Background and objective:
This study was conducted to evaluate the clinical efficacy of laser hair removal using a novel 650-microsecond pulsed Nd:YAG 1064 nm laser.
Materials and Methods:
Materials and Methods: Patients seeking laser hair removal with no prior laser hair removal treatment in the past one year were recruited from a dermatology clinic. A total of 298 adult subjects with skin types II-IV, received an average of 6 treatments at four-week intervals in various body locations including the facial, axillary, back, neck, arms, legs and bikini areas. At each four-week follow up and at six months post final treatment, an analysis of the clinical improvement as defined by percent hair reduction was performed. In addition, patient surveys were obtained to determine their level of satisfaction with treatment and to monitor the incidence of adverse events.
Results:
At least a 50% reduction in hair follicles was observed in all subjects in an average of six treatments at four-week intervals. Of the 298 subjects treated, 85% were satisfied with the extent of hair removal, 5% were neutral and 10% were not satisfied. There were no permanent adverse events observed. One patient had transient hypopigmentation that did not result in cessation of treatment and resolved in eight weeks.
Conclusion:
The novel 650-microsecond pulsed Nd:YAG 1064 nm laser is effective for laser hair removal and can generate high levels of patient satisfaction. Adverse events reported were limited to mild transient edema, erythema and one case of hypopigmentation, which resolved.
epilation; hair removal; laser, Nd:YAG; selective photothermolysis; short pulse
Unwanted hair causes significant stress in patients resulting inanxiety, depression and overall reduced quality of life [1]. Since their development in the 1960s, laser hair removal systems have continued to grow in popularity, as they are now one of the most common cosmetic procedures performed by dermatologists [2]. Unlike other hair removal techniques such as waxing, shaving, and electrolysis, laser hair removal is an efficient way to permanently reduce hair growth and has thus become the gold standard [3]. Laser, which stands for “light amplification stimulated emission of radiation” is a type of selective photothermolysis that targets light absorbing molecules or chromophores at a specific wavelength [4]. Melanin found in hair follicles is the chromophore that absorbs the energy emitted by laser and transforms it into heat that selectively damages hair follicles [5]. Today, there are a variety of laser hair removal systems used to target a variety of hair colors and skin types. Lasers utilizing shorter wavelengths such as the Ruby laser (694 nm) and Alexandrite laser (755 nm) have more superficial penetration into the epidermis and therefore have increased risk for epidermal melanin absorption and injury to the surrounding skin [6]. Subsequently, these lasers are typically avoided in patients with darker skin types (Fitzpatrick phototypes III-VI). Lasers with longer wavelengths, such as the Nd:YAG 1064 nm laser, provide deeper epidermal penetration to target follicular melanin with less absorption of surrounding skin. These lasers have been shown to be safe and effective for removal of hair in darker skin types [7].
In addition to selecting lasers with the appropriate wavelengths, determining the pulse duration and fluence (energy per square area) to optimize results and minimize side effects is also of utmost importance. High fluence and long pulse duration allows heat to diffuse to surrounding tissue and increases the risk for side effects such as scarring [8]. Pulse durations, in order to be effective should be shorter than or equal to the thermal relaxation time (TRT) of the hair shaft, which is estimated to be between 10 and 50 milliseconds [9]. As a result, most currently available laser hair removal systems use millisecond pulse widths.
Similarly, the majority of the studies that exist on Nd:YAG lasers exist on traditional long pulsed Nd:YAG lasers that deliver pulse widths of 3 to 30 milliseconds of fluence. These long pulsed Nd:YAG lasers are typically used with cooling systems to further reduce the incidence of epidermal damage. However, a 650 microsecond (µs) technique Nd:YAG laser has recently been found to have comparable results to longer pulse duration Nd:YAG lasers without skin cooling measures [10]. This study was conducted to evaluate the safety and patient satisfaction with laser hair removal using a novel portable and relatively inexpensive Nd:YAG laser with a short pulse of 650 µs.
Study design and patients
Patients were recruited from a dermatology clinic in New York City, New York. The procedure as well as the potential risks, were discussed and consent forms were signed with each patient. Study participants were treated with the 650 µs Nd:YAG 1064 nm laser at fluencies between 4-8 J/cm2, depending on skin type. Patients with Fitzpatrick skin types II-VI were included in this study. Patients with lighter skin types (II- III) were treated at a higher fluence of 6-8 J/cm2, whereas patients with darker skin types (IV-V) were treated at a lower fluence of 4-6 J/cm2.The inclusion criteria were aged 18 and older seeking hair removal from any of the following sites including bikini region, face, axilla, back, neck, arms and legs. Reasons for being excluded from this study were pregnancy, previous history of hypertrophic or keloidal scaring, prior laser hair removal treatment in the past 1 year and systemic immunosupression. Pulse duration of 650 µs was used in all patients.
Laser treatment
No intralesional or topical anesthetic was used prior to administering laser treatment. All treatments were performed by or under the direct supervision of a board certified dermatologist. Non-overlapping pulses of the 650 µs Nd:YAG laser were delivered to patients at fluencies between 4 to 8 J/cm2. The laser energy was delivered with an 8 mm beam diameter scanner. One or two passes of the laser treatment were delivered at each session and no epidermal air cooling technique was utilized before, during or post treatment. Follow-up treatments were scheduled for each patient at four-week intervals for an average of six treatments.
Efficacy assessments
Each patient was evaluated for improvement both before and immediately following each treatment session and six months following their final treatment. Clinical photographs were taken at each visit and were standardized such that the same camera, lighting, and exposure conditions were used each visit. Evaluation of efficacy was determined by both physician assessment and patient satisfaction surveys.
Physician assessment included both the overall clinical improvement and photographic comparison of the previous visit to determine the percent reduction in the number of hairs. Hair reduction was measured as a percentage of the number of hairs present at each follow up compared with the number of hairs at the previous visit. Investigators graded the photographsusing the following quartilehair reduction grading system: 1indicating less than 25%; 2: 25 to 50%; 3: 51 to 75%; 4: 76% to 100%. Unsatisfactory results were defined as quartile grading score of either 1or 2 (meaning <25% or 25-50% reduction in the number of hairs respectively). Grading results of either a 3 or 4 indicating a 50-75% or 75-100% reduction hair were considered satisfactory.
Patients scored subjective satisfaction at each visit by choosing satisfied, unsatisfied, or neutral on self-evaluation surveys. Subjects were also instructed to report any adverse cutaneous reactions including scarring, persistent erythema and pigment changesin the surrounding skin at each visit.
Hair reduction
At six months following the last treatment, all patients were found to have satisfactory hair reduction in treated areas. Satisfactory was again defined as a grade of either 3 or 4 signifying at least a 50% reduction in the number of hair follicles when compared to baseline photographs. No patients had unsatisfactory results with less than 50 percent reduction in hair. On average, six treatment sessions were performed to achieve satisfactory reduction in hair. However, some patients with thicker hair and darker skin required more than the average of six treatments to have satisfactory results.
Patient satisfaction
After an average of six treatments, 85% of subjects were satisfied with the extent of hair removal, 10% were unsatisfied and 5% were neutral (Figure 1).
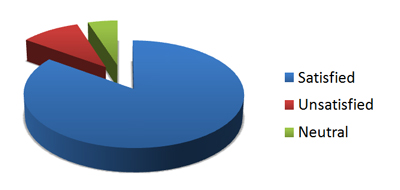
Figure 1. Percentage of individuals satisfied with the procedure. (n=298)
Adverse effects
The majority of patients did not report any serious adverse reactions to treatment including but not limited to scarring, vesiculation, crusting, persistent pigmentary changes or persistent erythema. There was one case of post inflammatory hypopigmentation in one subject who was type V skin and was treated at a fluence of 6 J/cm2 for folliculitis barbae (Figure 2). This hypopigmentation completely resolved in eight weeks however.All subjects tolerated the laser treatments with only mild transient pain and erythema noted, as well as mild transient hypopigmentation.All patients described the pain as “tolerable” and no patients voluntarily or involuntarily withdrew from our study or subsequent treatments due to adverse events.
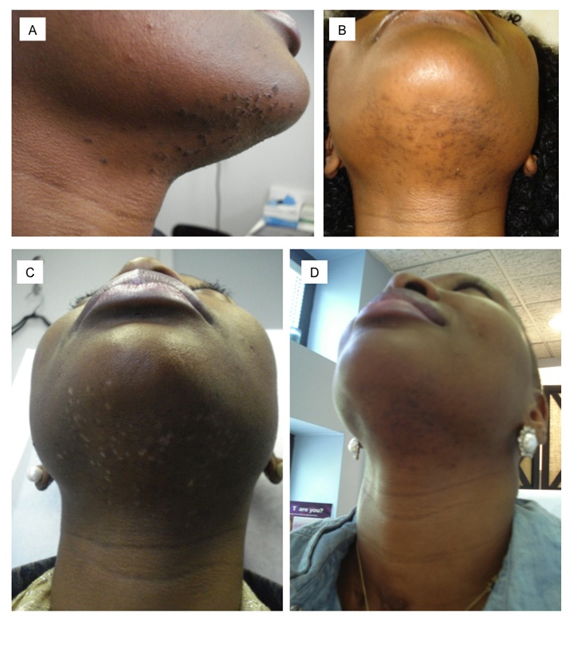
Figure 2. Patient with Fitzpatrick skin type V displaying folliculitis barbae (A and B) before treatment. Post treatment (C) with the 650 µsec Nd: YAG laser, patient had hypopigmented macules in treatment areas. In 8 weeks, patient had resolution of hypopigmentation (D) without any residual depigmentation.
There are many laser systems approved for laser hair removal each with their own advantages and disadvantages. Although there has been much advancement in thesetechnologies since becoming widely accepted almost 20 years ago, many gaps still exist in terms of optimizing treatment response. Specifically, no one system has been able to produce predictable, consistent results as treatment responses vary significantly based on skin type, ethnicity, hair color and treatment time interval [11]. Perception of laser hair removal systems depends largely on their acceptability by both patients and physicians in terms of its efficacy, safety and risk for complications. The Nd:YAG laser is known for it’s high safety profile, especially in darker skin patients with lower rates of dyspigmentation compared to shorter wavelength lasers such as the red light ruby and alexandrite systems [12].
The Nd:YAG 1064 has traditionally been studied using long pulse durations between 3 to 30 milliseconds. Recently, the increasing public demand for a low-cost hair removal service has urged new manufacturers to develop low-priced, compact sized systems such as the novel 650 microsecond pulsed Nd:YAG 1064 nm laser which are still in need clinical validation and long-term follow-up.When using the 650- microsecond pulse duration, the melanin in the epidermis is exposed to the same laser fluence as it passes through to the deeper dermis layers however;the time of this exposure is 5 to 50 times shorter [13]. As a result, epidermal melanin is exposed to and absorbs a lesser amount of energy.This causes less heat generation within the epidermis and allows treatment with no skin cooling and with minimal discomfort [13].
Our study proved that this novel 650 microsecond pulsed Nd:YAG 1064 nm laser is highly effective for laser hair removal treatment on various body locations including bikini region, face, axilla and extremities. High levels of patient satisfaction can be achieved using the device. When compared to traditional longer pulse durations and non portable Nd:YAG lasers, the short 650 microsecond pulsed Nd:YAG had similar hair reduction results. For instance, a recent study found that the traditional long pulsed Nd:YAG resulted in 54.20% reduction in axilla hair at 6 month follow up after receiving 5 monthly treatments [14]. Another study by Rao and Sankar, found similar results with the average percentage of hair reduction after long pulsed Nd:YAG laser being 54.3% [7]. As a result of these studies on long pulsed Nd:YAG, our study defined satisfactory results in hair reduction as greater than or equal to 50% of hair reduction (or a quartile grading score of atleast 3) as standard of acceptable treatment result when compared to traditional Nd:YAG systems. All patients treated in our study obtained this satisfactory reduction in hair follicles in an average of 6 treatment sessions. Comparably, the first clinical trial on the long-pulsed Nd:YAG for laser hair removal reported complete epilation in 4 to 6 sessions in 208 patients [15].
These results are also consistent with prior preliminary studies on the novel short pulsed 650-microsecond Nd:YAG laser that first demonstrated it’s safety and efficacy using objective histological evaluation. In these studies, treatment of the axilla in six females using the 650 microsecond Nd-YAG laser displayed a 76% reduction in average hair count 4 months after treatment using high fluence and 72% reduction in hair count using low fluence [10].
The adverse advents observed in this study were similar to studies on long pulsed Nd:YAG lasers. Mild erythema and pain were reported at treatment sites but were transient in all cases. In fact, perifollicular edema and erythema lasting a few hours is not believed to be a side effect of laser treatment but rather a necessary consequence of effective photothermolysis [16]. None-the-less, one patient with type V in our study experienced an unwanted side effect of hypopigmentation. This resolved in 8 weeks without any subsequent treatment. Similarly in a previous study of 224 patients treated with long pulsed Nd:YAG, one patient experienced hypopigmentation post treatment. This same study on the long pulsed Nd:YAG displayed a 2.1% incidence of hyperpigmentation in subjects with skin types IV to VI subjects [6]. However, when compared to other lasers such as the ruby and alexandrite, the Nd:YA Glaser is still known to have the lowest rates of pigmentary alterations [12,16]. Our particular study of the 650 microsecond Nd:YAG did not result in any cases of post treatment hyperpigmentation.
In summary, the 650 microsecond Nd:YAG laser is an alternative to the traditional long pulsed variant. While its size and ease of use make it an attractive choice for laser hair removal, its use may be limited when treating larger body surface areas such as the back or chest.
- 1) Watson RE, Bouknight R, Alguire PC (1995) Hirsutism: evaluation and management. J Gen Intern Med 10: 283–292.
- 2) Blume-Peytavi U, Hahn S (2008) Medical treatment of hirsutism. Dermatol Ther 21: 329-339.
- 3) Goldberg DJ, Silapunt S (2001) Hair Removal Using a Long-Pulsed Nd:YAG Laser: Comparison at Fluences of 50, 80, and 100 J/cm2. Dermatol Surg 27: 434-436. [Crossref]
- 4) Fernandez AA, Franca K, Chacon AH (2013) From flint razors to lasers: a timeline of hair removal methods. J Cosmet Dermatol 12: 153-162. [Crossref]
2021 Copyright OAT. All rights reserv
- 5) Ibrahimi OA1, Avram MM, Hanke CW, Kilmer SL, Anderson RR (2011) Laser hair removal. Dermatol Ther 1: 94-107. [Crossref]
- 6) Rao J, Goldman MP (2005) Prospective, Comparative Evaluation of Three Laser Systems Used Individually and in Combination for Axillary Hair Removal. Dermatol Surg 31: 1671-1677. [Crossref]
- 7) Rao K, Sankar TK (2011) Long-pulsed Nd: YAG laser-assisted hair removal in Fitzpatrick skin types IV-VI. Lasers Med Sci 26: 623- 626. [Crossref]
- 8) Anderson RR, Parrish JA (1983) Selective photothermolysis: Precise microsurgery by selective absorption of pulsed radiation. Science 220: 524–527. [Crossref]
- 9) Tanzi EL, Lupton JR, Alster TS (2003) Lasers in dermatology: Four decades of progress. J Am Acad Dermatol 49: 1–31. [Crossref]
- 10) Khatri KA, Lee RA, Goldberg LJ, Khatri B, Garcia V (2009) Efficacy and safety of a 0.65 millisecond pulsed portable ND: YAG laser for hair removal. J Cosmet Laser Ther1 1: 19-24. [Crossref]
- 11) Alster TS, Bryan H, Williams CM (2001) Long-pulsed Nd: YAG laser-assisted hair removal in pigmented skin: a clinical and histological evaluation. Arch Dermatol 137: 885-889. [Crossref]
- 12) Nanni CA, Alster TS (1999) Laser-assisted hair removal: Side effects of Q-switched Nd: YAG, long pulsed ruby, and alexandrite laser. J Am Acad Dermatol 41: 165-170. [Crossref]
- 13) http://aerolase.com/micropulse-1064-technology-overview/
- 14) Wanitphakdeedecha R, Thanomkitti K, Sethabutra P, Eimpunth S, Manuskiatti W (2012) A split axilla comparison study of axilla hair removal with low fluence high repetition rate 810 nm diode laser vs. high fluence low repetition rate 1064 nm Nd: YAG laser. J Eur Acad Dermatol Venereol 9: 1133-1136. [Crossref]
- 15) Garcia C, Alamoudi H, Nakib M, Zimmo S (2000) Alexandrite laser hair removal is safe for Fitzpatrick skin types IV-VI. Dermatol Surg 26: 130-134.
- 16) Lanigan SW (2003) Incidence of side effects after laser hair removal. J Am Acad Dermatol 49: 882-886. [Crossref]
- 17) Fontana CR, Bonini D, Bagnato VS (2013) A 12-month follow-up of hypopigmentation after laser hair removal. J Cosmet Laser Ther 15: 80-84. [Crossref]
Editorial Information
Editor-in-Chief
Torello Lotti
University of Rome "G.Marconi" Rome
Article Type
Research Article
Publication history
Received: October 06, 2014
Accepted: October 15, 2014
Published: October 19, 2014
Copyright
©2014 Giambrone D. This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Citation
Giambrone D, Ahn CS, Rao B (2014) Laser hair removal using a650 microsecond pulsed ND:YAG laser: A study of 298 patients. Glob Dermatol, 1: DOI: 10.15761/GOD.1000104


