Dealing with stress is of central importance. Lately, smartphone applications (apps) are deployed in stress interventions as they offer maximal flexibility for users. First results of experimental studies show that anti-stress-apps effect subjective perception of stress positively. However, current literature lacks studies on physiological stress reactions (e.g., cortisol), although they are of special interest to health issues. Therefore, the aim of this study was to investigate, for the first time, the effectiveness of an anti-stress-app in chronic and acute stress reduction on a physiological (cortisol) and psychological level (subjective perception of stress) in comparison to a face-to-face and a control group in a pre-post design. Sixty-two participants took part in the pretesting procedure (dropout of 53 %). Based on age, gender, physical activity and subjectively perceived acute stress due to the Trier Social Stress Test for Groups (TSST-G) as well as based on subjectively chronic stress assessed during the pretest, participants were matched in three groups (anti-stress-app: n = 10, face-to-face: n = 11, control group: n = 9). After six weeks of the cognitive-based resource-oriented intervention, participants were exposed to the TSST-G for post testing. Results did not show a change of cortisol secretion or cognitive appraisal of the acute stressor. Further, no changes were detected in the chronic physiological stress reaction. Possible causes are discussed.
transactional model of stress, Trier Social Stress Test, psychophysiology, stress perception
In a survey from 2017, three in ten Americans reported an increase of stress in the past year and 20% reported experiencing extreme stress [1]. The development of new ways to deal with stress at work and in everyday life is therefore a crucial challenge. Recently, smartphone applications (i.e., apps) have been increasingly deployed in the field of stress interventions due to its flexibility for users concerning time and location and to the fact that they are notably more cost-effective than well-established face-to-face stress interventions [2]. Results show that anti-stress-apps have a positive effect on subjective well-being [3]. However, so far there are no studies that compared the impact of anti-stress apps with control groups or integrated physiological aspects of stress reactions. Physiological reactions are of special interest because multidimensional comprehension of stress is only possible by assessing additional objective parameters and because stress hormones such as cortisol can have negative consequences on the immune system [4]. Therefore, the aim of this study was to investigate the effectiveness of an anti-stress-app regarding reduction of chronic and acute stress both at the physiological (i.e., cortisol) and at the psychological (i.e., subjective perception of stress) compared to a face-to-face stress intervention and a control group.
According to the Transactional Model of Stress, a psychophysiological reaction results when the demands of a relevant stressor exceed a person’s own appraisal of resources [5]. The negative impact of stress can be manifold: Acute stress can lead for instance to a decrease in performance and chronic stress may impact general health seriously [6,7]. Long-term-effects of chronic stress may also lead to considerable restriction of life and workplace quality and consequently represent a burden to society [2,8].
Well-established stress intervention programs are mainly conducted in group settings and consist of cognitive-behavioral skill training and/or relaxation techniques aiming to strengthen the participant’s resources to prevent stress and/or deal with negative consequences of stress more efficiently [9]. For example, it has been shown that progressive muscle relaxation, mindfulness training and stress management trainings based on cognitive behavior therapy can lead to a decrease in subjective perception of stress as well as to a reduction of objective stress markers such as cortisol release under acute stress [10-12]. However, it has been shown that participants often discontinue such trainings [13]. In order to counteract premature dropout in the beginning, the deployment of stress interventions via smartphone apps provides a promising alternative approach.
Smartphones are very popular with users and can be used independently of time and location [14]. They are comparatively inexpensive with reference to their broad functionality and appear to be socially accepted [15]. Interventions through smartphone application are low-priced and might therefore decrease expenses for anti-stress programs in the health insurance sector [16]. Hence, the use of smartphones could usher in a new era in clinical practice, but also contribute to the fields of pro- and reactive health promotion [17].
Recent reviews state that the effectiveness of stress interventions via smartphone apps has only scarcely been investigated in the clinical context as well as in the context of pro- and reactive health promotion [18,19]. However, these few studies tend to show positive results. The usage of anti-stress-apps by Swedish managers led to an increase in subjectively assessed general health symptoms in comparison to a control group [3]. Similar results are shown in a Finish study. The usage of an anti-stress-app for one month decreased stress perception significantly [20]. In contrast, an Italian investigation resulted in no change in subjective stress perception following an intervention via an anti-stress-app of 18 days [21]. Although this study implemented one, it has to be taken into account that several investigations lack control groups [20,22]. While first results seem to indicate positive effects of anti-stress-apps on subjectively perceived stress, it remains unclear whether it leads to the same extent of improvement as well-established face-to-face interventions do. Beyond this, it has yet not been investigated if the positive effects of anti-stress-apps are also reflected in objective measures of stress reactions, such as cortisol [23]. It is not sufficient to measure stress solely on a subjective level since stress reactions are of psychological and physiological nature. Stress can only be apprehended on a multidimensional level by measurements of parameters of both levels [5]. Additionally, effects of social desirability might occur when deploying only questionnaires [24].
Therefore, the aim of this study is to close this gap in the current literature and examine if an anti-stress-app and well-established face-to-face interventions show similar effects on the acute psychophysiological stress response as well as on the psychophysiological development of chronic stress. We hypothesize that by implementing an anti-stress-app as well as by applying a face-to-face stress intervention, resources of a person in relation to their coping skills can be increased in comparison to a control group [3,9]. Consequently, we assume that both types of intervention result in a reduction of subjectively perceived stress and cortisol levels in an acute stress situation as well as a decrease in chronic stress perception and in cortisol awakening response (CAR). However, no hypothesis regarding which type of intervention is more effectively can be formulated due to the lack of empirical evidence.
Sample
The study was approved by the ethical committee of the German Sport University Cologne and conducted in accordance with the Declaration of Helsinki.
A priori power analysis was conducted using G*Power analysis [25]. The a priori power was set to .80, alpha level was set to .05, and the correlation among repeated measurements was set to .50. Based on the effect size of Ly and colleagues, f = 0.25, a minimum of 42 participants was required [3]. However, as dropout rates in previous app intervention studies ranged from 8% up to 28% and have been shown in reviews to reach up to 80%, our goal was to recruit between 60 and 65 participants [3,22,26].
Recruiting began in March 2015 by newspaper advertisement, bulletin at universities and in cooperation with the city of Cologne, Germany. Interested people filled out an online screening questionnaire. The questionnaire included questions about drug use and the intake of medication, as well as physical and psychological illness. Sixty-two healthy persons participated in the following pretest, however the dropout rate after the pretest was at 53.22%.
The remaining 29 subjects were between 23 and 60 years old, did not suffer from an illness of the cardiovascular or endocrine system, were non-smokers, used no drugs or took medication and did not suffer from a psychological illness.
The subjects were matched in three groups (anti-stress-app: n = 10, face-to-face: n = 11, control group: n = 9) based on age, gender, physical activity, acute subjective stress levels as well as subjectively perceived chronic stress levels [27].
Subjectively perceived stress
Subjectively perceived acute stress
Visual analogue scales. The subjectively perceived acute stress level was assessed using visual analogue scales (VAS) [28]. Subjects were asked to reply to the statement “In this moment I feel stressed” on a 10 cm line with the extreme poles not at all and very much.
Primary Appraisal and Secondary Appraisal. The appraisal of the acute stress situation was assessed with the Primary Appraisal and Secondary Appraisal Scale (PASA) [29]. Subjects answered 16 questions on a 6-point Likert-scale from 1 completely wrong to 6 absolutely right. A stress index was calculated based on the subscales “threat”, “challenge”, “locus of control”, and “self-concept” [29]. The higher the stress index, the more subjectively stressed the subjects felt.
Subjectively perceived chronic stress
The subjectively perceived chronic stress level was assessed using the screening-scale of the German Trier Inventory of Chronic Stress (TICS) [30]. Subjects were asked to answer 12 questions about their stress level on a scale from 0 never to 4 very often. The higher the formed sum score, the more stressed the subjects felt in the last four weeks.
Objective stress
Acute objective stress.
The measurement of salivary cortisol served as the parameter for the objective stress level and was assessed during the pre and post assessment [31]. Subjects were asked to transfer sputum in a SaliCap-straw (ultra-pure polypropylene tube) via a commercially available straw (polypropylene). The samples were frozen at -80 degree Celsius after completion of the pre- and posttest respectively. Salivary cortisol levels (in nmol/l) were determined by using commercial enzyme-linked immunosorbent assay (ELISA) kits (Salivary Cortisol ELISA, SLV 2930, DRG Instruments, Marburg, Germany) with a sensitivity of 1.40 nmol/l, an intra-assay Variation of 1.80% (M = 35.30 nmol/l) and an inter-assay variation of 7.47% (M = 67.04 nmol/l).
Objective chronic stress
Due to logistic and economic reasons, the collection of cortisol awakening response (CAR) data as a measure for chronic stress levels was carried out by the participants themselves. They were asked to follow a standardized protocol and were instructed to collect saliva cortisol (five samples) on one day of the week for every 15 min within one hr after awakening in the morning [32].
Induction of stress
In order to induce stress the Trier Social Stress Test for Groups (TSST-G) was used in an adapted form with three subjects [33]. In a first step, participants were given 10 min to prepare themselves for a fake job interview. They were than ask to speak for 3 min in front of a two head jury that showed no emotional reactions. In the second part of the TSST-G, participants were asked to count backwards as fast as possible from 2013 in steps of 17. Making a mistake, participants were asked to start from the beginning. The TSST is one of the most reliable methods to increase stress [34].
Intervention
The content of both multimodal interventions consisted of three parts: (1) Psychoeducation as a theoretical basis, (2) a large part of exercise and (3) regular practical homework [9]. The intervention lasted six weeks. (Table 1)
Table 1. Detailed intervention content and relaxation techniques provided to participants
Time |
Intervention content |
Relaxation technique |
Intervention week 1 |
Introduction to stress; reflection on individual stress reaction pattern |
Progressive muscle relaxation |
Intervention week 2 |
Cognitive-behavioral based stress reactions |
Autogenic training |
Intervention week 3 |
Mindfulness training; dealing with emotions |
Mindfulness meditation |
Intervention week 4 |
Communication strategies and non-violent communication |
Mindfulness yoga |
Intervention week 5 |
Self-concept reflection, and social comparison theory |
Breathing exercises |
Intervention week 6 |
Reflection on past techniques and open questions |
– |
An app was developed for the app-intervention group using MIT App Inventor 2. The app consisted of six modules. Every module was password-protected and the passwords were mailed consecutively every week. Therefore, subjects had to unlock the weekly modules in order to prevent them from access to all videos at once.
The face-to-face stress intervention was offered twice a week in order to ensure high flexibility for our participants.
Evaluation of the intervention
The stress interventions were evaluated with two subscales of the quality assurance questionnaire (QS17) by Kleinert et al. [35]. Participants had to answer questions about the perceived support and the learned abilities/skills on a scale from 1 does not apply to 4 applies fully. Their overall satisfaction and recommendation rate was also assessed using percentages. Finally, participants could answer open questions on positive aspects and on possible improvements regarding the intervention.
Procedure
The pretest took place in April and May. After the intervention from May to June, posttest was conducted in June 2015.
Pre- and posttests were conducted after 1.00 p.m. in order to account for the diurnal cortisol fluctuations [31]. Additionally, it was ensured that pre- and posttesting were held at the same time of the day for each participant. They were asked to abstain from food and beverages except water as well as from exercise 2 hr prior to testing.
At the beginning of each testing, subjects were welcomed in the laboratory by the experimenter. Using a previously recorded audio file, subjects were informed about the procedure and asked to fill out an informed consent form. Afterwards the first saliva sample was collected (C1 at t -30). Next, subjects were instructed to fill out questionnaires assessing personal data and information about their last night’s sleeping behavior. Fifteen minutes later the second saliva sample was collected (C2 at t -15). After additional five minutes, subjects listened to standardized instructions of the TSST-G. Prior to the fake job interview, subjects were asked to fill out the PASA and to give their third saliva sample (C3 at t 0). The experimenter was leaving the laboratory afterwards and the TSST-G started. Subsequent to the TSST-G the experimenter reentered the room and requested subjects for their fourth saliva sample (C4 at t +15). Final saliva samples were collected at five minutes and fifteen minutes intervals, respectively (C5 at t +20; C6 at t +35; C7 at t +50). Furthermore, subjects were asked to fill out more questionnaires (e.g., TICS). During the preassessment, subjects were informed about the following procedure of the intervention. During the postassessment, subjects were debriefed after their last saliva sample. Additional to each saliva sample, subjectively perceived acute stress was assessed using visual analogue scales (VAS 1-7).
Data and statistical analyses
For acute subjective and objective stress data, the mean of the first two measurement times (VAS1 & VAS2; C1 & C2) was calculated, representing the baseline (BL). In order to describe changes of the subjectively perceived acute stress, the mean of VAS3 and VAS4 was calculated, expecting the highest levels of subjectively perceived acute stress at these measurement points (VAS peak). To display the changes in cortisol levels in proportion to the BL, the area under the curve with respect to increase (AUCI) was calculated in accordance to Fekedulegn and colleagues [36]. The bigger the amount of the AUCI, the higher is the increase of the cortisol level caused by the TSST-G. For objective chronic stress data, the AUCI of the cortisol awakening response (CAR) was calculated [36].
One-way repeated-measures analysis of variances (ANOVA) were performed in order to determine whether the TSST-G successfully resulted in an increase in subjectively perceived and objective stress level in the pre- and posttest.
Whether the intervention groups showed reductions in acute and chronic stress levels, both on a subjective as well as objective level, four repeated-measures ANOVAs (pre- vs. posttest) and group (anti-stress-app vs. face-to-face vs. control group) as between-subjects variables were conducted. The significance level was set at p < .05.
To investigate whether there are differences in the perceived support and the skill development between the anti-stress-app and face-to-face intervention group, two independent t-tests were performed. Further independent t-tests were conducted to compare satisfaction and recommendation between the intervention groups. The significance level was adjusted to p < .013 to avoid the problem of multiple comparisons.
All dependent variables were screened for statistical outliers (±3 SD) and tested for normal distribution. Two outliers, for the variables “CAR Post “(increase of morning cortisol in postintervention), and “AUCI Post” (increase of cortisol through TSST-G during the posttest period) were found. In the following, all results are presented including the outliers in order to provide a complete picture of the gathered data. However, all calculations were performed also without outliers and presented the same pattern of results. Descriptive data for all groups are shown in Table 2.
Table 2. Age, BMI and physical activity
Group |
|
|
Age |
BMI |
Physical activity in hr per week |
|
n |
♀ |
M |
SD |
Range |
M |
SD |
Range |
M |
SD |
Range |
App |
10 |
8 |
33.90 |
9.63 |
24–55 |
25.22 |
2.51 |
21.60–29.22 |
3.80 |
2.35 |
0–7 |
F2F |
11 |
8 |
41.00 |
13.45 |
23–60 |
22.91 |
3.13 |
19.59–28.28 |
3.18 |
3.49 |
0–12 |
CG |
8 |
4 |
37.75 |
13.84 |
23–58 |
26.30 |
4.53 |
20.66–34.29 |
2.63 |
2.26 |
0–7 |
Total |
29 |
20 |
37.66 |
12.32 |
23–60 |
24.64 |
3.57 |
19.49–34.29 |
3.24 |
2.76 |
0–12 |
Dropout |
33 |
22 |
39.27 |
12.57 |
20–60 |
23.50 |
3.67 |
19.84–40.00 |
3.30 |
3.19 |
0–12 |
Notes: App = anti-stress-app intervention group; F2F = face-to-face intervention group; CG = control group; Dropout = group of participants that participated only in the pretest; n = number of participants; BMI = Body Mass Index
TSST-G.
TSST-G increased both, the subjective stress level, F(6, 125) = 21.365; p < .001; ηp2 = .442 and the objective stress level, F(6, 168) = 13.103; p < .001; ηp2 = .319 with a power of > .99, during the pre- and posttest period [VASPost: F(6, 156) = 14.939; p < .001; ηp2 = .365; AUCIPost: F(6, 168) = 16.152; p < .001; ηp2 = .366]. Please see Figure 1a and 1b as well as Table 3.
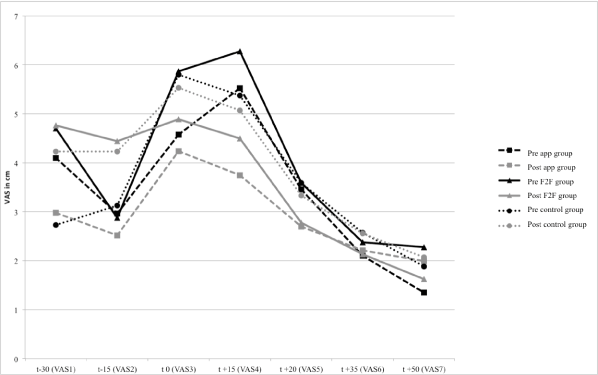
Figure 1a.Cortisol changes during pre- and posttests

Figure 1b.Self-perceived stress level during pre- and posttest
Table 3. Subjective and objective levels of acute and chronic stress pre and post intervention.
Group |
|
|
Acute stress |
Chronic stress |
|
|
|
Questionnaires (subjective) |
Cortisol (objective) |
Questionnaire
(subjective) |
Cortisol (objective) |
|
n |
|
PASA
M (SD) |
VAS BL
M (SD) |
VAS Peak
M (SD) |
BL in nmol/l
M (SD) |
AUCI in nmol/l
M (SD) |
TICS
M (SD) |
CAR in nmol/l
M (SD) |
App |
10 |
Pre |
-0.79 (1.37) |
3.53 (1.94) |
5.05 (1.04) |
9.47 (2.13) |
162.56 (125.31) |
19.30 (9.80) |
18.55 (384.65) |
Post |
-0.75 (0.57) |
2.75 (1.49) |
4.00 (1.58) |
9.08 (3.06) |
430.84 (596.71) |
27.13 (8.49) |
-67.24 (86.36) |
F2F |
11 |
Pre |
-0.86 (1.30) |
3.87 (1.67) |
5.66 (2.03) |
10.91 (4.75) |
94.17 (167.63) |
23.82 (5.47) |
157.97 (311.42) |
Post |
-0.53 (0.59) |
4.40 (2.16) |
4.59 (1.02) |
9.90 (2.61) |
304.24 (228.00) |
32.70 (5.62) |
-161.33 (564.32) |
CG |
8 |
Pre |
-1.08 (0.81) |
2.94 (1.47) |
5.74 (2.38) |
9.53 (3.30) |
357.66 (442.37) |
18.75 (7.74) |
-154.12 (331.12) |
Post |
-0.74 (0.75) |
3.89 (2.47) |
5.30 (2.02) |
9.95 (3.84) |
366.36 (389.42) |
28.00 (7.55) |
-4.16 (434.97) |
Dropout |
33 |
Pre |
-1.00 (1.40) |
3.58 (2.21) |
5.24 (2.10) |
8.43 (3.32) |
101.71 (171.62) |
26.27 (8.55) |
- |
Notes: App = anti-stress-app intervention; F2F = face-to-face intervention; CG = control group; Dropout = group of participants who only participated in the pretest; n = number of participants in different groups; PASA = Primary Appraisal and Secondary Appraisal questionnaires; VAS = visual analogue scale; BL = baseline (mean value of VAS1 and VAS2; C1 and C2); VAS Peak = mean value of VAS3 and VAS4); AUCI = area under the curve with respect to increase; TICS = Trier Inventory for Chronic Stress (screening scale); CAR = cortisol awakening response.
Intervention: Changes in subjective perception of stress
No significant main effect (p = .192; ηp2 = .065, power of .99) or interaction effect (p = .717; ηp2 = .025, power of .29) was found for the stress index (i.e., PASA) during the TSST-G. Similarly, analysis of the subjective perception of chronic stress (TICS) did not show an interaction effect (p = .848; ηp2 = .025, power of .29). Nevertheless, a main effect for time was detected, F (1, 22) = 42.379; p < .001; ηp2 = .658 with a power of > .99, indicating that the perception of chronic stress was higher during the posttest phase when compared to the pretest phase in all groups.
Intervention: Changes in objective stress levels.
Regarding the acute objective stress reaction, the ANOVA revealed a significant main effect for time, F(1, 26) = 4.653; p = .040; ηp2 = .152 with a power of .98. Contrary to our expectation, cortisol levels increased significantly in the posttest phase in comparison to the pretest phase. The expected interaction effect for the groups was not found, p = .383; ηp2 = .383 with a power of > .99. For the chronic objective stress reaction, no significant main effect (p = .279; ηp2 = .056 with a power of .62) or interaction effect was detected (p = .183; ηp2 = .15 with a power of .98).
Evaluation of intervention
There were no significant differences between both intervention groups (Table 4).
Table 4. Comparison of intervention quality between anti-stress-app and face-to-face group.
|
Anti-stress-app group |
Face-to-face group |
|
|
|
|
M |
SD |
Range |
M |
SD |
Range |
p |
d |
power |
Perceived support |
2.59 |
0.92 |
1.14–3.86 |
3.21 |
0.54 |
2.57–4.00 |
.078 |
0.88 |
.16 |
Learned abilities/skills |
2.52 |
1.02 |
0–3.50 |
2.78 |
0.06 |
2.00–3.50 |
.486 |
0.39 |
.07 |
Satisfaction |
61.11 |
25.22 |
20–80 |
74.00 |
15.10 |
50-100 |
.189 |
0.66 |
.11 |
Recommendation rate |
72.50 |
32.94 |
0–100 |
70.00 |
31.62 |
20–100 |
.864 |
0.08 |
.05 |
The goal of the 6-week intervention study was to compare an anti-stress-app to a face-to-face stress intervention and a control group in regard to their changes in psychophysiological acute and chronic stress reaction. The results show that none of our hypotheses were confirmed.
Subjective stress
In contrast to our expectations all groups had an increase in subjective chronic stress (i.e., TICS). As most of our participants were either university students or employees of the city Cologne, Germany, it is reasonable to assume that their workload and perceived stress levels increase at the end of the semester [37]. In the same line of argument, it is known that perceived stress is especially increased before upcoming vacations [38]. However, it remains to note that this same pattern is conceivable for the control group and that none of the stress interventions led to an increase in perceived chronic stress.
Objective stress
In regard to the physiological parameter cortisol, it is difficult to compare our results to previous research as it either focused on a one-time use of relaxation techniques (e.g., progressive muscle relaxation) or used a short-term intervention (e.g., 10 hr intervention) in which the TSST was used only once [10,12]. Further, none of these studies aimed to investigate effects of a smartphone application. Due to those reasons the discussion will primarily focus on contentual explanations as well as methodological aspects with regard to participants and high dropout rates in order to understand the current null results.
Satisfaction and intervention quality
Our results show no significant differences between the anti-stress-app and the face-to-face intervention group in regard to satisfaction, recommendation rate, the perceived support, and learned abilities/skills. These results carefully suggest that a face-to-face stress intervention not necessarily leads to higher satisfaction or provides better quality in comparison to an anti-stress-app intervention. Comparing the current results on satisfaction and intervention quality to previous research is however problematic, as most of those studies did not assess such parameters [3,21]. Yet, 83% of the participants of the study by Proudfoot and colleagues would recommend the app they used whereas only 73% of our participants would recommend the used anti-stress-app. The satisfaction within our sample was also lower in comparison to Proudfoot and colleagues’ participants [22]. It should be noted that this comparison needs to be interpreted cautiously as the sample sizes differ considerably.
Also, the intervention quality rating distribution in our app group was positively skewed, meaning a less favorable quality rating. This was mainly due to one participant in the app group. He wrote that the app is an “unsuitable medium” and that he would have preferred “closer support”. In contrast to his opinion were several participants that acknowledged the previously mentioned advantages of an anti-stress-app. They stated that they particularly liked the “modern use of the app and e-mail reminders”, the “flexibility” and the possibility that “all information can be accessed anytime” which supports results from previous research [20].
In comparison to previous research it needs to be noted that especially the features of the apps vary considerably. In the current study, participants were able to view psychoeducational videos and receive instructions for relaxation techniques as well as homework. In previous studies that found positive results of anti-stress-apps several additional features were installed such as written information, a therapist who would answer questions by participants and provide them with positive encouragement or there were more modules including an individual feedback function [3,20,22]. In comparison to the study by Carissoli and colleagues who found no changes in subjectively perceived stress in their participants, no further features were integrated in the app [21]. Consequently, an adaptation of features and a closer investigation to which features are particularly helpful for users could be beneficial in the future.
Sample size and dropout rate
The sample size in the current study is substantially smaller in comparison to previous research and in addition, smaller than the estimated sample size by the G*Power analysis. Due to the high dropout rate in our study (53%)–also in comparison to previous research on that topic–the necessary sample size was not reached and could be one of the explanations of the not significant results.
One reason of the high dropout rate might have been a deterrent effect of the TSST-G. Posteriori analyses however, could not confirm this assumption. Participants that discontinued after the pretest had neither significant differences in their cortisol increase (AUCI: p = .128) nor in their subjective stress appraisal of the situation (PASA stress index: p = .748). Yet, the perceived chronic stress in the dropout group was significantly higher: TICS: t(60) = 2.578, p = .012, d = 0.68. Also, the TICS screening values, which are a global indicator for chronic stress, were in an inflated range [30]. This indicates more concerns, overload, excessive demands, and diminished recognition and could be an indication that a participation in a 6-week program might rather be considered an extra burden that leads to a potentiation of excessive demands. As the participants did not provide any reasoning for their dropout this is only reasonable speculation. Even though, we would argue that the dropout is not due to the intervention itself, as participants dropped out before the beginning of the intervention, we need to recognize that especially those participants would potentially benefit from app interventions the most, however were less likely to participate.
Limitation and future research
The intervention study has, apart from the already discussed limitations, several limits that need to be mentioned in order to avert misinterpretations. Especially the cortisol awakening data needs to be considered carefully. Next to the high standard deviation, participants were asked to self-reliantly collect and store their saliva samples. Even though, we received five samples from each participant for pre- and posttesting and participants ensured the predetermined sampling and storage instructions, we were reliant on participants’ compliance. Overall, the cortisol awakening data points to an unregularly course of the curve [39]. Finally, it would have been useful to assess follow-up data, as possible effects of intervention can only be observed after a longer time period [22].
Overall, our study has several limitations that were extensively discussed. However, to our knowledge it is the first study that compared an anti-stress-app to a face-to-face and a control group with respect to acute and chronic psychophysiological changes, and found that most participants in the anti-stress-app group perceived this type of intervention as positive and especially appreciated its flexibility and accessibility. Still, there were participants for those the face-to-face intervention group would have been more beneficial. It appears that an agreement on the needs and wants of participants is and continuous to be of utmost relevance for successful stress interventions [40]. Whether an app can, also from an ethical perspective, better accommodate those needs and wants in a long-term remains to be seen [41]. However, as health care and anti-stress-apps represent a considerably large amount of app downloads without any validation to their usefulness or effectiveness, future research focusing on smartphone interventions is necessary and warranted [18].
We would like to thank all the participants and especially the city of Cologne for their support in recruitment. Finally, we thank the Institute of Psychology, Performance Psychology group in Cologne as well as the Institute for Sport Psychology and Sport Pedagogy in Leipzig for their critical feedback.
The current study was founded by the German Sport University Cologne. The authors are responsible for the content of this publication.
- American Psychological Association (2017) Stress in America: Coping with Change. Stress in AmericaTM Survey.
- Boorman S (2009) NHS Health and Wellbeing Review: Interim Report. Department of Health, Leeds.
- Ly KH, Asplund K, Andersson G (2014) Stress management for middle managers via an acceptance and commitment-based smartphone application: A randomized controlled trial. Internet Interv 1: 95-101.
- Kropiunigg U (1993) Basics in psychoneuroimmunology. Ann Med 25: 473-479. [Crossref]
- Lazarus RS (2000) How emotions influence performance in competitive sports. Sport Psychol 14: 229-252.
- Hill DM, Hanton S, Matthews N, Fleming S (2010) Choking in sport: A review. Int Rev Sport Exer P 3: 24-39.
- Brotman DJ, Golden SH, Wittstein IS (2007) The cardiovascular toll of stress. Lancet 370: 1089-1100. [Crossref]
- Hardy GE, Woods D, Wall TD (2003) The impact of psychological distress on absence from work. J Appl Psychol 88: 306-314. [Crossref]
- Richardson KM, Rothstein HR (2008) Effects of occupational stress management intervention programs: A meta-analysis. J Occup Health Psychol 13: 69-93. [Crossref]
- Pawlow LA, Jones GE (2002) The impact of abbreviated progressive muscle relaxation on salivary cortisol. Biol Psychol 60: 1-16. [Crossref]
- Warnecke E, Quinn S, Ogden K, Towle N, Nelson MR (2011) A randomised controlled trial of the effects of mindfulness practice on medical student stress levels. Med Educ 45: 381-388. [Crossref]
- Gaab J, Blättler N, Menzi T, Pabst B, Stoyer S, et al. (2003) Randomized controlled evaluation of the effects of cognitive–behavioral stress management on cortisol responses to acute stress in healthy subjects. Psychoneuroendocrino 28: 767-779. [Crossref]
- Groeneveld IF, Proper KI, van der Beek AJ, Hildebrandt VH, van Mechelen W (2009) Factors associated with non-participation and dropout in a lifestyle intervention for workers with an elevated risk of cardiovascular disease. Int J Behav Nutr Phy 6: 80.
- Griffiths KM, Christensen H (2007) Internet based mental health programs: A powerful tool in the rural medical kit. Aust J Rural Health 15: 81-87. [Crossref]
- Boschen MJ, Casey LM (2008) The use of mobile telephones as adjuncts to cognitive behavioral psychotherapy. Prof Psychol-Res Pr 39: 546-552.
- Proudfoot J (2013) The future is in our hands: The role of mobile phones in the prevention and management of mental disorders. Aust N Z J Psychiatry 47: 111-113. [Crossref]
- Donker T, Petrie K, Proudfoot J, Clarke J, Birch MR, et al. (2013) Smartphones for smarter delivery of mental health programs: A systematic review. J Med Internet Res 15: e247. [Crossref]
- Lui JH, Marcus DK, Barry CT (2017) Evidence-based apps? A review of mental health mobile applications in a psychotherapy context. Prof Psychol-Res Pr 48: 199-210.
- Payne HE, Lister C, West JH, Bernhardt JM (2015). Behavioral functionality of mobile apps in health interventions: A systematic review of the literature. JMIR mHealth and uHealth, 3: e20.
- Ahtinen A, Mattila E, Välkkynen P, Kaipainen K, Vanhala T, et al. (2013) Mobile mental wellness training for stress management: Feasibility and design implications based on a one-month field study. JMIR Mhealth Uhealth 1: e11. [Crossref]
- Carissoli C, Villani D, Riva G (2015) Does a meditation protocol supported by a mobile application help people reduce stress? Suggestions from a controlled pragmatic trial. Cyberpsychol Behav Soc Netw 18: 46-53. [Crossref]
- Proudfoot J, Clarke J, Birch M-R, Whitton AE, Parker G, et al. (2013) Impact of a mobile phone and web program on symptom and functional outcomes for people with mild-to-moderate depression, anxiety and stress: A randomized controlled trail. BMC Psychiatry 13: 312. [Crossref]
- Lappalainen R, Sairanen E, Järvelä E, Rantala S, Korpela R, et al. (2014) The effectiveness and applicability of different lifestyle interventions for enhancing wellbeing: The study design for a randomized controlled trial for persons with metabolic syndrome risk factors and psychological distress. BMC Public Health 14: 310. [Crossref]
- Krumpal I (2013) Determinants of social desirability bias in sensitive surveys: A literature review. Qual Quant 47: 2025-2047.
- Faul F, Erdfelder E, Lang A-G, Buchner A (2007) G* Power 3: A flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods 39: 175-191. [Crossref]
- Christensen H, Griffiths KM, Farrer L (2009) Adherence in internet interventions for anxiety and depression: Systematic review. J Med Internet Res 11: e13. [Crossref]
- Rimmele U, Zellweger BC, Marti B, Seiler R, Mohiyeddini C, et al. (2007) Trained men show lower cortisol, heart rate and psychological responses to psychosocial stress compared with untrained men. Psychoneuroendocrino 32: 627-635. [Crossref]
- Hayes MHS, Paterson DG (1921) Experimental development of the graphic rating method. Psychol Bull 18: 98-99.
- Gaab J (2009) PASA–Primary appraisal secondary appraisal. Verhaltenstherapie 19: 114-115.
- Schulz P, Schlotz W, Becker P (2004) TICS. Trierer Inventar zum chronischen Stress – Manual. Göttingen: Hogrefe.
- Kirschbaum C, Hellhammer DH (2000) Salivary free cortisol. In: G. Fink (Hrsg.), Encyclopedia of Stress (3rd Ed., p. 379-383). Oxford: Academic Press.
- Chida Y, Steptoe A (2010) Greater cardiovascular responses to laboratory mental stress are associated with poor subsequent cardiovascular risk status: A meta-analysis of prospective evidence. Hypertension 55: 1026-1032. [Crossref]
- Von Dawans B, Kirschbaum C, Heinrichs M (2011) The Trier Social Stress Test for Groups (TSST-G): A new research tool for controlled simultaneous social stress exposure in a group format. Psychoneuroendocrino 36: 514–522.
- Dickerson SS, Kemeny ME (2004) Acute stressors and cortisol responses: a theoretical integration and synthesis of laboratory research. Psychol Bull 130: 355-391.
- Kleinert J, Ohlert J (2014) Ergebnisqualität in der sportpsychologischen Beratung und Betreuung. Konstruktion und erste Ergebnisse des Befragungsinventars QS17. Z Sportpsycho 21: 13-22.
- Fekedulegn DB, Andrew ME, Burchfiel CM, Violanti JM, Hartley TA, et al. (2007) Area under the curve and other summary indicators of repeated waking cortisol measurements. Psychosom Med 69: 651-659.
- Weekes NY, Lewis RS, Goto SG, Garrison-Jakel J, Patel F, et al. (2008) The effect of an environmental stressor on gender differences on the awakening cortisol response. Psychoneuroendocrino 33: 766-772. [Crossref]
- Fritz C, Sonnentag S (2006) Recovery, well-being, and performance-related outcomes: The role of workload and vacation experiences. J Appl Psychol 91: 936-945. [Crossref]
- Wust S, Wolf J, Hellhammer DH, Federenko I, Schommer N, et al. (2000) The cortisol awakening response-normal values and confounds. Noise Health 2: 79-88. [Crossref]
- Lamontagne AD, Keegel T, Louie AM, Ostry A, Landsbergis PA (2007) A systematic review of the job-stress intervention evaluation literature, 1990–2005. Int J Occup Environ Health 13: 268-280. [Crossref]
- Jones N, Moffitt M (2016) Ethical guidelines for mobile app development within health and mental health fields. Prof Psychol-Res Pr 47: 155.

