Abstract
The project was developed with a goal to decrease stress and create a better work-life balance for registered nurses (RN) and staff working within two hospitals and one outpatient clinic in northeast central Pennsylvania. A review of the literature for best practices in fostering such an environment was the first step. This led to three evidenced-based projects: Compassion Fatigue – Causes and Symptoms; Compassion Fatigue – Interventions; and Resilience – What Can Improve Resilience? The outcome of the literature evaluation led to the development of this research project to evaluate levels of compassion and resilience in nurses and unit staff, and whether interventions can improve and restore compassion. The purpose of this quasi-experimental study was to evaluate the effectiveness of a staff implemented activity plan as demonstrated by comparison of pre-and post-survey results. The Professional Quality of Life Scale and the Connor-Davidson Resilience Scale are two validated survey tools that were used to measure compassion and resilience before and after the implementation of a staff developed activity plan. A convenience sample of approximately 180 nurses and support staff were used. All RNs and support staff Licensed Practical Nurses (LPNs), Unit Desk Clerks (UDCs), Nursing Assistants (NAs), and Patient Access Representatives (PARS)) from five different units were invited to participate. Nurses and staff completed the two surveys as a baseline, then completed a self-developed activity plan, and again completed the two surveys after the project. Findings showed that a self-developed activity plan can improve levels of compassion and resilience. The results reflected the goal although not to a high degree of change. Satisfaction and resilience can improve, and burnout and trauma can decrease when nurses work on creating the change. The change must come from within and nurses must identify the actions that work for them as individuals. The next important aspect is that the activity plans must be seriously created and worked on daily. Degree of commitment and readiness to change is important for such a project to be effective. The overall goal was to provide staff with resources that would help to reduce levels of stress, create a better work-life balance, promote resilience and decrease levels of compassion fatigue.
Key words
nursing, evidence based practice, research findings, fatigue
Background
For the past two years, this hospital in northeastern central Pennsylvania has experienced a decrease in their RN satisfaction scores (National Database of Nursing Quality Indicators). Feedback from exiting staff indicated the major reasons for leaving inpatient nursing was because staff were looking for less stressful positions coupled with hours of work that provided a better work-life balance. In addition, staff often complained that the stress of their jobs was a major element of dissatisfaction in their current nursing positions. As a Magnet organization, the hospital has an obligation to foster a healthy work environment that promotes job satisfaction, professional growth, and a healthy work-life balance. Thus, the need to conduct a review of the literature for best practices in fostering such an environment was identified. This further led to three evidenced-based projects: Compassion Fatigue–Causes and Symptoms; Compassion Fatigue–Interventions; and Resilience–What Can Improve Resilience? The outcome of the literature evaluation led to the development of this research project to evaluate levels of compassion and resilience in nurses and unit staff, and whether interventions could improve and restore compassion.
Overview of three evidence-based projects completed using the Johns Hopkins model of evidence based practice
The project began by doing an extensive review of the literature. After reviewing the literature, the decision was made to separate out the topics and complete three separate evidence-based projects: Causes and symptoms of compassion fatigue. Interventions for compassion fatigue, and resilience. The three outcomes are described below:
Causes and symptoms of compassion fatigue (CF)
It is the nature of healthcare professionals to be empathetic and overly involved in caring for their patients. This puts healthcare workers, such as nurses, at increased risk for compassion fatigue (CF). Compassion fatigue is a progressive and cumulative process that is influenced by interaction with patients, the nurses’ own resources and exposure to stress [1,2]. CF is a combination of burnout and secondary traumatic stress. Gilmore [3], states that compassion fatigue is not simply burnout; rather it is a behavioral response to constantly helping people who are sick and suffering.
Evidence has shown there are several factors that may lead to compassion fatigue. Prolonged and intense contact with patients, the constant giving of self, lack of recognition, the lack of self-care and depression are all causes of compassion fatigue. An individual’s resilience, capacity to cope and compassion satisfaction are all predictors of a nurse’s risk for developing CF [4,5]. Signs and symptoms include apathy and/or emotional numbness, over involvement or inability to connect with patients, stress and anxiety, depression, feelings of hopelessness or powerlessness, sleep disturbances, headaches, increased absenteeism, drug and alcohol abuse. Sorenson, Bolick, Wright & Manilton [6] presented a review of 307 articles summarizing prevalence, risk factors, symptoms and prevention measures.
The impact of CF is detrimental to the nurse, the patient, the organization and even society. Manifestations of CF may appear as anger, apathy, sarcasm, hopelessness or irritability. In research by Sheppard [7], the findings supported burnout as a significant risk factor for compassion fatigue, but that fear, distress and hypervigilance are also significant correlates of compassion fatigue. Compassion fatigue can lead to burnout, and may cause a nurse to be forgetful, have a decrease in attention span and even physical illness [8]. Therefore, CF may be attributed to job dissatisfaction, turnover, sick time, lower patient satisfaction and poor patient outcomes.
Improving recognition and awareness of CF will help to prevent its devastating effects. Early identification of CF coupled with effective interventions must exist to improve nurse satisfaction and patient care, and decrease nurse turnover [9]. Learning to intervene in those with CF will lead to resilience and help to eliminate CF.
Interventions for compassion fatigue
Healthcare organizations must understand the concept of CF and recognize when it occurs to develop support and interventions tailored to reduce CF, which will allow nurses to continue to give and provide excellent care [10]. Nurses are considered caring and compassionate professionals who are sought out by patients and families for support during times of physical, emotional and spiritual distress. However, with a continuous giving of self, nurses are at risk for developing compassion fatigue [10]. Compassion fatigue (CF) among nurses has been associated with less effective delivery of care which can lead to increased mortality, increase infection rates and decreased patient satisfaction [11].
Per an article by Aycock and Boyle [12], limited information is available about interventions to manage CF. Thus, a survey study was conducted to identify resources available to oncology nurses. The interventions were grouped into three major categories: onsite professional resources, educational programs and specialized retreats. Examples of onsite professional resources included employee assistance programs, pastoral care, counselor, and support groups/staff.
A program at Florida State University developed an Accelerated Recovery Program where certified Compassion Fatigue Specialists treated caregivers. They found that symptoms of CF were responsive to treatment and may even be the incentive that leads to the enhancement of clinical skills and personal life enrichment [13]. The Hospital of the University of Pennsylvania developed a nurse renewal program after completing a pre-implementation survey to get a better understanding of nursing interest for interventions. Using the survey information, they created a center that included a computer café, a meeting room, space for yoga and other training classes, relaxation room, meditation room, a lending library and refreshment room [11].
Much of the literature that discussed interventions to treat CF suggested implementation of assessment surveys to measure the effectiveness of the interventions. The surveys were conducted pre-and post-interventions. Examples of surveys that can be used are the Professional Quality Life Scale (Pro-QOL), Compassion Satisfaction Fatigue (CSF) test and the Maslach Burnout Inventory. The surveys alone provided education to nurses about CF [14].
Educational programs can consist of work/life balance programs and work setting interventions. In the article by Harris and Quinn [10], a “nourishing workplace” is crucial to overcoming CF. Specific work place interventions included acknowledgement of CF, placing CF on meeting agendas, discussion about patient care situations, acknowledging worker contributions, education, time outs in high acuity areas, rotating care of difficult patients, providing quiet rooms for staff, unit-based debriefing, offering collective ways to share difficult experiences and meeting outside of work.
Berger, Polivka, Smoot, & Owens [15], discussed a 12-week resilience training program for intensive care unit nurses. This program featured workshops, expressive writing sessions, counseling sessions, mindfulness-based stress reduction and an aerobic exercise program. Results demonstrated decreased anxiety/depression scores and improved resilience scores. Raab [16] explained possible methods including mindfulness to improve self-compassion within health care professionals.
By effectively implementing interventions to combat CF, organizations have seen an increase in staff morale and productivity, engagement in facility initiatives, reduced sick time, lower turnover rates as well as higher patient and family satisfaction [17]. The literature findings emphasized that for such interventions to be optimally effective, an organization needs support of leadership and leadership must invest (D. Davis, personal communication, January 13, 2016).
Resilience
Experts in resilience and resilience research have described the phenomenon as both a process and an outcome. Thus, resilience is an attribute that can be developed and enhanced through education and support [18-20]. Over the years, resilience has been defined as successful adaptation (including the ability to thrive) in the face of significant adversity.
Today’s nurses face increasing work force stress related to the nursing shortage [21]. It is anticipated that the shortage will continue to peak over the next 20 years related to age attrition, avoidance of the profession, poor recruitment, a shortage of faculty, vast increases in the number of people over age 65 and healthcare reform giving millions of people access to healthcare [22,23]. Given the fact that these dynamics will affect individual nurses’ wellbeing and the quality of patient care, it is imperative that healthcare organizations focus on ways to create a healthy work environment that fosters resilience and decreases the impact of workplace stress [21,24].
A review of nursing literature was completed to identify ways to better prepare nurses for practice and identify strategies to help nurses become and stay resilient. Resilience has been defined as the ability to bounce back or cope successfully despite adverse circumstances [25]. In a correlational cross sectional study of operating room nurses, Gillespie et al. [26] found that hope, self-efficiency, coping, control and competency explained 60% of the variance in resilience, but hope was the strongest unique contributor to resilience. Age, experience and years of employment were not statically significant in explaining resilience in these nurses [18].
A phenomenological study by Hodges, Keeley, and Troyan [27] looked at acute care nurses and identified themes that related to developing resilience in nursing practice: learning the milieu and culture, learning RN skill sets (techniques, time management and pace), and sensing discrepancies of one’s identity as a professional nurse. Critical reflection and reconciliation were also identified as successful strategies by the nurses.
A descriptive study in a Pediatric Intensive Care Unit, showed that interpersonal interactions including 1-on-1 discussion with colleagues and informal social gatherings out of work had a positive impact on resilience [28]. Other resources such as taking a break from stressful patients, being relieved of duty after a patient death, providing support for staff, structured social activities outside of work and Schwartz rounds were impactful, but underused [28]. A qualitative study by Cope, Jones and Hendricks [29] discussed how resilience can be taught and how it needs to be an essential element of professional practice.
Organizational approaches to help develop resilience were discussed in a quantitative study by Hudgins [22]. This study included 89 nurse leaders from a large, multi-hospital healthcare system. The results showed a significant relationship between resilience, job satisfaction and anticipated turnover [22]. The findings supported that a stable nursing team had a positive impact on patient outcomes. Nurse leaders can mitigate the impact of the nursing shortage by enhancing their resilience and by recruiting, hiring and retaining resilient staff nurses to improve their “intent to remain.” Nurse leaders with higher resilience are more likely to remain in their leadership positions [22]. Assi and Leichamn [30] present details on how healthcare institutions can use holistic care models to promote nurse resilience.
Rushton, Batcheller, Schroeder, and Donohue [31], looked at burnout and resilience among nurses working in high-intensity settings such as pediatrics, oncology and critical care. A cross sectional survey was used to describe the experiences of these nurses. The results indicated that nurses were vulnerable to burnout because of patients’ intense needs, uncertain outcomes, and the highly-charged context of the nurses’ work, especially the impact of witnessing suffering and death. Moral distress was a significant predictor of burnout. There was also an association between burnout and resilience. Greater resilience protected nurses from emotional exhaustion and contributed to personal accomplishment. Also, spiritual wellbeing reduced emotional exhaustion and depersonalization. Higher levels of resilience were associated with hope and reduced stress. The authors concluded that developing strategies to reduce nurses’ vulnerability to emotional exhaustion and to increase hope, spiritual and physical well-being helps cultivate resilience [31]. Gillman, Adams, Kovac, Kilcullen, House and Doyle [32] presented a comprehensive review of literature and discussed strategies which can be used to promote coping and resilience in nurses.
This review of literature included multiple studies that discussed factors that influence resilience. However, limited empirical evidence made it difficult to determine the most effective approaches to promote development of resilience. Also, there was a lack of large, well designed, multi-site, experimental studies that evaluated the effectiveness of organizational interventions.
The findings from the evidence-based projects led to discussion among the nurses of moving forward with a research project to assess whether staff could on their own, improve their levels of compassion and resilience. The remainder of the article presents the research study.
Hypothesis and specific aims for the research project
Hypotheses
Nurses and staff who complete an activity plan to improve compassion will demonstrate an improvement in scores on the Professional Quality of Life Scale and the Connor-Davidson Resilience Scale.
Specific Aim 1
Nurses and staff who complete an activity plan to improve their level of compassion, will reflect a difference in the scores on the Professional Quality of Life Scale.
Specific Aim 2
Nurses and staff who complete an activity plan to improve their level of resilience, will reflect a difference in the on the Connor-Davidson Resilience Scale.
Specific Aim 3
The overall unit resilience score will influence the post activity Professional Quality of Life scores.
Theoretical framework: professional practice model and Watson’s caring theory
The hospital’s Professional Practice Model (PPM) guides nursing practice and the delivery of patient care. The illustration below depicts the professional practice model, starting in the center and moving outward through each concentric ring. Nurses’ actions at Geisinger Medical Center are based on the central focus of the professional practice model: the patient and family. The next ring focuses on the Nursing Care Delivery Model integrated with our theorists. Continuing the outer progression, nursing values are listed on the next outermost ring, followed by the nursing vision and mission — Quality, Securing the Legacy, Innovations, and Market Growth — to focus on our values of caring.
Jean Watson’s Caring Theory provides the framework for the practice of nursing and highlights the nurse-patient relationship and human interaction that occurs with each patient encounter. The central focus of the model is the patient and family, emphasizing that this is the core of nursing practice. Caring is a value also recognized by the entire Health System as the basis for all interactions with patients, the healthcare team, and each another.
Watson’s Human Caring Theory [33,34] not only provides the foundation for implementation of compassionate nursing care designed to enhance patient healing, but also for fostering nurse well-being and progression toward self-actualization. This theoretical perspective recognizes the importance of the caregiver (and caregiver well-being) and requires a commitment to self-care as an essential aspect in enabling nurses to work from a caring-healing paradigm.
Sister Callista Roy’s Theory of Adaptation [35] compliments Watson’s theory in guiding nursing practice. Nurses assist patients and families in adapting to their continually changing health and form caring nurse-patient relationships. The PPM follows this belief by placing the patient and the family, our clients, at the center of the professional practice model to create the foundation for nursing practice (Figure 1).
Figure 1. Professional practice model to create the foundation for nursing practice
The practice of nursing in a caring manner as outlined in the PPM requires effort from the nurse during each interaction. CF may lead to a sense of decreased caring that may be felt by the patient or internalized by the nurse. Nurses who are experiencing compassion fatigue need attention to ensure that they can interact in a caring fashion with the patients and the others who they encounter each day. Developing resilience and the ability to bounce back from fatigue is vital for self-care.
Project design
A quasi-experimental design was used for this evidence-based project. A sample of convenience was used. All RNs and support staff (LPNs, UDCs, NAs, and PARs) from four different inpatient units and one clinic located at two hospitals in the health system were invited to participate. Of the 188-staff employed on those five units, it was expected that 80% or 150 staff would chose to participate. Results indicated that 168 staff completed the pre-surveys and 157 completed the post- surveys. The study team distributed a packet containing the invitation to participate/study information letter, a demographic information sheet, and two surveys for the staff to complete if they wished to participate.
Nurses and staff completed two surveys as a baseline. The two surveys were the Professional Quality of Life Scale [36] and the Connor-Davidson Resilience Scale (CD-RISC) [37]. Participation in the study took approximately 50 minutes total. The Professional Quality of Life Scale took approximately 15 minutes to complete. The Connor-Davidson Resilience Scale took approximately 10 minutes to complete.
After the pre-surveys were completed, staff were then asked to develop an activity plan they felt that would best improve their levels of compassion and resilience. Operations Managers from the units were present but weren’t the leaders responsible for the activity plan development. However, they could participate in the activities if they so wished. Once the activity plans were completed, the nurses and staff then had two months to operationalize their respective activity plans.
At the end of the two-month period, the nurses and staff were then asked to complete the two surveys a second time. The study began in November of 2016 and concluded in March of 2017.
Description of the surveys
The Professional Quality of Life Scale – version 5 (ProQOL 5 Self-Score measure) (ProQOL.org 2015) [36] is available for free use online – no permission needed unless a change is made on the instrument. The ProQOL, V5 measures both Compassion Fatigue (CF) and Compassion Satisfaction (CS). The ProQOL, V5 is a 30-item instrument assessing how often respondents experienced a particular situation in the workplace in the past 30 days. Each subscale includes 10 items that use a 5-point Likert type scale (1=never, 5=very often). Construct validity has been established. The Cronbach alpha reliabilities are: CS: .88; burnout: .75; and CF: .81. The items in each subscale are summed for a mean score. Higher scores on the CS indicate greater satisfaction in your ability to do your job. Higher scores on the burnout subscale indicate greater likelihood for burnout. Higher scores on the STS may indicate feeling overwhelmed with thoughts of the patients you have helped [36].
For the Connor-Davidson Resilience Scale (CD-RISC) [37], a contract was signed for permission to use the scale. This 25-item scale is used to measure hardiness, faith, support/purpose, and persistence factors by using a 5-point Likert scale. Total scores range from 0 to 100, with higher scores indicating greater resilience. The instrument has demonstrated reliability (Cronbach Alpha, 0.64-0.76) and convergent validity (stress r=0.32; social support r=0.36). The mean (SD) normative resilience score is 80.4 (12.8); scores greater than 92 are considered evidence of resilience [37].
Activity plans
Some of the unit ideas that nurses and staff identified as activities included:
Sign-ups for fun activities off the unit such as ice skating, tobogganing at a nearby mountain lake, participation in a mystery room and painting events to name just a few.
On unit activities included Volunteer Office coordinated visits from therapy dogs on the unit, Reiki performed by Spiritual Care staff, work-life balance discussions, debriefing sessions following particularly stressful situations, journal club on self-care, perspective channeling, posting YouTube links for stress reduction/meditation. Other activities included, celebrations on the unit, discussing how to minimize negativity, stressing the benefits of positive outlook on self and making resilience an agenda item for unit meetings.
Some of the ideas that individuals identified as activities on their plans included:
Meditation
Relaxation exercises
Counting blessing on way to work
15-20-minute walk after work
Doing something for someone without them knowing (secret pal)
Being a positive role model
Exercise
Healthy eating
Daily positive readings
Volunteer for something you are passionate about
Telling a co-worker one positive each day
Results and findings
One hundred sixty-eight nurses and support staff completed the survey in the pre-intervention period and 157 in the post intervention period. The Compassion Satisfaction score was the sum of responses to questions 3, 6, 12, 16, 18, 20, 22, 24, 27, and 30. Higher scores indicated higher satisfaction; The Burnout score was the sum of responses to questions 1, 4, 8, 10, 15, 17, 19, 21, 26, and 29, with higher scores indicating more burnout; and The Secondary Traumatic Stress score was the sum of responses to questions 2, 5, 7, 9, 11, 13, 14, 23, 25, and 28. Higher scores indicated more stress and higher resilience. Mantel-Haenszel chi-square and exact Mantel-Haenszel chi-square tests were used to test for a linear association between the period and the ordinal survey responses.
The Professional Quality of Life Scale scores were slightly higher among the post-intervention respondents. The mean Compassion Satisfaction score was higher in the post intervention period (39.6 vs. 38.0, p=0.0084), the mean Burnout score was lower in the post intervention period (22.1 vs. 23.9, p=0.0012), and the mean Secondary Traumatic Stress score was lower in the post evaluation period (19.6 vs. 22.5, p<0.0001). The mean CDRISC scores were also better among the post-intervention respondents (74.2 vs. 70.6, p=0.0088). See Table and Bar Graph for full results (Table 1 and Figure 2).
Table 1. PROQOL and CDRISC survey score comparison
|
Survey scores
|
Pre
(n = 168)
|
Post
(n = 157)
|
P-Value
|
|
PROQOL- Compassion Satisfaction, mean (S.D.)
n = 1 missing pre-survey
|
38.0 (5.3)
|
39.6 (5.4)
|
0.0084
2021 Copyright OAT. All rights reserv
|
|
PROQOL- Burnout, mean (S.D.)
n = 1 missing pre-survey
|
23.9 (5.2)
|
22.1 (4.7)
|
0.0012
|
|
PROQOL- Secondary Traumatic Stress, mean (S.D.)
n = 1 missing pre-survey
|
22.5 (5.1)
|
19.6 (5.1)
|
< 0.0001
|
|
CDRISC Score, mean (S.D.)
|
70.6 (12.8)
|
74.2 (11.8)
|
0.0088
|
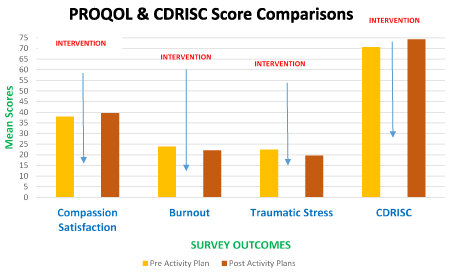
Figure 2. PROQOL and CDRISC score comparisons
The results indicate that RNs and support staff who participated in the study by completing activity plans improved their level of compassion and resilience and lowered their stress level. Satisfaction and resilience can improve, and burnout and trauma can decrease when nurses work on creating the change. The change must come from within and nurses must identify the actions that work for them as individuals. The next important aspect is that the activity plans must be seriously created and worked on daily. Degree of commitment and readiness to change is important for such a project to be effective.
Implications for nurses in practice, leadership and education
Nurses may develop compassion fatigue as a culmination of many factors they experience each day during their nursing career. The concept of compassion fatigue is not a new phenomenon for the nursing profession. Older terminology such as burnout has been used for many decades to describe the feelings of ongoing fatigue and disengagement that nurses sometimes experience.
To avoid compassion fatigue, the individual must develop strategies to prevent the development or progression of compassion fatigue and learn to maintain resilience. Based on the results of this study, incorporating various self-directed activities can help to decrease compassion fatigue levels experienced by individuals.
Education about the possibility to develop compassion fatigue, signs and symptoms and activities to reduce stress and fatigue should be incorporated into nursing education [38,39]. Additionally, inclusion of this education at the time of orientation would increase awareness and help to decrease incidence. Creative and individualized or group activities suggestions can be provided. Education to develop resiliency and methods of self-care can improve a professional’s competence in coping with compassion fatigue [40].
The role of leadership in the lessening of compassion fatigue is crucial. Many nurse leaders also develop fatigue and similar symptoms from the rigorous schedules they maintain. They need to lead by example and encourage their teams to participate in activities of their choice to promote resilience. Open discussion and recognition of compassion fatigue and its impact on nurses across the continuum of their career is essential. Research by Wei and Taormina [41] provides strong evidence that organizational socialization facilitates resilience, that resilience engenders career success and that knowing this permits a more complete understanding of personal resilience, which could benefit nurses, help nurse administrators with their work and help in treating patients. Thompson [42] discusses the incorporation of Schwartz Rounds by hospitals to combat CF. Schwartz Rounds provide an open, supportive environment for discussion. Through better support of colleagues, improved communication and the sharing of experience, staff can be reminded of their value and why they entered a caring profession. Time needs to be allocated for this initiative to work, and it needs to be integrated into staff professional development as opposed to being a forum that can be attended only if staff have time.
Healthcare facilities should consider implementing processes and activities that assist nurses in developing resources to promote resilience to maintain their health. Facilities should also consider providing resources that will reduce employee stress levels and facilitate a better work-life balance. The balance between satisfaction and fatigue is considered professional quality of life [43]. Research has demonstrated the long-term benefits that nurses can gain from compassion fatigue intervention programs. Developing resiliency in nurses can improve decision-making, clarity of communication and nurse satisfaction [44].
Further research is needed to evaluate changes in level of compassion and resilience in different practice settings and the degree to which compassion and resilience affects personal and professional well-being. Further exploring the balance between a quality professional life and the stressors that put nurses at risk for compassion fatigue is also important. Identifying which elements have more effect and which can be changed or modified may help prevent fatigue from developing.
References
- Fetter K (2012) We grieve too: One inpatient oncology unit’s interventions for recognizing and combating compassion fatigue. Clinical Journal of Oncology Nursing 16: 559-561
- Mason V, Leslie G, Clark K, Lyons P, Walke E, et al. (2014) Compassion fatigue, moral distress, and work engagement in surgical intensive care unit Trauma. Nurses Dimensions of Critical Care Nursing 33: 215-225.
- Gilmore C (2012) Compassion fatigue--what it is and how to avoid it. Nurs N Z 18: 32. [Crossref]
- Kelly L, Runge J, Spencer C (2015) Predictors of Compassion Fatigue and Compassion Satisfaction in Acute Care Nurses. J Nurs Scholarsh 47: 522-528. [Crossref]
- Neville K, Cole D (2013). The relationship among health promotion behaviors, compassion fatigue, burnout, and compassion satisfaction in nurses practicing in a community medical center. Journal of Nursing Administration 43: 348-354.
- Sorenson C, Bolick B, Wright K, Hamilton R (2016). Understanding compassion fatigue in healthcare providers: A review of current literature. Journal of Nursing Scholarship 48: 456-465.
- Sheppard K (2015) Compassion fatigue among registered nurses: Connecting theory and research. Applied Nursing Research 28: 57-59.
- Ledoux K (2015) Understanding compassion fatigue: understanding compassion. J Adv Nurs 71: 2041-2050. [Crossref]
- Hunsaker S, Chen H, Maughan D, Heaston S (2015). Factors that influence the development of compassion fatigue, burnout, and compassion satisfaction in emergency department nurses. Journal of Nursing Scholarship 47: 186-193.
- Harris C, Griffin MT (2015) Nursing on empty: compassion fatigue signs, symptoms, and system interventions. J Christ Nurs 32: 80-87. [Crossref]
- Romano J, Trotta R, Rich VL (2013) Combating compassion fatigue: an exemplar of an approach to nursing renewal. Nurs Adm Q 37: 333-336. [Crossref]
- Aycock N, Boyle D (2009) Interventions to manage compassion fatigue in oncology nursing. Clin J Oncol Nurs 13: 183-191. [Crossref]
- Gentry J (2002) Compassion fatigue: A crucible of transformation. Journal of Trauma Practice 1(34): 37-61.
- Najjar N, Davis LW, Beck-Coon K, Carney Doebbeling C (2009) Compassion fatigue: a review of the research to date and relevance to cancer-care providers. J Health Psychol 14: 267-277. [Crossref]
- Berger J, Polivka B, Smoot EA, Owens H (2015) Compassion Fatigue in Pediatric Nurses. J Pediatr Nurs 30: e11-17. [Crossref]
- Raab K (2014) Mindfulness, self-compassion, and empathy among health care professionals: a review of the literature. J Health Care Chaplain 20: 95-108. [Crossref]
- Boyle DA (2011) Countering compassion fatigue: a requisite nursing agenda. Online J Issues Nurs 16: 2. [Crossref]
- Gillespie BM, Chaboyer W, Wallis M, Grimbeek P (2007) Resilience in the operating room: developing and testing of a resilience model. J Adv Nurs 59: 427-438. [Crossref]
- Mealer M, Jones J, Newman J, McFann KK, Rothbaum B, et al. (2012) The presence of resilience is associated with a healthier psychological profile in intensive care unit (ICU) nurses: Results of a national survey. International Journal of Nursing Studies 49: 292-299.
- Mealer M, Jones J, Moss M (2012) A qualitative study of resilience and posttraumatic stress disorder in United States ICU nurses. Intensive Care Med 38: 1445-1451. [Crossref]
- Lowe L (2013) Creating a caring work environment and fostering nurse resilience. International Journal for Human Caring 17: 52-59
- Hudgins TA (2016) Resilience, job satisfaction and anticipated turnover in nurse leaders. J Nurs Manag 24: E62-69. [Crossref]
- American Nurses Association (2016) Nursing shortage: The shortage isn’t stopping soon. Position Statement. Retrieved from http://www.nursingworld.org
- Smart D, English A, James J, Wilson M, Daratha KB, et al. (2014) Compassion fatigue and satisfaction: A cross-sectional survey among US healthcare workers. Nursing & Health Sciences 16: 3-10.
- Hart PL, Brannan JD, De Chesnay M (2014) Resilience in nurses: an integrative review. J Nurs Manag 22: 720-734. [Crossref]
- Gillespie BM, Chaboyer W, Wallis M (2009) The influence of personal characteristics on the resilience of operating room nurses: A predictor study. International Journal of Nursing Studies 46: 968–976.
- Hodges HF, Keeley AC, Troyan PJ (2008) Professional resilience in Baccalaureate-prepared acute care nurses: First steps. Nursing Education Perspectives 29: 80–89.
- Lee KJ, Forbes ML, Lukasiewicz GJ, Williams T, Sheets A, et al. (2015) Promoting Staff Resilience in the Pediatric Intensive Care Unit. Am J Crit Care 24: 422-430. [Crossref]
- Cope V, Jones B, Hendricks J (2016) Resilience as resistance to the new managerialism: Portraits that reframe nursing through quotes from the field. Journal of Nursing Management 24: 115-122.
- Assi M, Leichman (2017) CNO roundtable: Using holistic care models to promote nurse resilience, Press Ganey, July 19, 2017 Podium Presentation.
- Rushton CH, Batcheller J, Schroeder K, Donohue P (2015) Burnout and Resilience Among Nurses Practicing in High-Intensity Settings. Am J Crit Care 24: 412-420. [Crossref]
- Gillman L, Adams J, Kovac R, Kilcullen A, House A, et al. (2015) Strategies to promote coping and resilience in oncology and palliative care nurses caring for adult patients with malignancy: A comprehensive systematic review. JBI Database of Systematic Reviews & Implementation Reports 13: 131-204
- Watson MJ (1988) New dimensions of human caring theory. Nurs Sci Q 1: 175-181. [Crossref]
- Watson J (2008) Nursing: The philosophy of the science of caring (2nd ed.). Boulder, CO: University Press of Colorado.
- Roy C (2008) The Roy Adaptation Model. New York: Pearson.
- Stamm B (2015) Professional Quality of Life Measurement Survey. http://proqol.org/Home_Page.php
- Connor KM, Davidson JR. (2003). Development of a new resilience scale: The Connor-Davidson Resilience Scale (CD-RISC). Depress Anxiety 18: 76-82.
- Houck D (2014) Helping nurses cope with grief and compassion fatigue: an educational intervention. Clin J Oncol Nurs 18: 454-458. [Crossref]
- Coetzee SK, Klopper HC (2010) Compassion fatigue within nursing practice: a concept analysis. Nurs Health Sci 12: 235-243. [Crossref]
- Sanso N, Galiana L, Oliver A, Pascual A, Sinclair S, et al. (2015). Palliative care professionals’ inner life: Exploring the relationships among awareness, self-care, and compassion satisfaction and fatigue, burnout, and coping with death. Journal of Pain and Symptom Management 50: 200-207.
- WeiWei B, Taormina R (201 A new multidimensional measure of personal resilience and its use: Chinese nurse resilience, organizational socialization and career success. Nursing Inquiry 21: 346–357.
- Thompson A (2013) How Schwartz rounds can be used to combat compassion fatigue. Nursing Management 20: 16-20.
- Sacco TL, Ciurzynski SM, Harvey ME, Ingersoll GL (2015) Compassion Satisfaction and Compassion Fatigue Among Critical Care Nurses. Crit Care Nurse 35: 32-43. [Crossref]
- Potter P, Deshields T, Berger JA, Clarke M, Olsen S, et al. (2013) Evaluation of a compassion fatigue resiliency program for oncology nurses. Oncol Nurs Forum 40: 180-187. [Crossref]


