Abstract
Introduction: The use of serum or plasma in clinical pathology remains controversial. Using gel separator tubes is time consuming and may not help in clinical analysis during emergency cases. We compared the effect of heparin, K2EDTA, sodium citrate anticoagulants to gel separator tubes on lipid profile.
Methods: This cross-sectional study was conducted in Bekwai Government Hospital. A total number of 115 participants were recruited for this study. Fasting blood samples were collected from each patient into heparin, K2EDTA, sodium citrate and gel separator tubes simultaneously. Samples in anticoagulant tubes were immediately centrifuged and plasma was obtained while samples in gel separator tubes were made to clot before centrifugation to obtain serum. The plasma and serum obtained was used to estimate total cholesterol (TC), triglyceride (TG), low density lipoprotein (LDL-c), and high-density lipoprotein (HDL-c) using an automated chemistry Analyser.
Results: The mean levels of TC (p<0.001), TG (p<0.001), LDL-c (p<0.0001) were reduced and significantly different in heparin tubes compared to gel separator tubes. Using K2EDTA the mean levels of TG (p>0.05) was not different but TC (p<0.001) and LDL-c (p<0.001) were reduced and significantly different compared to gel separator tubes. Meanwhile, mean levels of TC (p<0.05), TG (p<0.05), LDL-c (p<0.05) were reduced and significantly different in sodium citrate tubes compared to gel separator tubes. Mean HDL-c levels did not significantly differ using heparin, K2EDTA and sodium citrate anticoagulant tube compared to gel separator tubes (p>0.05).
Conclusion: K2EDTA anticoagulant tubes may not have significant changes in TG levels. Heparin, K2EDTA and sodium citrate anticoagulant tubes may serve as substitute for gel separator tube for HDL-c analysis in emergency cases.
Key words
anticoagulants,gel separator,heparin,K2EDTA,lipoprotein, sodium citrate
Abbreviations:
CVD: Cardiovascular diseases; HDL: High density lipoprotein; K2EDTA: Ethylene Diamine Tetraacetic Acid Di Potassium; LDL:Low Density Lipoprotein; TC: Total Cholesterol; TG: Triglyceride
Introduction
Although cardiovascular disease (CVD) is still the leading cause of death, age-related CVD mortality has also been falling over the past 25-30 years. Numerous studies suggest that risk-factor reductions and treatment of established disease each account for approximately 40-60% of the decline in CVD mortality, with another 0-10% attributable to undetermined causes [1].
Lipid profile is the most important blood test for cardiac risk assessment. The lipid profile is used to help determine an individual's risk of heart disease and to help make decisions about what treatment may be best if there is borderline or high risk. It measures TC, TG, HDL-c and LDL-c in the blood of an individual [2].
Anticoagulants are additives that inhibit the clotting of blood, thereby ensuring the concentration of the substance to be measured is changed as little as possible before the analytical [3]. Anticoagulation is achieved either by the chelating of calcium ions (K2EDTA, citrate) or by the inhibition of thrombin (heparin). Serum from coagulated blood is the preferred specimen for clinical chemistry analysis but plasma obtained with an appropriate anticoagulant may be an equally valid specimen and in certain conditions preferable to serum [4]. Although these anticoagulants are not free of interferences, it is still used most recently by some laboratories like Roche which might be due to the fact that plasma, unlike serum, can be centrifuged immediately after taking the blood sample. Besides, coagulated blood prevents blocking of autoanalyzer probes with clots of blood particles and its anticipated negligible effect on cholesterol [5].
Because the harvest of serum requires 15-30 min wait for coagulation completion before centrifugation, the use of plasma expedites analysis in emergency situations. Furthermore, plasma yield from a given volume of whole blood is always greater than the yield of serum [4]. Thus, analysis must be performed on plasma anti-coagulated with various types of anticoagulants, most commonly K2EDTA, sodium citrate and lithium heparin. The use of serum or plasma in clinical pathology remains controversial. Serum is preferred by many laboratories for biochemical test since it avoids the addition of anticoagulants that can interfere with some analytical methods or change the concentration of the parameters being measured [6]. However, the use of plasma is preferred in some centres because plasma samples can be centrifuged directly after sample collection unlike serum which has to wait until coagulation is complete. Thus, the use of plasma would allow quick analysis of biochemical measurement in an emergency situation. There is little information on the effects of the different types of anticoagulants on lipid profile parameters in the Ghanaian setting. It is against this background that this study determined the effect of K2EDTA, lithium heparin and sodium citrate on lipid profile and compared it to gel separator tube.
Materials and method
The study is a cross-sectional study which was conducted at the Bekwai Government Hospital. Bekwai Government Hospital is a governmental organization which seeks to provide holistic health care to all patients that visit the facility. In all a total 115 patients visiting the laboratory facility of the hospital were consented and absorbed into the study. All the subjects considered were patient who were above 18 years and had fasted for at least twelve hours. Patients who had not fasted for 8-12 hours were excluded. An approved research information leaflet form was provided to prospective participants to decide if they would like to be part of the study.
Sample collection and biochemical assays
A volume of 6 mL of venous blood was taken after a 12 hour or minimum of 8 hours overnight fast via phlebotomy. Approximately, 1.5ml of the blood collected was be dispensed into the four test tubes (K2EDTA, Sodium citrate, Lithium heparin and Gel separator tubes) and were immediately analyzed for total cholesterol (TC), triglycerides (TG) and HDL-cholesterol (HDL-c) using BS-130 Chemistry Analyzer by MINDRAY diagnostics Limited, USA. The concentration LDL-cholesterol was calculated using the Friedewald formula (LDL-c=TC-HDL-c-(1∕5) TG). The biochemical assays were repeated for all samples.
Total cholesterol concentration was determined after enzymatic hydrolysis and oxidation. The colorimetric indicator is quinoneimine which is generated from 4-aminoantipyrine and phenol by hydrogen peroxide under the catalytic action of peroxidase (Tinder’ reaction).
Triglyceride was determined after enzymatic splitting with lipoprotein lipase. Indicator is quinoneimine which is generated from 4-aminoantipyrine and 4-chlorophyl by hydrogen peroxide under the catalytic action of peroxidase.
The method used for the HDL-c determination employs an immune inhibition reagent which measures HDL-c directly. The method is in a two-reagent format. The first reagent contains anti human β-lipoprotein antibody which binds to lipoproteins (LDL-c, VLDL-c and chylomicrons) other than HDL. The second reagent contains enzymes which then selectively react with the cholesterol present in the HDL particles. Consequently, only HDL cholesterol is subject to cholesterol measurement.
Data analysis
Information from all the subjects was recorded on an Excel spreadsheet. It was then analyzed using Graph Pad Prism version 6. The percentage or proportions were calculated for discrete variables while the mean with its standard deviation computed for continuous variables. Paired sample t-test was used in comparing lipid levels in anticoagulant tubes against gel separator tubes. The 95% confidence interval or the p-value was calculated. In all statistical tests, a value of p<0.05 was considered significant.
Results
As shown in Figure 1, there were more females 55.7%(64/115) compared to male participants 47.5%(51/115).
The mean age of participants was 40.2 years. The most represented age group was 40-59 years 56.5%(65/115), followed by 60-79 years 21.7%(25/115), 20-39 years 14.8%(17/115) and <20 years 7.0%(8/115) (Figure 2). Table 1 shows the effect of anticoagulants on lipid profile markers. Mean levels of total cholesterol, triglycerides and LDL-c were significantly lower in heparin tubes, K2EDTA and sodium citrate anticoagulant tube compared to serum gel (p<0.05). However, levels of HDL-c were not significantly different in anticoagulant tubes compared to gel separator.
|
|
Gel separator
|
Heparin tube
|
K2EDTA
|
Sodium citrate
|
|
Parameters (mmol/l)
|
(n=115)
|
(n=115)
|
(n=115)
|
(n=115)
|
|
T. cholesterol
|
4.52 ± 0.06
|
4.37 ± 0.04**
|
4.44 ± 0.03**
|
4.48 ± 0.02*
|
|
Triglyceride
|
0.65 ± 0.03
|
0.60 ± 0.02**
|
0.64 ± 0.02
|
0.62 ± 0.03*
|
|
HDL-c
|
1.47 ± 0.04
|
1.47 ± 0.01
|
1.46 ± 0.01
|
1.48 ± 0.03
|
|
LDL-c
|
2.86 ± 0.06
|
2.74 ± 0.06***
|
2.78 ± 0.05**
|
2.80 ± 0.06*
|
Table 1. Mean levels of lipid profile markers in anticoagulants tube compared to gel separator tubes. Values are presented mean ± SD. *p<0.05, **p<0.001, ***p<0.0001 indicate the degree of significant difference compared to gel separator tube. HDL: high density lipoprotein; LDL: Low density lipoprotein.
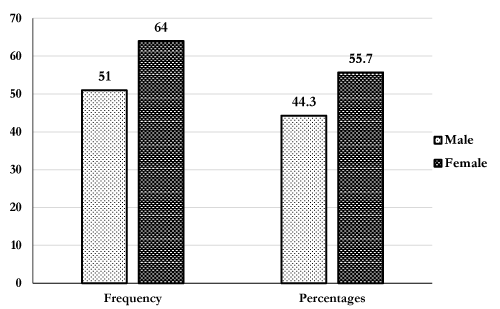
Figure 1. Gender distribution of study participants.
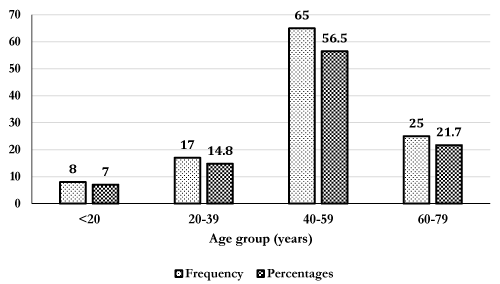
Figure 2. Age distribution of study participants.
Table 2 shows the mean difference between serum gel separator tube and plasma heparin, K2EDTA and sodium citrate. The mean difference for total cholesterol, triglycerides, HDL-c and LDL-c using heparin tube in comparison with gel separator tube were 0.15 mmol/l, 0.05 mmol/l, 0.0 mmol/l and 0.12 mmol/l respectively. The mean difference for total cholesterol, triglycerides, HDL-c and LDL-c using K2EDTA in comparison with gel separator tube were 0.08 mmol/l, 0.01 mmol/l, 0.01 mmol/l and 0.08 mmol/l respectively. The mean difference for total cholesterol, triglycerides, HDL-c and LDL-c using sodium citrate in comparison with gel separator tube were 0.04 mmol/l, 0.03 mmol/l, -0.01 mmol/l and 0.06 mmol/l respectively.
|
|
Heparin tube
|
K2EDTA
|
Sodium citrate
|
|
Parameters (mmol/l)
|
(n=115)
|
(n=115)
|
(n=115)
|
|
T. cholesterol
|
0.15
|
0.08
|
0.04
|
|
Triglyceride
|
0.05
|
0.01
|
0.03
|
|
HDL-c
|
0.00
|
0.01
|
-0.01
|
|
LDL-c 2021 Copyright OAT. All rights reserv
|
0.12
|
0.08
|
0.06
|
Table 2. Mean effect difference (Bias) between gel separator tubes and anticoagulant tube.
Discussion
The use of serum or plasma in clinical pathology remains controversial. Therefore, the study determined the effect of K2EDTA, lithium heparin and sodium citrate on lipid profile and compared it to gel. The results of this study indicated a statistically significantly reduced mean levels of TC, LDL-c, and TG when heparin, K2EDTA and sodium citrate anticoagulant tubes were used compared to gel separator tube (p<0.05). Meanwhile, HDL-c levels was non-significantly reduced when heparin, K2EDTA and sodium citrate anticoagulant tubes were used compared to gel separator tube. This study observed significantly reduced levels of TC, TG and LDL-c using heparin anticoagulant tube compared to gel separator tube (Table 1).
The reduced levels in TG is consistent with a cross-sectional study by Yang et al. [7] who observed a significant reduction in TG levels when low molecular weight heparin was administered to hyperlipidaemia diabetic patients on haemodialysis. Another study by Katopodis et al. [8] has shown that a reduction in TG levels in first, second and third hour administration of unfractionated IV heparin in patient on renal replacement therapy. Although the aforementioned studies determined the effect of administered heparin by on lipid TG, this study used in vitro heparin anticoagulant tube. The mechanism linking heparin-induced decrease in TG level in vitro is not well understood. However, heparin is directly stimulating of lipoprotein lipase (LPL) release into plasma from epithelial cells. The increase in LPL enhances the body's ability to remove TG, thereby lowering plasma concentrations [9].
Another finding of this study was that heparin anticoagulant had no significant change in HDL-c levels compared to using gel separator tube as depicted by a mean difference of 0.0 mmol/l. A study by Sassolas et al. [10] did not find any significant difference in using heparin anticoagulant which agree with the findings of this study. This implies that heparin anticoagulant tube could equally be used for measuring HDL assay in clinical chemistry laboratories. However, a large cohort of study is needed to confirm this finding.
There was a significantly reduced level of TC, and LDL-c by when K2EDTA anticoagulant tube was used (Table 1). K2EDTA anticoagulant did not significantly alter in concentration of TG and HDL-c levels compared to using gel separator tube as depicted by a mean difference of 0.0mmol/l though a reduced concentration were observed when compared to gel separator tube (Table 2). A study by Sharifi et al. [11] did not find any significant difference in TG concentration using K2EDTA anticoagulant and this concur well with the findings of this study. This implies that K2EDTA anticoagulant tube could equally be used for measuring HDL-c and TG assay in clinical chemistry laboratories. However, a large cohort of study is needed to confirm this findings. However, the non-significant variation in levels triglyceride and HDL-c using K2EDTA anticoagulant is not clear.
There was a significantly reduced level of TC, TG and LDL-c by a mean difference of 0.04 mmol/l, 0.03 mmol/l, and 0.06 mmol/l respectively when sodium citrate anticoagulant tube was used compared to gel separator tube (Table 2). It is believed that small variations in the amount of blood collected into citrate tubes such as a dilution of >1:10 could have contributed to the lower concentration in citrated plasma. Citrate also could have inhibited the reaction of TC, TG, HDL-c and LDL-c [12]. However, the exact reason for this result is not clear. Another finding of this study was the increase and non-significant in HDL-c levels with an average bias of -0.01 mmol/l using sodium citrate tube compared to gel separator tubes. It is possible that HDL-c concentration are not affected by citrate anticoagulant and may be useful in emergency clinical chemistry assay.
Conclusion
Using K2EDTA tube for triglyceride estimation and Heparin, K2EDTA and sodium citrate anticoagulant for HDL-c estimation does not significantly alter concentrations compared to using gel separator tube and thus should be employed in routine clinical chemistry assay during emergency situations. Further studies are needed to confirm this finding using a large cohort of healthy population.
Ethics approval and consent to participate
The study was approved by the Committee on Human Research Publication and Ethics, Kwame Nkrumah University of Science and Technology, Kumasi Ghana. Written informed consent was obtained from each participant. Respondents were assured that the information gathered was to be used strictly for research and academic purpose only. In addition, respondents were given the freedom to opt out any time they think they cannot continue with the study.
Authors’ contributions
EOA contributed to the conception of the research idea, data collection, interpretation, paper drafting and revision. WKBAO contributed to the conception of the research idea. CO, EA, BOA, BA, and SD contributed to the paper drafting and revision. SPS contributed to data collection and sample analysis. AAO contributed to patient recruitment and sample collection. All authors approved the final manuscript before publication and agree to be accountable for all aspects of the work.
Acknowledgement
Our sincere gratitude to the management and staffs of the Bekwai Government hospital, Laboratory Unit.
References
- Fuster V, Mearns BM (2009) The CVD paradox: mortality vs prevalence. Nat Rev Cardiol 6: 669. [Crossref]
- Williams CL, Hayman LL, Daniels SR, Robinson TN, Steinberger J, et al. (2002) Cardiovascular health in childhood: A statement for health professionals from the Committee on Atherosclerosis, Hypertension, and Obesity in the Young (AHOY) of the Council on Cardiovascular Disease in the Young, American Heart Association. Circulation 106: 143-160. [Crossref]
- Guder WG, Ehret W, da Fonseca-Wollheim F, Heil W, Muller-Plathe O, Schmitt Y, et al. (2002) The quality of diagnostic samples. Laboratoriums Medizin 26: 267-283.
- Young D, Bermes E (1999) Tietz Textbook of Clinical Chemistry. In: Specimen Collection and Processing: Sources of Biological Variation. (edn). Saunders Philadelphia pp: 42-72.
- Wild D (2013) The immunoassay handbook: theory and applications of ligand binding, ELISA and related techniques: Newnes.
- Cerón JJ, Marti´nez-Subiela S, Hennemann C, Tecles F (2004) The effects of different anticoagulants on routine canine plasma biochemistry. Vet J 167: 294-301. [Crossref]
- Yang CW, Wu TH, Huang CC (1998) Low molecular weight heparin reduces triglyceride, VLDL and cholesterol/HDL levels in hyperlipidemic diabetic patients on hemodialysis. Am J Nephrol 18: 384-390. [Crossref]
- Katopodis KP, Koliousi E, Gouva C, Balafa O, Bairaktari E, et al. (2007) Acute effect of heparin on lipid parameters in patients on renal replacement therapy. ASAIO J 53: 46-49. [Crossref]
- Weintraub M, Rassin T, Eisenberg S, Ringel Y, Grosskopf I, et al. (1994) Continuous intravenous heparin administration in humans causes a decrease in serum lipolytic activity and accumulation of chylomicrons in circulation. J Lipid Res 35: 229-238. [Crossref]
- Sassolas A, Cheillan D, Drai J, Bondon P, Cartier R (2004) Should blood samples be drawn on heparin-anticoagulant for lipid analysis? Ann Biol Clin (Paris) 62: 583-586. [Crossref]
- Sharifi M, Javdan S, Fesharaki M (2004) The Effect of EDTA and Garlic Extract Combination on Plasma Lipids, Lipoporteins, and Fatty Streaks in Cholesterol Fed Male Rabbit Aorta. J Res Med Sci 9: 270-274.
- Stokol T, Tarrant JM, Scarlett JM (2001) Overestimation of canine albumin concentration with the bromcresol green method in heparinized plasma samples. Vet Clin Pathol 30: 170-176. [Crossref]


