Abstract
One of the most common problems in today´s clinics is tooth wear, specifically when related to bruxism. The prefabricated restorations have some advantages of direct composite and indirect restorations. The following case report describes the step-by-step treatment of rehabilitation of multiple restorations in a patient with indirect prefabricated composite veneers and the one year follow-up after this rehabilitation. An interesting aesthetic result that accommodates a patient´s financial means and that restores the smile can be achieved using this simple technique.
Key words
tooth wear, ceramic, aesthetic treatment
Introduction
The demand for aesthetic treatments in dentistry has increased progressively over the years and has resulted in the development of dental materials that meet both aesthetic and functional requirements of patients [1].
Ceramics have been considered the material of choice for reconstruction of anterior teeth [2]. This material has shown effectiveness in reproducing the structure and translucency of a natural tooth. Various studies have shown high success rates and excellent biocompatibility and chemical stability studies of large follow-up times [3-6]. Meanwhile, the indirect composite resins have been an alternative to these ceramic materials. Although they are more recently used, the direct technique with composite resins requires much skill and professional training, as well as care during the execution of preparation, which can increase treatment costs [7]. A newer alternative has been introduced recently in the dental market and may also be utilized: Componeers (Coltène Whaledent). The prefabricated composite veneer technique has some of the advantages of direct composite and ceramic restorations, as only one session is required without the need to take impressions and send them to the prosthetic laboratory. Furthermore, minimal preparation is usually required. The Componeer is a pre-fabricated nano-hybrid-composite enamel veneer in order to combine the advantages of direct composite resin with laboratory-fabricated laminate veneers [8]. In addition, the context of this system relies in the context of “natural layering concept“ in which two layers with the incremental technique is able to mimic the natural anatomy of a tooth [9].Despite being a new material, this technique has shown promising results in cases of devitalized teeth with dentin discoloration [10], in multiple old restorations with marginal discoloration [2], and in dental fluorosis [11]; however, it no case reports using these prefabricated veneers in large old restorations in patients with Para functional habits, or more accurately, bruxism, were found in the literature.
In this way, the aim of this case report is to describe the step-by-step treatment of rehabilitation of multiple restorations in a patient with indirect prefabricated composite veneers (Componeer system) and the one-year follow-up after this rehabilitation in a patient with bruxism.
Case report
A 58-year-old male patient sought the School of Dentistry for aesthetic treatment, complaining about the lackingaestheticof his smile. A detailed dental and medical history was obtained. Clinically, the patient presented low periodontal condition, with wide and faulty multiple-composite resin restorations in the anterior upper teeth and a gold crow on the tooth # 12, which was fractured. In addition, the anterior lower teeth had wear facets due to bruxism history (Figure 1).
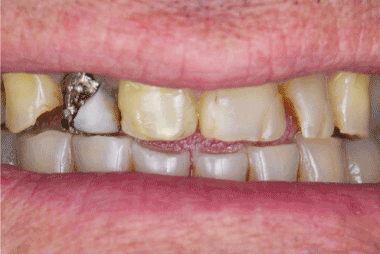
Figure 1. Initial smile, Note the discolorations and multiple old restorations, as well as a gold crow on fractured tooth # 12.
In the first session, an initial impression with addition silicone (Virtual®, Ivoclar-Vivadent, Schaan, Liechtenstein) was done to prepare stone models, a diagnostic wax-up and a mock-up to obtain study design and planning for the treatment [12]. Also, a periodontal prophylaxis was performed in order to remove supragingival calculus, especially in the anterior lower teeth.
After careful evaluation of the patient’s expectations with regard to his smile, the esthetic treatment plans included dental bleaching in order to increase the outline of the clinical procedures, followed by multiple direct composite resin restorations and indirect prefabricated composite veneers with the Componeer system on teeth # 13, 12, 11, 21, 22, and 23.
The next session was held to remove the fractured crown of tooth # 12. After its removal, it was observed that the post and core of this tooth was properly adapted and confirmed in detailed clinical and radiographic examinations. So, the tooth was re-prepared to receive an all-ceramic crown. A ferrule at the coronal end on the buccal, palatal, mesial, and distal surfaces with 2.0 mm in height and 1.2 mm in depth was confirmed and obtained. Reductions of 1.5 to 2.0 mm were performed on the occlusal surfaces and 1.0 to 1.5 mm in buccal and palatal surfaces. All angles were rounded, and the cervical finish line was continuous, defined, and clear. After the re-preparation, the core was finished and polished with Sof-Lex aluminum oxide discs (3M-ESPE, St Paul, MN, USA); and an impression of the prepared crown was taken with addition silicone (Virtual®, Ivoclar-Vivadent) and sent to a prosthetic laboratory. The all-ceramic crown was fabricated with the IPS e-max System (Ivoclar-Vivadent).
One week after testing, the all-ceramic crown was cemented on tooth #12 (Figure 2). The internal area of the crown was conditioned with 37% phosphoric acid gel (Total Etch, Ivoclar-Vivadent) for 1 min and water rinsed for 2 min. The surfaces of the core and the remaining tooth substrate were etched with 37% phosphoric acid gel (Total Etch, Ivoclar-Vivadent) for 30s and 15s, respectively,and they were rinsed for 60 s with an air-water spray; both conditionings (crown and core) with the cleaning purpose. Excess water was removed by gently blowing air. After that, the silane (Ivoclar-Vivadent) was applied on the indirect crown and left to dry during 20s. A dual-cure adhesive system (Excite DSC [commercially available in the USA as Excite F DSC], Ivoclar-Vivadent) was applied on the core and on the remaining tooth substrate and light-cured for 10 s. The base and catalyst components of Variolink II shade A3 (Ivoclar-Vivadent) were mixed and introduced into the indirect crown. The crown was seated, the excess resin cement was removed, and the cement was light-cured for 40 s on each crown surface. Excess cement was removed with a #12 scalpel blade.
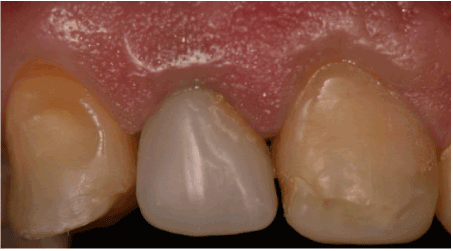
Figure 2. The all-ceramic crown was cemented on tooth # 12
In another session, it was decided to repair or replace all the defective restorations of teeth # 14, 13, 11, 21, 22, 23,24, 25, 34, 35, 44, and 45 using direct composite resin (Opallis, FGM, Joinville, SC, Brazil) (Figure 3).
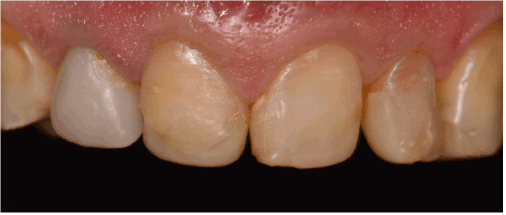
Figure 3. Final view after replacement of old restorations.
After all completed restorations, based on the initial planning, the veneers’ prefabricated composite Componeer (COLTÈNE, Altstätten, Switzerland) asselected with the Guiide out Lines Brilliant NG Componeer present in the kit (COLTÈNE, Altstätten, Switzerland) (Figure 4). After the relative isolation of the operative field, made with cotton rollers and yarn retractor, minimally invasive preparations were made with bevel, not exceeding 0.3 mm thick enamel (Figure 5). These preparations were made to promote perfect fit of the veneers.
These prefabricated veneers are made of a pre-cured hybrid composite, Synergy D6 (COLTÈNE), and must be cemented to the same hybrid composite in which they are made, thereby providing a restoration as a monoblock unit. For the process of grouting, the acid 37% (during 30s and rinsed with water) and adhesive system Magic Coltene (15s) was applied to all areas of enamel and dentin to be cemented. The coat adhesive system (COLTÈNE) was applied to the tooth structure and the inner surface or the contact of the veneers for at least 20s, and then the stream of air was applied shortly. Then, without curing of the adhesive system, a resin portion was placed on the enamel dental and also on the inner surface of the veneer to provide shape and contour restorations to mimic the color naturally with the adjacent enamel (Figure 7).
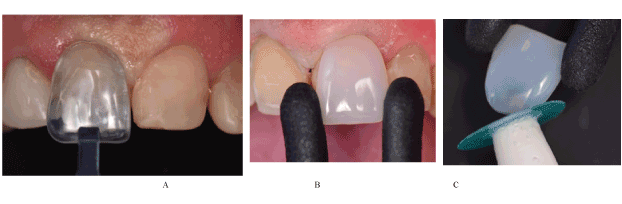
Figure 4. A) Size selection using contour guide B) Selection of prefabricated veneer B) Adaptation the prefabricated veneer with a abrasive disk.
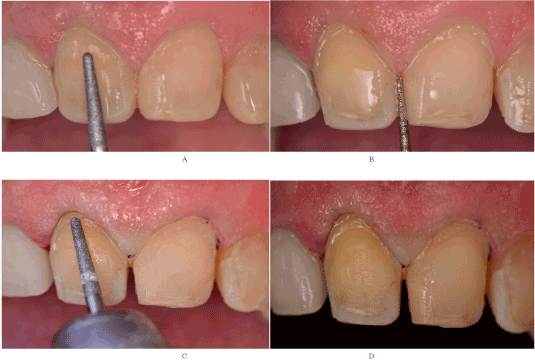
Figure 5. A) An extra-fine diamond is used to finish the preparations. B) Preparation of tooth to receive the veneers C) The cervical marginis delimited with a bur. D) View final of tooth preparation.
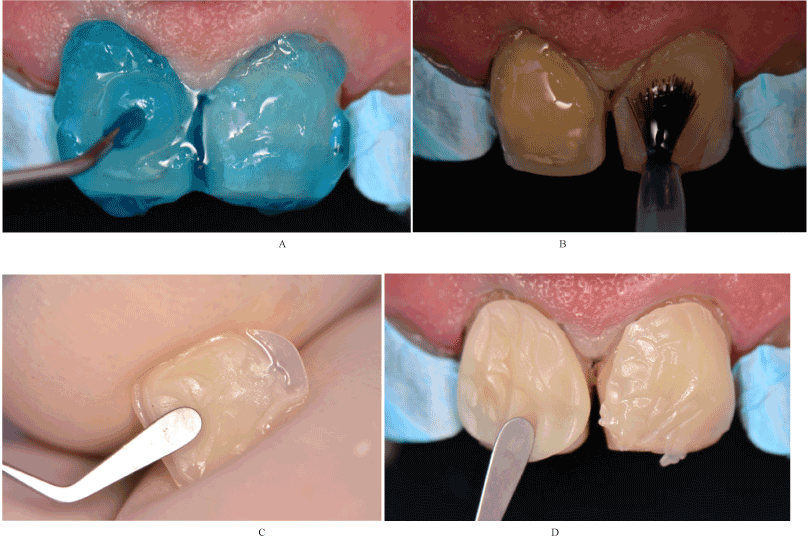
Figure 6. A) Preparations were etched with phophoric acid. B) Application of the dentin adhesive to the preparations. C) Enamel composite was applied on the surface of the prefabricated veneer D) Composite was applied on to the tooth surface.
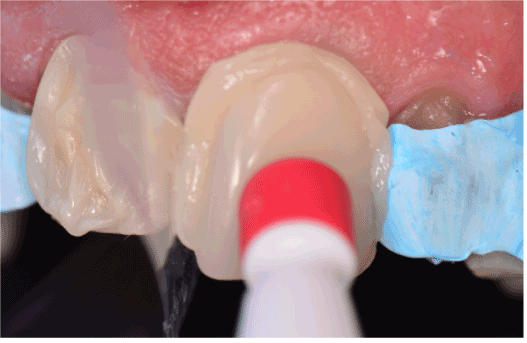
Figure 7. Positioning of the veneers. The restorations were aligned with the midline and the incisal position checked prior to light-curing.
The veneer is then placed on the tooth. With its own device system for placement of facets, Componeer is then moved carefully to the end position, causing a slight but steady pressure (Figure 6). In this case, the restorations were more than two front teeth, so the alignment of facets began with the two central incisors. While the veneer was maintained in the desired position, the excess over flowed material was removed; the matrix previously placed in the interdental space prevented the adhesion of the tooth adjacent to the tooth to be restored (Figure 8). After this step, the set was light-cured with LED (VALO, Ultradent Products, Inc., South Jordan, USA) for 20 s at1400 mW/cm2.
Contours and occlusal interferences fit into a high-speed bur as needed. Finishing and polishing strips were used in the proximal area (Hot Spot Design, Curitiba, Paraná, Brazil). Finally, disks and silicone rubber (TDV, Pomerode, Santa Catarina, Brazil) were used for the polishing of restorations, followed by polishing paste application (Universal Polishing Paste, Ivoclar Vivadent, Barueri, São Paulo, Brazil) with felt disks (TDV) (Figure 9).
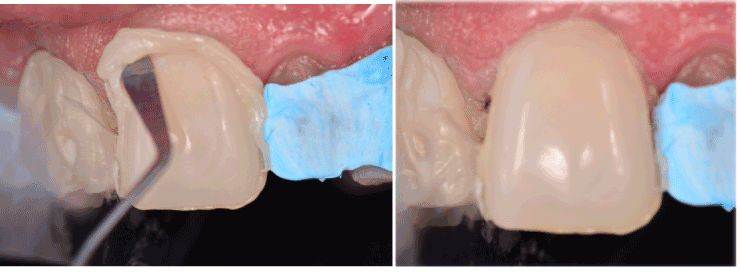
Figure 8. A) Excess material was removed. B)The matrix previously placed in the interdental space prevented the adhesion of the tooth adjacent.
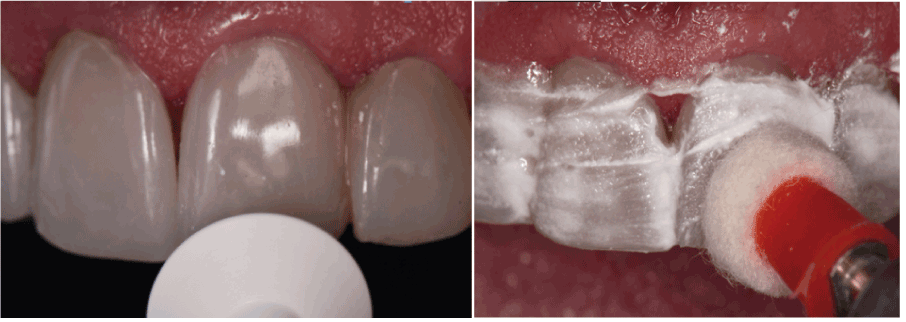
Figure 9. A) Finishing and polishing the restorations using discs and silicone rubber pointsB) Polishing paste application.
As for bruxism frame that the patient presents, counseling was managed as well as preparation of occlusal splint to manage and reduce daily stress, so as to preserve the oral health of the patient, especially after the cementation of veneers. After seven days, the patient returned and new adjustments were made, especially occlusal and proximal as well as new polishing.
The final aspect of the case can be observed immediately (Figure 10), and one year after cementation of veneers (Figure 11), whereby the frame remained stable for esthetic and mastication of the patient, confirming the efficacy of treatment using prefabricated veneers.
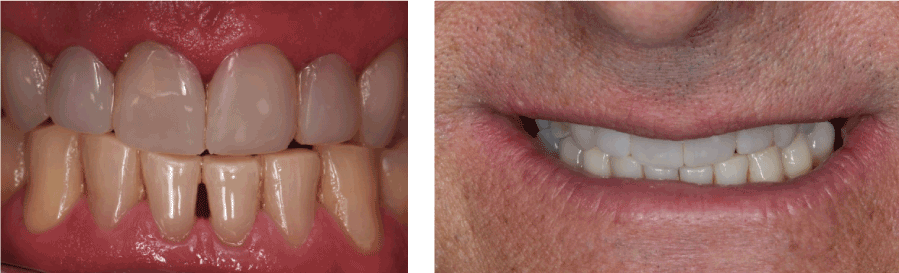
Figure 10. Final clinical case.
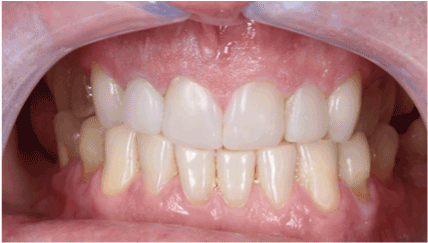
Figure11. The view of the restorations at one-year recall.
Discussion
There are several therapeutic options for the treatment of teeth with old and large restorations with marginal discoloration, infiltration and mismatches (Dietschi 2008). However, in this present case described, the use of prefabricated facets composite was presented our choice, since the technique is conservative, allowing a minimum wear of the tooth structure.
In comparation to the facets on ceramic, or even crowns have disadvantages such as excessive wear during tooth preparation, and even damage to the surrounding tissues (Peumans et al. 2000). Furthermore, cost of treatment is significantly more than dental ceramics; approximately 60 USD versus 30 USD.
Moreover, many authors have shown that in patients with parafunction, the success rate of ceramic restorations reduced by 60% (Magne et al. 1999). In addition, a decrease in wear resistance and a higher incidence of fractures in ceramic restorations has been observed in these patients (Granell-Ruiz et al. 2014, Reitemeier et al. 2013). In these cases, so there is the possibility of using composites (Mangani et al. 2007).
Indirect ceramic restorations have some advantages relative to composite resins, among which are greater color stability, wear resistance, biocompatibility, and durabilidade [13-15], other hand are friable and thus more susceptible to fracture .Excessive wear promotes the antagonist teeth, which in this case is the main problem since the patient has evidence of bruxism, in addition to requiring more invasive preparations when associated with metallic structures [14,16]. Direct composite resin restorations would also be a treatment option in this case, as has been observed in the literature, but it was not the technique of choice for this event due to the time required for its development and the difficulty of applying the technique [17-19].
When comparing the direct restorations, prefabricated veneers have the advantage of reduction of polymerization shrinkage, which remains limited to cementation line, decreasing the formation of gaps at the interface tooth/restoration, post-operative hypersensitivity, and micro leakage [20,21]. On the advantage that the technique of prefabricated composite veneers present as well as the time. In this case, the results were achieved with only four visits until the additional polishing accompaniments at the end. It was necessary to make an impression only for the restoration of tooth #12.Alsoindirect work at a prosthetic laboratory was necessary because of the replacement of the gold crown. In addition, occlusal adjustment was employed to homogenize the contacts and eliminate premature ones.
The concept of one-visit prefabricated resin-based veneers is not new. In the early 1980s, prefabricated acrylic veneers were introduced as Mastique Laminate Veneer System (Caulk, Milford, DE, USA). The intaglio surface of Mastique veneers was etched with poly acrylic acid and then adapted to acid-etched enamel using a light-curing composite and an unfilled bonding resin. These veneers had limited success because of technological limitations and poor surface qualities [22,23]. Clinical studies have confirmed good performance of porcelain veneer restorations, with excellent aesthetics, overall patient satisfaction, and no adverse effects on the periodontal tissues [24]. Whereas the main reason for failure was fracture of the ceramic, increased failure rates were associated with nonvital teeth and bruxism; for this reason, ceramic laminates were not chosen in this case.
The clinical outcome of indirect veneers depends on the strength of two interfaces: the tooth/resin cement and the veneer/resin cement interfaces. A recent bond strength study reported that Componeer prefabricated veneers resulted in micro shear bond strengths statistically similar to those of etched IPS E.max Press (Ivoclar Vivadent, Schaan, Liechtenstein), [25] when the respective adhesive and luting composite were applied to the intaglio surfaces. The high bond strengths obtained between the Componeer intaglio surface and the respective hybrid composite may be a result of two mechanisms: a strong adsorbed layer of polymer material forms on the intaglio surface. This adsorption is a consequence of an initial increase in the ionization rate of the carboxylic groups in the adhesive used because of the production of acid via the photo initiator [25,26], and residual reactive methacrylate functionalities on the intaglio surface may form a network with the bonding agent after polymerization [27], which may explain the relatively high bond strengths associated with the adhesive joint formed by the prefabricated veneer, the dentin adhesive, and the direct hybrid composite resin.
The literature reports that some type of occlusal interference can be found in all patients with bruxism, which can be extremely damaging [28,29]. With the elimination of interference at the expense of the bitesplintor occlusal adjustment, the muscular behavior usually becomes normal [29,30]. Despite this difficulty but with the need for restructuring the patient’s harmony and function, we opted for the choice of treatment coupled with the production of a plate to ease the symptoms of bruxism and also protect the new restorations of the patient.
In the clinical situation presented, it is crucial to evaluate the clinical behavior of this restorative technique performed, especially in situations like the present case report in which the patient had assigned wear to bruxism. At one-year follow-up after treatment, there is still high patient satisfaction. All restorations were fixed in place, aesthetics were very good, margins were sound, and there was no staining or discoloration.
The clinical technique described in this paper has the potential to be used routinely to lengthen the anterior teeth, to correct malpositioned teeth, to mask discolorations, and to close diastemas [25,31]; therefore, it can be concluded that the proposed treatment held a financially advantageous solution, besides being appropriate to restore harmony aesthetics and conservative when compared to a treatment involving the prosthetic work. The removal of tooth structure was negligible, and rehabilitation with the prefabricated composite veneers in a single session was possible, with stable and satisfactory aesthetic results. Although the case of this study has shown promising results in patients with various restorations and Para functional habits, more clinical studies are needed to validate it.
Conclusion
Prefabricated composite veneers have some of the advantages of direct composite restorations, as only one session is required and there is no need to make impressions or engage in laboratory work. Additionally, the restorations can be customized (color and shape) and are more affordable than other indirect restorations, resulting in a very aesthetic outcome. It is crucial to assess the clinical behavior of this restorative technique prior to recommending it in general practice.
Disclosure and Acknowledgements
The authors do not have any financial interest in the companies whose materials are included in this article.
References
- Pini NP, Aguiar FHB, Lima DANL, Lovadino JR, Terada RSS, et al. (2012) Advances in dental veneers: materials, applications, and techniques. Clin Cosmet Investig Dent 4: 9–16. [Crossref]
- Gomes G, Perdigão J (2014) Prefabricated compositeres in veneers – A clinical review. J Esthet Restor Dent 26: 302-313. [Crossref]
- Kreulen CM, Creugers NHJ, Meijering AC (1998) Meta-analysis of anterior veneer restorations in clinical studies. J Dent 26: 345-353. [Crossref]
- Mangani F, Cerutti A, Putignano A, Bollero R, Madini L (2007) Clinical approach to anterior adhesive restorations using resin composite veneers. Eur J Esthet Dent 2:188-209. [Crossref]
- Lawson NC, Burgess JO (2014) Dental ceramics: a current review. Compend Contin Educ Dent 35: 161-166. [Crossref]
- Li RW, Chow TW, Matinlinna JP (2014) Ceramic dental biomaterials and CAD/CAM technology: state of the art. J Prosthodont Res 58: 208-216. [Crossref]
- Dietschi D, Devigus A (2011) Prefabricated composite veneres :Historical perspectives, indications and clinical application. Eur J Esthet Dent 6:178–187. [Crossref]
- Aschheim K (2014) Esthetic Dentistry. A Clinical Approach to techniques and materials. (3rd edn.) Elsevier (MO).
- Dietschi D, Ardu S, KrejciI (2006) A new shading concept basedon natural tooth color applied to direct composites restorations. Quintessence Int 37: 91-102. [Crossref]
- Gonçalves R, Correia I, Ferreira JC, et al. (2015) Descoloração dentinária: aplicação de facetas Componeer. Rev Port Estomat Med Dent Cir Maxil 56:132–138.
- Du Toit J, Patel N, Montalli V, et al. (2012) Aesthetic treatment of severely fluorosed teeth with prefabricated composite veneers: a case report. Int Dent Sou Afr 2: 44-50.
- Viana PC, Correia A, Neves M, Kovacs Z, Neugbauer R (2012) Soft tissue waxup and mock-up as key factors in a treatment plan: case presentation. Eur J Est Dent 7: 310-323. [Crossref]
- Attia A, Abdelaziz KM, Freitag S, Keran M (2006) Fracture load of composite resin and felds pathicall-ceramic CAD/CAM crowns. J Prosthet Dent 95:117-123. [Crossref]
- Kassem AS, Atta O, El-Mowafy O (2012) Fatigue resistance and microleakage of CAD/CAM ceramic and composite molar crowns. J Prosthodont 21: 28-32.
- Stawarczyk B, Egli R, Roos M, et al. (2011) The impact of in vitro aging on the mechanical and optical properties of indirect veneering composite resins. J Prosthetic Dent 106: 386-398. [Crossref]
- Tsitrou EA, Helvatjoglu-Antoniades M, Van Noort R (2010) A preliminaryevaluation of the structural integrity and fracture mode of minimally prepared resin bonded CAD/CAM crowns. J Dent 38:16-22. [Crossref]
- Terry DA (1999) Direct reconstruction of the maxillary anterior dentition with composite resin: A case report. Pract Period Aesthet Dent 11:361–367. [Crossref]
- Pontons-Melo JC, Pizzatto E, Furuse AY, et al. (2012) A conservative approach for restoring anterior guidance: a case report. J Esthet Restor Dent 24: 171-182. [Crossref]
- Ahmed KE, Murbay S (2015) Survival rates of anterior composites in managing tooth wear: systematic review. J Oral Rehabil 43:145-153. [Crossref]
- El Zohairy AA, De Gee AJ, Mohsen MM, et al. (2003) Microtensile bond strength testing of luting cements to prefabricated CAD/CAM ceramic and composite blocks. Dent Mater 19: 575-583. [Crossref]
- Batalha-Silva S, Andrada MA, Maia HP, et al. (2013) Fatigue resistance and crack propensity of large MOD composite resin restorations: Direct versus CAD/CAM inlays. Dent Mater 29: 324-331. [Crossref]
- Dietschi D, Devigus A (2011) Prefabricated composite veneers: Historical perspectives, indications and clinical application. Eur J Esthet Dent 6: 178–187. [Crossref]
- Jensen OE, Soltys JL (1986) Six months clinical evaluation of prefabricated veneer restorations after partial enamel removal. J Oral Rehabil 13: 49–55. [Crossref]
- Peumans M, Van Meerbeek B, Lambrechts P, Luque-Martinez IV, Loguercio AD. (2000) Porcelain veneers: A review of the literature. J Dent 28:163–177. [Crossref]
- Perdigão J, Sezinando A, Muñoz M A, Luque-Martinez IV, Loguercio AD (2014) Prefabricated veneers — bond strengths and ultra-morphological analyses. J Adhes Dent 16: 137–146. [Crossref]
- Sahin G, Albayrak AZ, Bilgici ZS, Avci D (2009) Synthesis and evaluation of new dental monomers with both phosphonic and carboxylic acid functional groups. J Polym Sci Part A Polym Chem 47: 1953–1965.
- Moszner N, Salz U, Zimmermann J (2005) Chemical aspects of self-etching enamel-dentin adhesives: A systematic review. Dent Mater 2: 895–910. [Crossref]
- Bernardon JK, Maia EA, Cardoso AC (2002) Diagnosis and management of maxillary incisor saffected by incisal wear: an interdisciplinary case report. J Esthet Restor Dent 14: 331–339. [Crossref]
- Dawson PE (2007) Functional occlusion: from TMJ to smile design.
- Granell-Ruíz M, Agustín-Panadero R, Fons-Font A, et al. (2014) Influence of bruxism on survival of porcelain lamínate veneers. Med Oral Patol Oral Cir Bucal 19: 426-432. [Crossref]
- Dietschi D (2008) Optimizing smile composition and esthetics with resin composites and other conservative esthetic procedures. Eur J Esth Dent 3:14-29. [Crossref]











