Abstract
Background: Little is known about whether US clinicians feel obligated to provide referrals for women desiring abortion. We assessed attitudes about and correlates of abortion referral among clinicians in a rural US state.
Methods: We surveyed family medicine and ob-gyn clinicians in the rural state of Nebraska about referral for in vitro fertilization, high-risk prenatal care, abortion and suspected gynecologic malignancy. We asked whether clinicians have a professional obligation to refer and whether they would indeed refer. We assessed correlates of obligation and referral using multivariate logistic regression.
Results: We analyzed 501 respondents who reported an obligation to refer for abortion least often (52%) compared with in vitro fertilization (78%), suspected gynecologic malignancy (96%), and high-risk prenatal care (98%). High religiosity was independently, negatively correlated with an obligation for abortion referral (OR 0.39, 95% CI 0.24-0.63, p <0.001). Sixty-four percent of respondents would refer for abortion. In multivariate analysis, women were more likely to refer for abortion (OR 1.97, 95% CI 1.13-3.44, p=0.02), while Catholic and more religious clinicians were less likely to refer (OR 0.22, 95% CI 0.06-0.79, p=0.02 and OR 0.17, 95% CI 0.10-0.28, p<0.001, respectively).
Conclusion: Many clinicians in a rural US state believe they are not professionally obligated to and would not refer for abortion. This may lead to delayed care and increased morbidity for women.
Key words
abortion, Nebraska, professionalism, referral
Introduction
Although abortion is legal in the United States (US), increasing abortion restrictions and decreasing numbers of abortion providers have led to unique public health challenges for women accessing abortion services, particularly those in rural settings. Nearly 1 in 5 people live in rural areas of the US [1]. Eighty-nine percent of US counties have no abortion provider [2]. When patients need medical care not available in their community, as is often the case for abortion services, clear referral patterns between primary care providers and specialists provide appropriate and timely care.
Access to specialty reproductive healthcare services for rural women is challenging because US states with the largest rural populations have the lowest number of ob-gyns per 10,000 reproductive-aged women [3]. One in six of all women and nearly one in four rural women who seek abortions in the US must travel greater than 50 miles for care [4]. Previously identified reasons for delays in obtaining abortion care include difficulties finding an abortion provider, distance from the clinic, referral to another clinic (both clinics that do and do not provide abortions) and delays in getting an abortion referral [5]. Prompt and accurate referral to abortion clinics may facilitate a woman’s ability to obtain an abortion.
Numerous professional organizations support referral for abortion as part of pregnancy options counseling, including the International Federation of Gynecology and Obstetrics [6], the Royal College of Obstetricians and Gynecologists [7], the American College of Obstetricians and Gynecologists [8], and the World Medical Association [9]. The World Health Organization (WHO) states that all women should have access to safe and timely abortion care and that healthcare systems should work to reduce barriers to accessing abortion care [10]. Despite these recommendations, US physicians are divided over their professional obligation to refer for services they feel are immoral [11]. For example, one study found that 14% of physicians feel it is ethically permissible to withhold information about safe, legal medical procedures with which a physician disagrees and 29% do not feel obligated to refer for such a procedure [12]. Scholars studying conscientious refusal often argue that physicians who refuse to provide a clinical service should refer the patient to a physician who will [13]. Referral has also been suggested as the preferred method of handling patients seeking services to which a primary care physician objects [14], and obstetrician-gynecologists support conscientious refusal to provide abortion services as long as the physician refers the patient [15]. We explored clinicians’ opinions on professional obligation to refer for abortion and other ob-gyn in Nebraska, a rural US state.[1]
Materials and methods
From October 2014 until January 2015, we mailed a confidential, self-administered survey to eligible licensed clinicians in the state of Nebraska about their referral opinions and practices for four obstetrical and gynecological health scenarios: in vitro fertilization, high-risk prenatal care for fetal anomalies, abortion and suspected gynecologic malignancy. Eligible clinicians were identified through the Health Professions Tracking Service—a directory maintained by the College of Public Health at the University of Nebraska Medical Center. The database contains contact information and practice location for physicians, nurse practitioners and physician assistants with active Nebraska licenses. In this census-based sample, we included all physicians, advanced practice nurses (including nurse practitioners, certified nurse midwives and clinical nurse specialists) and physician assistants who self-identified their primary specialty as obstetrics/gynecology, family medicine, women’s health and/or nurse midwifery. We excluded clinicians in training (i.e., resident physicians). The intuitional review boards at the University of Nebraska Medical Center and the University of California, San Francisco approved the study.
The survey mailing included a personalized cover letter, the consent form with a waiver of written consent, participant bill of rights, paper survey, and a self-addressed return envelope. For subjects who preferred to complete the survey online, we provided a web link to the survey hosted in REDCap, a secure, web-based application for online surveys. We sent reminder letters providing the web link to the online survey two weeks after the initial mailing to clinicians who had not yet returned the survey.
The Health Professions Tracking Service provided clinician type, age, sex, primary specialty, and practice location. The survey asked about referral practices for four clinical scenarios in the following order: in vitro fertilization, high-risk prenatal care for fetal anomalies, abortion for an undesired pregnancy and suspected gynecologic cancer (Table 1). For each scenario, we asked clinicians how and where they would refer the patient, if they had previously referred a patient for similar services and if they had experienced any barriers in the referral process. The survey provided opportunities for write-in responses and general comments for each scenario. At the end of the survey, we asked participants to indicate which of the four clinical scenarios they felt health care providers are professionally obligated to refer for specialty care.
Table 1. Characteristics of survey respondents (n=496)*.
Characteristic |
n (%) |
Age (mean ± SD), years |
46.5 ± 11.6 |
Male |
183 (37) |
Marital status |
|
Single |
57 (12) |
Married |
431 (89) |
Children |
|
None |
50 (12) |
One or more |
382 (88) |
Race |
|
White |
459 (95) |
Non-white |
23 (5) |
Practice characteristics |
|
Specialty |
|
OB/Gyn |
100 (20) |
Family medicine |
396 (80) |
Clinician type |
|
Physician |
247 (50) |
Advanced practice nurse |
122 (25) |
Physician assistant |
127 (26) |
County of practice† |
|
Urban |
282 (57) |
Rural |
214 (43) |
Obstetrics services offered in practice |
297 (61) |
Standardized referral process |
327 (67) |
Years in practice (mean ± SD) |
15.8 ± 10.9 |
Years in practice in Nebraska (mean ± SD) |
14.5 ± 10.4 |
Religious characteristics |
|
Religion |
|
None |
36 (7) |
Protestant |
277 (57) |
Catholic |
157 (32) |
Other |
13 (3) |
Attendance at religious services |
|
Never |
51 (11) |
Once a month or less |
124 (26) |
Twice a month or more |
306 (64) |
Intrinsic religiosity |
|
Low |
219 (47) |
Moderate |
109 (23) |
High |
143 (30) |
Data presented as n (%) or mean ± standard deviation (SD).
*Some groups add to less than 496 because of missing responses. Numbers and percentages are unweighted. Percentages may add to more than 100 due to rounding.
†Rural vs. urban county based on the Office of Rural Health Policy definition.
The survey included questions on general demographic information, the number of years the clinician had been in practice (both overall and in current state), whether their practice offers obstetrical services, if their clinic has a standardized referral process and the religion with which the clinician identified. We categorized religion as Protestant (including Baptist, Methodist, Episcopalian, Christian, Mormon, and Orthodox), Catholic, none (including atheist, agnostic and none) and other (including Jewish, Hindu, Muslim, and Buddhist). We assessed clinician’s intrinsic religiosity by asking to agree or disagree with two statements: “I try hard to carry my religious beliefs over into all my other dealings in life” and “My whole approach to life is based on my religion”. These two statements are from Hoge’s Intrinsic Religious Motivation Scale and have been validated in previous studies [16,17]. We categorized religiosity as low if the respondent disagreed with both statements, moderate if they agreed with one statement and high if they agreed with both. We asked about frequency of attending religious services (never, once a month or less, or twice a month or more) to assess participatory religiosity [18].
Our primary outcome—professional obligation to refer for each clinical scenario—was defined as an affirmative response to the question “Please indicate which of the following clinical scenarios you feel healthcare providers are professionally obligated to refer for specialty care: in vitro fertilization, high-risk prenatal care for fetal anomalies, abortion and suspected gynecologic cancer”. Our secondary outcome—active referral—was defined as any response to the question “how would you refer the patient” indicating referral for each scenario including (1) gives patient clinic name(s) and/or phone number(s), (2) sends patient’s records to the clinic, (3) contacts the clinic and/or clinician, (4) places an electronic referral to a provider, including provide phone numbers or (5) any responses to the open ended questions by the clinician indicating they would give a patient referral information. If a clinician indicated that they would allow the patient to find a provider herself or wrote in that they would not participate in referral, we categorized them as “no referral”.
All data were de-identified, cleaned and collected in RedCap. Paper surveys were manually entered and all were crosschecked for duplicates. We performed logistic regression to evaluate correlates of obligation to refer and to evaluate correlates of active referral for abortion. The multivariate models included clinician age, sex, specialty, clinician type, provision of obstetric services in the practice, rural vs. urban practice, religion and intrinsic religiosity a priori. We also included predictors with a p value of <0.1 in bivariate analysis using chi-squared tests for categorical variables and Kruskal Wallis test for continuous variables. We used STATA version 13.1 for statistical analysis.
Results
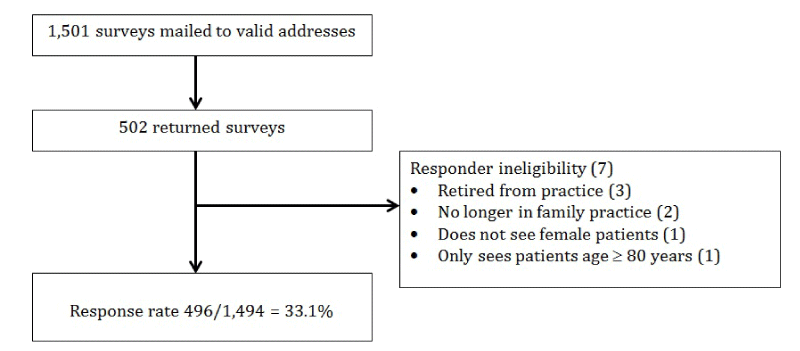
Of 1,501 valid surveys mailed to clinicians, a total of 506 (34%) were returned (111 electronically and 396 by mail). We excluded those who were retired (3), did not see women of reproductive age (4), had duplicate identification numbers (3) and one survey that was >90% blank. Thus we analyzed 496 of 1,495 (33%) of surveys. Study respondents were more likely to be younger, female, and identify as an advanced practice nurse or physician assistant when compared with non-respondents.
The majority of respondents were married, had children, provided family medicine care and had been in practice for a mean of 15.8 ± 10.9 years (Table 1). Similar to the state overall, 43% of respondents practiced in rural counties. For our primary outcome—obligation to refer—clinicians reported a professional obligation to refer most often for fetal anomalies (98%) and least often for abortion (52%, Table 2). For our secondary outcome—active referral—all clinicians (493) indicated they would provide an active referral for suspected gynecologic cancer, compared with 64% (312/488) of those who would provide an active referral for abortion (Table 2).
Clinical scenario* |
Proportion of participants who feel clinicians have a professional obligation to refer (n=481) |
Proportion of participants who would provide an active referral† (n=481-493)‡ |
In vitro fertilization |
A 30-year-old G0 desires to become pregnant. She underwent a bilateral salpingectomy to remove a symptomatic hydrosalpinx 3 years ago. She requests a referral to a fertility center that provides in vitro fertilization. |
78 |
98
|
High-risk
prenatal care |
A 24-year-old G1P0 is found to have a fetus with open spina bifida on her 20-week anatomy scan. She desires to continue the pregnancy and requests referral to a medical center that can care for her infant upon delivery. |
98 |
99.6
|
Abortion |
A 32-year-old G2P1001 has an undesired pregnancy at 7 weeks. She requests a referral for an abortion. |
52 |
64
|
Suspected gynecologic cancer |
A 48-year-old female is noted to have an asymptomatic adnexal mass on CT scan. She is concerned about ovarian cancer and requests a referral to a gyn-oncologist. |
96 |
100
|
Table 2. Clinical scenarios presented to OB/Gyn and family medicine clinicians in a rural US state.
*For all scenarios, participants were told that referral was not limited by insurance.
†Active referral defined as any of the following: 1) gives patient clinic name(s) and/or phone number(s), 2) sends patient’s records to the clinic, 3) contacts the clinic and/or clinician, 4) places an electronic referral to a provider.
‡Not all participants answered each question; for reporting an active method of referral, responses were in vitro fertilization (491), fetal anomalies (481), abortion (488) and suspected gynecologic cancer (493).
In multivariate analysis, only intrinsic religiosity was associated with decreased odds of reporting an obligation to refer for abortion (moderate intrinsic religiosity OR 0.59, 95% CI 0.35-0.98, p=0.04; high intrinsic religiosity OR 0.39, 95% CI 0.24-0.63, p<0.001; Table 3). We found a trend for clinicians who offered obstetric services in their practice being less likely to report an obligation to refer for abortion (OR 0.67, 95% CI 0.44-1.04, p=0.07).
Table 3. Odds of reporting an obligation to refer for abortion among clinicians in a rural US state (n=481).
|
n(%)
reporting an obligation to refer |
Unadjusted OR
(95% CI) |
P |
Adjusted OR*
(95% CI) |
P |
Personal characteristics |
|
|
|
|
|
Age (mean ± SD), years |
46.5±11.7 |
1.00 (0.99-1.02) |
0.86 |
1.00 (0.99-1.02) |
0.67 |
Sex |
|
|
|
|
|
Male |
82 (47) |
Ref |
|
Ref |
|
Female |
166 (54) |
1.32 (0.91-1.92) |
0.15 |
1.28 (0.77-2.14) |
0.34 |
Marital status |
|
|
|
|
|
Single |
32 (57) |
Ref |
|
- |
|
Married |
216 (51) |
0.78 (0.45-1.37) |
0.39 |
- |
|
Children |
|
|
|
|
|
None |
29 (58) |
Ref |
|
- |
|
One or more |
192 (51) |
0.76 (0.42-1.39) |
0.38 |
- |
|
Race |
|
|
|
|
|
White |
231 (51) |
Ref |
|
- |
|
Non-white |
14 (64) |
1.65 (0.68-4.03) |
0.26 |
- |
|
Practice characteristics |
|
|
|
|
|
Specialty |
|
|
|
|
|
OB/Gyn |
56 (57) |
Ref |
|
Ref |
|
Family medicine |
192 (50) |
0.75 (0.48-1.18) |
0.23 |
0.67 (0.38-1.16) |
0.15 |
Clinician type |
|
|
|
|
|
Physician |
112 (47) |
Ref |
|
Ref |
|
Advanced practice nurse |
67 (56) |
1.41 (0.91-2.19) |
0.13 |
1.09 (0.63-1.89) |
0.77 |
Physician assistant |
69 (56) |
1.40 (0.90-2.17) |
0.13 |
1.19 (0.70-2.02) |
0.52 |
County of practice |
|
|
|
|
|
Urban |
141 (51) |
Ref |
|
Ref |
|
Rural |
107 (52) |
1.01 (0.70-1.44) |
0.96 |
1.35 (0.88-2.05) |
0.17 |
Obstetric services offered in practice |
|
|
|
|
|
No |
104 (56) |
Ref |
|
Ref |
|
Yes |
148 (49) |
0.74 (0.51-1.07) |
0.11 |
0.67 (0.44-1.04) |
0.07 |
Standardized referral process |
|
|
|
|
|
No |
79 (51) |
Ref |
|
|
|
Yes |
164 (51) |
1.00 (0.68-1.47) |
0.98 |
- |
|
Years in practice (mean ± SD) |
15.7±11.2 |
1.00 (0.98-1.01) |
0.84 |
- |
|
Years in practice in Nebraska (mean ± SD) |
14.2±10.5 |
1.00 (0.98-1.01) |
0.68 |
- |
|
Religious characteristics |
|
|
|
|
|
Religion |
|
|
|
|
|
None |
24 (66) |
Ref |
|
Ref |
|
Protestant |
143 (52) |
0.55 (0.26-1.14) |
0.11 |
0.67 (0.30-1.49) |
0.32 |
Catholic |
69 (45) |
0.41 (0.19-0.88) |
0.02 |
0.51 (0.22-1.18) |
0.12 |
Other |
8 (73) |
1.33 (0.30-5.96) |
0.71 |
1.22 (0.25-6.08) |
0.80 |
Intrinsic religiosity‡ |
|
|
|
|
|
Low |
134 (62) |
Ref |
|
Ref |
|
Moderate |
50 (48) |
0.56 (0.35-0.89) |
0.02 |
0.59 (0.35-0.98) |
0.04 |
High |
55 (39) |
0.40 (0.26-0.61) |
<0.001 |
0.39 (0.24-0.63) |
<0.001 |
Data are as n (%) or mean + standard deviation.
CI = confidence interval. SD = standard deviation.
*The multivariate models included age, sex, specialty, clinician type, provision of obstetric services in the practice, rural vs. urban practice, religion and intrinsic religiosity.
†Rural vs. urban county based on the Office of Rural Health Policy definition.
‡Intrinsic religiosity defined based on agreement or disagreement with two statements: 1) “I try hard to carry my religious beliefs over into all my other dealings in life” and 2)“My whole approach to life is based on my religion”. Intrinsic religiosity was categorized as high for agreement with both statements, moderate for agreement with one statement and low for disagreement with both statements.
Thirty seven percent (181/488) of clinicians reported they had previously referred a patient for an abortion. Family medicine clinicians were less likely to report referring for abortion than ob-gyn clinicians (31% vs. 60%, p<0.001). Previous referral for abortion did not vary by clinician type (41% physician, 38% nurse practitioner, 29% physician assistant, p=0.09).
In multivariate analysis, female clinicians were more likely to provide an active method of abortion referral (OR 1.97, 95% CI 1.13-3.44, p=0.02) than male clinicians, and Catholic clinicians were less likely to provide an active method of abortion referral (OR 0.22, 95% CI 0.06-0.79, p=0.02; Table 4) than those without a religious affiliation. Clinicians with increasing levels of intrinsic religiosity also were less likely to provide an active method of abortion referral (moderate intrinsic religiosity OR 0.44, 95% CI 0.25-0.77, p<0.01; high intrinsic religiosity OR 0.17, 95% CI, 0.10-0.28, p<0.001; Table 4).
Table 4. Odds of providing an active referral* for abortion among clinicians in a rural US state (n=488).
|
n (%)
providing an active referral |
Unadjusted OR (95% CI) |
P |
Adjusted OR† (95% CI) |
P |
Personal characteristics |
|
|
|
|
|
Age (mean ± SD), years |
46.6 ± 11.7 |
1.00 (0.99-1.02) |
0.86 |
1.02 (0.99-1.04) |
0.15 |
Sex |
|
|
|
|
|
Male |
100 (57) |
Ref |
|
|
|
Female |
211 (68) |
1.64 (1.13-2.41) |
0.01 |
1.97 (1.13-3.44) |
0.02 |
Marital status |
|
|
|
|
|
Single |
41 (72) |
Ref |
|
- |
|
Married |
267 (63) |
0.67 (0.36-1.23) |
0.20 |
- |
|
Children |
|
|
|
|
|
None |
32 (64) |
Ref |
|
- |
|
One or more |
248 (66) |
1.11 (0.59-2.03) |
0.77 |
- |
|
Race |
|
|
|
|
|
White |
287 (64) |
Ref |
|
- |
|
Non-white |
16 (70) |
1.31 (0.53-3.24) |
0.57 |
- |
|
Practice characteristics |
|
|
|
|
|
Specialty |
|
|
|
|
|
OB/Gyn |
70 (70) |
Ref |
|
Ref |
|
Family medicine |
242 (62) |
0.71 (0.44-1.14) |
0.16 |
0.80 (0.43-1.50) |
0.49 |
Clinician type |
|
|
|
|
|
Physician |
145 (60) |
Ref |
|
Ref |
|
Advanced practice nurse |
81 (67) |
1.35 (0.86-2.14) |
0.19 |
0.95 (0.51-1.77) |
0.87 |
Physician assistant |
86 (69) |
1.48 (0.93-2.33) |
0.10 |
1.22 (0.68-2.20) |
0.51 |
County of practice‡ |
|
|
|
|
|
Urban |
180 (65) |
Ref |
|
Ref |
|
Rural |
131 (62) |
0.89 (0.61-1.29) |
0.54 |
1.29 (0.81-2.05) |
0.28 |
Obstetric services offered in practice |
|
|
|
|
|
No |
115 (62) |
Ref |
|
Ref |
|
Yes |
192 (65) |
1.15 (0.78-1.68) |
0.49 |
1.13 (0.70-1.82) |
0.61 |
Standardized referral process |
|
|
|
|
|
No |
97 (63) |
Ref |
|
|
|
Yes |
206 (64) |
1.06 (0.71-1.58) |
0.77 |
- |
|
Years in practice (mean ± SD) |
15.6 ± 10.9 |
1.00 (0.98-1.01) |
0.73 |
- |
|
Years in practice in Nebraska (mean ± SD) |
14.3 ± 10.6 |
1.00 (0.98-1.02) |
0.83 |
- |
|
Religious characteristics |
|
|
|
|
|
Religion |
|
|
|
|
|
None |
31 (89) |
Ref |
|
Ref |
|
Protestant |
177 (65) |
0.24 (0.08-0.70) |
<0.01 |
0.35 (0.10-1.26) |
0.11 |
Catholic |
88 (57) |
0.17 (0.06-0.50) |
<0.01 |
0.22 (0.06-0.79) |
0.02 |
Other |
10 (77) |
0.43 (0.08-2.26) |
0.32 |
0.47 (0.07-3.11) |
0.44 |
Intrinsic religiosity§ |
|
|
|
|
|
Low |
175 (81) |
Ref |
|
Ref |
|
Moderate |
67 (62) |
0.37 (0.22-0.63) |
<0.001 |
0.44 (0.25-0.77) |
<0.01 |
High |
57 (40) |
0.15 (0.09-0.25) |
<0.001 |
0.17 (0.10-0.28) |
<0.001 |
Data are as n (%) or mean + standard deviation.
CI = confidence interval. SD = standard deviation.
*Active referral defined as any of the following: 1) gives patient clinic name(s) and/or phone number(s), 2) sends patient’s records to the clinic, 3) contacts the clinic and/or clinician, 4) places an electronic referral to a provider.
†The multivariate models included age, sex, specialty, clinician type, provision of obstetric services in the practice, rural vs. urban practice, religion and intrinsic religiosity.
‡Rural vs. urban county based on the Office of Rural Health Policy definition.
§Intrinsic religiosity defined based on agreement or disagreement with two statements: 1) “I try hard to carry my religious beliefs over into all my other dealings in life” and 2)“My whole approach to life is based on my religion”. Intrinsic religiosity was categorized as high for agreement with both statements, moderate for agreement with one statement and low for disagreement with both statements.
Discussion
Our study found that clinicians in one rural US state were less likely to feel professionally obligated to refer and less likely to directly refer for abortion than for other reproductive health scenarios. More religious clinicians were less likely to consider abortion referral an obligation and to provide active referrals for abortion services. Female clinicians gave active referrals for abortion more often than males. Approximately 1 in 5 clinicians in our study reported they would not participate in referring a patient for an abortion.
In our study, almost half of clinicians did not feel professionally obligated to refer for abortion, substantially more than a national survey of US physicians that found 29 percent of doctors do not believe they have an obligation to disclose information about safe, legal, medically available treatment that the doctor considers morally objectionable [12]. Similar to our study, a previous survey of US physician attitudes about helping a woman obtain an abortion found that female clinicians are more likely to facilitate a woman obtaining an abortion [19].
Strengths of this study include the variety of clinician types surveyed: both family medicine and ob-gyn clinicians as well as advanced practice nurses and physician assistants in addition to physicians. In primarily rural states like Nebraska, physician assistants and advanced practice nurses provide much of the healthcare (39% of ob-gyn clinicians and 41% of family medicine clinicians in the database used for the study). These primary care clinicians serve as a resource and access point for specialty care, but their opinions on abortion referral have previously not been assessed. Their attitudes about abortion referral are of particular importance for rural women because nurse practitioners and physician assistants are more likely to practice in rural areas [20]. These clinicians care for patients presenting with undesired pregnancies and provide abortions with the same safety as physicians around the globe, including one US state [21]. Studies like ours will inform the need for clinician education to include counseling and referral so that these healthcare providers are competent to care for their patients.
Limitations of this study include our generalizability as clinicians’ complex attitudes on abortion and specific obstacles to abortion referral may vary by region [19]. Additionally, clinician responses to the presented hypothetical scenarios presented may not reflect their day-to-day practice. The abortion scenario in our study did not give additional social or medical circumstances surrounding the women’s reasons for choosing an abortion, which may influence a clinician’s decision to refer for abortion [19]. Finally, our low response rate may also indicate a biased sample, but it is comparable to other studies of clinicians [22]. Respondents may represent a group of clinicians who feel more strongly about abortion than non-respondents.
Family planning services are critical components of public health. Early access to safe abortion is important for decreasing maternal morbidity and mortality. While our study surveyed clinicians in one country where abortion is unrestricted, a recent systematic review of barriers to abortion services in the US and 8 other countries with varying abortion restrictions found that women continue to face significant challenges accessing the quality abortion services as recommended by the WHO [10]. In countries with more abortion restrictions, a failure to refer for safe services may increase the likelihood of a woman seeking an unsafe abortion. We propose dedicating resources to ensure clinicians understand their local abortion laws and where women may obtain safe services.
When faced with a woman who desires abortion, clinicians should provide unbiased counseling and prompt referral. That half of clinicians in our sample do not believe referral is a professional obligation once more raises the question asked by lawyer R. Alta Charo in a New England Journal of Medicine commentary: to what extent do professionals have a collective duty to ensure that their profession provides nondiscriminatory access to all professional services [23]? As a medical and public health community responsible for caring for women across the lifespan, clinicians must support women’s autonomy, and if a patient chooses abortion, ensures that she accesses it through appropriate referral.
Authorship
Valerie French: Study design, data collection, data analysis, manuscript writing.
Renaisa Anthony: Study design, oversight of data collection, manuscript writing.
Susana Berrios: Data collection, manuscript writing.
Libby Crockett: Study design, data collection, manuscript writing.
Jody Steinauer: Senior2021 Copyright OAT. All rights reservection, data analysis and manuscript writing.
Funding
Funded by a grant from the Society of Family Planning, number A123460.
Disclosure
The authors did not report any potential conflicts of interest.
[1] The Census Bureau's urban areas represent densely developed territory and encompass residential, commercial, and other nonresidential urban land uses. The Census Bureau identifies two types of urban areas: “urbanized areas” of 50,000 or more people and “urban clusters” of at least 2,500 and less than 50,000 people. “Rural” encompasses all population, housing and territory not included within an urban area. (2010 United States Census)
References:
- 2010 United States Census. Frequently asked questions. https://ask.census.gov/faq.php?id=5000&faqId=5971. Accessed August 3, 2015.
- Jones RK, Jerman J (2014) Abortion incidence and service availability in the United States, 2011. Perspect Sex Reprod Health 46: 3-14.
- Jones RK, Jerman J (2013) How far did US women travel for abortion services in 2008? J Women’s Health (Larchmt) 22: 706-713. [Crossref]
- Rayburn WF, Klagholz JC, Murray-Krezan C, Dowell LE, Strunk AL (2012) Distribution of American congress of obstetricians and gynecologists fellows and junior fellows in practice in the United States. Obstet Gynecol 119: 1017-1022. [Crossref]
- Drey EA, Foster DG, Jackson RA, Lee SJ, Cardenas LH, et al. (2006) Risk factors associated with presenting for abortion in the second trimester. Obstet Gynecol 107: 128-135. [Crossref]
- International Federation of Gynecology and Obstetrics, Society of Obstetricians and Gynaecologists of Canada (2004) International joint policy statement. FIGO professional and ethical responsibilities concerning sexual and reproductive rights. J Obstet Gynaecol Can 26: 1097-1099, 1105-1107.
- Royal College of Obstetricians and Gynecologists. The care of women requesting induced abortion: Evidence-based clinical guideline number 7. 2011.
- American College of Obstetricians and Gynecologists (2007) ACOG committee opinion no. 385 November 2007: The limits of conscientious refusal in reproductive medicine. Obstet Gynecol 110: 1203-1208. [Crossref]
- World Medical Association (2006) WMA declaration on therapeutic abortion. Handbook of WMA policies.
- World Health Organization. Safe abortion: Technical and policy guidance for health systems. 2nd ed. Geneva: 2012.
- Combs MP, Antiel RM, Tilburt JC, Mueller PS, Curlin FA (2011) Conscientious refusals to refer: Findings from a national physician survey. J Med Ethics 37: 397-401. [Crossref]
- Curlin FA, Lawrence RE, Chin MH, Lantos JD (2007) Religion, conscience, and controversial clinical practices. N Engl J Med 356: 593-600. [Crossref]
- Savulescu J (2006) Conscientious objection in medicine. BMJ 332: 294-297. [Crossref]
- Brauer SG, Yoon JD, Curlin FA (2015) US primary care physicians' opinions about conscientious refusal: A national vignette experiment. J Med Ethics.
- Rasinski KA, Yoon JD, Kalad YG, Curlin FA (2011) Obstetrician-gynaecologists' opinions about conscientious refusal of a request for abortion: Results from a national vignette experiment. J Med Ethics 37: 711-714. [Crossref]
- Koenig H, Parkerson GR Jr, Meador KG (1997) Religion index for psychiatric research. Am J Psychiatry 154: 885-886. [Crossref]
- Gorsuch RL, McPherson SE (1989) Intrinsic/extrinsic measurement, I/E-revised and single-item scales. J Sci Study Relig 28: 348-354.
- Ellison CG, Gay DA, Glass TA (1989) Does religious commitment contribute to individual life satisfaction? Soc Forces 68: 100-123.
- Harris LH, Cooper A, Rasinski KA, Curlin FA, Lyerly AD (2011) Obstetrician-gynecologists' objections to and willingness to help patients obtain an abortion. Obstet Gynecol 118: 905-912. [Crossref]
- Freedman L, Landy U, Darney P, Steinauer J (2010) Obstacles to the integration of abortion into obstetrics and gynecology practice. Perspect Sex Reprod Health 42: 146-151. [Crossref]
- Freedman L, Battistelli MF, Gerdts C, McLemore M (2015) Radical or routine? nurse practitioners, nurse-midwives, and physician assistants as abortion providers. Reprod Health Matters 23: 90-92. [Crossref]
- McLeod CC, Klabunde CN, Willis GB, Stark D (2013) Health care provider surveys in the United States, 2000-2010: A review. Eval Health Prof 36: 106-126. [Crossref]
- Charo RA (2005) The celestial fire of conscience -- refusing to deliver medical care. N Engl J Med 352: 2471-2473. [Crossref]