Renal sinus cyst are benign. Cysts involving the renal pelvis are classified as Para pelvic or peri pelvic cyst (renal sinus cyst) according to their site of origin.
Para pelvic cyst: originate from the adjacent parenchyma and protrude into the renal sinus. Histologically, they are lined with a single epithelial layer.
Peri pelvic cyst: originate within the sinus itself and have a lymphatic origin.
Abbreviation
NECT=Non-enhanced Computerized Tomography, CECT= Contrast enhanced Computerized Tomography and USG= Ultra sonography
Clinical indication
49 yrs. old male patient with left loin pain.
Patient referred for Renal Ultrasound for evaluation of urinary stone and obstruction.
Renal Ultrasound reveals: Left mild hydro nephrosis. Renal pelvic was not demonstrated.
No stone. No hydro ureter.
Non-contrast CT: recommended after USG as Ultrasound demonstrates left hydro nephrosis and failed demonstrating stone.
Non-contrast CT: Again, appears as left mild hydro nephrosis without stone and hydro ureter. CT urogram performed and reveals non-dilated left pelvicalyceal system. No stone in kidneys, ureters and urinary bladder. Re-demonstration of cystic structures from left renal pelvis extending alongside of non-dilated pelvicalyceal system.
Incidental note: Mesenteric root fat stranding with multiple lymph nodes, representing mesenteric panniculitis.
These are simple renal cyst that plunge into the renal sinus from the adjacent renal parenchyma. They are usually single or few and resemble simple renal cortical cyst in morphology. A Para pelvic cyst at times may cause compression of the pelvicalyceal system resulting into hydro nephrosis.
These are frequently bilateral. They appear as water attenuation cysts closely abutting the pelvis and infundibula; rarely cause functional renal derangement by compression. When followed up they remain unchanged in size. They may be confused with hydro nephrosis on NECT and USG (as in this case), but differentiation is very obvious on CECT t as it demonstrates contrast in non-dilated pelvicalyceal system and cyst are seen adjacent to pelvicalyceal system.
Peri pelvic (Renal sinus) cysts can mimic hydro nephrosis but CT Urogram/ Intra venous urography studies will demonstrate unremarkable or narrowed/stretched/displaced (but non- dilated) collecting system.
Peri pelvic cysts are asymptomatic cysts that arise from the lymphatics of the renal hilum. Peri pelvic renal cysts defined as cysts which are situated in the renal hilus, closely related with the renal pelvis and calyces. It can be simple or multiloculated and single or multiple. Peri pelvic cysts are not buried within renal parenchyma and not appearing as mass in polar region or as exophytic on renal surface like simple renal parenchymal cyst. Usually they compress and displace the renal pelvis and vascular pedicle. If they are large, they may protrude from the renal hilum.
Their appearance is often difficult to distinguish from hydro nephrosis in Ultrasound and non-contrast CT. However, the distinction is readily apparent on contrast-enhanced excretory phase CT images, where the high-attenuation contrast agent–filled collecting system can easily be distinguished from fluid-attenuation renal sinus cysts
Peri pelvic cysts which are large enough to cause symptoms or be detectable radiographs are rare and have rarely reported in the urological or radiological literature.
Mesenteric panniculitis is a rare disorder characterized by a chronic nonspecific inflammation involving the adipose tissue of the bowel mesentery. The cause of the disease is unclear. Autoimmune response to unknown sources and ischemia of the mesentery has been proposed as pathogenic mechanisms. Whether mesenteric panniculitis occurs independently or in association with other disorders is not yet clear. The disease has been related to a variety of conditions such as vasculitis, granulomatous disease, rheumatic disease, malignancies, and pancreatitis.
The condition mostly in middle or late adulthood with a slight male predominance. When symptomatic, patients may present with a palpable abdominal mass and systemic manifestation, including abdominal pain, pyrexia, weight loss, and bowel disturbance of variable duration. Symptoms may be progressive, intermittent, or absent. Laboratory findings, including elevation in erythrocyte sedimentation rate and anaemia, are absent or nonspecific. Complete resection of the mass is usually impossible and is generally considered to be of not curable or beneficial.
In most cases the mesenteric panniculitis is incidentally identified during a CT examination for an unrelated condition as in this study.
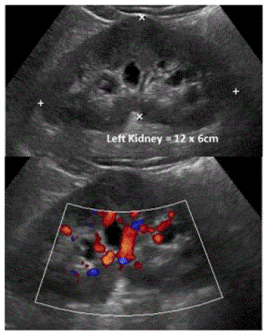
Figure 1. Renal ultrasound recommended to rule out urinary stone. Ultrasound demonstrates left mild hydro nephrosis. Renal pelvic was not demonstrated. No Stone. No hydro ureter.
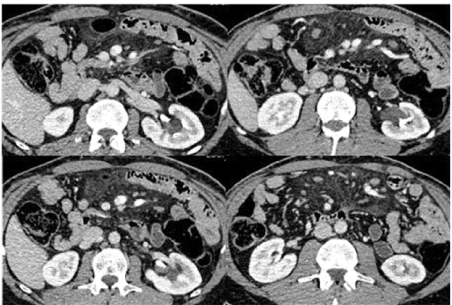
Figure 2. Axial Images: CT urogram was advised to exclude stone. CT urogram shows no hydro nephrosis. No stone in kidneys, ureters and urinary bladder. Re-demonstration of cystic structures from left renal pelvis extending alongside of calyceal system.
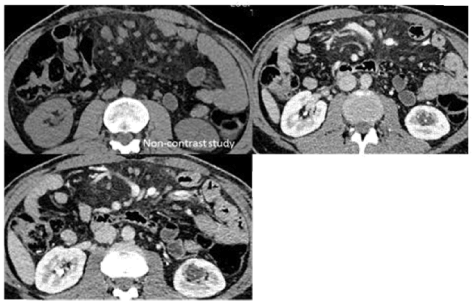
Figure 3. Axial Images: CT urogram was advised to exclude stone. CT urogram shows no hydro nephrosis. No stone in kidneys, ureters and urinary bladder. Re-demonstration of cystic structures from left renal pelvis extending alongside of non-dilated calyceal system. Incidentally noted mesenteric root fat stranding with multiple lymph nodes, representing mesenteric panniculitis. Non-contrast study for comparison.
2021 Copyright OAT. All rights reserv
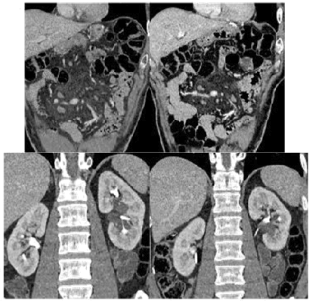
Figure 4. Coronal reconstruction: for better depiction of cystic structures in left renal pelvis extending alongside of calyceal system with no hydro nephrosis. Contrast filled pelvicalyceal system.
The disease was usually asymptomatic and frequently associated with abdominal or distal malignancy. CT features, including the envelopment of the superior mesenteric vessels by a well-delineated fatty mass, the displacement of adjacent bowel loops, well-defined soft-tissue nodules less than 5 mm, a fatty halo, and a hyper attenuated stripe, may enable differentiation of mesenteric panniculitis from other potentially confusing conditions [1-3].
- Wood CG, Stromberg LJ, Harmath CB, Horowitz JM, Chun Feng, et al. (2015) CT and MR Imaging for Evaluation of Cystic Renal Lesions and Diseases.
- Rha SE, Byun JY, Jung SE, et al. (2004) The renal sinus: pathologic spectrum and multimodality imaging approach. Radiographics 24: S117–S131. [Crossref]
- Daskalogiannaki M, Voloudaki A, Prassopoulos P, Magkanas E, Stefanaki K, et al. (2000) CT evaluation of mesenteric panniculitis: prevalence and associated diseases. AJR Am J Roentgenol [Crossref]




 2021 Copyright OAT. All rights reserv
2021 Copyright OAT. All rights reserv