Introduction: Subretinal hemorrhage is most commonly associated with choroidal neovascular membrane secondary to age-related macular degeneration (ARMD).
Case presentation: A case of submacular hemorrhage is described in a 69-year-old male with dry age-related macular degeneration (ARMD) hours after undergoing an uncomplicated, routine cataract surgery of the left eye. Methods and results: Fluoroscein angiography (FA) performed the day after surgery showed a hypofluorescent lesion corresponding to the subretinal hemorrhage. Intravitreal bevacizumab, tissue plasminogen activator (TPA), and C3F8 were given and the visual acuity (VA) improved to 20/40 on the 2-month follow-up visit.
Conclusion: To our knowledge, this is the first atypical case in which subretinal hemorrhage occurred shortly after routine cataract surgery as a result of weakening of Bruch's membrane associated with long axial length.
submacular hemorrhage, age-related macular degeneration (ARMD), fluoroscein angiography (FA), cataract surgery
A 69-year-old man with history of smoking, colon cancer, and TIA presented to the VA Long Beach Eye Clinic complaining of blurriness, glare, and halos in his vision occurring especially at night that began several years ago. The patient’s ophthalmic history was unremarkable, but his family history was significant for blindness likely secondary to ARMD. Visual acuity was 20/60 in the right eye and 20/30 in the left eye, without improvement using glasses. Intraocular pressures were 16 mmHg and 14 mmHg in the right and left eye, respectively. Fundus examination revealed mild drusen and mild retinal pigment epithelium (RPE) changes in both eyes. Optical coherence tomography (OCT) demonstrated few drusenoid pigment epithelial detachments (PEDs) causing irregularities in contour consistent with dry macular degeneration, and absence of macular edema or subretinal fluid in either eye. Slit lamp examination showed moderate nuclear sclerotic, cortical, and posterior subcapsular cataracts in both eyes. The decision was made by the patient to proceed with cataract extraction with intraocular lens implantation (CEIOL) in both eyes beginning with the right eye.
One month after successful CEIOL was performed on the right eye, a CEIOL was performed on the left eye due to imbalance in quality of vision. The procedure was performed without any intraoperative complications. However, on the evening of the surgery, the patient developed sudden blurry vision and complained of a “dark blob” in the center of his vision on the left eye. On postoperative day #1, VA was 20/70. Fundus examination of the left eye revealed an inferior sub-macular hemorrhage sparing the fovea, with sub-RPE blood just under the fovea. OCT confirmed subretinal hemorrhage in the inferotemporal macula abutting the fovea and sub-RPE hemorrhage with RPE tear. FA was performed and revealed a hypofluorescent area corresponding to the subretinal hemorrhage with no evidence of choroidal neovascular membrane (CNVM) causing leakage (Figure 1). In order to prevent further bleeding, intravitreal injection of bevacizumab 1.25 mg was performed. This injection was repeated at 4-6 week intervals hereafter, totaling 5 doses over an 8-month period.
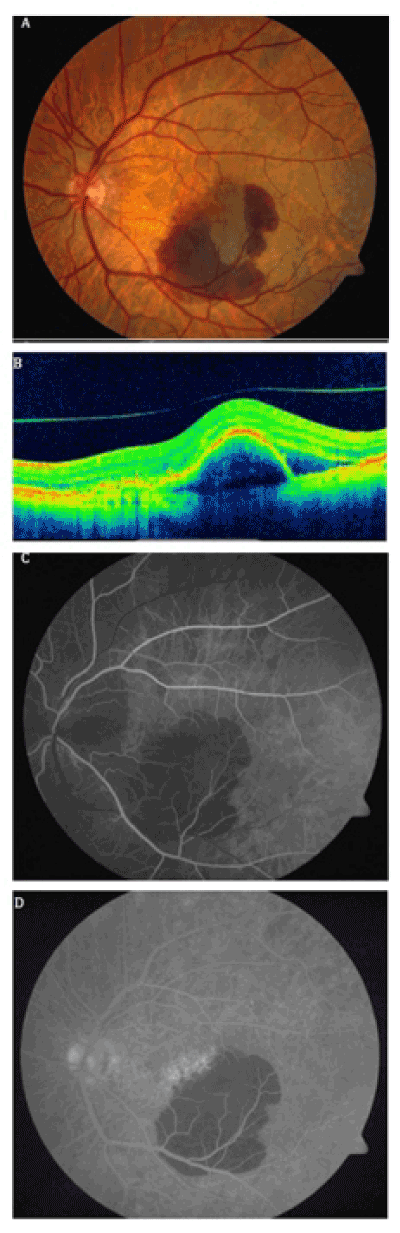
Figure 1. Left Eye on Postoperative Day #1. (A) Fundus photograph reveals subretinal hemorrhage in the inferotemporal macula next to the fovea. (B) OCT is compatible with subretinal and sub-RPE hemorrhage with RPE tear. (C) Early and (D) Late phase of FA shows a hypofluorescent area corresponding to the subretinal hemorrhage with absence of CNVM causing leakage.
On postoperative day #2, the patient also received intravitreal injection of tissue plasminogen activator (TPA) and C3F8 gas for thrombolysis and displacement of submacular hemorrhage. At the 1-month follow-up visit, VA improved to 20/50 OS with reduced subretinal fluid on OCT. Indocyanine green angiography (ICGA) showed normal filling time, no increasing hyper-ICG activity, and no evidence of leakage (Figure 2). On postoperative week #6, SRF resolved on OCT. By postoperative week #8, VA OS was 20/40.
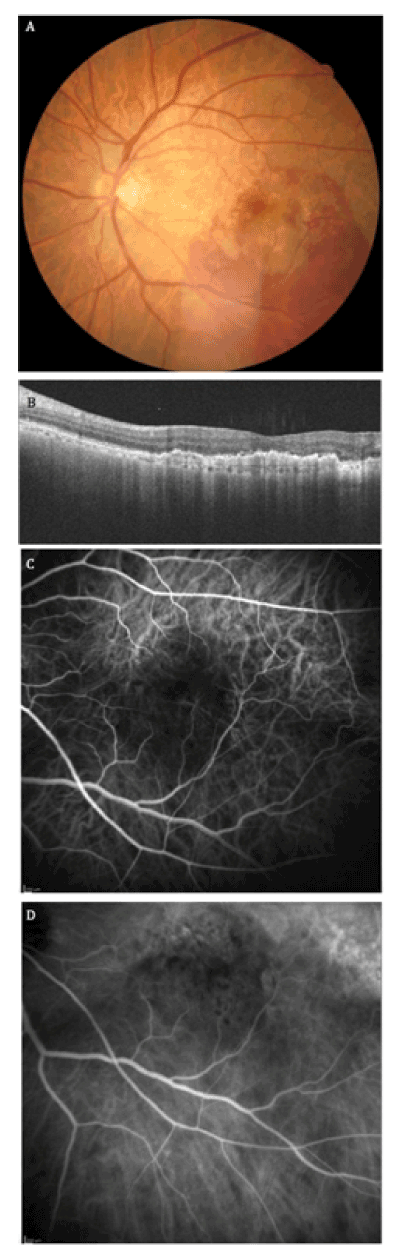
Figure 2. Left Eye on Postoperative Month #1. (A) Fundus photograph reveals improving subretinal hemorrhage. (B) OCT is compatible with reduced subretinal fluid. (C-D) ICGA shows normal filling time, no increasing hyper-ICG activity, and no evidence of leakage.
Subretinal hemorrhage is most commonly associated with choroidal neovascular membrane secondary to age-related macular degeneration (ARMD). Other causes include: presumed ocular histoplasmosis, high myopia, retinal arterial microaneurysm, and trauma [1]. In this case, the cause of subretinal hemorrhage was less likely due to ARMD as the FA showed absence of CNVM and leakage. In absence of CNVM and leakage, a more likely explanation of unilateral postoperative submacular hemorrhage in this patient is the relatively elongated axial length. Review of axial length measurements prior to surgery revealed a value of 25.46 mm OS, compared to 24.97 OD. Long axial length is characterized by anteroposterior elongation of the scleral envelope associated with secondary ocular changes such as weakening of Bruch’s membrane. This condition predisposes to RPE tearing and choroid-derived hemorrhage in the subretinal space [2].
Other similar cases of subretinal hemorrhage after cataract surgery have been reported. Kim et al. [3] reported a case of submacular hemorrhage from idiopathic polypoidal choroidal vasculopathy (IPCV) one week after CEIOL. In that case, an abrupt drop in the IOP aggravated IPCV, leading to vascular rupture and hemorrhage. In addition, Bruee et al. [4] reported three cases in which peripheral polypoidal choroidal vasculopathy was identified as an underlying potential cause in spontaneous limited choroidal hemorrhage during uncomplicated routine cataract surgery.
More common early postoperative complications of cataract surgery include cystoid macular edema, iris prolapse, endophthalmitis, dropped nucleus, raised intraocular pressure, and toxic anterior segment syndrome [5]. To our knowledge, this is the first case in which subretinal hemorrhage occurred shortly after routine cataract surgery as a result of long axial length causing weakening of Bruch's membrane.
- Hochman MA, Seery CM, Zarbin MA (1997) Pathophysiology and management of subretinal hemorrhage. Surv Ophthalmol 42: 195-213. [Crossref]
- Avila MP, Weiter JJ, Jalkh AE, Trempe CL, Pruett RC, et al. (1984) Natural history of choroidal neovascularization in degenerative myopia. Ophthalmology 91: 1573-1581. [Crossref]
- Kim M, Han J, Yu SY, Kwak HW (2012) Aggravation of polypoidal choroidal vasculopathy after cataract surgery. Indian J Ophthalmol 60: 162-163. [Crossref]
- Bruee C, Chang LK, Freund KB, Yannuzzi LA (2009) Peripheral polypoidal choroidal neovascularization, subretinal hemorrhage, and cataract surgery. Retin Cases Brief Rep 3: 364-366. [Crossref]
2021 Copyright OAT. All rights reserv
- Kurt E (2013) Early Post-Operative Complications in Cataract Surgery. Cataract Surg.


