Abstract
Q fever is a worldwide zoonosis caused by Coxiella burnetii. Looking to the duration of the disease, Q fever may be divided into acute and chronic forms. In humans, acute C. burnetii is often asymptomatic or mistaken for an influenza-like illness or atypical pneumonia. On the other hand, chronic Q fever is characterized by a spontaneous evolution lasting for > 6 months and a high level of IgG antibodies titre, generally determined by the indirect fluorescence antibody (IFA). However, other clinical manifestations may be observed, including hepatic, neurologic, dermatologic, and cardiac disturbs. Teha last one includes pericarditis, which has been observed in 1% of patients affected by C. burnetii infection. However, this incidence is probably underestimated. In fact, over 80% of acute as well as recurrent pericarditis remains aetiologically unexplained.
We describe a case of a 36-year-old man reporting progressive onset of dyspnea, chest pain and dysthermia sensation. Ambulatory treatment was unsatisfactory developing a severe respiratory failure recquiring his admission in the Critical Care Department. Blood test showed discrete leukocytosis with left deviation and increased reactive protein C levels. Thoracic computed tomography (CT) showed a 22mm pericardial effusion with a bilateral pleural effusion more marked in the left lung area. Microbiological as well as serological studies showed positive IgM titers to C. Burnetii. Doxycycline treatment was initiated with postive results.
Introduction
Q fever is a worldwide zoonosis caused by Coxiella Burnetii. Humans, ruminants (cattle, sheep, goats), and pets are the most frequently host observed, but in rare cases this microorganism may be observed in reptiles, birds, and ticks. Humans infections are generally produced due to the inhalation of infected aerosols, usually associated with direct or indirect contact with infected animals, or by ingestion of unpasteurized milk from infected farm animals [1,2].
Q fever is commonly divided into acute and chronic forms. In humans, acute C. burnetii is often asymptomatic or mistaken for an influenza-like illness or atypical pneumonia. On the other hand, chronic Q fever is characterized by a spontaneous evolution lasting for > 6 months and a high level of IgG antibodies titre, generally determined by the indirect fluorescence antibody (IFA) [3].
Both Q fever diseases (acute as well as chronic C. burnetti infecion) may produce important organs disturbs, including pericarditis [4]. Acute and recurrent pericarditis remains aetiologically unexplained in over 80% of cases [5]. Infectious pathogens are detected in about 20% of patient affected by pericarditis, being more frequently observed viruses like Echo-virus and Coxsackie virus. Coxiella Burnetii is the most common frequently bacteria involved in pericarditis disease (5-7%) [6,7].
Hereby, we present a case report of a young man affected by acute C. burnetii infection with acute respiratory infection and acute pericarditis, we summarize a short review of this pathology.
Case Report
A previously healthy 36-year-old man with no prior significant medical history was admitted in our Emergency Department reporting progressive onset of dyspnea of moderate activities, chest pain of mechanical charasterictics and dysthermia sensation without fever. Physical exploration revealed crackles in left lung base. A chest X-ray was also performed revealing a consolidative process in left lung base confirming the diagnosis of pneumonia. In view of his good general condition, the patient was discharged with levofloxacin 500mg 1/24 h during 7 days and acetaminophen if the patient observed dysthermia sensation or fever.
Two days latter, the patient was readmitted in our Emergency Department tachypneic, sweaty and in poor general condition. His vital signs were blood pressure of 120/60 mmHg, 110 bpm and oxygen saturation of 90% with 40% FiO2 setting via Venturi-mask. Physical exploration revealed bilateral crackles in both basis as well as rhythmic and muted heart tones. Any disturbs were observed at abdominal or extremities exploration.
During his admission, an electrocardiogram was performed showing low voltages with rectification of the PR segment in the lateral and inferior walls (Figure 1). A blood test was also realized showing a discrete leukocytosis with left deviation (14.38x1000 / μL with 86.6% neutrophilia), increased reactive protein C levels (160 mg/L), and decreased prothrombin time (49%) An arterial blood gases was also performed showing pO2 of 47mmHg and basal oxygen saturation of 83.0%. A chest X-ray was also performed showing generalized bilateral lung infiltrates being more marked in the left lung area (Figure 2). A thoracic computed tomography (CT) was also realized observing a 22mm pericardial effusion with a bilateral pleural effusion more marked in the left lung area (Figure 3).
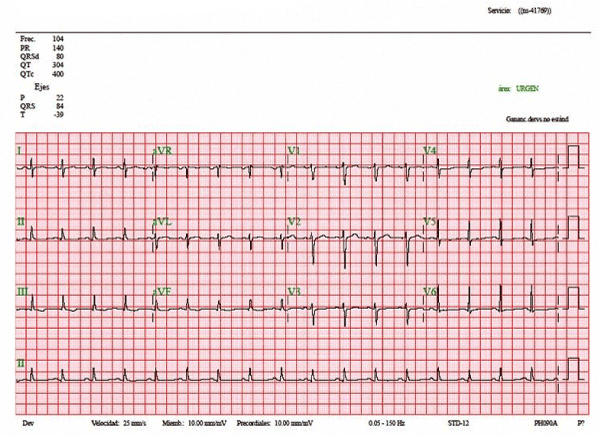
Figure 1. Electrocardiogram showing sinusalrhytm with low voltages and rectification of the PR segment in the lateral as well as inferior walls.
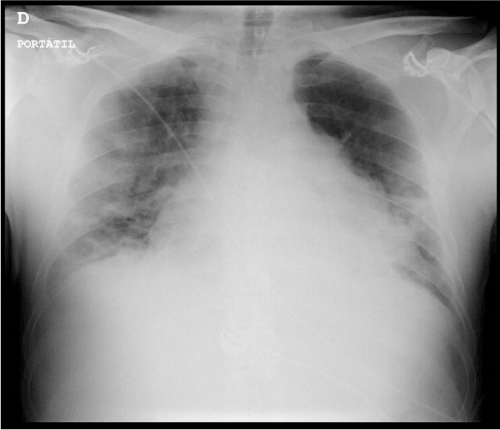
Figure 2.Chest X-ray revealing generalized bilateral lung infiltrates more marked in the left lung area.
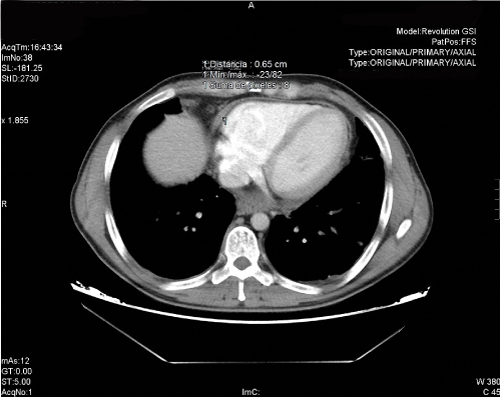
Figure 3.Thoracic computerized axial tomography (CT) showing a 22mm pericardial effusion with a bilateral pleural effusion more marked in the left lung area.
Attending to the disturbs observed, high-flow oxygen therapy, antibiotic therapy (Meropenem 1gr/8h IV), non-steroidal anti-inflammatory drugs (NSAIDs) for pain control, intravenous corticosteroids, and vitamin K (to mititgate coagulation alterations) were administered. According to the diagnosis severe respiratory failure with pleural effusion and mild pericarditis, the patient was admitted in the Critical Care Department. During his admission, a ecochardiogram was performed confirmng the pericardial effusion. In addition, microbiological as well as serological studies were performed showing positive IgM titers to C. Burnetii. The rest of the studies were negative, including HIV, Influenzae virus, Mycoplasma and Chlamydia infections. According to these results, Doxycycline treatment was initiated. After 4 days of therapy, the patient was discharged from Critical Care Department to Infectious Department to complete the treatment. After two weeks of admission in this Department, the patient was discharged due to the improve of his general condition and normalization of chest X-ray as well as ecochardiogram disturbs.
Discussion:
Q fever was first described in 1983 [8]. This term was provided because of the abbreviature of “query” and was applied at a time when the causative agent was unknown. The pathogen was discovered in 1937 [9], and was originally identified as a species of Rickettsia. Nowadays, C. burnetii is no longer regarded as closely related to Rickettsiae, but as similar to Legionella and Francisella. This specie is an obligate intracellular, small gram-negative bacterium [2].
Q fever is a worldwide zoonosis. Humans infections are generally produced due to the inhalation of infected aerosols, usually associated with direct or indirect contact with infected animals, or by ingestion of unpasteurized milk from infected farm animals [1,2]. This disease is more frequently reported in spring and early summer. In addition, it may occurs at all ages and is more frequently observed in men. This infection is usually benign, but mortality rates in patients affected by chronic Q fever are 1-11% [10].
Looking to the duration of the disease, Q fever may be divided into acute and chronic forms. In humans, acute C. burnetii is often asymptomatic or mistaken for an influenza-like illness or atypical pneumonia. In Spain, 21% of episodes of fever lasting for more than 1 week and less than 3 weeks has been observed to be produced by C. burnetii. On the other hand, chronic Q fever is characterized by a spontaneous evolution lasting for > 6 months and a high level of IgG antibodies titre, generally determined by IFA [2,3].
However, other clinical manifestations may be observed, including hepatic, neurologic, dermatologic, and cardiac disturbs [11]. In case series, pericarditis has been observed in 1% of patients affected by C. burnetii infection. However, this incidence is probably underestimated. In fact, over 80% of acute as well as recurrent pericarditis remains aetiologically unexplained [1].
Diagnosis is based in serologic studies. Techniques used include IFA (method of choice), complement fixation (less sensitive and specific), and enzyme-linked immunosorbent assay (ELISA) (comparable to IIF). In pericarditis caused by C. burnetii, when pericardial fluids are available (which is a rare event), it would be probably be interesting to systematically test them by cultura and PCR analysis. However, these tests are not frequently realized [12]. Due to that, some kits has been developed to promote this diagnosis [13].
2021 Copyright OAT. All rights reserv
Attending to the treatment, when it is necessary, acute forms of Q fever are treated with doxycycline for 3 weeks. On the other hand, chronic forms are treated with a combination of doxycycline and hydroxychloroquine for at least 1 year [14]. In pregnants, co-trimoxazole has been shown to significantly decrease the risk of adverse consequences for the fetus compared to doxycycline [15].
In conclusion, C. burnetii pericarditis is rare but its incidence is probably underestimated. It accounted for 1% of our cases of acute Q fever. Given the potential severity of the cardiac complications of Q-fever (pericaditis, endocarditis…), we recommend to develop cultures as well serologies of C. burnetii in patients affected of pericarditis, specially in patients with an unsatisfactory evolution. In addition, if drainage es developed, pericardial fluid must be tested.
Conflict of interest
No conflict of interest shown in the realization of this writing.
Funding
No external funding sources and any comments are received.
Finally all the authors assert agree with their work and actively collaborating in its development.
References
- Levy PY, Carrieri P, Raoult D (1999) Coxiella burnetii pericarditis: report of 15 cases and review. Clin Infect Dis 29: 393-397. [Crossref]
- Honarmand H (2012) Q Fever: an old but still a poorly understood disease. Interdiscip Perspect Infect Dis 2012: 131932.
- Eldin C, Mélenotte C, Mediannikov O, Ghigo E, Million M, et al. (2017) From Q Fever to Coxiella burnetii Infection: a Paradigm Change. Clin Microbiol Rev 30: 115-190. [Crossref]
- Gunn TM, Raz GM, Turek JW, Farivar RS (2013) Cardiac manifestations of Q fever infection: case series and a review of the literature. J Card Surg 28: 233-237. [Crossref]
- Ivić I, Božić I, Ledina D (2016) Coxiella burnetii chronic pericarditis: a case report. Neth J Med 74: 362-364. [Crossref]
- Levy PY, Habib G, Collart F, Lepidi H, Raoult D (2006) Etiological diagnosis of pericardial effusion. Future Microbiol 1: 229-239. [Crossref]
- Fardman A, Charron P, Imazio M, Adler Y (2016) European Guidelines on Pericardial Diseases: a Focused Review of Novel Aspects. Curr Cardiol Rep 18: 46.
- Derrick EH (1983) "Q" fever, a new fever entity: clinical features, diagnosis and laboratory investigation. Rev Infect Dis 5: 790-800.
- Burnet FM, Freeman M (1983) Experimental studies on the virus of "Q" fever. Rev Infect Dis 5: 800-808. [Crossref]
- Million M, Raoult D (2015) Recent advances in the study of Q fever epidemiology, diagnosis and management. J Infect 1: S2-9.
- Morroy G, Keijmel SP, Delsing CE, Bleijenberg G, Langendam M, et al. (2016) Fatigue following Acute Q-Fever: A Systematic Literature Review. PLoS One 11: e0155884.
- Hartzell JD, Wood-Morris RN, Martinez LJ, Trotta RF (2008) Q fever: epidemiology, diagnosis, and treatment. Mayo Clin Proc 83: 574-579. [Crossref]
- Levy PY, Gouriet F, Habib G, Bonnet JL, Raoult D (2009) Diagnosis of Coxiella burnetii pericarditis by using a systematic prescription kit in cases of pericardial effusion: an 8-year experience. Clin Microbiol Infect 2: 173-175.
- Kersh GJ (2013) Antimicrobial therapies for Q fever. Expert Rev Anti Infect Ther 11: 1207-1214.
- Carcopino X, Raoult D, Bretelle F, Boubli L, Stein A (2009) Q Fever during pregnancy: a cause of por fetal and maternal outcome. Ann N Y Acad Sci 1166: 79-89.



