hyperthyroidism, hyperpigmentation, periorbital, Jellinek
Among cutaneous manifestations of hyperthyroidism during Graves’ disease there is generalized or localized hyperpigmentation. When the latter involves periorbital area, it is called “Jellinek sign”. Here are two cases
Case 1: A 59 years old woman without any special pathological history has shown signs of a frank hyperthyroidism during one month. Clinical examination notes in addition to tachycardia and goiter, the presence of hyperpigmentation of the lower eyelids (Figure 1) evolving for 2 years. The biological balance confirm the diagnosis of hyperthyroidism of Graves’ disease, the anti-receptor TSH antibodies was positive.

Figure 1. periorbital hyperpigmentation with goiter in pigmented phenotype woman.
Case 2: A 37 years old man with a pigmented phenotype was referred by his endocrinologist for vitiligo of the lips. He had a severe Graves disease for 3 years. In addition to its vitiligo, dermatological examination notes a periorbital hyperpigmentation affected mostly the margins of eyelids since the latest year (Figure 2). No medication or other pathology were mentioned.
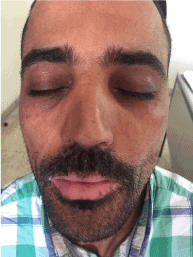
Figure 2. hyperpigmentation of the eyelids with exophtalmia and lips vitiligo in a man with severe Graves’ disease.
Graves' disease (GD) is an autoimmune thyroiditis considered to be the most common cause of hyperthyroidism in iodine deficient areas. It involves all organ systems and the skin is no exception. Cutaneous manifestations of GD are variable; affecting all the integuments (skin, mucosa, nails and hair). There are two types: specific extrathyroidal manifestations; affecting the orbit (Graves’ orbitopathy) and the skin (thyroid dermopathy or pretibial myxedema) which are correlated to severe forms; and other cutaneous signs, common to all the etiologies of hyperthyroidism [1].
In hyperthyroidism, skin shows some signs like warmness, moistness, softness, hyperhidrosis, onycholysis, alopecia, and hyperpigmentation [2]. Indeed, about 2% of patients exhibit hyperpigmentation in both generalized and localized distribution, typically to the palmar creases, soles, gingiva, and buccal mucosa, probably secondary to increased release of pituitary adrenocorticotropic hormone compensating for accelerated cortisol degeneration [3]. Rarely, this hyperpigmentation involves periorbital areas and eyelids, and then it’s called Jellinek sign [4].
Jellinek sign still poorly reported despite being known for a long time by veteran dermatologists and endocrinologists. It is a progressively installed hyperpigmentation of the eyelids, more marked on pigmented skin [5], generally appearing subsequent to the development of thyroid disease, but may be the first presenting sign or even precede the diagnosis by many years; Thus, it could help to early detect Graves’ disease. Classically, it regresses after treatment of hyperthyroidism.
In addition to Jellinek sign, periorbital hyperpigmentation may be secondary to several conditions that could be eliminated easily, namely genetic excessive pigmentation, post inflammatory hyperpigmentation secondary to atopic or allergic contact dermatitis, systemic disorders, drug induced hyperpigmentation, sleep disturbances, or nutritional deficiencies [6].
The authors declare that they have no competing interest.
- Bartalena L, Fatourechi V (2014) Extrathyroidal manifestations of Graves' disease: a 2014 update. J Endocrinol Invest 37: 691-700.
- Doshi DN, Blyumin ML, Kimball AB (2008) Cutaneous manifestations of thyroid disease. ClinDermatol 26: 283-287.
- Kasumagic-Halilovic E (2014) Thyroid Disease and the Skin. Annals Thyroid Res 1: 27-31.
- Urrets-Zavalia JA, Esposito E, Garay I, Monti R, Ruiz-Lascano A, et al. (2016) The eye and the skin in endocrine metabolic diseases. Clin Dermatol 34: 151-65.
- Anania C, Rubenfeld S (1989) Hyperpigmentation in Graves' disease. Thyroidology 1: 127-129.
- Roberts WE (2014) Periorbital hyperpigmentation: review of etiology, medical evaluation, and aesthetic treatment. J Drugs Dermatol13: 472-482.


