Abstract
Introduction: Long-lasting IUD continuation is the most important requirement of intrauterine contraception.
Areas covered: This expert opinion examines the continuation rates of contraceptive methodologies and formulates recommendations to maximize continuation of use.
Expert opinion: IUDs are long-acting reversible contraceptives (LARC) which have the potential advantage to be used for the full approved duration of action. However, early discontinuation is often the case due to a variety of factors. We examine the main factors and suggest how IUD continuation of use could be enhanced. IUDs that fit uterine cavities of varied sizes are proposed in an attempt to improve continuation of use.
Introduction –The problem
In order to prevent unintented pregnancy, it is necessary that contraceptives are used correctly and consistently; however, in real life this rarely occurs. Short-acting contraceptives (oral contraceptives, the contraceptive patch and the vaginal ring) have typical pregnancy rates (effectiveness during actual use) of 9% during the first year whilst the pregnancy rate during perfect use is only 0.3% [1]. Adolescents are more likely than adult women to discontinue a range of contraceptive methods, including pills and injectables, and are extremely vulnerable to unintended pregnancy. IUDs are highly, if not the most effective method of contraception with typical use related failure rates of between 0.2-0.8% with hormonal IUDs only being numerically more effective than most copper IUDs. The differences between the effectiveness of hormonal devices over copper ones is of little clinical importance. Implants have an even lower typical failure rate of 0.05%. Both IUDs and implants are long-acting with duration of action from 3 years in the case of implants and 5 to 10 years for IUDs. IUDs and implants should, therefore, be considered as first-line choices for young women especially if user compliance is a problem [2]. IUDs are the most cost effective methods of contraception available, as well as one of the most convenient. However, many patients chose to discontinue their use well before their approved effective periods, excluding subjects who discontinue due to a desire to conceive. Identification of the factors that contribute to this premature discontinuation and their elimination will likely extend the continuation rates in many women.
Anatomical considerations
Da Costa et al conducted a study in 828 women and girls between 10 and 40 years old using transabdominal ultrasonography [3]. Women were divided into two groups: group 1 consisted of 477 (57.6%) adolescents, and group 2 comprised 351 (42.3%) women 20–40 years old. The overall size of the uterus as judged by uterine volume increased with the presence of menarche, age, and parity (P<0.05). Nulliparous and primiparous adolescents younger than 18 years old had a smaller uterine volume, 41.3 ± 17.9 and 51.6 ± 19.7 cm3, respectively, than nulliparous and primiparous women 20–40 years old (P<0.001). The uterus is structurally a prolate ellipsoid and since the uterine cavity is symmetrical it is likely to also be the same. Thus, based on these studies, many adolescent girls may not be appropriate candidates for most used conventional designed IUD simply because their uterine size may not adequately accommodate them.
IUDs are inserted in the uterine cavity to prevent fertilization. IUDs are foreign bodies that lie in the cavity in the case of most conventional devices while frameless systems which lack the conventional transverse arm are attached to the uterine wall using an anchoring system. Conventional T-shaped or framed devices have an overall diameter of approximately 32 mm while frameless systems are much smaller being <3 mm in width. It is evident that the geometric relationship of the uterine cavity and IUD should be optimal as a disharmony between the two will determine patient acceptance or result in discontinuation because of problematical side effects. Since the 1960s, IUD research has focused on the optimization of this relationship. Surprisingly, almost 50 years ago, researchers found that pain during use of the IUD is related to the disparity between the size of the uterine cavity and that of the IUD. Particularly, a device that was too wide for a woman’s uterine cavity was found to be cumbersome resulting in pain and discomfort. The reverse scenario of a device being too small for a uterine cavity was found to be problematic in retaining the IUD in the uterus. A transverse diameter of the uterine cavity in the fundus that is greater than the width of the IUD has a higher risk of expulsion or displacement [4]. Recent studies using 2D and 3D ultrasonography have found that uterine cavities, although overall ellipsoidal come in varied shapes and sizes in contrast to that depicted in most medical texts. Many are cylindrical (narrow ellipsoid) and have narrow transverse diameters of the uterine cavity in the fundus not wide enough to accommodate current conventional framed IUDs [5] (Table 1).
Table 1: Uterine fundus transverse diameter measured in 408 nulliparous women (Contrel Research, Data on File).
|
Mean |
Range |
% less than Mean (2D+3D) |
3D (n=152) |
21.67 |
6.0 – 40.0 |
50.61 |
2D (n=258) |
22.42 |
5.9 – 39.5 |
Note: The width of Paragard and Mirena is 32 mm.
The length of the IUD does not seem to be important clinically, unless there is a great difference between cavity length and the length of the stem of the IUD. Studies reported that if the length of IUD exceeded the uterine cavity length by 10 mm or more, expulsion rate can also be increased [6].
Evaluating the uterine cavity –Measuring the cavity width
As uterine cavities differ in size and shape, and most current copper T-shaped IUDs and the Mirena® LNG-IUS (Bayer Healthcare, Germany) have a transverse arm length of 32 mm, and the new Jaydess®/Skyla® (Bayer Healthcare, Germany) a transverse arm length of 28 mm, knowing the dimensions of the uterine cavity is essential when inserting these framed devices in order to maximize the likelihood of maximal patient comfort to ensure long-term use. The maximal fundal transverse dimension is of paramount importance with respect to IUD acceptance, as women tolerate the IUD much better when the IUD fits properly [7].
Imaging plays an important role in evaluating the uterine cavity and has led to our better understanding of IUD compatibility. Ultrasonography is simple, noninvasive, cost-effective and readily available in most gynecological offices worldwide. 2D transverse sonography in the premenstrual phase shows a distinct endometrial echo; however measuring the transverse distance in the early proliferative phase can occasionally be challenging. In these cases, the instillation of a few milliliter of gel (GIS) will, as seen in Figure 1, aid to visualize the cavity and allow measurement of the width precisely. 3D ultrasound of the uterine cavity is increasingly being used, particularly the coronal view, which allows for a more careful evaluation of the size and shape of the cavity (Figure 1) and a simultaneous assessment of IUD placement post insertion.
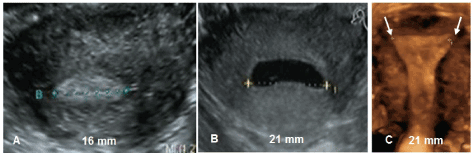
Figure 1: 2D and 3D ultrasound showing the width of the uterine cavity. A) Premenstrual evaluation of the width of the cavity; B) Measurement of the width using gel instillation sonography (GIS); C) 3D ultrasound of the uterine cavity width (courtesy Dr. S. Jandi, Berlin, Germany).
In cases where uterine and/or pelvic pathology is suspected, computed tomography (CT) or magnetic resonance imaging (MRI) may be helpful given their larger field of view; however, their utility as a first-line methodology is limited because of the associated radiation and cost.
Hysteroscopy may also be useful in certain cases to exclude associated pathology (e.g., fibroids, polyps) or to evaluate a congenital anomaly of the uterus (e.g., uterus subseptus, septus). Overall, about 5.5% uterine anomalies are diagnosed in an unselected population. Arcuate uteri are the most common abnormalities affecting 3.9% of all women [8].
Framed IUDs
LARC methods are considered important for reducing the number of unintended pregnancies. The Contraceptive CHOICE Project (CHOICE) was developed to promote the use of long-acting methods in the St. Louis region (USA); most subjects aged 18 years and older selected intrauterine contraception (∼70%) [9]. Current IUDs, however, have a number of drawbacks, particularly when used in young, nulliparous, or adolescent women [10]. An essential feature of intrauterine contraceptives is their long duration of action which could be a useful strategy to prevent unintended pregnancy, however, this only applies in the absence of side effects. According to H. Hasson, “The optimum geometric relationship of a properly inserted IUD is one in which the greatest transverse dimension of the IUD is equal or slightly in excess of the fundal transverse dimension” [11]. This statement suggests that measuring the width of the uterine cavity is paramount in the acceptance, performance and continuation of use of the method as geometric compatibility will result in fewer side effects. IUDs should ideally be used for the full approved duration of action. This is, however, still a challenge for researchers as early discontinuation happens too often [12].
An IUD design that fits properly will likely lead to higher patient acceptability, a prerequisite to continuation of use. Dimensional incompatibility, on the other hand, can be a cause of cramping, pain, erratic bleeding or menorrhagia, displacement or expulsion. These effects may be exacerbated around the time of menses when the uterine contraction forces can be substantial. The size of the intrauterine foreign body, in relation to the uterine cavity, determines its acceptability and influences menstrual bleeding. Abnormal and heavy menstrual bleeding in IUD users is an issue which can be resolved. The effect may be eliminated or reduced through the use of hormonal IUDs which effectively mask menstrual bleeding but the underlying cause of uterine incompatibility is still present. The IUD in Figure 2A demonstrates an optimal relationship for a conventional framed T-shape device with the uterine cavity with a maximal fundal distance of 32 mm. Insertion of such a device in a women with a smaller cavity of 15 mm (Figure 2B) would likely result in severe discomfort, malpositioning and displacement. This woman had a successful insertion of a frameless device (Figure 2B). Women with a malpositioned IUD as in Figure 2C are likely to request removal of the IUD. A review of recent IUD studies in young women reported discontinuation rates up to 45% during the first year [10]. The majority of women using conventional framed IUDs discontinue IUD use long before the end of the lifespan of the IUD [13]. In the CHOICE study, continuation rates at 5 year were 51.7% for the LNG-IUS and 55.9% for the TCu380 IUD, respectively [14].
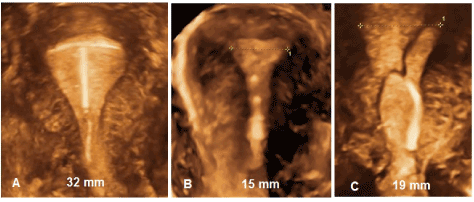
Figure 2: A) 3D ultrasound of a T-shaped IUD in a 32 mm wide uterus width (courtesy Dr. B.enacerraf, Boston, USA); B) 3D ultrasound of narrow uterine cavity (15 mm) width (courtesy Dr. S. Jandi, Berlin, Germany); C) 3D ultrasound demonstrating geometric discrepancy between IUD and uterine cavity leading to early discontinuation width (courtesy Dr. S. Jandi, Berlin, Germany) .
Hysteroscopy allows direct observation of the uterus and is a perfect tool to identify IUD problems in the office. Moreover, it allows the IUD to be repositioned if the uterine cavity is suitable. Figures 3A and 3B show some examples of displaced IUDs of patient who consulted with problems of pain and bleeding. Approximately 50% of patients with displaced IUDs are symptomatic leading to removal of the IUD [15].
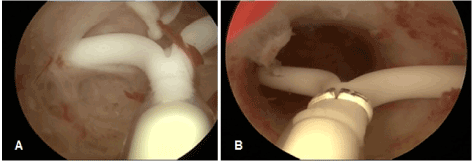
Figure 3: A) IUD with embedded arms in the fundal portion of the uterus; B) Displaced IUD with both arms embedded in the cervix.
Frameless IUDs
Frameless, copper-releasing and levonorgestrel-releasing intrauterine devices are anchored to the fundus of the uterus. The anchor consists of a preformed knot consisting of non-absorbable suture material. It is inserted into the fundus with a simple device which allows for proper placement and minimizes risk of inadvertent perforation. After ensuring fundal placement the frameless IUD conforms to each transverse width of the uterine cavity and exhibits a high degree of flexibility due to its segmented design features. The device’s small size, its flexibility and its unique anchoring mechanism assure that the device is resistant to myometrial expulsive forces. Clinical trials suggest a one-dimensional frameless copper IUD or frameless levonorgestrel-releasing intrauterine system most likely to be symptom free, because it is theoretically capable of adapting to asymmetrical myometrial forces (Figure 3). The myometrial forces act below the anchor mechanism and largely below the linear shape of the frameless devices, which may allow them to adapt to the highly distorted uterine cavity shape which the changes and pressures of severe asymmetrical forces can produce. Figure 4 illustrates the position of the frameless IUD in the uterine cavity as well as the dimensional compatibility, even if the fundal transverse diameter is sometimes extremely small.
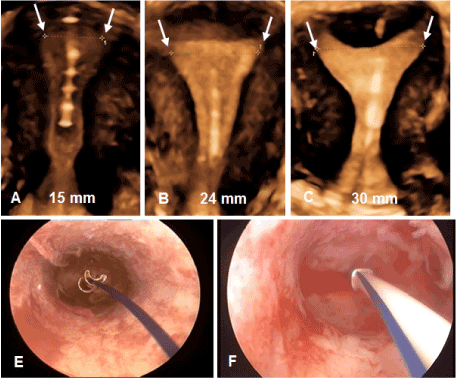
Figure 4: 3D ultrasound and hysteroscopic pictures of frameless copper and levonorgestrel-releasing IUDs. A – C) 3D of frameless GyneFix® copper IUD in cavities of different size and shape width (courtesy Dr. S. Jandi, Berlin, Germany); E) Hysteroscopic view of frameless copper IUD in narrow uterine cavity; F) 3D of frameless Fibroplant® levonorgestrel IUD (APCOR R&M, Ghent, Belgium).
The frameless IUD offers some significant advantages as the risk of malposition of the IUD is unlikely if the fundus is accessible and not deformed due to the presence of a septum or an acquired abnormality (e.g., adenomyosis, fibroid). Its small size allows it to be used without consideration of uterine size or shape. It can easily be inserted in small or large uterine cavities due to its anchoring mechanism. Its location can easily be assessed with the use of ultrasound, either 2D or 3D. The frameless systems has been inserted in numerous women with smaller uterine cavities some being as small as 6 to 8 mm in diameter. As the force to remove the IUD is substantial, expulsion or displacement is rare [16]. The one-dimensional design of the frameless IUS explains its high acceptability and high continuation of use. Clinical trials reported no or very limited decrease in annual removal rates over time, up to 5 years if adjusted for removal because of desire of pregnancy. Continuation rates with the frameless GyneFix 200 IUD and the frameless LNG-IUS remain high (over 90% at 5 years) due to the low rates of removal for bleeding and pain, whereas these rates reduce by up to 10% each year with conventional T-shaped IUDs yielding continuation rates of only 40 to 50% at 5 years [10,17].
Conclusion
In terms of IUD tolerance and continuation of use, from a practical point of view, the worst case is to insert an IUD which is too big for the uterine cavity. To be well tolerated, an IUD, whether framed or frameless in design, should cause a minimum of distortion of the endometrial cavity during the maximum degree of the contraction phase of the uterus during menstruation. In theory, a one-dimensional frameless IUD/intrauterine system probably provokes the least reaction from the uterus and is likely to be universally tolerated, as clinical trials suggest [18].
Providers of IUDs should realize that the best way to obtain comfort during IUD use and a high continuation rate is by using an IUD that is not wider than the width of the uterine cavity. The new smaller version of Mirena, named Jaydess/Skyla has a transverse arm length of 28 mm. The results of initial clinical trials are encouraging [19,20] but the long-term results may not be significantly different from Mirena. The 28 mm transverse arm may still be too long for many women as the mean IUD cavity width is less than 22 mm in many of them. The smaller the transverse width of the uterine cavity, the more likely incompatibility problems may occur. Therefore, the design characteristics of the frameless IUD would be attractive as a possible first choice method for many women, especially for those found to have a small (e.g., nulliparous women) or a too big cavity, and for women who have experienced problems with framed IUDs.
Expert opinion
Key findings
The overall objective of any LARC is to reduce unintended pregnancies. IUDs are almost universally viewed by physicians, researchers and AID organizations as potentially being able to contain the epidemic of unwanted pregnancies and are therefore advocated as they don’t require daily adherence as do the pill, the dermal patch, and the vaginal ring. Locally acting drugs also avoid systemic effects which may cause health and sexual problems such as vascular disease and decreased libido. IUDs also have the highest continuation of use of all contraceptives, and thus protect up to 20 times better than pills, patches, and rings to prevent pregnancy [21].
Contrary to current beliefs, uterine cavities are different from woman to woman and, therefore intrauterine contraception must be individualized with attention to width and length of the uterine cavity. When evaluating the size and shape of the uterine cavity, 2D and 3D ultrasonography is by far the easiest and cheapest method to also diagnose uterine anomalies or other gynecological conditions which may affect IUD/uterus compatibility. The evaluation of the uterine cavity by ultrasound is simple and fast. Unfortunately, sonographic cavimetry as a screening for uterine size and to identify congenital or gynecological uterine anomalies is not yet carried out routinely in most clinical practices. Some practitioners organize special consultations for IUD insertion and reserve sufficient time for pre-insertion counselling, ultrasound evaluation of the uterine cavity, and pre-insertion pain relief (e.g., local anesthesia, anesthetic gel instillation). These thoughtful attentions are highly appreciated by women and help with the acceptance of the IUD.
Frameless IUDs have significant potential advantages over framed IUDs, as they fit in cavities of every size and shape (“one size fits all”). Due to the absence of a plastic frame, measuring the size of the uterine cavity is unnecessary, but may still be performed to aid in insertion planning.
The challenge
The selection of a T-shaped IUD based on the measurement of the transverse width of the uterine cavity is best practice as it likely will result in higher continuation rates. Today, most IUDs have a transverse width of 28 or 32 mm. IUDs with a shorter arm length are required that match the reduced width of uterine cavities in many women. Health care providers with special interest in intrauterine contraception should give attention to spatial compatibility and to mastering the anchoring technique as it is the only type of technology that fits all uterine cavities.
Declaration of interest
Dirk Wildemeersch, MD, PhD, has been involved in the optimization of new, innovative, drug delivery systems for use in the uterus. He did not receive any financial compensation of any kind. He is currently advisor in devising new concepts in controlled release for contraception and gynecological treatment. Thomas Hasskamp, Norman Goldstuck: nil.
References:
2021 Copyright OAT. All rights reserv
- Trussell J (2011) Contraceptive failure in the United States. Contraception 83: 397–404. [Crossref]
- American Congress of Obstetricians and Gynecologists (2012) Committee Opinion number 539.
- Da Costa A, Filho FM, Ferreira AC, Spara P, Mauad FM (2004) Uterine volume in adolescents. Ultrasound Med Biol 30: 7–10. [Crossref]
- Chen X, Guuo Q, Wang W, Huang L (2015) Three-dimensional ultrasonography versus two dimensional ultrasonography for the diagnosis of intrauterine device malposition. Int J Obstet Gynecol 128: 157–159. [Crossref]
- Wildemeersch D, Hasskamp T, Nolte K, Jandi S, Pett A, et al. Uterine cavity width in over 400 nulliparous women –A multicenter study. (Contrel Research, Data on File).
- Canteiro R, Bahamondes V, dos Santos Fernandes A, Espejo-Arce X, Marchi NM, et al. (2010) Length of the endometrial cavity as measured by uterine sounding and ultrasonography in women of different parities. Contraception 81: 515–519. [Crossref]
- Kurz KH (1984) Cavimeter uterine measurements and IUD clinical correlation. In: Zatuchni GI, Goldsmith A, Sciarra JJ, editors. Intrauterine Contraception: Advances and Future Prospects. Philadelphia: Harper and Row:142–162.
- Chan YY, Jayaprakasan K, Zamora J, Thornton JG, Raine-Fenning N, et al. (2011) The prevalence of congenital uterine anomalies in unselected and high-risk populations: a systematic review. Hum Reprod Update 17: 761–771. [Crossref]
- Mestad R, Secura G, Allsworth JE, Madden T, Zhao Q, et al. (2011) Acceptance of long-acting reversible contraceptive methods by adolescent participants in the Contraceptive CHOICE Project. Contraception 84: 493–498. [Crossref]
- Wildemeersch D, Jandi S, Pett A, Nolte K, Hasskamp T, et al. (2014) Use of frameless intrauterine devices and systems in young nulliparous and adolescent women: results of a multicenter study. Int J Womens Health 6: 727–734. [Crossref]
- Hasson HM (1984) Clinical studies of the Wing Sound II metrology device. In: Zatuchni GI, Goldsmith A, Sciarra JJ, editors. Intrauterine Contraception: Advances and Future Prospects. Philadelphia: Harper and Row: 126–141.
- Wildemeersch D (2011) Intrauterine contraceptives that do not fit well contribute to early discontinuation. Eur J Contracept Reprod Health Care 16: 135–141. [Crossref]
- Moreau C, Trussell J, Rodriguez G, Bajos N, Bouyer J (2007) Contraceptive failure rates in France: results from a population-based survey. Hum Reprod 22: 2422–2427. [Crossref]
- Diedrich JT, Madden T, Zhao Q, Peipert JF (2015) Long-term ultilization and continuation of intrauterine devices. Am J Obstet Gynecol 213: 822.e1-6. [Crossref]
- Liang H, Li L, Yuan W, Zou Y, Gao ES (2014) Dimensions of the endometrial cavity and intrauterine device expulsion or removal for displacement: a nested case–control study. BJOG. [Crossref]
- Wildemeersch D (2004) The force required to remove the frameless 0-suture anchoring system: comparison between pre- and postmenopausal women. Contraception 69: 513–515. [Crossref]
- Wildemeersch D, Pett A, Jandi S, Hasskamp T, Rowe P, et al. (2013) Precision intrauterine contraception may significantly increase continuation of use: a review of long-term clinical experience with frameless copper-releasing intrauterine contraception devices. Int J Women’s Health 5: 215–225. [Crossref]
- Goldstuck N, Wildemeersch D (2014) Role of uterine forces in intrauterine embedment, perforation, and expulsion. Int J Women’s Health 6: 735–744. [Crossref]
- Nelson A, Apter D, Hauck B, Schmelter T, Rybowski S, et al. (2013) Two low-dose levonorgestrel intrauterine contraceptive systems: a randomized controlled trial. Obstet Gynecol 122: 1205–1213. [Crossref]
- Gemzell-Danielsson K, Buhling KJ, Dermout SM, Lukkari-Lax E, Montegriff E, et al. (2016) A Phase III, single-arm study of LNG-IUS 8, a low-dose levonorgestrel intrauterine contraceptive system (total content 13.5 mg) in postmenarcheal adolescents. Contraception 93: 507–512. [Crossref]
- Winner B, Peipert JF, Zhao Q, Buckel C, Madden T, et al. (2012) Effectiveness of long-acting reversible contraception. N Engl J Med 366: 1998–2007. [Crossref]




