Lymphangioma circumscriptum (LC) is a rare benign disorder of lymphatic channels in deep dermal and subcutaneous layers. LC can occur either as a congenital abnormality or as acquired damage to previously normal lymphatic channels. LC of the vulva is very rare specially during pregnancy. A rare case of lymphangioma circumscriptum of vulva in pregnancy is reported which was managed successfully.
Lymphangiomas are rare lymphatic abnormality which rarely involves vulva. Lymphangioma circumscriptum commonly occurs in extremities,trunk and rarely on genital skin and is common in infancy but acquired lymphangioma can occur at any age. We report a rare case of lymphangioma circumscriptum of vulva in pregnancy to emphasize the importance of recognising this condition in pregnancy and differentiating it from other vulvar dermatoses which can present similarly but may require different approach to management.
A 24 year old female patient at 28 weeks of pregnancy presented to obstetrics OPD of our institute with complaints of lesions over vulva along with drainage of clear fluid from lesions. Patient was G3P2A0L1 with history of a female baby of 3 years of age and a male baby delivered one and half year back by emergency caesarean section due to fetal distress and baby expired 3 days after birth. She gives h/o these lesions since her second pregnancy when lesions were few in number and started erupting over right thigh and slowly involved whole vulva and groins. On examination during present pregnancy there were multiple verrucous, coalescent papules on vulva (Figures 1 and 2). Oozing and drainage of clear fluid was seen from lesions and patient complaint of itching over lesions. The remaining physical examination was normal. On per abdominal examination fundal height corresponds to 28 weeks and presentation was cephalic with regular fetal heart. A transverse suprapubic scar was seen. Routine laboratory examination including complete blood count & differential WBC count were within normal limit and ESR was 20 mm/hr. Serological tests for HIV, CMV, Herpes simplex and VDRL were negative.
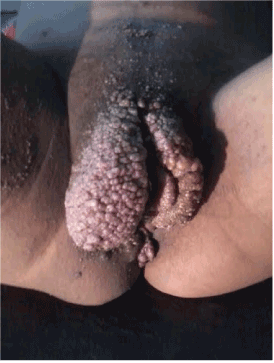
Figure 1. LC lesions involving whole vulva and thighs.

Figure 2. LC in pregnant female.
The differential diagnosis of Genital warts, Angiokeratoma of vulva, Lymphangioma circumscriptum of vulva and Fabry’s Anderson disease was made by dermatologist. Skin biopsy was taken and histopathological examination revealed parakeratosis, acanthosis and elongation of rete ridges and expansion of papillary dermis with multiple dilated lymphatics in superficial dermis and these findings showed close resemblance to lymphangioma circumscriptum and hence diagnosis was made (Figure 3).
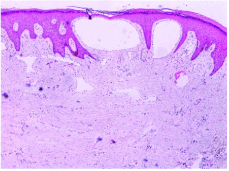
Figure 3. Histopathological View in LC of vulva.
She had no complaints except extensive distribution of the lesions. As she was pregnant only cryotherapy was tried on the patient. She underwent many sessions of cryotherapy in third trimester. At 35 weeks gestation she complaint of swelling and pain in right thigh. She was reffered for surgical consultation. Her venous Doppler study was normal. Her total leucocyte count was increased suggestive of cellulitis. She was given a course of antibiotics and was managed conservatively. At 38 weeks of gestation she suddenly complaint of loss of fetal movements and her liquor came to be significantly reduced. She was taken up for emergency caesarean section and delivered a healthy male baby of 3.0 kg. Her post operative period was uneventful and she was discharged on 7th post operative day and was advised to follow up after 6 weeks in skin clinic for further treatment of those lesions.
A lymphangioma or lymphatic malformation represents a congenital proliferation of lymphatic vessels. There are 3 types of lymphangioma: circumscriptum, cavernous and cystic [1]. LC is either primary (presents at birth or develops in early childhood) or secondary (induced by impairment of blood flow) [2]. Secondry lymphangioma is also termed acquired lymphangioma and lymphangiectasis. The most common form of cutaneous lymphangioma is lymphangioma circumscriptum which arises in infancy but may occur at any age. It is characterized by small clusters of vesicles, measuring about 2-4 mm that usually contains clear lymph fluid [3]. The typical history includes a small number of vesicles on the skin at birth or in childhood & in subsequent years, they tend to increase in numbers and the area of skin involved continues to expand. Usually lesions are asymptomatic but patients may have spontaneous episodes of minor bleeding and copious drainage of clear fluid from ruptured vesicles as in our patient.
Although it may appear localized to the dermis this neoplasm frequently extends deeply and laterally. The lesions can have a warty appearance as a result they are often confused with warts as in our patient. The sites of predilection are the proximal extremities, trunk, axilla and oral cavity. Involvement in the other areas such as scrotum is not uncommon. Primary vulvar LC is very rare and this appearance may mimic vulval tumors [4]. Secondary lymphangioma of the vulva is a complication of pelvic lymphatic obstruction which occurs in the long term. Acquired lympphangioma occurs most commonly in the vulvar region compared to the other regions of the body which can be frequently associated with surgery, radiation therapy, infection (erysipelas, tuberculosis), crohn’s disease, congenital dysplastic angiopathy and congenital lymphedema [5]. There is a pregnant case presented in the literature with lesions which clinically mimicked genital warts and actually stemmed from congenital deficiencies of the lymphatic system and occurred due to lymphatic circulation failure induced by pregnancy [6]. The same is seen in our case but here lesions are even more extensive. At first glimpse our patient was considered to have vulval warts, however detailed history taking, dermatologic and histopathological examinations confirmed vulvar lymphangioma circumscriptum.
The traditional treatment of LC is surgical removal (vulvectomy) not done in pregnant female and is usually not successful due to rapid relapses and should be considered after treatment failures [7]. Vaporization with CO2 laser is the recent recommendation for LC of vulva and is suggested to yield acceptable cosmetic results [8]. In our patient due to extensive distribution and pregnancy cryotherapy sessions were given and after pregnancy laser was advised.
Detailed dermatological and histopathological examination should be performed on patients presenting with vulvar papular lesions. Deep lymphatic ducts should be eradicated in order to avoid recurrences. LC must certainly be considered in the differential diagnosis of verrucous lesions of the anogenital lesions.
- Brown JV Stenchever MA (1989) Cavernous lymphangioma of the vulva. Obstet Gynecol 73: 877-879. [Crossref]
- Patel GA, Siperstein RD, Ragi G, Schwartz RA (2009) Zosteriform lymphangioma circumscriptum. Acta Dermatovenerol Alp Pannonica Adriat 18: 179-182. [Crossref]
- Whimster IW (1976) The pathology of lymphangioma circumscriptum. Br J Dermatol 94: 473-486. [Crossref]
- Mu XC,
Tran TA, Dupree M, Carlson JA (1999) Acquired vulvar lymphangioma mimicking genital warts. A case report and review of the literature J Cutan Pathol 2: 150-154. [Crossref]
- Ghaemmaghami F, Zarchi MK (2007) Giant lymphangioma circumscriptum mimicking vulvar tumor; A case report and literature review. J Low Genit Tract Dis 11: 281-283. [Crossref]
2021 Copyright OAT. All rights reserv
- Al-aboud K, Al-Hawsawi K, Ramesh V, Al-Aboud D, Al-Githami A (2003) Vulval lymphangioma mimicking genital warts. J Eur Acad Dermatol Venereol 17: 684-685. [Crossref]
- Elizeri YD, Saklar JA (1988) Lymphangioma circumscriptum; review and evaluation of W2 laser vaporization. J Dermatol Surg Oncol 14: 357-364. [Crossref]
- Haas AF, Narurkar VA (1998) Recalcitrant LC ultrapulse CO2 laser. Dermatologic surgery 24: 893-895.



