Mucinous cystic neoplasms (MCN) of the mesentery are rare tumors which are difficult to diagnose accurately preoperatively and carry the risk of being borderline or malignant. This is a case of a 37 years old female who was referred to a tertiary gynecological oncology center for a suspected ovarian tumor and was found to have a borderline MCN, originating from the descending and sigmoid colon mesentery. To the best of our knowledge, this is the largest borderline MCN of mesenteric origin reported in the literature so far and only the second case managed by a gynecologist. We are also presenting a literature review of the similar cases reported up-to-date.
mesenteric cyst, mucinous neoplasm, gynaecological oncology, enucleation, ovarian, adnexal cyst
Mesenteric cysts are a rare diagnosis, accounting for 1/100 000 to 1/250 000 of adult hospital admissions, with equal distribution between sexes [1]. The first reported case dates back to 1507 by Florentine anatomist Benevieni and was described at an autopsy of an 8 year old boy [2]. About half of them are chylous cysts, but may be of mesothelial, enteric, dermoid, urogenital, traumatic, or infectious genesis [2].
The origin of extra-ovarian mucinous cystic neoplasms (MCN) has been attributed to implanted or ectopic ovarian tissue, supernumerary ovaries or monolineage development of a component of a teratoma [3]. The most widely accepted hypothesis for the aetiology of extra-ovarian MCN is the coelomic mucinous metaplasia of epithelial cells or invaginated peritoneum along the course of ovarian descent [3]. In this paper we are presenting our experience with a case report of an MCN which was misdiagnosed as a possible broad ligament cyst and we are discussing the management in view of the up-to-date literature evidence.
A 37 year old female, with previous three full term normal deliveries, presented with a history of abdominal distension and mild pain. She had three vaginal deliveries and no medical comorbidities. She had a history of laparoscopic left ovarian cystectomy in 2006. In 2010 she underwent a midline laparotomy for a suspected large ovarian cyst, which intraoperatively was found to be of extra-ovarian origin and was drained. The cytology at that time was unremarkable. Both surgeries were preformed overseas. On clinical examination, the abdomen was soft and a large mobile mass filling the whole abdominal cavity was palpated. Ultrasound scan (USS) showed a normal left ovary. Magnetic Resonance Imaging (MRI) scan revealed a 20.1 x 12.4 cm mass, arising from the left adnexa, containing solid components, which was separate from the left ovary. The report was inconclusive of the exact source of the mass and suspected a possible broad ligament origin (Figure 1). The CT (Chest and abdomen) scan showed no evidence of disease at any other site outside the left adnexal mass (Figure 2). The tumour markers were within normal limits.
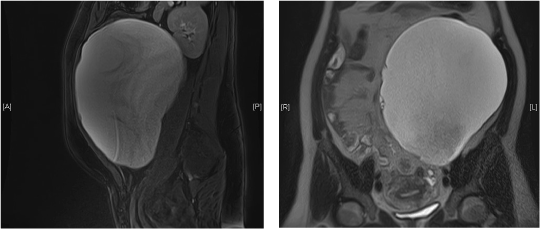
Figure 1.MRI images of the mesenteric cyst.
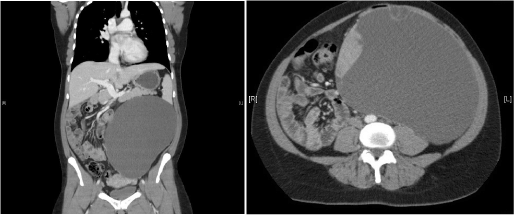
Figure 2.CT images of the mesenteric cyst.
Following a gynaecological oncology multidisciplinary team meeting, the patient gave consent for fertility preserving surgery including excision of the mass and submitting it for frozen section +/- omentectomy +/- peritonectomy +/- pelvic and para-aortic lymph nodes excision + excision of any other visible tumour.
At laparotomy we found a large retroperitoneal cyst measuring 25 x 20 x 17 cm in the descending and sigmoid colon mesentery (Figure 3). The mesentery of the large bowel was opened and the cyst was removed intact after being dissected from the left ureter and inferior mesenteric artery (Figure 4). There was no evidence of disease elsewhere. The cyst was sent fresh for frozen section histology. Examination in the histology laboratory revealed 3400 ml of cloudy mucoid fluid within the cyst and a solid mural nodule measuring 14 x 9 x 3 cm. Two samples from the solid nodule within the cyst were taken and the frozen section was reported as a mucinous borderline tumour. Based on the result of the frozen section we proceeded to bilateral ovarian biopsies, pelvic and para-aortic lymph node sampling, infracolic omentectomy, peritoneal biopsies and appendicectomy. Advice from colorectal team was sought and they agreed with the management. No bowel resection was required and the procedure was uneventful with minimal blood loss (100 ml). The final histopathology examination confirmed a mucinous borderline tumour in keeping with primary mesenteric origin (Figure 4). The ovarian biopsies, omentum, appendix and peritoneal biopsies showed no abnormal histology.
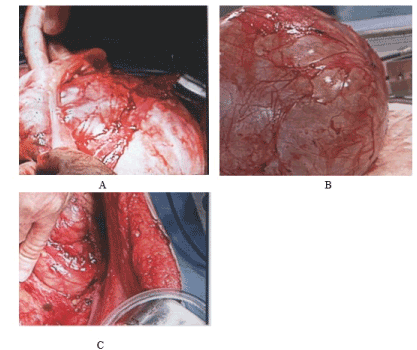
Figure 3.A: The descending colon mesentery was opened to enucleate the cyst. B: Cyst delivered intact to abdominal wall. C: The post enucleation bed (left colon mesentery and left renal compartment).
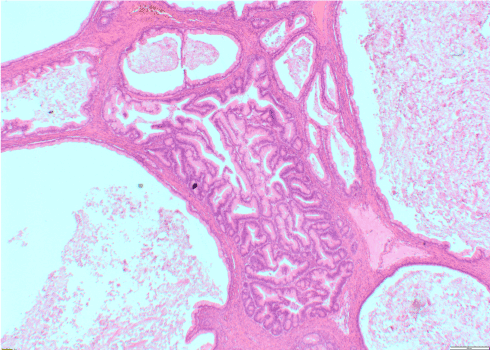
Figure 4.Histological image of the MCN, haematoxylin & eosin, x100 magnification).
The lymph nodes sampled were negative and peritoneal washings showed no abnormal cells. The patient recovered well for three days in hospital and was followed up two weeks after surgery with excellent recovery and no postoperative complication.
There are twenty documented cases of mesenteric mucinous cystic neoplasms (MCN) in the literature prior to this report, eleven of which were located in the mesocolon [4-18]. In five of them the final histology was reported as borderline MCN [4,6,10,13,19], in three as mucinous adenocarcinoma [12,18] and one case recurred as malignant after incomplete resection of a benign mesenteric cyst [8]. In most cases (including the currently presented one) the pre-operative imaging did not correlate with the exact tumour origin found intraoperatively (Table 1). The fact that mesenteric MCN was reported in two male patients raises doubt about the theory of ectopic ovarian tissue origin [5,16].
Table 1. Reported cases of MCN in the literature, including the current case.
Study |
N of cases |
Year of study |
Age (years) |
Sex |
Main symptoms |
Size of MCN (CM) |
Location of MCN |
Preoperative diagnosis |
Management |
Histology |
Banerjee & Gough (Banerjee and Gough, 1988) |
2 |
1988 |
58 |
F |
Incidental finding |
7 |
Hepatic flexure |
US/uncertain |
Right hemicolectomy, appendicectomy and excision of 3 cm of terminal ileum |
Benign |
|
|
|
38 |
F |
Abdominal pain and abdominal distension |
11 |
Descending colon |
US/uncertain |
Left colectomy and left salpingoopherectomy |
BOT |
Cohen et al. (Cohen et al., 1988) |
1 |
1988 |
36 |
F |
Diagnosed in pregnancy |
40 |
Ileum |
Uncertain |
Laparotomy/resection |
Benign |
Bury & Pricolo (Bury and Pricolo, 1994) |
1 |
1994 |
36 |
F |
Abdominal pain |
NS |
Small bowels |
CT/Uncertain |
Laparotomy/incomplete excision |
Transformed to malignant after recurrence |
McEvoy et al. (McEvoy et al., 1997) |
1 |
1997 |
24 |
F |
Vague abdominal pain |
20
x15 |
Sigmoid |
US/Ovarian origin |
Enucleation |
Benign |
Vrettos et al. (Vrettos et al., 2000) |
1 |
2000 |
38 |
F |
Abdominal pain/nausea and vomiting |
17
x12 |
Sigmoid |
US/CT mesenteric cyst |
Enucleation |
BOT |
Felemban & Tulandi (Felemban and Tulandi, 2000) |
1 |
2000 |
20 |
F |
Abdominal pain |
7.6
x7
x5.3 |
Appendix |
US ovarian origin |
Laparoscopic enucleation/
appendicectomy |
Benign |
Linden et al. (Linden and Ashley, 2000) |
1 |
2000 |
32 |
F |
Incidental finding |
15
x18 |
Transverse colon |
US/CT uncertain |
Laparotomy/enucleation |
Malignant |
Talwar et al. (Talwar et al., 2004) |
1 |
2004 |
32 |
F |
Abdominal pain and vomiting |
10
x7
x5 |
Descending colon |
US/ovarian origin |
Left hemicolectomy |
BOT |
Czubalski et al. (Czubalski et al., 2004) |
1 |
2004 |
38 |
F |
NS |
NS |
Small bowels |
Ovarian origin |
Laparotomy/
excision |
Benign |
Shioho et al (Shiono et al., 2006) |
1 |
2006 |
14 |
F |
NS |
15 |
NS |
NS |
NS |
Benign |
Luo et al. (Luo et al., 2008) |
1 |
2008 |
5 |
M |
Abdominal pain/swelling |
25 |
Small bowels |
NS |
Unresectable/
biopsy |
Benign |
Zwaveling et al. (Zwaveling et al., 2008) |
1 |
2008 |
18 |
F |
Abdominal swelling |
15 |
Right hemicolon |
CT/US intra-abdominal cyst |
Laparotomy
/enucleation of the cyst |
Benign |
Tan et al. (Tan et al., 2009) |
2 |
2009 |
NS |
NS |
NS |
NS |
NS |
NS |
NS |
Malignant |
Metaxas et al. (Metaxas et al., 2009) |
1 |
2009 |
22 |
F |
Pain |
8.5
x6
x3.5 |
Descending and sigmoid colon |
US/CT/MRI uncertain |
Enucleation |
Benign |
Cauchy et al. (Cauchy et al., 2012) |
2 |
2012 |
57 |
M |
Asymptomatic |
8
x7 |
Sigmoid |
US/CT gastrointestinal stromal tumour |
Laparotomy/enucleation |
Benign |
|
|
|
53 |
F |
Asymptomatic |
8
x9 |
Right mesocolon |
US/CT mesenteric mass |
Laparotomy/ ileocecal resection with en-bloc excision of the mass |
Benign,
high-grade dysplasia |
Mistry et al. (Mistry et al., 2012) |
1 |
2012 |
48 |
F |
Incidental |
10.5
x8.2
x6.5 |
Sigmoid |
US/CT ovarian origin |
Laparoscopic enucleation |
BOT |
Poudel et al. (Poudel et al., 2015) |
1 |
2015 |
33 |
F |
Abdominal pain |
10.5 x 6.5 x 2.0 |
Right colon |
CT uncertain |
Laparotomy/enucleation |
BOT |
Present case |
1 |
2016 |
37 |
F |
Abdominal discomfort and distension |
25
x 20 x 17 |
Descending and sigmoid colon |
US/CT/MRI broad ligament cyst |
Laparotomy/enucleation |
BOT |
N: number. CM: centimetre. NS: None specified. BOT: borderline tumour.
Only one of the tumours was operated on by a gynaecologist and was removed laparoscopically [11]. The choice between minimal access or open surgery depends on the certainty of preoperative diagnosis, size of the cyst and the skills of the surgeon. In our case, laparoscopic approach was not recommended because of the large size of the cyst to avoid the risk of rupture and peritoneal spillage of the cyst contents, especially as malignancy could not be ruled out preoperatively.
There is a group of tumours reported in the literature as primary retroperitoneal mucinous tumours. They are rare (about 20 case reports) and we differentiate them from our mesenteric MCN as they are not specifically allocated to the mesentery [20]. They are similar in origin and management. However, due to their non-mesenteric site, the risk of bowel resection would be less.
Our case adds to the literature series of the rare entity of mesenteric MCN. It represents the largest borderline MCN, where diagnosis could not be achieved preoperatively and surgery was performed by the gynaecological oncology team. It highlights as well the benefit of frozen section in some cases when management can be directed by intraoperative frozen section histology. We think that our case could be a recurrence of the previously drained extra-ovarian cyst.
Mucinous cystic neoplasms of the mesentery are a rare pathology, presenting mostly in women in reproductive age. The risk of borderline and malignancy of mesenteric MCN in the literature is 48% (11/20). They are difficult to diagnose accurately on imaging and should be treated with complete excision, rather than drainage because of the risk of missing the diagnosis of a borderline MCN, recurrence and malignant transformation.
- Santana WB, Poderoso WL, Alves JA, Melo VA, Barros Cd, et al. (2010) [Mesenteric cyst--clinical and pathological aspects]. Rev Col Bras Cir 37: 260-264. [Crossref]
- Tebala GD, Camperchioli I, Tognoni V, Noia M, Gaspari AL (2010) Laparoscopic treatment of a huge mesenteric chylous cyst. JSLS 14: 436-438. [Crossref]
- Metaxas G, Tangalos A, Pappa P, Papageorgiou I (2009) Mucinous cystic neoplasms of the mesentery: a case report and review of the literature. World J Surg Oncol 7: 47. [Crossref]
- Mistry K, Penna M, Dindyal S, Mukhtar H (2012) A mucinous cystic neoplasm of the mesocolon showing features of malignancy. Case Rep Surg 2012: 727105. [Crossref]
- Cauchy F, Lefevre JH, Mourra N, Parc Y, Tiret E, et al. (2012) Mucinous cystadenoma of the mesocolon, a rare entity frequently presenting with features of malignity: two case reports and review of the literature. Clin Res Hepatol Gastroenterol 36: e12-16. [Crossref]
- Poudel R, Acharya A, Pokhrel S, Adhikari SK (2015) Mucinous Cystic Borderline Tumor of the Mesentery: A Case Report. Kathmandu Univ Med J (KUMJ) 13: 170-171. [Crossref]
- Cohen I, Altaras M, Lew S, Jaffe R, Ben-Aderet N (1988) Huge mesenteric mucinous cystadenoma in normal pregnancy. Obstet Gynecol 71: 1030-1032. [Crossref]
- Bury TF, Pricolo VE (1994) Malignant transformation of benign mesenteric cyst. Am J Gastroenterol 89: 2085-2087. [Crossref]
- McEvoy AW, Cahill CJ, Jameson C (1997) Mucinous cystadenoma of the sigmoid mesocolon: a previously unreported abdominal tumour. Eur J Surg Oncol 23: 88-90. [Crossref]
- Vrettos ME, Kostopoulou E, Papavasileiou C, Sikas N, Agelidou S (2000) A mucinous tumor of the mesocolon with features of borderline malignancy. Surg Endosc 14: 595. [Crossref]
- Felemban A, Tulandi T (2000) Laparoscopic excision of a mesenteric cyst diagnosed preoperatively as an ovarian cyst. J Am Assoc Gynecol Laparosc 7: 429-431. [Crossref]
- Linden PA, Ashley SW (2000) Mucinous cystadenocarcinoma of the mesentery. Surgery 127: 707-708. [Crossref]
- Talwar A, Bell NJ, Nicholas D (2004) Mucinous cystadenoma of colonic mesentery: report of a case. Dis Colon Rectum 47: 1412-1414. [Crossref]
- Czubalski A, Barwijuk A, Radiukiewicz G (2004) [Large mesenteric cyst in a patient suspected of ovarian cyst]. Ginekol Pol 75: 545-547. [Crossref]
- Shiono S, Suda K, Nobukawa B, Arakawa A, Yamasaki S, et al. (2006) Pancreatic, hepatic, splenic, and mesenteric mucinous cystic neoplasms (MCN) are lumped together as extra ovarian MCN. Pathol Int 56: 71-77. [Crossref]
- Luo JJ, Baksh FK, Pfeifer JD, Eastman JT, Beyer FC 3rd, et al. (2008) Abdominal mucinous cystic neoplasm in a male child. Pediatr Dev Pathol 11: 46-49. [Crossref]
- Zwaveling S, den Outer AJ, da Costa SA (2008) A mucinous cystadenoma in the mesentery of the right hemicolon. Acta Chir Belg 108: 354-355. [Crossref]
- Tan JJ, Tan KK, Chew SP (2009) Mesenteric cysts: an institution experience over 14 years and review of literature. World J Surg 33: 1961-1965. [Crossref]
- Banerjee R, Gough J (1988) Cystic mucinous tumours of the mesentery and retroperitoneum: report of three cases. Histopathology 12: 527-532. [Crossref]
- Thamboo TP, Sim R, Tan SY, Yap WM (2006) Primary retroperitoneal mucinous cystadenocarcinoma in a male patient. J Clin Pathol 59: 655-657. [Crossref]




