Abstract
The aim of this article is the analysis of a multidisciplinary developed first prototype of an innovative Arm‐Support‐Device (ASD) for laparoscopic surgery. This device follows the motions of the leaned lower arm of the surgeon and supports the posture in order to relief the surgeon. During the multidisciplinary development process, important requirements of surgeons from gynecology and urology were compiled. Requirements like physical relief and usability‐enhancement when using comparable techniques are shown in some studies. The fulfillment of further important requirements concerning the human‐machine‐interaction between surgeon and ASD as well as the effects of the ASD on the body‐, arm‐ and hand‐posture of the surgeon are analyzed in this study. Therefore 12 surgeons performed simulated laparoscopic static and dynamic tasks on a so‐called pelvi‐trainer in laboratory‐setting using the developed ASD and without using the ASD. For analysis life‐record data from two perspectives (frontal and sagittal), the method of thinking aloud and the interview were used. The analysis shows that body‐, arm‐ and hand postures of the surgeons are mainly similar independent of the use of the ASD. The surgeons used the ASD intuitively for getting in, operating and getting out, which were important requirements. Nevertheless a familiarization is necessary. It is expected that some deficits of the ASD‐prototype can be avoided in the possible next step of developing an end‐design‐product by using the results of this study. These deficits are skidding down of the arm of the surgeon from the support for some steeper arm‐postures and rarely appearing collision of the support with the fixed endoscope.
Key words
arm‐support‐device, armrest, laparoscopic surgery, body‐, arm‐ and hand‐posture, usability, multidisciplinary development
Introduction
Analysis of the popular and because of its advantages for the patient important laparoscopic surgery shows ergonomic deficits which provide opportunities for optimization. Many studies showed physical strain and fatigue of the neck, back and shoulder of surgeons/assistants resulting from the forced static uncomfortable and exhausting arm‐ and body‐posture among other things [1‐9]. A further aspect is the higher physical stress with its possible negative influence on the operating quality because of the adaptation to the ergonomic situation in laparoscopic surgery [7].
The multidisciplinary “Industry‐on‐Campus‐Project” aims to improve especially the physical stress and strain in laparoscopic surgery. The team consists of clinical partners, engineers and occupational health physicians as well as industrial partners. This consortium was an important aspect for the systematic development of the prototype of the Arm‐Support‐Device (ASD) using the engineering methodology of the VDI 2221 [10,11]. This method suggests the approach of defining tasks, conception, draft and workout for the development of technical products. Results from the initial analysis of ergonomics of surgeons and assistants during laparoscopic interventions in urology and gynecology and many discussions were used for gaining important requirements for the development of a first ASD‐prototype without a real end‐product‐design. In order to meet the important requirement of maintaining the current operating technique and instruments with direct haptic feedback, the ASD is made as a moveable armrest which follows and supports the surgeons’ arm while taking the posture [10]. Further important requirements for the developed ASD mentioned by the surgeons were besides the reduction of the physical strain and enhancing the performance (analyzed in [12], not in this article), the intuitive use of the ASD and possible fast getting out from the system in case of emergency [10].
The fulfillment of the mentioned last requirements (intuitive use and fast getting out) and the body‐, arm‐ and hand‐postures while using the ASD are the analyzed aspects of the presented evaluation in this article, which was made with 12 surgeons in laboratory setting. Consequently, the main objective of this study is the analysis of body‐, arm‐ and hand‐posture of the surgeons in dependence of the ASD. The second objective of this study is the analysis of the human‐machine‐interaction between surgeon and ASD. Human‐machine‐interaction means in this context, the interaction (recognition of the interface, behavior, use) between the surgeon and the ASD with and without using instruments for performing laparoscopic tasks. Besides the important analysis of the physical stress and usability, which was shown in some similar studies [13‐15], it is important to analyze the human‐machine interaction between surgeon and ASD, because of the acceptance of the system and to get further information towards an end‐design‐product.
The article will show the used methods and results of the evaluation with focus on posture and the use and end with a conclusion/discussion.
Materials and methods
The content of the whole study was to analyze physical stress, number of errors and needed time for performing pre‐defined tasks [12] as well as the qualitative analysis of body, arm‐, hand‐posture and the human‐machine‐interaction when using the ASD, which is the focus and limitation of this article. The results of the study concerning physical stress, number of errors and needed time for performing the pre‐defined tasks are shown in [12].
Type of participants
The ASD‐prototype was evaluated by twelve experienced surgeons in laboratory setting. Seven surgeons were from gynecology and five surgeons from urology, whereby two surgeons were female and ten surgeons male.
Design of the tasks
The evaluation consisted of two appointments. The aim of the first appointment was to get a first experience of using the ASD and performing the tasks. This took approximately 1 to 2 hours. This should avoid the influence of learning effects on the evaluation and deliver more realistic results for the main analysis at the second appointment. This appointment was made on another day.
The surgeons performed two different laparoscopic tasks at a covered pelvi‐trainer on a heightadjusted table in order to simulate laparoscopic interventions. These tasks were performed with and without using the ASD based on a randomization. The position of the endoscope in the pelvi‐trainer was adjusted for every surgeon before the task and was fixed during the task[12].There were situations during the task, where the position of the endoscope was adjusted again, if the surgeon needed it. The gripper instrument was put in the pelvi‐trainer before the tasks and was freely movable in the appropriate rubber reception of the pelvi‐trainer (Figure 1).
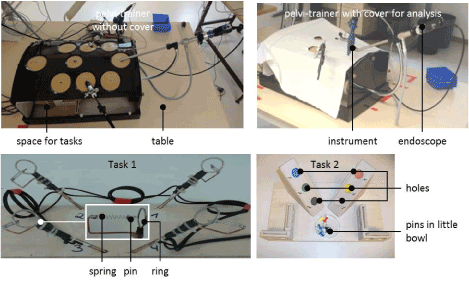
Figure 1.Pelvi-trainer and the two different tasks for simulation of laparoscopic interventionsTasksprepared by UKT.
Task 1 was performed only with the right arm / hand holding a gripper instrument and simulated a static situation with focus on precision, where a metal sleeve with a hole‐diameter of 4 mm was put over a relevant pin through a ring with 20 mm diameter. The pin was fixed on a stored spring and the aim of the task was not to contact the ring. This construction consisted of 4 different positions in order to allow different (extreme) body and arm postures similar to real laparoscopic interventions (Figure 1)[12].
Task 2 was performed with both arms/hands holding two gripper instruments with the aim to simulate a dynamic situation with focus on fast performance. The subjects should take a pre‐defined pin from the little bowl with one instrument and give it to the second instrument. Then the pin should be put in the appropriate pre‐defined hole. This was made for six pins and afterwards the pins were taken from the hole with one instrument, given to the second instrument and then put back in the little bowl (Figure 1)[12].
Design of methods
Life‐record‐data from two perspectives was used in order to analyze body‐, arm‐ and hand‐posture as well as the use (one part of interaction) of the ASD. One camera was positioned in front of the surgeon in order to record the frontal plane of the surgeon, especially the hand‐arm‐system (left and right) and the body. The second camera was positioned right beside the surgeon in order to analyze the right hand‐arm‐system in the sagittal plane of the surgeon (Figure 2).

2021 Copyright OAT. All rights reserv
Figure 2. Setting when using Arm-Support-Device.
The methods of thinking aloud during the performance of the tasks as well as an expert interview afterwards were used in order to get further information about the human‐machine‐interaction between surgeon and ASD.
Approach of operation of the Arm‐Support‐Device
The surgeon’s proximal lower arm leans [16] on the support of the ASD like on an armrest to get into the ASD. By doing this, the ASD is activated and follows the motions of the lower arm with 5 DOF (degree of freedom) as shown in figure 2. Then he picks up the instrument with his hand and performs the tasks. In order to get out of the ASD, the surgeon raises his arm quickly and the ASD stands still [10].For further information about the ASD please look at [10]. Figure 2 shows a situation, when the ASD supports the surgeon.
Results
The results shown in this paragraph refer to the main experiment.
Body‐, arm‐ and hand‐posture
The results of the body‐, arm and hand‐posture are based on the analysis of the life‐record data of the frontal and sagittal view at the surgeons performing the experimental tasks. Four similar situations for task 1 (four positions, Figure 1) and six similar situations for task 2 (put down blue pin/before picking up the red pin/put down red pin/pick up blue pin/pick up red pin from hole/put red pin in little bowl) were compared with and without using the ASD for every surgeon. The results of body‐, arm‐ and hand‐posture base on the analysis of these situations.
Figure 3 shows an exemplary result for one surgeon analyzing the frontal and sagittal view with and without using the ASD for three situations, because this result is similar transferable to the other surgeons and situations. Situation one is putting down the blue pin, situation two is before picking the red pin and situation three is putting down the red pin. In the frontal view the body‐ and arm posture can be analyzed. The arm posture is defined in this view by the arm abduction angle (α not using ASD, β using the ASD). In the sagittal view the flexion‐angle between the upper and lower arm (γ not using ASD, δ using ASD) and the ulnar‐ /radial‐abduction‐angle of the hand (ε not using ASD, η using ASD) can be analyzed.

Figure 3. Body-, arm- and hand-posture with and without using Arm-Support-Device - frontal and sagittal view of an exemplary surgeon for three different situations.
Body‐, arm‐ and hand‐posture of the surgeons were mainly similar for the performance of both tasks (static and dynamic) when using and not using the ASD (Figure 3). For all surgeons (12 from 12), the arm abduction angle β (using ASD) was sometimes slightly higher than the arm abduction angle α (not using ASD) for the left and the right arm while performing both tasks. The analysis of the frontal view showed for 9 from 12 surgeons slightly higher inclination of the body towards the support while performing task 1 (static task with one arm) when using ASD compared to the unsupported situation. The flexion‐angle (γ not using ASD, δ using ASD) was mainly similar for 9 from 10 sagittal analyzed surgeons independent of the use of the ASD for both tasks (sagittal life‐record‐data of 2 surgeons couldn’t be analyzed). Thus, the arm‐posture in sagittal view was mainly similar. The ulnar‐ / radialabduction‐ angle of the hand (ε not using ASD, η using ASD) and consequently the hand‐posture were mainly similar for 12 from 12 surgeons independent of the use of the ASD for both tasks.
Qualitative analysis of the Human‐Machine (ASD)‐Interaction
The observation and the interview showed that getting in the system as well as the getting out (theuse of the ASD) of the system was made intuitively by the surgeons after presentation by theresearcher at the first appointment. The human‐machine‐interface was recognized by the surgeonsand the movements (the use of the ASD) were made intuitively although it is only a prototype andnot an end‐product‐design. They leaned intuitively the middle of the lower arm or the proximal partof the lower arm on the support.
According to the interviews the support was generally perceived as comfortable, but for steeperangles of the lower arm (higher flexion angle δ) the surgeons proposed a higher friction betweensupport and arm. It was observed in the life‐record data that for steeper angles the arm of somesurgeons skidded from the support. In the study the naked lower arm of the surgeons leaned on thesupport. In the real OR (operating room), they would have surgical gowns, and consequently anotherfriction coefficient. One surgeon mentioned that he would wish a tighter U‐Form of the support.
The observation showed temporary collisions of the lower arm / hand with the static endoscope for 6from 12 surgeons with and without using the ASD. Consequently these collisions can’t be justified by the use of the ASD. Infrequent collisions between support and the fixed endoscope were observedfor 4 from 12. Collision between pelvi‐trainer and the support wasn’t observed.
During the performance of the tasks, the surgeons had partly problems to see the picture sent by the endoscope to the monitor. The surgeons adjusted the endoscope partly by themselves and used the ASD for this. Thus, the ASD was used intuitively for this unpredictable situation. The surgeons didn’tleave the ASD in this case.
Discussion and conclusion
The results show that the postures are similar performing the tasks with or without ASD. According to the DIN EN 1005‐4 the supported postures are acceptable regarding the health risk, because themaximal supported static arm‐abduction‐angle isn’t higher than 60°. The unsupported static posture isn’t optimal for higher arm‐abduction‐angle than 20° [17]. The similar body‐, arm‐ and hand postures independent of the use of the ASD may be explained by the intuitiveness when using the system with its five DOF (Degree Of Freedom).
In reality the endoscope is moved by the assistant (or an assistance system), so that the mentionedcollisions might be avoided. This was said by one surgeon. The construction of the support can bemore compact in an end‐design‐product, so that the collision between support and endoscope canbe avoided. The placement of the ASD in the OR was discussed in [10] and can be adapted in the nextpossible step of construction of the compact and optimized end‐design‐product.
The important requirement of fast getting out of the system, (e. g. in case of emergency situations), can be fulfilled, because the surgeons left the system intuitively after the introduction into thesystem. The intuitive recognition of the support and use are indicators for the high self‐explanatoryand the low operating‐complexity of the ASD. The fact, that the surgeons used the ASD intuitively inthe shown unpredictable situations without getting out of the system shows that there is theintention of comfort and trust to the ASD. Every assistance device needs the trust of his user. Afamiliarization is necessary, but the observed intuitive use of the ASD may be an indication for a fastfamiliarization to an optimized future‐system. This should be tested by using the system for a longerperiod in a possible next step. The short time for performing the tasks was a limitation.
There are few studies which evaluated armrests in laboratory setting for laparoscopic tasks. Galleanoet al.[14] used a horizontally movable armrest and showed positive effects on the reduction of thesignificant trapezius muscle as well as the reduction of the error rate for the tasks and thediscomfort. Jafri et al.[13] used an armrest which is moveable in the horizontal plane and also showedpositive effects on the error rate and lower energy consumption. Consequently the armrest is apossibility to reduce the physical strain and enhance the quality in laparoscopic surgery. But noresearch was found focusing on the posture while using an ASD for laparoscopic tasks, which followsand supports at the same time the spatial motions of the lower arm of the surgeon and thusenhances the mobility of application. Odellet al.[15] mentioned differences in behavior when using anmovable armrest for a mousing task (not laparoscopic task) regarding the wrist posture incomparison to the unsupported situation. Furthermore no research was found concerning the abovementioned intuitiveness of using and recognizing such an ASD. Galleanoet al.[14] showed that subjectsleaned different parts of the forearm on horizontally movable armrest and that some subjects didn’t keep their forearms on the armrest for the whole time. According to Jafriet al.[13] 12 from 16 surgeonsfavored using a horizontally movable armrest during his evaluation.
It was important to analyze the requirements of the surgeons in order to enhance the experience insuch a kind of assistance device for surgery. Some different experience exists already, like from Odellet al.[15] who gives some important feedback for the design of forearm support devices in generalwithout special attention to surgery or from Galleanoet al.[14] and Jafriet al.[13] who focus on surgery.
Acknowledgement
The study is a component of the “Industry on Campus” project IoC‐103 (MinisteriumfuerWissenschaft, Forschung und Kunst Baden Wuerttemberg, induced by InteruniversitaeresZentrumfuermedizinischeTechnologien Stuttgart‐Tuebingen) with the title “InteraktionsbasiertemanipulatorgestützteAssistenz” in cooperation with FESTO and TRUMPF Medical.
References
- Gofrit ON, Mikahail AA, Zorn KC, Zagaja GP, Steinberg GD, et al. (2008) Surgeons' perceptions and injuries during and after urologic laparoscopic surgery. Urology 71: 404-407. [Crossref]
- Karlovic K, Pfeffer S, Maier T, Sievert K, Rothmund R, et al. (2014) Analysis and comparison of ergonomics in laparoscopic and open surgery – a pilot study.V.G. Duffy: Digital Human Modeling. Applications in Health, Safety, Ergonomics and Risk Management, Human Computer Interaction International, Vol 8529 of the series lecture notes in computer science 273-281. CretaMaris,Heraklion, Crete, Greece June 2014. Springer International Publishing.
- Karlovic K, Pfeffer S, Maier T, Sievert K, Rothmund R (2014) Human Factors View of theAssistant at Laparoscopic Procedures – A Pilot Study. Advances in Human Ascepts of Healthcare, Proceedings of the 5th International Conference on Applied Human Factors and Ergonomics: 345-351, Karkow, Poland, July 2014.
- Pfeffer S, Hofmann A, Maier T, Rothmund R, Sievert KD, et al. (2013) Ergonomics of Selected Laparoscopic Procedures - Need for Action? Biomed Tech (Berl). [Crossref]
- Miller K, Benden M, Pickens A, Shipp E, Zheng Q (2012) Ergonomics principles associated with laparoscopic surgeon injury/illness. Hum Factors 54: 1087-1092. [Crossref]
- Hubert N, Gilles M, Desbrosses K, Meyer JP, Felblinger J, e al. (2013) Ergonomic assessment of the surgeon's physical workload during standard and robotic assisted laparoscopic procedures. Int J Med Robot 9: 142-147. [Crossref]
- Berguer R, Rab GT, Abu-Ghaida H, Alarcon A, Chung J (1997) A comparison of surgeons' posture during laparoscopic and open surgical procedures. SurgEndosc 11: 139-142. [Crossref]
- Quick NE, Gillette JC, Shapiro R, Adrales GL, Gerlach D, et al. (2003) The effect of using laparoscopic instruments on muscle activation patterns during minimally invasive surgical training procedures. SurgEndosc 17: 462-465. [Crossref]
- Nguyen NT, Ho HS, Smith WD, Philipps C, Lewis C, et al. (2001) An ergonomic evaluation of surgeons' axial skeletal and upper extremity movements during laparoscopic and open surgery. Am J Surg 182: 720-724. [Crossref]
- Karlovic K, Pfeffer S, Maier T, Heidingsfeld M, Ederer M, et al. (2015) Effects on performance when using a Posture Assistance Device – results of a usability evaluation in laboratory setting. 6th International Conference on Applied Human Factors andErgonomics (AHFE 2015) and the Affiliated Conferences 3: 1395-1402. Las Vegas, USA, July 2015. Elsevier B.V.
- Steinhilber B, Hoffmann S, Karlovic K, Pfeffer S, Maier T, et al. (2015) Development of an arm support system to improve ergonomics in laparoscopic surgery: study design and provisional results. SurgEndosc 29: 2851-2858. [Crossref]
- Steinhilber B, Seibt R, Kustermann A, Rieger MA, Karlovic K, et al. (in press) Ein Arm-Stütz-System fürlaparoskopischtätigeChirurgen: Evaluation auf vorklinischerEbene. Arbeit in komplexenSystemen. Digital, vernetzt, human?!, 62. Frühjahreskongress der GeselllschaftfürArbeitswissenschaft (GfA). Aachen, 2016 (accepted for publication).
- Jafri M, Brown S, Arnold G, Abboud R, Wang W (2013) Energy consumption during simulated minimal access surgery with and without using an armrest. SurgEndosc 27: 971-977. [Crossref]
- Galleano R, Carter F, Brown S, Frank T, Cuschieri A (2006) Can armrests improve comfort and task performance in laparoscopic surgery? Ann Surg 243: 329-333. [Crossref]
- Odell D, Barr A, Goldberg R, Chung J, Rempel D (2007) Evaluation of a dynamic arm support for seated and standing tasks: a laboratory study of electromyography and subjective feedback. Ergonomics 50: 520-535. [Crossref]
- Bullinger HJ, Solf JJ (1979) ErgonomischeArbeitsmittelgestaltung I–Systematik. ForschungsberichtNr. 196 BundesanstaltfürArbeitsschutz und Unfallforschung Dortmund. Bremerhaven: Writschaftsverlag NW.
- DIN EN 1005‐4. Januar 2009, Sicherheit von Maschinen–MenschlichekörperlicheLeistung–Teil 4: Bewertung von Körperhaltungen und Bewegungenbei der ArbeitanMaschinen.


 2021 Copyright OAT. All rights reserv
2021 Copyright OAT. All rights reserv
