Abstract
Both Nocardia and non-tubercular mycobacteria are opportunistic human pathogens. Co-infection is rare and not found in the literature. We detected a young female suffering from such a co-infection in both lungs, joints and bones. She subsequently improved on simultaneous treatment for both of these organisms.
Key words
nocardia, non-tubercular mycobacteria, co-infection, pulmonary disease, osteomyelitis
Introduction
Nocardia is a soil borne saprophytic, aerobic actinomycete causing either localised infection of lung or wide spread disseminated infection particularly to the brain, soft tissue and skeletal structures. Nocardia asteroides is the main human pathogen (85%); N.brasiliensis, N.otitidiscaviarum are the other main pathogenic nocardiae. Nocardiosis chiefly affects immunocompromised hosts such as patients with lymphoreticular malignancies; solid tumours, transplant recipients, HIV infection, alcoholism, diabetes mellitus, trauma, prior granulomatous diseases like tuberculosis, connective tissue diseases like sarcoidosis, systemic lupus erythematosus [1].
Non-tubercular mycobacteria (NTM) are widely distributed in the environment with high isolation rates worldwide [2]. Organisms can be found in soil and water, including both natural and treated water sources (M.kansasii, M. xenopi, and M. simiae are recovered almost exclusively from municipal water sources and rarely, if ever, fromother environmental sources). Human disease is suspected to be acquired from environmental exposures, although the specific source of infection usually cannot be identified. NTM may cause both asymptomatic infection and symptomatic disease in humans including lung, soft-tissues etc. Joints, bones, tendons are usually affected by local inoculation of the pathogen by direct trauma or surgery [3]. Occasionally, axial bones or extremities may be affected by NTM without apparent trauma.
Case report
A 27 years old non-diabetic female presented with low-grade evening rise of temperature, productive cough, anorexia and significant weight-loss for last one and a half years. It was soon followed by swelling of both her ankles, right elbow and both wrist joints along with dorsum of feet and hands. All the sites were tender and there was blood mixed sero-sanguinous discharge from the swelling of hands and feet. Her complaints underwent a waxing and waning course with chronic ill-health during this time-period.
She developed left sided tubercular pleural effusion three years back and received two months of ATD (rifampicin, isoniazid, pyrazinamide, ethambutol). But with partial recovery she stopped her treatment prematurely. Pleural effusion recurred after one year for which she again received ATD for eight months with complete cure this time.
On-examination, she was pale, cachectic, with swelling of dorsum of both hands (Figure 1a), right wrist (Figure 1b), right elbow (Figure 1c), dorsum of right foot (Figure 2), right ankle. Joint temperature was normal with restricted movement and sero-sanguinous discharge was noted from all the involved joints. Spleen was palpable 3cm below left costal margin. Coarse crackles were present in the right infraclavicular region.
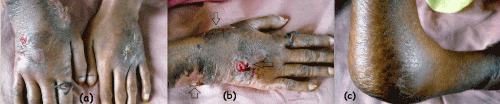
Figure 1. Lesions of (a) both hands, (b) right wrist and (c) right elbow at presentation.
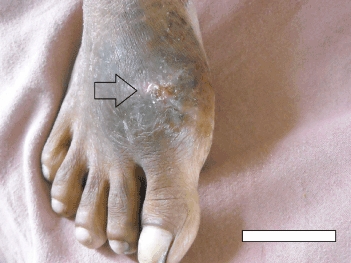
Figure 2. Lesion around the ball of great toe of right foot at presentation
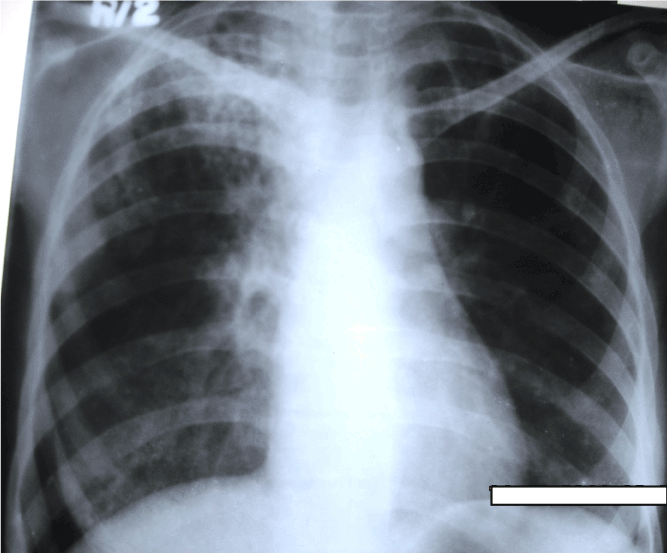
Chest x-ray (Figure 3) revealed in non-homogenous opacities involving both upper zones and right mid-zone. X-ray right hand (Figure 4a) and right foot (Figure 4b) revealed osteolytic lesions. Sputum and wound-discharge from multiple sites including both hands and feet for acid fast bacilli (AFB) were positive. Gram stained smear of sputum showed gram positive beaded, branched organisms suggestive of nocardia (Figure 5). Culture grew non-tubercular mycobacteria (NTMs- Mycobacterium abscessus) and Nocardia asteroides from the discharge of hands and feet. HIV serology was negative and she was not on any immunosuppressive medication.
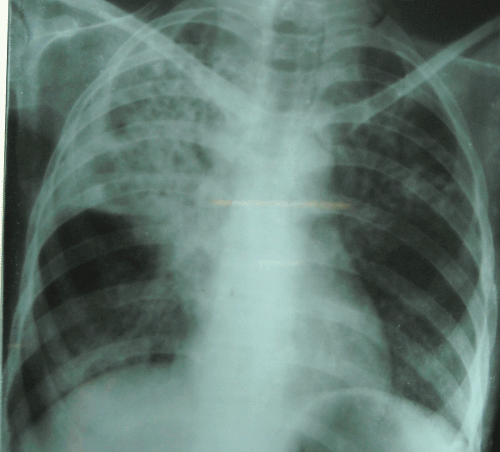
Figure 3. Chest X-ray at presentation, showing non-homogeneous opacity in right upper, middlezones and left upper zone.
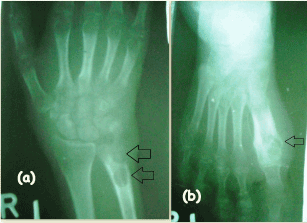
Figure 4. X-ray of (a) right hand and (b) right foot at presentation showing osteolytic lesions.
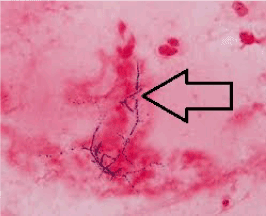
Figure 5. Gram stained smear of sputum showed gram positive beaded, branched organisms suggestive of nocardia.
In addition to surgical wound debridement treatment was started with oral co-trimoxazole, co-amoxiclav for Nocardia and clarithromycin, amikacin and imipenem for NTM as per Infectious Disease Society of America (IDSA) guidelines [4]. After one month, fever subsided with reduction of cough, expectoration and joint swelling. Lesions of the hands (Figure 6a), foot (Figure 6b) and chest x-ray (Figure 7) showed improvement. She was advised to continue the treatment for 12 months when co-trimoxazole and co-amoxiclav were stopped and sputum was found to be negative for both the organisms. Other medicines were continued for total duration of 24 months (to achieve a goal of 12 months of sputum negativity for M. abcessus). She is being followed up and is asymptomatic till date.
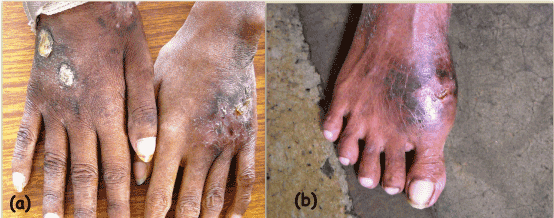
Figure 6. Lesions of (a) hands and (b) right foot after 1 month of treatment
 Nocardiosis. Clinical Infectious Diseases 22: 894-895</li>
<li>Falkinham JO (2002) Nontuberculous mycobacteria in the environment. <em>Clin Chest Med </em>23:520–551.</li>
<li>Hoffman PC, Fraser DW, Rohicsek F, O’Bar PR, Mauney CU (1981) Two outbreaks of sternal wound infections due to organisms of the <em>Mycobacterium fortuitum </em>complex. <em>J Infect Dis </em>143:533–542. <a href=)
[Crossref]
Griffith DE, Aksamit T, Brown-Elliott BA, Catanzaro A, Daley C, et al. (2007) An Official ATS/IDSA Statement: Diagnosis, Treatment, and Prevention of Nontuberculous Mycobacterial Diseases. Am J RespirCrit Care Med 175: 367–416. [Crossref]
Harrison’s Principles of Internal Medicine; Nocardiosis; Gregory A. Filice; (18thedn), 1323.
http://www.isradiology.org/tropical_deseases/tmcr/chapter6/clinical5.htm