest.
- Bosamiya SS (2011) The immune reconstitution inflammatory syndrome. Indian J Dermatol 56: 476-479. [Crossref]
- Gbery IP, Djeha D, Kacou DE, Aka BR, Yoboue P, et al. (1999) [Chronic genital ulcerations and HIV infection: 29 cases]. Med Trop (Mars) 59: 279-282. [Crossref]
- Strick LB, Wald A, Celum C (2006) Management of herpes simplex virus type 2 infection in HIV type 1-infected persons. Clin Infect Dis 43: 347-356. [Crossref]
- Shelburne SA 3rd, Hamill RJ, Rodriguez-Barradas MC, Greenberg SB, Atmar RL, et al. (2002) Immune reconstitution inflammatory syndrome: Emergence of a unique syndrome during highly active antiretroviral therapy. Medicine (Baltimore) 81: 213–227. [Crossref]
2021 Copyright OAT. All rights reserv
- Couppié P, Sarazin F, Clyti E, El Guedj M, Vaz T, et al. (2006) Increased Incidence of Genital Herpes after HAART Initiation: A Frequent Presentation of Immune Reconstitution Inflammatory Syndrome (IRIS) in HIV-Infected Patients. AIDS patient care STDS 20: 143-145. [Crossref]
- Palamaras I, Richardson D, Healy V, Lyons D, Byrne M, et al. An atypical herpetic vulval ulcer in an African woman: an important lesson. Int J STD AIDS 17: 427-428. [Crossref]
- Mosunjac M, Park J, Wang W, Tadros T, Siddiqui M, et al. (2009) Genital and perianal herpes simplex simulating neoplasia in patients with AIDS. AIDS Patient Care STDS 23: 153-158. [Crossref]


